Summary
Synopsis
Amiodarone, originally developed over 20 years ago, is a potent antiarrhythmic drug with the actions of all antiarrhythmic drug classes. It has been successfully used in the treatment of symptomatic and life- threatening ventricular arrhythmias and symptomatic supraventricular arrhythmias. In patients with left ventricular dysfunction amiodarone does not usually produce any clinically significant cardiodepression and the drug has relatively high antiarrhythmic efficacy. Preliminary studies indicate that amiodarone may have a beneficial effect on mortality and survival in certain groups of patients with ventricular arrhythmias, an action probably related to both its antiarrhythmic and antifibrillatory effects.
The adverse effect profile of amiodarone is diverse, involving the cardiac, thyroid, pulmonary, hepatic, gastrointestinal, ocular, neurological and dermatological systems. Interstitial pneumonitis and hepatitis are potentially fatal, but the vast majority of adverse events are less serious, and some may be dose dependent. Pretreatment monitoring, regular assessments and the use of minimum effective doses are, therefore, necessary.
Thus, with appropriate monitoring to control its well recognised adverse effects amiodarone has an important place as an effective ‘broad spectrum’ antiarrhythmic drug which has, so far, been used when other treatments have proved ineffective. More recent preliminary data also suggest that it may also have a beneficial effect in the prevention of sudden death in some patients.
Pharmacodynamic Properties
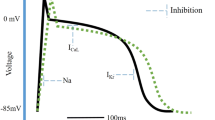
Amiodarone was originally described as a class III antiarrhythmic owing to its ability to increase the action potential duration, thereby prolonging repolarisation and refractoriness. In addition, class I antiarrhythmic effects, calcium channel blocking effects and a propensity to non-competitively antagonise α- and β-adrenergic receptors have been seen. On acute administration amiodarone inhibits inactivated membrane sodium channels, producing a decrease in the rate of phase 0 depolarisation \((\dot V_{\max } )\). In ischaemic conditions class I antiarrhythmic effects predominate. Long term administration results in prolongation of the action potential duration in conjunction with a decrease in \(\dot V_{\max }\).
In clinical electrophysiological studies long term oral amiodarone increases atrial, atrioventricular nodal, His-Purkinje and ventricular refractoriness, sinus cycle length and QT interval, and moderately slows intracardiac conduction.
In animal models of arrhythmia amiodarone reduced the incidence of ischaemia-induced ventricular arrhythmias in the dog. Furthermore, there is some evidence of a cardioprotective effect in ischaemic models, with reductions in the area of necrosis following infarction.
Neither intravenous nor oral amiodarone appears to alter haemodynamic function in a clinically significant way, although in patients with severely depressed left ventricular function hypotension has been reported.
Pharmacokinetic Properties
The pharmacokinetics of amiodarone and its main metabolite, desethylamiodarone (DEA), are not completely understood and there are large interindividual variations in bioavailability, plasma concentrations and elimination half-life. Oral bioavailability of amiodarone is approximately 40%, probably reflecting incomplete and slow gastrointestinal absorption, and the time to reach peak plasma concentration ranges from 2 to 10 hours. Long term oral treatment does not produce steady-state plasma concentrations for at least 1 month, although antiarrhythmic effects are seen before this time. A therapeutic plasma concentration range of 1 to 2.5 mg/L has been suggested as a rough guide, but clinical response should also be used for determining dose. Amio- darone displays extensive tissue distribution, with the highest concentrations found in adipose tissue. DEA concentrations exceed those of amiodarone in all tissues except fat. The volume of distribution is high, approximately 5000L, and in plasma the drug is approximately 95% protein bound.
Metabolism is partly intestinal but mainly hepatic and virtually all the drug is metabolised. Biliary and faecal excretion are the major routes of elimination, with renal excretion responsible for less than 1% of the administered dose, making dosage adjustment unnecessary in cases of renal impairment. Elimination appears biphasic following single oral and intravenous doses, with terminal elimination half-lives of 3.2 to 21 hours reported. Following long term oral administration the average terminal elimination half-life is 40 days. This has important implications for dosage adjustment, as it may take at least 1 month for new plasma concentrations to stabilise, while total clearance from the body can take more than 4 months.
Therapeutic Use
The vast majority of patients treated with amiodarone have generally presented with the more severe and sustained refractory arrhythmias.
In ventricular arrhythmias intravenous amiodarone (usually 5 mg/kg over 20 to 30 minutes as a loading dose) has suppressed life-threatening sustained ventricular tachycardia or ventricular fibrillation in approximately 40% of patients. Oral treatment (loading plus maintenance therapy) has reduced the recurrence of ventricular tachycardia or ventricular fibrillation in 70 to 95% of patients in noncomparative studies and these effects persisted for long periods. In comparative studies oral amiodarone has proved significantly more effective than placebo, and of comparable efficacy to sotalol, propranolol, flecainide, encainide, propafenone and moricizine in patients with ventricular arrhythmias. Several studies indicated that amiodarone may reduce the incidence of sudden death in patients with arrhythmias associated with organic heart disease, an effect probably related to its antiarrhythmic and antifibrillatory effects.
In patients with atrial tachyarrhythmias amiodarone has proved very successful in both restoring and maintaining sinus rhythm in 30 to 95% of patients when used in conjunction with electrocardioversion, particularly in paroxysmal arrhythmias. Amiodarone has generally been more successful than either verapamil or quinidine, and appears promising in moderate to marked left atrial dilatation.
Suppression of paroxysmal supraventricular tachycardia (SVT) [with or without Wolff-Parkinson-White syndrome] is seen in approximately 75% of patients following treatment with amiodarone. This, along with efficacy in a range of re-entry arrhythmias, may relate to amiodarone’s propensity to suppress premature beats and increase the refractory periods of the atrioventricular node and accessory conduction pathways.
In both hypertrophic and dilated cardiomyopathy amiodarone has proved effective in suppressing both ventricular tachycardia and SVT, and may be associated with improved survival in those patients with hypertrophic cardiomyopathy.
Tolerability
Adverse effects of amiodarone are mainly dose dependent, and predominantly endocrine (hypo-or hyperthyroidism), pulmonary (interstitial pneumonitis), hepatic (abnormally elevated liver enzymes, hepatitis), cardiac (proarrhythmia, bradycardia, worsening congestive heart failure), gastrointestinal (nausea, anorexia, constipation), ocular (corneal microdeposits), neurological (tremor, neuropathy) and dermatological (photosensitivity, grey/blue discoloration). These range from minor asymptomatic problems requiring no intervention to life-threatening problems necessitating drug withdrawal and supportive measures. Interstitial pneumonitis is probably the most serious toxic reaction. Pretreatment assessment and regular monitoring, in conjunction with the use of minimum effective doses, provide the basis for early recognition and appropriate effective management.
Drug Interactions
Amiodarone alters the pharmacokinetics of digoxin, oral anticoagulants, class I antiarrhythmic drugs, β-blockers and calcium channel blockers. Importantly, the long plasma elimination half-life of amiodarone means that the potential for significant drug interaction persists for some time after treatment has stopped. Dosages of digoxin should be reduced by 25 to 50%, while those of oral anticoagulants (warfarin, acenocoumarol) should be reduced by about 50%. Close monitoring of plasma digoxin levels and prothrombin time is essential. There is a possibility of potentiating sinus bradycardia or arrest, or proarrhythmic effects when amiodarone is used in conjunction with class I antiarrhythmics, β-blockers and calcium channel blockers.
Dosage and Administration
The recommended dosage of amiodarone administered intravenously in adults with any tachyarrhythmia is up to 5 mg/kg over 20 to 120 minutes, in conjunction with ECG monitoring. Doses of 10 to 20 mg/kg may be infused in a 24-hour period. Rapid intravenous bolus injection may induce hypotension. When administered orally loading doses of 600 to 1200 mg/day are generally given for 1 to 2 weeks and then the dose is titrated down to 400 to 800 mg/day for a month. Maintenance therapy is usually 200 to 400 mg/day.
Similar content being viewed by others
References
Abdollah H, Brien JF, Brennan FJ. Antiarrythmic effects of desethylamiodarone in dogs with subacute myocardial infarction and inducible ventricular arrhythmias. Journal of Cardiovas- cular Pharmacology 13(1): 37–44, 1989
Abdollah H, Brien JF, Brennan FJ. Antiarrhythmic effect of chronic oral amiodarone treatment in dogs with myocardial infarction and reproducibly inducible sustained ventricular arrhythmias. Journal of Cardiovascular Pharmacology 15(5): 799–807, 1990
Adams GD, Kehoe R, Lesch M, Glassroth J. Amiodarone-induced pneumonitis. Assessment of risk factors and possible risk reduction. Chest 93(2): 254–263, 1988
Adams PC, Holt DW, Storey GCA, Morley AR, Callaghan J, et al. Amiodarone and its desethyl metabolite: tissue distribution and morphologic changes during long-term therapy. Circulation 72: 1064–1075, 1985
Albert SG, Alves LE, Rose EP. Thyroid dysfunction during chronic amiodarone therapy. Journal of the American College of Cardiology 9(1): 175–183, 1987
Alboni P, Shantha N, Pirani R, Baggioni F, Scarfo S, et al. Effects of amiodarone on supraventricular tachycardia involving bypass tracts. American Journal of Cardiology 53: 93–98, 1984
Amiodarone vs Sotalol Study Group. Multicentre randomized trial of sotalol vs amiodarone for chronic malignant ventricular tachyarrhythmias. European Heart Journal 10(8): 685–694, 1989
Andreasen F, Agerbaek H, Bjerregaard P, Gotzsche H. Pharmacokinetics of amiodarone after intravenous and oral administration. European Journal of Clinical Pharmacology 19: 293–299, 1981
Aomine M. Acute effects of amiodarone on action potentials of isolated guinea-pig ventricular muscle exposed to simulated ischemic solution and metabolic inhibitors. General Pharma- cology 19(4): 609–613, 1988a
Aomine M. Does acute exposure to amiodarone prolong cardiac action potential duration? General Pharmacology 19(4): 615–619, 1988b
Aomine M. Acute effects of amiodarone on action potentials of isolated canine purkinje fibers: comparison with tetrodotoxin effects. General Pharmacology 19(4): 601–607, 1988c
Aomine M. Inhibition by amiodarone of slow response action potentials and contraction in guinea pig ventricular muscle. General Pharmacology 19(4): 621–623, 1988d
Aomine M. Multiple electrophysiological actions of amiodarone on guinea pig heart. Naunyn-Schmiedeberg’s Archives of Pharmacology 338: 589–599, 1988e
Aomine M. Inhibition of tetrodotoxin-sensitive plateau sodium current by amiodarone in guinea pig cardiac muscles. General Pharmacology 20(5): 653–658, 1989
Arredondo MT, Guillen SG, Quinteiro RA. Effect of amiodarone on ventricular fibrillation and defibrillation thresholds in the canine heart under normal and ischemic conditions. European Journal of Pharmacology 125: 23–28, 1986
Bach N, Schultz BL, Cohen LB, Squire A, Gordon R, et al. Amiodarone hepatotoxicity: Progression from steatosis to cirrhosis. Mount Sinai Journal of Medicine 56(4): 293–296, 1989
Batisse A, Sardet A, Fermont L, Kachaner J. Traitement des tachycardies ventriculaires du nourrisson et de l’enfant par l’a-miodarone. Archives des Maladies du Coeur et des Vaisseaux 75(8): 829–835, 1982
Bayés de Luna A, Guindo J, Borja J, Roman M, Madoery C. Recasting the approach to the treatment of potentially malignant ventricular arrhythmias after the cast study. Cardiovascular Drugs and Therapy 4: 651–656, 1990
Beckers J, Kulbertus HE. Class III drugs: Amiodarone. European Heart Journal 8 (Suppl. A): 53–59, 1987
Berdeaux A, Roche A, Labaille T, Giroux B, Edouard A, et al. Tissue extraction of amiodarone and N-desethylamiodarone in man after a single oral dose. British Journal of Clinical Pharmacology 18: 759–763, 1984
Bertini G, Conti A, Fradella G, Francardelli L, Giglioli C, et al. Propafenone versus amiodarone in field treatment of primary atrial tachydysrhythmias. Journal of Emergency Medicine 8: 15–20, 1990
Biron P, Turcotte F, Barrette A, Mailhot C, Rimeau RE. Life table estimation of amiodarone induced corneal microdeposits. Canadian Journal of Cardiology 3(7): 334–335, 1987
Blevins RD, Kerin NZ, Benaderet D, Frumin H, Faitel K, et al. Amiodarone in the management of refractory atrial fibrillation. Archives of Internal Medicine 147(8): 1401–1404, 1987
Bogers AJJC, Quaegebeur JM, Ottenkamp J, Huysmans HA. Treatment of ventricular arrhythmia after corrective cardiac surgery in a neonate with intravenous amiodarone. Thoracic and Cardiovascular Surgeon 35: 124–125, 1987
Bonati M, D’Arrano V, Galletti F, Fortunati MT, Tognoni G. Acute overdosage of amiodarone in a suicide attempt. Journal of Toxicology, Clinical Toxicology 20: 181–186, 1983
Branzi A, Rappezzi C, Benenati PM, Binetti G, Piovaccari G, et al. Haemodynamic effects of short term intravenous amiodarone for hypertrophic cardiomyopathy. British Heart Journal 59: 446–452, 1988
Brennan FJ, Brien JF, Armstrong PW. Plasma concentration time course and pharmacological effects of a standardized oral amiodarone dosing regimen in humans. Canadian Journal of Cardiology 7(3): 117–124, 1991
Brodsky MA, Allen BJ, Walker CJ, Casey TP, Luckett CR, et al. Amiodarone for maintenance of sinus rhythm after conversion of atrial fibrillation in the setting of a dilated left atrium. American Journal of Cardiology 60: 572–575, 1987
Brugada P. Should electrophysiologic studies be performed to assess drug efficacy in patients receiving amiodarone? American Journal of Cardiology 59(15): 1415–1416, 1987
Burkart F, Pfisterer M, Kiowski W, Follath F, Burckhardt D. Effect of antiarrhythmic therapy on mortality in survivors of myocardial infarction with asymptomatic complex ventricular arrhythmias: Basel antiarrhythmic study of infarct survival (BASIS). Journal of the American College of Cardiology 16(7): 1711–1718, 1990
Cairns JA, Connolly SJ, Gent M, Roberts R. Post-myocardial infarction mortality in patients with ventricular premature depolarisations. Canadian Amiodarone Myocardial Infarction Arrhythmia Trial Pilot Study. Circulation 84: 550–557, 1991
Campbell TJ, Hemsworth PD. Selective depression of maximum rate of depolarization of guinea-pig ventricular action poten- tials by amiodarone and lignocaine in simulated ischaemia: comparison with encainide. Clinical and Experimental Pharmacology and Physiology 17: 135–145, 1990
Cantor J. Elevation of serum cholesterol and triglycerides as a complication of amiodarone therapy. Journal of the Royal College of General Practitioners 39(323): 258, 1989
Caraco Y, Chajek-Shaul T. The incidence and clinical significance of amiodarone and acenocoumarol interaction. Thrombosis and Haemostasis 62(3): 906–908, 1989
CAST Investigators. Cardiac arrhythmia suppression trial. New England Journal of Medicine 321: 406–412, 1989
Ceppi JA, Zaninovich AA. Effects of amiodarone on 5’-deiodi- nation of thyroxine to tri-iodothyronine in rat myocardium. Journal of Endocrinology 121:431–434, 1989
Chalmers RJG, Muston HL, Srinivas V, Bennett DH. High in- cidence of amiodarone-induced photosertsitivity in Northwest England. British Medical Journal 285: 341, 1982
Chow CC, Cockram CS. Thyroid disorders induced by lithium and amiodarone: an overview. Adverse Drug Reactions and Acute Poisoning Reviews 9(4): 207–222, 1990
Cleland JGF, Dargie HJ, Findlay IN, Wilson JT. Clinical, haemo- dynamic, and antiarrhythmic effects of long term treatment with amiodarone of patients in heart failure. British Heart Journal 57: 436–445, 1987a
Cleland JGF, Dargie HJ, Ford I. Mortality in heart failure: clinical variables of prognostic value. British Heart Journal 58: 572–582, 1987b
Clement RS, MacKintosh HT. Drug induced ocular lipoidosis. Transactions of the Ophthalmological Societies of New Zealand 34: 52–58, 1982
Cobbe SM, Manley BS. The influence of ischaemia on the elec- trophysiological properties of amiodarone in chronically treated rabbit hearts. European Heart Journal 8: 1241–1248, 1987
Colvin RA, Ashavaid TF, Katz AM, Messineo FC. Amiodarone, verapamil, and quinidine do not affect equilibrium binding of digoxin. Journal of Cardiovascular Pharmacology 16: 519–522, 1990
Cote P, Bourassa MG, Delaye J, Janin A, Froment R, et al. Effects of amiodarone on cardiac and coronary hemodynamics and on myocardial metabolism in patients with coronary artery disease. Circulation 54: 1165–1172, 1979
Coulter DM, Edwards IR, Savage RL. Survey of neurological problems with amiodarone in the New Zealand Intensive Medicines Monitoring Programme. New Zealand Medical Journal 103(885): 98–100, 1990
Counihan PJ, McKenna WJ. Low-dose amiodarone for the treatment of arrhythmias in hypertrophic cardiomyppathy. Journal of Clinical Pharmacology 29(5): 436–438, 1989
Counihan PJ, McKenna WJ. Risk-benefit assessment of amio- darone in the treatment of cardiac arrhythmias. Drug Safety 5(4): 286–304, 1990
Daniels JM, Leeder RG, Brien JF. Repeated amiodarone exposure in the rat: toxicity and effects on hepatic and extrahepatic monooxygenase activities. Canadian Journal of Physiology and Pharmacology 68: 1261–1268, 1990
DeBoer LWV, Nost JJ, Loner RA, Braunwald E. Studies of amiodarone during experimental myocardial infarction: beneficial effects on haemodynamics and infarct size. Circulation 65(3): 508–512,1982
De Paola AAV, Horowitz LN, Spielman SR, Brady P, Morganroth J, et al. Development of congestive heart failure and alterations in left ventricular function in patients with sustained ventricular tachyarrhythmias treated with amiodarone. American Journal of Cardiology 60(4): 276–280, 1987
Desmet M, Massart DL. Determination of amiodarone and desethylamiodarone in plasma with a standardised extraction and chromatographic optimisation procedure. Journal of Pharmaceutical and Biomedical Analysis 6(3): 277–284, 1988
Dunn M, Glassroth J. Pulmonary complications of amiodarone toxicity. Progress in Cardiovascular Diseases 31(6): 447–453, 1989
Dusman RE, Stanton MS, Miles WM, Klein LS, Zipes DP, et al. Clinical features of amiodarone-induced pulmonary toxicity. Circulation 82(1): 51–59, 1990
Editorial. Amiodarone and torsade de pointes. Annals of Internal Medicine 111 (7): 549-551, 1989
Editorial. Surgical treatment of hypertrophic obstructive cardio- myopathy. Lancet 1 (8634): 358-362, 1989
Emmertsen K, Bjerregaard B, Andreasen F. Amiodarone for refractory supraventricular tachycardias. Acta Medica Scandinavica 221(5): 435–439, 1987
Fain ES, Lee JT, Winke RA. Effects of acute intravenous and chronic oral amiodarone on defibrillation energy requirements. American Heart Journal 114(1): 8–17, 1987
Falik R, Flores BT, Shaw L, Gibson GA, Josephson ME, et al. Relationship of steady-state serum concentrations of amiodarone and desethylamiodarone to therapeutic efficacy and adverse effects. American Journal of Medicine 82: 1102–1108, 1987
Fananapazir L, Epstein SE. Value of electrophysiologic studies in hypertrophic cardiomyopathy treated with amiodarone. American Journal of Cardiology 67(2): 175–182, 1991
Fananapazir L, Leon MB, Bonow RO, Tracy CM, Cannon RO, et al. Sudden death during empiric amiodarone therapy in symptomatic hypertrophic cardiomyopathy. American Journal of Cardiology 67(2): 169–174, 1991
Feld GK, Nademanee K, Stevenson W, Weiss J, Klitzner T, et al. Clinical and electrophysiologic effects of amiodarone in patients with atrial fibrillation complicating the Wolff-Parkinson-White syndrome. American Heart Journal 115: 102–107, 1988
Figge HL, Figge J. The effects of amiodarone on thyroid hormone function: a review of the physiology and clinical manifestations. Journal of Clinical Pharmacology 30(7): 588–595, 1990
Finerman WB, Hamer A, Peter T, Weiss D, Mandel WJ. Elec- trophysiologic effects of chronic amiodarone therapy in patients with ventricular arrhythmias. American Heart Journal 104(5): 987–996, 1982
Fish FA, Roden DM. A prolonged QTc inverval. Is it an important effect of antiarrhythmic drugs? Medical Toxicology and Adverse Drug Experience 4(6): 400–411, 1989
Fisher JD, Kim SG, Waspe LE, Johnston DR. Amiodarone: value of programmed electrical stimulation and holter monitoring. Pacing and Clinical Electrophysiology 9: 422–435, 1986
Flaharty KK, Chase SL, Yaghsezian HM, Rubin R. Hepatotoxicity associated with amiodarone therapy. Pharmacotherapy 9(1): 39–44, 1989
Fogoros RN. Amiodarone-induced refractoriness to cardioversion. Annals of Internal Medicine 100: 699–700, 1984
Fogoros RN. Current status of amiodarone. Primary Cardiology 15: 61–66, September 1989
Follmer CH, Aomine M, Yeh JZ, Singer DH. Amiodarone-in- duced block of sodium current in isolated cardiac cells. Journal of Pharmacology and Experimental Therapeutics 243(1): 187–194, 1987
Foresti V, Carini L, Lovagnini-Scher CA, Parisio E, Scolari N, et al. Amiodarone lung toxicity: role of pulmonary function tests. International Journal of Clinical Pharmacology Research 7(5): 373–380, 1987
Foresti V, Pepe R, Parisio E, Scolari N, Zubani R, et al. Antithyroid antibodies during amiodarone treatment. Acta Endocrinologica 121(2): 203–206, 1989
Foster CJ, Love HG. Amiodarone in pregnancy. Case report and review of the literature. International Journal of Cardiology 20: 307–316, 1988
Fournier C, Brunei M, Bah M, Kindermans M, Boujon B, et al. Comparison of the efficacy of propranolol and amiodarone in suppressing ventricular arrhythmias following myocardial in- farction. European Heart Journal 10: 1090–1100, 1989
Frame LH. The effect of chronic oral and acute intravenous amiodarone administration on ventricular defibrillation threshold using implanted electrodes in dogs. Pacing and Clinical Electrophysiology 12: 339–346, 1989
Frumin H, Kerin NZ, Rubenfire M. Classification of antiarrhythmic drugs. Journal of Clinical Pharmacology 29: 387–394,1989
Gallagher JD, Bianchi J, Gessman LJ. A comparison of the electrophysiologic effects of acute and chronic amiodarbne administration on canine purkinje fibers. Journal of Cardiovascular Pharmacology 13(5): 723–729, 1989
Gallastegui JL, Bauman JL, Anderson JL, Winkle RA, Ezri MD, et al. Worsening of ventricular tachycardia by amiodarone. Journal of Clinical Pharmacology 28: 406–411,1988
Gammage MD, Franklyn JA. Amiodarone and the thyroid. Quarterly Journal of Medicine 62(238): 83–86, 1987
Garson A, Gilette PC, McVey P, Hesslein PS, Porter CJ, et al. Amiodarone treatment of critical arrhythmias in children and young adults. Journal of the American College of Cardiology 4: 749–755, 1984
Gembruch U, Manz M, Bald R, Rüddel H, Redel DA, et al. Repeated intravascular treatment with amiodarone in a fetus with refractory supraventricular tachycardia and hydrops fetalis. American Heart Journal 118(6): 1335–1338, 1989
Giardina E-GV, Schneider M, Barr ML. Myocardial amiodarone and desethylamiodarone concentrations in patients undergoing cardiac transplantation. Journal of the American College of Cardiology 16(4): 943–947, 1990
Gilinsky NH, Briscoe GW, Kuo C-S. Fatal amiodarone hepatoxocity. American Journal of Gastroenterology 83(2): 161–163, 1988
Gleadhill IC, Wise RA, Schonfeld SA, Scott PP, Guarnieri T, et al. Serial lung function testing in patients treated with amiodarone: a prospective study. American Journal of Medicine 86(1): 4–10, 1989
Goddard CJR, Whorwell PJ. Amiodarone overdose and its management. British Journal of Clinical Practice. 43(5): 184–186, 1989
Gomes JA, Winters SL, Ergin A, Machac J, Estioko M, et al. Clinical and electrophysiologic determinants, treatment and survival of patients with sustained malignant venntricular tachyarrhythmias occurring late after myocardial infarction. Journal of the American College of Cardiology 17(2): 320–326, 1991
Gosselink A, Crijns H, Van Gelder I, Lie K. Low dose amiodarone prophylaxis after electrical cardioversion of chronic atrial fibrillation or flutter. Abstract. European Heart Journal 11 (Suppl.): 6, 1990
Gottlieb S, Sonnenblick M. Effect of amiodarone on blood lipids. American Journal of Cardiology 63(20): 1540, 1989
Gotzsche LSB-H, Boye N, Laurberg P, Andreasen F. Rat heart thyroxine 5′-deiodinase is sensitively depressed by amiodarone. Journal of Cardiovascular Pharmacology 14(6): 836–841, 1989
Greco R, D’Alterio D, Schiattarella M, Musto B, Wolff S, et al. Intravenous amiodarone in acute anterior myocardial infarction: a controlled study. Cardiovascular Drugs and Therapy 2: 791–794, 1989
Greenberg ML, Lerman BB, Shipe JR. Kaiser DL; Dimarco JP. Relation between amiodarone and desethylamiodarone plasma concentrations and electrophysiologic effects, efficacy and toxicity. Journal of the American College of Cardiology 9(5): 1148–1155,1987
Greenberg ML, Lerman BB, Haines DE, Baron JA, DiMarco JP. Stability of electrophysiological parameters after acute amiodarone loading: implications for patient management. Pacing and Clinical Electrophysiology 12(1): 1038–1043, 1989
Greene HL. The efficacy of amiodarone in the treatment of ventricular tachycardia or ventricular fibrillation. Progress in Cardiovascular Diseases 31(5): 319–354, 1989
Gross SA, Bandyopadhyay S, Klaunig JE, Somani P. Amiodarone and desethylamiodarone toxicity in isolated hepatocytes in cultures (42844). Proceedings of the Society for Experimental Biology and Medicine 190: 163–169, 1989
Guccione P, Paul T, Garson Jr A. Long-term follow-up of amiodarone therapy in the young: Continued efficacy, unimpaired growth, moderate side effects. Journal of the American College of Cardiology 15(5): 1118–1124, 1990
Hamer A, Peter T, Mandel WJ, Scheinman MM, Weiss D. The potentiation of warfarin anticoagulation by amiodarone. Circulation 65: 1025–1029, 1982
Hamer AWF, Arkles LB, Johns JA. Beneficial effects of low dose amiodarone in patients with congestive cardiac failure: a pla- cebo-controlled trial. Journal of the American College of Cardiology 14(7): 1768–1774, 1989
Hansten PD, Horn JR. Amiodarone drug interactions. Drug In- teractions Newsletter 7(3): 13–16, 1987
Harris L, McKenna WJ, Rowland E, Krikler DM. Side effects and possible contraindications and amiodarone use. American Heart Journal 106: 916–923, 1983
Heger JJ. Monitoring and treating side effects of amiodarone therapy. Cardiovascular Reviews and Reports 9: 47–54, 1988
Helmy I, Herre JM, Gee G, Sharkey H, Malone P, et al. Use of intravenous amiodarone for emergency treatment of life- threatening ventricular arrhythmias. Journal of the American College of Cardiology 12(4): 1015–1022, 1988
Herre JM, Ross BA. Amiodarone in children: borrowing from the future? Journal of the American College of Cardiology 15(5): 1125–1126,1990
Herre JM, Sauve MJ, Malone P, Griffin JC, Helmy I, et al. Long- term results of amiodarone therapy in patients with recurrent sustained ventricular tachycardia or ventricular fibrillation. Journal of the American College of Cardiology 13(2): 442–449, 1989
Hockings BEF, George T, Mahrous F, Taylor RR, Hajar HA. Effectiveness of amiodarone on ventricular arrhythmias during and after acute myocardial infarction. American Journal of Cardiology 60(93): 967–970, 1987
Hoffmann A, Kappenberger L, Jost M, Burckhardt D. Effect of amiodarone on sinus node function in patients with sick sinus syndrome. Clinical Cardiology 10(8): 451–452, 1987
Hohnloser SH, Meinertz T, Dammbacher T, Steiert K, Jahnchen E, et al. Electrocardiographic and antiarrhythmic effects of intravenous amiodarone: results of a prospective, placebo-con- trolled study. American Heart Journal 121(1): 89–95, 1991
Holt AW. Hemodynamic responses to amiodarone in critically ill patients receiving catecholamine infusions. Critical Care Medicine 17(12): 1270–1276, 1989
Holt DW, Tucker GT, Jackson PR, Storey GCA. Amiodarone pharmacokinetics. American Heart Journal 106(4): 840–847, 1983
Hoogma RPLM, Heide Dvd. Amiodarone and thyroid function. Netherlands Journal of Medicine 36: 209–216, 1990
Horowitz LN, Borggrefe M. Many things are not found in books or journals … but some things are! Value of electrophysiologic testing in patients with malignant ventricular arrhythmias. American Journal of Cardiology 62(17): 1282–1294, 1988
Ibsen HHW, Frandsen F, Brandrup F, Moller M. Epididymitis caused by treatment with amiodarone. Genitourinary Medicine 65(4): 257–258, 1989
Impact Research Group. International mexiletine and placebo antiarrhythmic coronary trial: I. Report on arrhythmia and other findings. Journal of the American College of Cardiology 4(6): 1148–1163, 1984
Ingram DV, Jaggarao NSV, Chamberlain DA. Ocular changes resulting from therapy with amiodarone. British Journal of Ophthalmology 66: 676–679, 1982
Johnston A, Walker S, Robinson KC, McKenna WJ, Holt DW. The digoxin-amiodarone interaction. British Journal of Clinical Pharmacology 24(2): 253P, 1987
Jorens PG, Van Den Heuvel PA, Ranquin REF, Van Den Branden FA, Parizel GA. Amiodarone induced torsades de pointe. Report of three cases and review of literature. Acta Cardiologica 44(5): 411–421, 1989
Kadish AH, Buxton AE, Waxman HL, Flores B, Josephson ME, et al. Usefulness of electrophysiologic study to determine the clinical tolerance of arrhythmia recurrences during amiodarone therapy. Journal of the American College of Cardiology 10(1): 90–96, 1987
Kadish A, Morady F. The use of intravenous amiodarone in the acute therapy of life-threatening tachyarrhythmias. Progress in Cardiovascular Diseases 31(4): 281–294, 1989
Kannan R, Nadamanee K, Hendrickson JA, Rostami HJ, Singh BN. Amiodarone kinetics after oral doses. Clinical Pharmacology and Therapeutics 31(4): 438–444, 1982
Kannan R, Yabek SM, Garson A, Miller S, McVey P, et al. Amiodarone efficacy in a young population: relationship to serum amiodarone and desethylamiodarone levels. American Heart Journal 114(2): 283–287, 1987
Kaplan LJ, Cappaert WE. Amiodarone keratopathy. Correlation to dosage and duration. Archives of Ophthalmology 100: 601–602, 1982
Karlson JA, Hopkins RW, Moran JM, Karlson KE. Long-term amiodarone administration protects against global myocardial ischemia. Annals of Thoracic Surgery: 50(4): 575–578, 1990
Kasim SE, Bugchi N, Brown TR, Khilnani S, Jackson K, et al. Amiodarone-induced changes in lipid metabolism. Hormone and Metabolic Research 22(7): 385–388, 1990
Kato R, Venkatesh N, Kamiya K, Yabek S, Kannan R, et al. Electrophysiologic effects of desethylamiodarone, an active metabolite of amiodarone: comparison with amiodarone during chronic administration in rabbits. American Heart Journal 115:351–359, 1988
Katritsis D, Camm AJ. Amiodarone in long term prophylaxis. Drugs 41 (Suppl. 3): 1–13, 1991
Kenny D. Amiodarone prophylaxis in hypertrophic obstructive cardiomyopathy. Lancet 1(8639): 671, 1989
Kennedy JI. Clinical aspects of amiodarone pulmonary toxicity. Clinics in Chest Medicine 11(1): 119–129, 1990
Kennedy RL, Griffiths H, Gray TA. Amiodarone and the thyroid. Clinical Chemistry 35(9): 1882–1887, 1989
Kerin NZ, Aragon E, Faitel K, Frumin H, Rubenfire M. Long- term efficacy and toxicity of high- and low-dose amiodarone regimens. Journal of Clinical Pharmacology 29(5): 418–423, 1989
Kerin NZ, Blevins RD, Goldman L, Faitel K, Rubenfire M. The incidence, magnitude, and time course of the amiodarone-war- farin interaction. Archives of Internal Medicine 148(8): 1779–1781, 1988
Kim SG, Felder SD, Figura I, Johnston DR, Waspe LE, et al. Comparison of programmed stimulation and holter monitoring for predicting long-term efficacy and inefficacy of amio- darone used alone or in combination with a class 1A antiar- rhythmic agent in patients with ventricular tachyarrhythmia. Journal of the American College of Cardiology 9(2): 398–404, 1987
Kirkah Z. Amiodarone-induced sterile epididymitis. Urologia In- ternationalis 43: 372–373, 1988
Kopelman HA, Horowitz LN. Efficacy and toxicity of amioda- rone for the treatment of supraventricular tachyarrhythmias. Progress in Cardiovascular Diseases 31(5): 355–366, 1989
Kreamer JW, Zevitz M, Somberg JC. The role of electrophysiol- ogic testing in the selection of amiodarone therapy. Journal of Clinical Pharmacology 29(5): 429–435, 1989
Kudenchuk PJ, Pierson DJ, Green HL, Graham EL, Sears GK, et al. Prospective evaluation of amiodarone pulmonary toxicity. Chest 86: 541–548, 1984
Kuhlman JE, Teigen C, Ren H, Hurban RH, Hutchins GM, et al. Amiodarone pulmonary toxicity: CT findings in symptomatic patients. Radiology 177: 121–125, 1990
Kusniec J, Sclarovsky S, Agmon J, Strasberg B, Rechavia E. Amiodarone-induced polymorphous ventricular tachycardia. Israel Journal of Medical Sciences 25(10): 585–586, 1989
Lakhdar A, Farish E, Dunn FG, Hillis WS. Amiodarone therapy, glucose tolerance and lipids — a prospective trial. European Heart Journal 9 (Suppl. 1): 4, 1988
Lalloz MRA, Byfield PGH, Greenwood RM. Binding of amiodarone by serum proteins and the effects of drugs, hormones and other interacting ligands. Journal of Pharmacy and Pharmacology 36: 366–372, 1984
Lazzara R. Amiodarone and torsade de pointes. Annals of Internal Medicine 111: 549–551, 1989
Leclercq J-F, Coumel P, Denjoy I, Maisonblanche P, Cauchemez B, et al. Long-term follow-up after sustained monomorphic ventricular tachycardia: causes, pump failure, and empiric antiarthythmic therapy that modify survival. American Heart JournaT 121: 1685–1692, 1991
Lesko LJ. Pharmacokinetic drug interactions with amiodarone. Clinical Pharmacokinetics 17(2): 130–140, 1989
Levick CE, Mizgala HF, Kerr CR. Failure to pace following high dose antiarrhythmic therapy. Reversal with isoproterenol. Pacing and Clinical Electrophysiology 7: 252–256, 1984
Levy S. The value of oral amiodarone in the treatment of ventricular arrhythmias in heart disease. Drugs 41 (Suppl. 2): 47–53, 1991
Lewis JH, Ranard RC, Caruso A, Jackson LK, Mullick F, et al. Amiodarone nepatotoxicity: prevalence and clinicopathologic correlations among 104 patients. Hepatology 9(5): 679–685, 1989
Magro SA, Lawrence EC, Wheeler SH, Krafcheck J, Lin HT, et al. Amiodarone pulmonary toxicity: prospective evaluation of serial pulmonary function tests. Journal of the American College of Cardiology 12: 781–788, 1988
Maling T. Amiodarone therapeutic plasma concentration monitoring: is it practical? Clinical Pharmacokinetics 14: 321–324, 1988
Manolis AS, Uricchio F, Estes NAM. Prognostic value of early electrophysiologic studies for ventricular tachycardia recurrence in patients with coronary artery disease treated with amiodarone. American Journal of Cardiology 63(15): 1052–1057, 1989
Manz M, Gembruch U, Nitsch J, Hansmann M, Lüderitz B. Treatment of supraventricular tachycardia in fetus with severe hydrops: amiodarone applied intravascularly. Abstract. European Heart Journal 11 (Suppl.): 275, 1990
Marchlinski FE. Amiodarone: therapeutic but toxic. New York State Journal of Medicine 87(6): 322–324, 1987
Marinchak RA, O’Connor KM, Friehling TD, Kowey PR. Acute electrophysiologic effects and antiarrhythmic/antifibrillatory activity of intravenous amiodarone in a chronic feline infarction model. Journal of Cardiovascular Pharmacology 14(3): 389–395, 1989
Martin WJ, Rosenow EC. Amiodarone pulmonary toxicity. Recognition and pathogenesis (part 1). Chest 93(5): 1067–1075, 1988
Martino E, Aghini-Lombardt F, Mariotti S, Bartalena L, Braverman L, et al. Amiodarone: A common source of iodine-induced thyrotoxicosis. Hormone Research 26(4): 158–171, 1987
Mas IJ, Massumi A, Harlan M, Seger JJ, Hall RJ. Electrophy- siologic testing: predictive of amiodarone efficacy in recurrent sustained ventricular tachycardia? Texas Heart Institute Journal 14: 382–388, 1987
Mason JW. Drug therapy: amiodarone. New England Journal of Medicine 316(8): 455–466, 1987
Mason JW. Prediction of amiodarone-induced pulmonary toxicity. American Journal of Medicine 86(1): 2–3, 1989
Mason JW, Hondeghem LM, Katzung BG. Block of inactivated sodium channels and of depolarisation-induced automaticity in guinea-pig papillary muscle by amiodarone. Circulation Research 55: 277–285, 1984
Massacci E, de Pieri g, Morellini MC, Longobardi M, Chioffi M, et al. The pharmacologic control with flecainide or amiodarone in the idiopathic paroxysmal atrial fibrillation. Abstract. European Heart Journal 11 (Suppl.): 6, 1990
Mattioni TA, Zheutlin TA, Dunnington C, Kehoe RF. The proarrhythmic effects of amiodarone. Progress in Cardiovascular Diseases 31(6): 439–446, 1989a
Mattioni TA, Zheutlin TA, Sarmiento JJ, Parker M, Lesch M, et al. Amiodarone in patients with previous drug-mediated tor-sade de pointes. Long term safety and efficacy. Annals of Internal Medicine 111(7): 574–580, 1989b
McAlister HF, Luke RA, Whitlock RM, Smith WM. Intravenous amiodarone bolus versus oral quinidine for atrial flutter and fibrillation after cardiac operations. Journal of Thoracic and Cardiovascular Surgery 99: 911–918, 1990
McCollam PL, Parker RB, Beckman KJ, Hariman RJ, Bauman JL. Proarrhythmia: A paradoxic response to antiarrhythmic agents. Pharmacotherapy 9(3): 144–153, 1989
McKenna WJ, Adams KM, Poloniecki JD, Dickie S, Oakley CM, et al. Long term survival with amiodarone in patients with hypertrophic cardiomyopathy and ventricular tachycardia. British Heart Journal 61(5): 472, 1989
McKenna WJ, England D, Harris L, Oakley C, Krikler DM, et al. Arrhythmia in hypertrophic cardiomyopathy: treatment with amiodarone. Abstract. Circulation 64(2): IV–25, 1981
Meinertz T, Hofmann T, Zehender M. Can we predict sudden cardiac death? Drugs 41 (Suppl. 2): 9–15, 1991
Melmed S, Nademanee K, Reed AW, Hendrickson JA, Singh BN, et al. Hyperthyroxinemia with bradycardia and normal thy- rotropin secretion after chronic amiodarone administration. Journal of Clinical Endocrinology and Metabolism 53(5): 997–1001, 1981
Menius JA, Cummings RG, Muhlbaier LH, Smith LR, Lowe JE. Effects of amiodarone on myocardial energy metabolism during ischemia. Abstract. Circulation 82 (Suppl. 4): III–145, 1990
Mitchell LB, Wyse G, Gillis AM, Duff HJ. Electropharmacology of amiodarone therapy initiation. Time courses of onset of electrophysiologic and antiarrhythmic effects. Circulation 80: 34–42, 1989
Mooss AN, Mohiuddin SM, Hee TT, Esterbrooks DJ, Hilleman DE, et al. Efficacy and tolerance of high-dose intravenous amiodarone for recurrent, refractory ventricular tachycardia. American Journal of Cardiology 65: 609–614, 1990
Morady F, DiCarlo LA, Krol RB, Baerman JM, de Buitleir M. Acute and chronic effects of amiodarone on ventricular refractoriness, intraventricular conduction and ventricular tachycardia induction. Journal of the American College of Cardiology 7(1): 148–157, 1986
Mostow ND, Rakita L, Vrobel TR, Noon D, Blumer J. Amiodarone: intravenous loading for rapid suppression of complex ventricular arrhythmias. Journal of the American College of Cardiology 4: 97–104, 1984
Mostow ND, Vrobel TR, Noon D, Rakita L. Rapid control of refractory atrial tachyarrhythmias with high-dose oral amiodarone. American Heart Journal 120(6): 1356–1363, 1990
Munoz A, Karila P, Gallay P, Zettelmeier F, Messner P, et al. A randomized hemodynamic comparison of intravenous amio- darone with and without Tween. 80. European Heart Journal 9: 142–148, 1988
Murphy JAM, Fitzsimons BM, Meute MA, Wilkinson WC, Luck JC, et al. Amiodarone: a postmarketing evaluation of moni- toring for drug-induced toxicity. Drug Intelligence and Clinical Pharmacy 24(10): 1001–1006, 1990
Myers M, Peter T, Weiss D, Nalos PC, Gang ES, et al. Benefit and risks of long-term amiodarone therapy for sustained ventricular tachycardia/fibrillation: minimum of three-year follow-up in 145 patients. American Heart Journal 119(1): 8–14, 1990
Naccarelli GV, Rinkenberger RL, Dougherty AG, Fitzgerald DM. Adverse effects of amiodarone, pathogenesis, incidence and management. Medical Toxicology and Adverse Drug Experience: 4(4): 246–253, 1989
Naccarelli GV, Rinkenberger RL, Dougherty AH, Giebel RA. Amiodarone: pharmacology and antiarrhythmic and adverse effects. Pharmacotherapy 5: 298–313, 1985
Nademanee K, Hendrickson J, Kannan R, Singh BN. Antiarrhythmic efficacy and electrophysiologic actions of amioda- rone in patients with life-threatening ventricular arrhythmias: potent suppression of spontaneously occurring tachyarrhyth- mias versus inconsistent abolition of induced ventricular tachycardia. American Heart Journal 103(6): 950–959, 1982a
Nademanee K, Kannan R, Hendrickson J, Burnam M, Kay I, et al. Amiodarone-digoxin interaction during treatment of resistant cardiac arrhythmias. Abstract. American Journal of Cardiology 49(2): 1026, 1982b
Nademanee K, Piwonka RW, Singh BN, Hershman JM. Amio- darone and thyroid function. Progress in Cardiovascular Diseases 31(6): 427–437, 1989
Nademanee K, Singh BN, Cannom DS, Weiss J, Feld G, et al. Control of sudden recurrent arrhythmic deaths: role of amio- darone. American Heart Journal 106(4): 895–901, 1983b
Nademanee K, Singh BN, Hendrickson J, Intarachot V, Lopez B. Amiodarone in refractory life-threatening ventricular arrhyth- mias. Annals of Internal Medicine 98(5): 577–584, 1983a
Nattel S. Pharmacodynamic studies of amiodarone and its active N-desethyl metabolite. Journal of Cardiovascular Pharmacology 8: 771–777, 1986
Nattel S. Antiarrhythmic drug classifications: a critical appraisal of their history, present status and clinical relevance. Drugs 41: 672–701, 1991
Nattel S, Davies M, Quantz M. The antiarrhythmic efficacy of amiodarone and desethylamiodarone, alone and in combination, in dogs with acute myocardial infarction. Circulation 77: 200–208, 1988
Nattel S, Talajic M. Recent advances in understanding the pharmacology of amiodarone. Drugs 36: 121–131, 1988
Nattel S, Talajic M, Quantz M, DeRoode M. Frequency-depend- ent effects of amiodarone on atrioventricular nodal function and slow channel action potentials: evidence for calcium chan- nel-blocking activity. Circulation 76: 442–449, 1987
Neri R, Mestroni L, Salvi A, Pandullo C, Camerini F. Ventricular arrhythmias in dilated cardiomyopathy: Efficacy of amioda- rone. American Heart Journal 113(3): 707–715, 1987
Nicolet-Chatelain G, Prevost M-C, Escamilla R, Migueres J. Amiodarone-induced pulmonary toxicity. Immunoallergologic tests and bronchoalveolar lavage phospholipid content. Chest 99(2): 363–369, 1991
Nishimura M, Follmer CH, Singer DH. Amiodarone blocks calcium current in single guinea pig ventricular myocytes. Journal of Pharmacology and Experimental Therapeutics 251(2): 650–659, 1989
Nitsch J, Luderitz B. Enhanced elimination of amiodarone by cholestyramine. Deutsche Medizinische Wochenschrift 111: 1241–1244, 1986
Noc M, Stajer D, Horvat M. Intravenous amiodarone versus verapamil for acute conversion of paroxysmal atrial fibrillation to sinus rhythm. American Journal of Cardiology 65(9): 679–680, 1990
Nokin P, Jungbluth L, Mouton J. Protective effects of amiodarone pretreatment on mitochondrial function and high energy phosphates in ischaemic rat heart. Journal of Molecular and Cellular Cardiology 19: 603–614, 1987a
Nokin P, Mercadier J-J, Nahum D, Bouveret P, Wisnewsky C, et al. Effect of amiodarone on myosin isoenzymic distribution in rat ventricular myocardium. European Journal of Pharmacology 138: 277–280, 1987b
Ochi RP, Goldenberg IF, Almquist A, Pritzker M, Milstein S, et al. Intravenous amiodarone for the rapid treatment of life- threatening ventricular arrhythmias in critically ill patients with coronary artery disease. American Journal of Cardiology 64: 599–603, 1989
Ogle CL, Reasor MJ. Response of alveolar macrophages to amio- darone and desethylamiodarone, in vitro. Toxicology 62: 227–238, 1990
Ohar JA, Jackson F, Redd RM, Evans GR, Bedrossian CW. Use- fulness of serial pulmonary function testing as an indicator of amiodarone toxicity. American Journal of Cardiology 64: 1322–1326, 1989
Olson PJ, Woelfel AK, Simpson RJ, Foster JR. Do any patients treated with amiodarone for sustained ventricular tachycardia/ ventricular fibrillation have an acceptably low risk of sudden death? Abstract. Circulation 82 (Suppl. 4): 111–83, 1990
O’Reilly RA, Trager WF, Rettie AE, Goulart DA. Interaction of amiodarone with racemic warfarin and its separated enantiom- orphs in humans. Clinical Pharmacology and Therapeutics 42(3): 290–294, 1987
Ou C-N, Rognerud CL, Duong LT, Frawket VL. Liquid-chromatographic determination of amiodarone and N-desethylamiodarone in serum. Clinical Chemistry 36(3): 532–534, 1990
Paczkowski D, Poplawska W, Filipek M, Podlesny J. Determination of amiodarone and its metabolite desethylamiodarone in human plasma and serum. Polish Journal of Pharmacology and Pharmacy 41: 359–367, 1989
Pallandi RT, Campbell TJ. Resting, and rate-dependent depression of.Vmax of guinea-pig ventricular action potentials by amiodarone and desethylamiodarone. British Journal of Pharmacology 92(1): 97–103, 1987
Paton DM, Webster DR, Neutze JM. A review of the clinical pharmacokinetics of amiodarone. Methods and Findings in Experimental and Clinical Pharmacology 6(1): 41–49, 1984
Patterson E, Eller BT, Abrams GD, Vasiliades J, Lucchesi BR. Ventricular fibrillation in a conscious canine preparation of sudden coronary death — prevention by short- and long-term amiodarone administration. Circulation 68(4): 857–864, 1983
Perkins MW, Dasta JF, Reilley TE, Halpern P. Intraoperative complications in patients receiving amiodarone: characteristics and risk factors. Drug Intelligence and Clinical Pharmacy 23(10): 757–763, 1989
Perticone F, Cuda G, Spadea F, Pintaudi C, Tropea R. Malignant ventricular arrhythmia in the Wolff-Parkinson-White syndrome during amiodarone treatment. Clinical Cardiology 10(8): 477–480, 1987
Peter T, Hamer A, Mandel WJ, Weiss D. Evaluation of amiodarone therapy in the treatment of drug-resistant cardiac arrhythmias: long-term follow-up. American Heart Journal 106(4): 943–950, 1983
Peter TM, Hamer A, Weiss D, Mandel WJ. Prognosis after sud- den cardiac death without associated myocardial infarction: one year follow-up of empiric therapy with amiodarone. American Heart Journal 107(2): 209–213, 1984
Pfeiffer A, Vidon N, Bovet M, Rongier M, Bernier J-J, et al. In-testinal absorption of amiodarone in man. Journal of Clinical Pharmacology 30: 615–620, 1990
Pfisterer M, Burkart F, Kiowski W. Protective effect of amiodarone after myocardial infarction in patients with complex arrhythmias and preserved but not impaired LV function. Abstract. Circulation 82 (Suppl. 4): 111–97, 1990
Pfisterer M, Burkart F, Müller-Brand J, Kiowski W. Important differences between short- and long-term hemodynamic effects of amiodarone in patients with chronic ischemic heart disease at rest and during ischemia-induced left ventricular dysfunction. Journal of the American College of Cardiology 5: 1205–1211, 1985
Pickoff AS, Singh S, Flinn CJ, Wolff GS, Gelband H. Use of amiodarone in the therapy of primary ventricular arrhythmias in children. Developmental Pharmacology and Therapeutics 6(2): 73–82, 1983
Pilati G, Lenzi T, Trisolino G, Cavazza M, Binetti N, et al. Amiodarone versus quinidine for conversion of recent onset atrial fibrillation to sinus rhythm. Current Therapeutic Research 49(1): 140–146, 1991
Piwowarska W, Sniezek-Maciejewska M. Clinical value of cordarone as an antiarrhythmic agent. Cor et Vasa 29(4): 269–277, 1987
Plomp TA, van Rossum JM, Robles de Medina EO, van Lier T, Maes RAA. Pharmacokinetics and body distribution of amiodarone in man. Arzneimittel-Forschung/Drug Research 34(1): 513–520, 1984
Poirier JM, Escoubet B, Jaillon P, Coumel Ph, Richard MO, et al. Amiodarone pharmacokinetics in coronary patients: differences between acute and one-month chronic dosing. European Journal of Drug Metabolism and Pharmacokinetics 13(1): 67–72, 1988
Pollak PT, Sharma AD, Carruthers SG. Elevation of serum total cholesterol and triglyceride levels during amiodarone therapy. American Journal of Cardiology 62(9): 562–565, 1988
Pourbaix S, Berger Y, Desager J-P, Pacco M, Harvengt C. Absolute bioavailability of amiodarone in normal subjects. Clinical Pharmacology and Therapeutics 37(2): 118–123, 1985
Primeau R, Agha A, Giorgi C, Shenasa M, Nadeau R. Long term efficacy and toxicity of amiodarone in the treatment of re- fractory cardiac arrhythmias. Canadian Journal of Cardiology 5(2): 98–104, 1989
Proclemer A, Facchin D, Fresco C, Bernardi G, Fontanelli A, et al. Contribute iallo studio delle aritmie ventricolari maligne nella fase subacuta e tardiva deH’infarto miocardico. Giornale Italiano di Cardiologia 20: 400–411, 1990
Prystowsky EN, Heger JJ, Miles WM, Zipes DP. Amiodarone treatment in patients with ventricular arrhythmias. Drugs 29 (Suppl. 3): 47–52, 1985
Puech P. Practical aspects of the use of amiodarone. Drugs 41 (Suppl. 2): 67–73, 1991
Quyyumi AA, Ormerod LP, Clarke SW, Evans TR, Ward RL. Pulmonary fibrosis-a serious side-effect of amiodarone therapy. European Heart Journal 4(7): 521–524, 1983
Rakita L, Sobol SM. Amiodarone in the treatment of refractory ventricular arrhythmias. Journal of the American Medical Association 250(10): 1293–1295, 1983
Rakita L, Sobol SM, Mostow N, Vrobel T. Amiodarone pulmonary toxicity. American Heart Journal 106(4): 906–916,1983
Rankin AC, Pringle SD, Cobbe SM. Acute treatment of torsades de pointes with amiodarone: Proarrhythmic and antiarrhythmic association of QT prolongation. American Heart Journal 119(1): 185–186, 1990
Rappersberger K, Hönigsmann H, Ortel B, Tanew A, Konrad K, et al. Photosensitivity and hyperpigmentation in amiodarone-treated patients: incidence, time course, and recovery. Journal of Investigative Dermatology 93(2): 201–209, 1989
Rasmussen K, Winkle R, Ross D, Griffin J, Peters F, et al. Antiarrhythmic efficacy of amiodarone in recurrent ventricular tachycardia evaluated by multiple electrophysiological and ambulatory ECG recordings. Acta Medica Scandinavica 212(6): 367–374, 1982
Reasor MJ, Ogle CL, Kacew S. Amiodarone-induced pulmonary toxicity in rats: biochemical and pharmacological characteristics. Toxicology and Applied Pharmacology 97: 124–133, 1989
Remme WJ, van Hoogenhuyze DCA. Hemodynamic profile of amiodarone during acute and long-term administration in patients with ventricular dysfunction. Cardioscience 1(3): 169–176, 1990
Remme WJ, van Hoogenhuyze DCA, Kruyssen DACM, Krauss XH, Storm CJ. Amiodarone: haemodynamic profile during intravenous administration and effect on pacing-induced ischaemia in man. Drugs 29 (Suppl. 3): 11–22, 1985
Rey E, Bachrach LK, Burrow GN. Effects on amiodarone during pregnancy. Canadian Medical Association Journal 136(9): 959–960, 1987
Riva E, Hearse DJ. Anti-arrythmic effects of amiodarone and desethylamiodarone on malignant ventricular arrythmias arising as a consequence of ischaemia and reperfusion in the anaesthetised rat. Cardiovascular Research 23: 331–339, 1989
Riva E, Marchi S, Pesenti A, Bizzi A, Cini M, et al. Amiodarone induced phospholipidosis: Biochemical, morphological and functional changes in the lungs of rats chronically treated with amiodarone. Biochemical Pharmacology 36(19): 3209–3214, 1987
Robinson K, Johnston A, Walker S, Mulrow JP, McKenna WJ, et al. The digoxin-amiodarone interaction. Cardiovascular Drugs and Therapy 3: 25–28, 1989b
Robinson K, Johnston A, Walker S, Mulrow J, Holt D, et al. Stability of plasma amiodarone levels during chronic oral therapy. Cardiovascular Drugs and Therapy 4(2): 529–530, 1990
Robinson KC, McKenna WJ, Krikler DM. Amiodarone: current perspectives from Europe. Heart and Lung 16(6): 636–639, 1987
Robinson K, Mulrow JP, Rowland E, McKenna WJ. Long-term effects of amiodarone on hepatic function. American Journal of Cardiology 64(1): 95–96, 1989a
Rochas MA, Caillard C, Coulais Y, Sqalli A, Houin G. High performance liquid chromatographic method for routine monitoring of amiodarone and desethylamiodarone plasma levels. Annales de Biologie Clinique 47: 135–137, 1989
Rosen MR, Wit AL. Electropharmacology of antiarrhythmic drugs. American Heart Journal 106: 829–839, 1983
Rosenbaum MB, Chiale PA, Haedo A, Lazzari JO, Elizari MV. Ten years of experience with amiodarone. American Heart Journal 106(4): 957–964, 1983
Rosenberg EM, Elbl F, Solinger RE, Palakurthy P, Rees AH. Neonatal refractory supraventricular tachycardia: Successful treatment with amiodarone. Southern Medical Journal 81(4): 539–540, 1988
Rosenfeld LE, Kennedy EE, Perlmutter RA, Bookbinder MJ, McPherson CA, et al. Dissociation of electrophysiologic and pharmacologic stability during an abbreviated oral loading regimen of amiodarone. American Heart Journal 114(6): 1367–1373, 1987
Rosenheck S, Sousa J, Calkins H, Schmaltz S, deBuitleir M, et al. Comparison of the results of electrophysiologic testing after short-term and long-term treatment with amiodarone in patients with ventricular tachycardia. American Heart Journal 121: 1693–1698, 1991
Rotmensch HH, Belhassen B. Amiodarone in the management of cardiac arrhythmias: current concepts. Medical Clinics of North America 72(2): 321–357, 1988
Rotmensch HH, Belhassen B, Swanson BN, Shoshani D, Spielman SR, et al. Steady-state serum amiodarone concentrations: relationships with antiarrhythmic efficacy and toxicity. Annals of Internal Medicine 101: 462–469, 1984
Rotmensch HH, Swanson BN, Greenspon AJ, Shoshani D, Greenspan AM. Amiodarone: individualizing dosage with serum concentrations. Pace-Pacing and Clinical Electrophysiology 6(6): 1327–1335, 1983
Rowland E, McKenna W, Holt D, Harris L, Krikler D. Control of the ventricular response with oral amiodarone in patients with rapidly conducted atrial fibrillation complicating the Wolff-Parkinson-White syndrome. Abstract. Circulation 64(2): IV–317,1981
Rowland E, McKenna WJ, Krikler DM. Amiodarone for the conversion of established atrial fibrillation and flutter. British Journal of Clinical Practice 40 (Suppl. 44): 39–41, 1986
Royal Pharmaceutical Society of Great Britain. AntiArrhythmic Agents. In Reynolds JEF (Ed.) Martindale: the extra pharmacopoeia, 29th ed., The Pharmaceutical Press, London, 1989
Rumessen JJ. Hepatotoxicity of amiodarone. Acta Medica Scandinavica 219: 235–239, 1986
Rumolo R, Vitolo E, Tronci M, Massari D, Cavagnini F, et al. Alterations in thyroid function induced by chronic administration of amiodarone. Drugs under Experimental and Clinical Research 13(1): 29–35, 1987
Saal AK, Werner JA, Gross BW, Gorham DR, Graham EL, et al. Interaction of amiodarone with quinidine and procainamide. Circulation 66(4): 11–224, 1982
Safran M, Martino E, Aghini-Lombardi F, Bartalena L, Balzano S, et al. Effect of amiodarone on circulating antithyroid antibodies. British Medical Journal 297: 456–457, 1988
Salerno DM, Gillingham KJ, Berry DA, Hodges M. A comparison of antiarrhythmic drugs for the suppression of ventricular ectopic depolarizations: a meta-analysis. American Heart Journal 120(2): 340–353, 1990a
Salerno DM, Fifield J, Hodges M. Antiarrhythmic drug therapy for suppression of ventricular arrhythmia: experience with 122 patients treated for two years. Journal of Clinical Pharmacology 30(3): 226–234, 1990b
Sano T, Sugiyama S, Taki K, Hanaki Y, Shimada Y, et al. Effects of antiarrhythmic agents classified as class III group on ischaemia-induced myocardial damage in canine hearts. British Journal of Pharmacology 99(3): 577–581, 1990
Santostasi G, Fantin M, Maragno I, Gaion RM, Basadonna O, et al. Effects of amiodarone on oral and intravenous digoxin kinetics in healthy subjects. Journal of Cardiovascular Pharmacology 9: 385–390, 1987
Schmidt A, König W, Binner L, Mayer U, Stauch M. Efficacy and safety of intravenous amiodarone in acute refractory arrhythmias. Clinical Cardiology 11(7): 481–485, 1988
Schmidt G, Goedel-Meinen L, Jahns G, Linne R, Schaudig U, et al. Long term efficacy of class I antiarrhythmic agents and amiodarone in patients with malignant ventricular arrhythmias. Drugs 29 (Suppl. 3): 37–46, 1985
Schmitt C, Brachmann J, Waldecker B, Rizos I, Senges J, et al. Amiodarone in patients with recurrent sustained ventricular tachyarrhythmias: results of programmed electrical stimulation and long-term clinical outcome in chronic treatment. American Heart Journal 114(2): 279–283, 1987
Schützenberger W, Leisch F, Gmeiner R. Enhances accessory pathway conduction following intravenous amiodarone in atrial fibrillation. A case report. International Journal of Cardiology 16(1): 93–95, 1987
Schutzenberger W, Leisch F, Kerschner K, Harringer W, Herbinger W. Clinical efficacy of intravenous amiodarone in the short term treatment of recurrent sustained ventricular tachycardia and ventricular fibrillation. British Heart Journal 62: 367–371, 1989
Schwartz A, Shen E, Morady F, Gillespie K, Scheinman M, et al. Hemodynamic effects of intravenous amiodarone in patients with depressed left ventricular function and recurrent tachycardia. American Heart Journal 106: 848–856, 1983
Sclarovsky S, Lewin RF, Kracoff O, Strasberg B, Arditti A, et al. Amiodarone-induced polymorphous ventricular tachycardia. American Heart Journal 105: 6–12, 1983
Shahar E, Barzilay Z, Frand M, Feigl A. Amiodarone in control of sustained tachyarrhythmias in children with Wolff-Parkinson-White syndrome. Pediatrics 72(6): 813–816, 1983a
Shahar E, Barzilay Z, Shem-Tov AA, Shohet I, Frand M. Preexcitation syndrome in infants and children. Effect of digoxin, verapamil, and amiodarone. Archives of Disease in Childhood 58:207–211, 1983b
Shea P, Schechtman K, Lai R, Kim SS, Ruffy R. Amiodarone -flecainide interaction. Abstract. Journal of the American College of Cardiology 7(2): 93A, 1986
Sheinman BD, Evans T. Acceleration of ventricular rate by amio- darone in atrial fibrillation associated with the Wolff-Parkin- son-White syndrome. British Medical Journal 285: 999–1000, 1982
Sheldon RS, Mitchell LB, Duff HJ, Wyse DG, Manyari DE. Right and left ventricular function during chronic amiodarone therapy. American Journal of Cardiology 62(10): 736–740, 1988
Singh BN. When is QT prolongation antiarrhythmic and when is it proarrhythmic? American Journal of Cardiology 63: 867–869, 1989
Singh B. Advantages of beta blockers versus antiarrhythmic agents and calcium antagonists in secondary prevention after myocardial infarction. American Journal of Cardiology 66(9): 9C–20C, 1990
Singh BN. When is drug therapy warranted to prevent sudden cardiac death? Drugs 41 (Suppl. 2): 24–46, 1991
Singh BN, Nademanee K. Amiodarone and thyroid function: Clinical implications during antiarrhythmic therapy. American Heart Journal 106(4): 857–869, 1983
Singh BN, Nademanee K, Kannan R, Ikeda N. The clinical results of amiodarone in cardiac arrhythmias: Optimal dosing. Pace-Pacing and Clinical Electrophysiology 7(1): 109–124, 1984
Singh BN, Venkatesh N, Nademanee K, Josephson MA, Kannan R. The historical development, cellular electrophysiology and pharmacology of amiodarone. Progress in Cardiovascular Diseases 31(4): 249–280, 1989
Sloskey GE. Amiodarone: a unique antiarrhythmic agent. Clinical Pharmacy 2(4): 330–340, 1983
Smith WM. Lubbe WF, Whitlock RM, Mercer J, Rutherford JD, et al. Long-term tolerance of amiodarone treatment for cardiac arrhythmias. American Journal of Cardiology 57(15): 1288–1293, 1986
Somani P. Basic and clinical pharmacology of amiodarone: relationship of antiarrhythmic effects, dose and drug concentrations to intracellular inclusion bodies. Journal of Clinical Pharmacology 29(5): 405–412, 1989
Somani P, Bandyopadhyay S, KJaunig JE, Gross SA. Amioda- rone- and desethylamiodarone-induced myelinoid inclusion bodies and toxicity in cultured rat hepatocytes. Hepatology 11(1): 81–92, 1990
Staubli M. Side effects of amiodarone. Deutsche Medizinische Wochenshrift 115: 102–105, 1990
Storey GCA, Holt DW. High-performance liquid chromato- graphic measurement of amiodarone and desethylamiodarone in plasma or serum at the concentrations attained following a single 400mg dose. Journal of Chromatography 245: 377–380, 1982
Strasberg B. Intravenous amiodarone for conversion of atrial fibrillation to sinus rythm. American Journal of Cardiology 67(4): 325, 1990
Strasberg B, Kusniec J, Zlotikamien B, Mager A, Sclarovsky S. Long-term follow-up of postmyocardial infarction patients with ventricular tachycardia or ventricular fibrillation treated with amiodarone. The American Journal of Cardiology 66: 673–678, 1990
Strunge P, Fransden J, Andreasen F. Amiodarone during pregnancy. European Heart Journal 9: 106–109, 1988
Stanton MS, Prystowsky EN, Fineberg NS, Miles WM, Zipes DP, et al. Arrhythmogenic effects of antiarrhythmic drugs: a study of 506 patients treated for ventricular tachycardia for fibrillation. Journal of the American College of Cardiology 14: 209–215, 1989
Takanaka C, Singh BN. Barium-induced nondriven action potentials as a model of triggered potentials from early afterde-polarizations: significance of slow channel activity and differing effects of quinidine and amiodarone. Journal of the American College of Cardiology 15: 213–221, 1990
Talajic M, DeRoode MR, Nattel S. Comparative electrophysiologic effects of intravenous amiodarone and desethylamiodarone in dogs: evidence for clinically relevant activity of the metabolite. Circulation 75(1): 265–271, 1987
Talajic M, Nattel S, Davies M, McCans J. The class III effects of amiodarone depend on intact thyroid function. Abstract. Journal of the American College of Cardiology 11(2): 41 A, 1988
Tonet JL, Bernardeau C, Lechat Ph, Frank R, Touzet I, et al. Comparison between the efficacy of amiodarone and quinidine in the treatment of atrial cardiac arrhythmias. British Journal of Clinical Practice 40 (Suppl. 44): 42–48, 1986
Tonet J, Frank R, Fontaine G, Grosgogeat Y. Efficacy and safety of low doses of beta-blocker agents combined with amiodarone in refractory ventricular tachycardia. Pace-Pacing and Clinical Electrophysiology 11: 1984–1989, 1988
Tonet J, Frank R, Fontaine G, Grosgogeat Y. Efficacite de l’association de faibles doses de beta-bloquants a l’amiodarone dans le traitement des tachycardies ventriculaires réfractaires. Archives des Maladies du Coeur et des Vaisseaux 82(9): 1511–1517,1989
Touboul P, Atallah G, Kirkorian G. Effect of intravenous amiodarone in patients with intraventricular conduction disorders. European Heart Journal 3: 546–552, 1982
Tuzcu EM, Gilbo J, Masterson M, Maloney JD. The usefulness of amiodarone in management of refractory supraventricular tachyarrhythmias. Cleveland Clinic Journal of Medicine 56(3): 238–242, 1989
Urso R, Aarons L. Bioavailability of drugs with long elimination half-lives. European Journal of Clinical Pharmacology 25(5): 689–693, 1983
Vaitkus PT, Buxton AE, Josephson ME, Marchlinski FE. Cycle-length response of ventricular tachycardia associated with coronary artery disease to procainamide and amiodarone. American Journal of Cardiology 66(7): 710–714, 1990
Varró A, Bódi I, Rabloczky G. Antiarrhythmic effect of desethylamiodarone in conscious rats. Journal of Pharmacy and Pharmacology 39(6): 483–484, 1987
Varro A, Nakaya Y, Elharrar V, Surawicz B. The effects of amiodarone on repolarization and refractoriness of cardiac fibers. European Journal of Pharmacology 154(1): 11–18, 1988
Vazquez Blanco M, Milei J, Piñeiro DJ, Buceta JE, Dreyer MP. Long term-treatment of ventricular tachycardia in ambulatory patients with amiodarone. Acta Cardiologica 38(2): 125–132, 1983
Veltri EP, Griffith LSC, Platia EV, Guarnieri T, Reid PR. The use of ambulatory monitoring in the prognostic evaluation of patients with sustained ventricular tachycardia treated with amiodarone. Circulation 74(5): 1054–1060, 1986
Vitolo E, Tronci M, Larovere MT, Rumolo R, Morabito A. Amiodarone versus quinidine in the prophylaxis of atrial fibrillation. Acta Cardiologica 36(6): 431–444, 1981
Vozeh S, Schmidlin O. Important physicochemical and pharmacokinetic properties of individual drugs and drug classes. In Speight TM (Ed.) Avery’s drug treatment: principles and practice of clinical pharmacology and therapeutics, 3rd ed., ADIS Press, Auckland, 1987
Vrobel TR, Miller PE, Mostow ND, Rakita L. A general overview of amiodarone toxicity: Its prevention, detection and management. Progress in Cardiovascular Diseases 31(6): 393–426, 1989
Ward MJ, Routledge PA, Hutchings A, Morris JM. Association of seminal desethylamiodarone concentration and epididymitis with amiodarone treatment. British Medical Journal 296: 19–20, 1988
Waxman HL. The efficacy of amiodarone for ventricular arrhythmias cannot be predicted with clinical electrophysiological studies. International Journal of Cardiology 3(1): 76–80, 1983
Waxman HL, Groh WC, Marchlinski FE, Buxton AE, Sadowski LM, et al. Amiodarone for control of sustained ventricular tachyarrhythmia: clinical and electrophysiologic effects in 51 patients. American Journal of Cardiology 50(5): 1066–1074, 1982
Wellens HJJ, Brugada P, Abdollah H. Effect of amiodarone in paroxysmal supraventricular tachycardia with or without Wolff-Parkinson-White syndrome. American Heart Journal 106: 876–880, 1983
Wilson JS, Podrid PJ. Side effects from amiodarone. American Heart Journal 121(1): 158–171, 1991
Windle J, Prystowsky EN, Miles WM, Heger JJ. Pharmacokinetic and electrophysiologic interactions of amiodarone and procainamide. Clinical Pharmacology and Therapeutics 41(6): 603–610, 1987
Winslow E, Campbell JK, Barron E. Effects of amiodarone on cardiac electrophysiology and inducibility of arrythmias in chronically infarcted dogs: Late arrhythmias, haemodynamics, and sympatholytic actions. Journal of Cardiovascular Pharmacology 16(6): 896–904, 1990
Wynne J, Braunwald E. The cardiomyopathies and myocarditis. In Braunwald E, et al. (Eds) Harrison’s principles of internal medicine, 11th ed., McGraw-Hill Book Company, 1987
Yazaki Y, Haffajee CI, Gold RL, Bishop RL, Alpert JS. Electrophysiologic predictors of long-term clinical outcome with amiodarone for refractory ventricular tachycardia secondary to coronary artery disease. American Journal of Cardiology 60(4): 293–297, 1987
Zatuchni J. The treatment of atrial fibrillation. Clinical Therapeutics 10(5): 468–486, 1988
Zehender M, Meinertz T, Geibel A, Hofmann T, Hohnloser S. Sudden death in dilated cardiomyopathy. Conventional versus amiodarone treatment. Abstract. Journal of the American College of Cardiology 15(2): 33A, 1990
Zhu J, Haines DE, Lerman BB, Di Marco JP. Predictors of efficacy of amiodarone and characteristics of recurrence of arrhythmia in patients with sustained ventricular tachycardia and coronary artery disease. Circulation 76(4): 802–809, 1987
Zuanetti G, Latini R, Neilson JMM, Schwartz PJ, Ewing DJ. Heart rate variability in patients with ventricular arrhythmias: effect of antiarrhythmic drugs. Journal of the American College of Cardiology 17(3): 604–612, 1991
Author information
Authors and Affiliations
Additional information
Various sections of the manuscript reviewed by: B. Belhassen, Department of Cardiology, Tel Aviv Medical Center, Sackler Faculty of Medicine, Tel Aviv University, Tel Aviv, Israel; J.H.N. Bett, Director of Cardiology, The Prince Charles Hospital, Brisbane, Queensland, Australia; P. Brugada, Postgraduate School of Cardiology, O.L Vrouwziekenhuis, Aalst, Belgium; A.J. Camm, Department of Cardiological Sciences, St George’s Hospital Medical School, London, England; R.W.F. Campbell, Academic Department of Cardiology, Freeman Hospital, University of Newcastle Upon Tyne, Newcastle Upon Tyne, England; PJ. Counihan, Department of Cardiological Sciences, St George’s Hospital Medical School, London, England; D.C. Harrison, University of Cincinnati Medical Center, Cincinnati, Ohio, USA; H.A. Kopelman, Cardiac Electrophysiology, St Joseph’s Hospital of Atlanta, Atlanta, Georgia, USA; S Nattel, Institut de Cardiologie de Montréal, Montreal, Quebec, Canada; A. Pfeiffer, Department of Medicine, Stadt Krankenhaus München-Bogenhausen, Munich, Federal Republic of Germany; M.Pfisterer, Division of Cardiology, University Hospital Basel, Basel, Switzerland; PJ. Podrid, Section of Cardiology, The University Hospital, Boston University Medical Center, Boston, Massachusetts, USA; L. Rakita, Division of Cardiology, Cleveland Metropolitan General Hospital, Case Western Reserve University, Cleveland, Ohio, USA.
Rights and permissions
About this article
Cite this article
Gill, J., Heel, R.C. & Fitton, A. Amiodarone. Drugs 43, 69–110 (1992). https://doi.org/10.2165/00003495-199243010-00007
Published:
Issue Date:
DOI: https://doi.org/10.2165/00003495-199243010-00007