Summary
Synopsis
Chronic granulomatous disease is a group of rare x-linked or autosomal genetic disorders of the phagocytic NADPH oxidase system involved in host defence against various microorganisms. It is manifested by a common phenotype consisting of recurrent serious, life-threatening infection and granuloma formation. Following the finding that interferon gamma-1b (IFNγ-1b) can potentiate phagocyte activity in some other disease states as well as restoring defective phagocyte NADPH oxidase system activity in at least some patients with chronic granulomatous disease, a large-scale placebo-controlled trial was undertaken with IFNγ-1b in patients with chronic granulomatous disease.
Long term treatment with a therapeutic dosage of IFNγ-1b produced a significant reduction in the incidence of serious clinical events necessitating hospitalisation. The relative risk of serious infection and the number of days in hospital were each reduced by about two-thirds, and the mean duration of hospital stay by about one-third in those who did experience infection. The greatest therapeutic benefit was found in patients aged < 10 years, but all patients were improved regardless of age, sex, use of prophylactic antibiotics or genetic pattern of inheritance. The drug was well tolerated with the commonest adverse effects (e.g. fever, headache, chills, injection site erythema) usually being mild, transient, and relieved by symptomatic treatment.
IFNγ-1b therefore provides an effective and well tolerated therapy for patients with chronic granulomatous disease, offering an important clinical advance in the treatment of this rare genetic disorder by improving the prognosis of its serious and life-threatening infectious sequelae.
Pharmacodynamic Properties
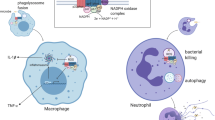
IFNγ-1b is an Escherichia coli-derived recombinant DNA product which has biological activity identical to natural human IFNγ. IFNγ possesses pleiotropic effects as a biological response modifier, but of specific relevance to chronic granulomatous disease, it has been shown in vitro and in vivo to increase the response of normal phagocytes with enhanced production of toxic oxygen metabolites via the NADPH oxidase pathway and by more efficient killing of various microorganisms. Indeed, chronic granulomatous disease is a heterogeneous group of x-linked and autosomal recessive disorders of the phagocytic NADPH oxidase system, which renders the host prone to recurrent severe infection that can be life-threatening. These patients also exhibit abnormal inflammatory responses that can induce granuloma formation.
However, preclinical in vitro and in vivo studies have not always revealed an enhancement of defective phagocyte function by IFNγ in cells derived from patients with chronic granulomatous disease: it was very frequent in those with x-linked disease but less common in those with autosomal recessive disease. Furthermore, despite the equal therapeutic benefit related to IFNγ-1b for both forms of the disease in the large-scale clinical trial of the drug, complementary ex vivo study of phagocytes revealed no change in superoxide production, bacterial killing or cytochrome b levels compared with placebo in either genetic form of the disease. The precise mechanism of action of interferon gamma in chronic granulomatous disease therefore requires further elucidation.
Pharmacokinetic Properties
Pharmacokinetic studies have been performed in healthy subjects but not in patients with chronic granulomatous disease. IFNγ-1b was rapidly cleared after intravenous injection of a single 100 μg/m2 dose (1.4 L/min), and was slowly absorbed after intramuscular or subcutaneous injection of the same dose (> 89% of the dose absorbed). Mean elimination half-lives were 0.6, 2.9 and 5.9 hours after intravenous, intramuscular and subcutaneous injection, respectively, while mean peak plasma concentration occurred at 4 hours (1.5 μg/L) and 7 hours (0.6 μg/L) after intramuscular and subcutaneous injection, respectively. No accumulation was evident after repeated once daily administration of IFNγ-1b 100 μg/m2 subcutaneously for 12 days. The drug is not detected in urine after parenteral administration to humans, and animal studies indicated clearance by the liver and kidneys.
Therapeutic Use
The clinical efficacy (and tolerability) of IFNγ-1b is essentially based on the results of a multicentre double-blind placebo-controlled parallel-group trial in 128 evaluable patients with x-linked or autosomal recessive chronic granulomatous disease. After randomisation and stratification patients received IFNγ-1b or placebo by subcutaneous injection 3 times weekly for up to 12 months. The dose was administered on the basis of body surface area if ⩾ 0.5m2 (50 μg/m2) and on the basis of bodyweight if < 0.5m2 (1.5 μg/kg). The mean duration of treatment was 8.9 months (equivalent to 95 patient-years).
Based on Kaplan-Meier plots, more patients receiving IFNγ-1b were free of serious infection at 12 months than were placebo recipients (77 vs 30%, p=0.0006). 14 of 63 patients receiving IFNγ-1b (22%) and 30 of 65 receiving placebo (46%) experienced at least 1 serious infection (p = 0.0006). The total number of infections was also significantly lower in the patients receiving IFNγ-1b (20 vs 56, p < 0.0001). Placebo recipients required about 3 times as many days of hospitalisation (1493 vs 497 days) and their mean hospital stay when infection did occur was longer (48 vs 32 days) compared with patients receiving IFNγ-1b.
IFNγ-1b conferred clinical benefit when subanalysis was performed for the main demographic and clinical factors used for stratification (age, pattern of inheritance, prophylactic antibiotic use and sex). While all patients benefited from therapy, patients aged < 10 years received the greatest benefit.
Clinical Tolerability
During the placebo-controlled trial of IFNγ-1b in patients with chronic granulomatous disease, adverse effects occurring at a significantly higher rate during active treatment (compared with placebo) included fever, headache, chills and erythema at the injection site. Most symptoms were mild and relieved by paracetamol (acetaminophen). There were fewer reactions with administration of IFNγ-1b at bedtime. Adverse effects occurred more frequently in those aged > 10 years compared with < 10 years. Withdrawals because of toxicity were infrequent, and resulted most commonly from rash, flu-like symptoms and worsened granulomatous colitis. No laboratory test abnormalities (including rheumatoid factor or antinuclear antibodies, ESR, thyroid function or sex hormone levels) or neutralising antibodies to IFNγ-1b were detected. Certain other adverse effects have been reported with the higher dosages of IFNγ-1b used in disease states other than chronic granulomatous disease.
Dosage and Administration
The recommended dosage of IFNγ-1b is 50 μg/m2 (1.5 × 106 U/m2) if body surface area is > 0.5m2, and 1.5 μg/kg if body surface is ⩽ 0.5m2, administered subcutaneously 3 times weekly. The dose should be halved or the drug withdrawn in the event of serious adverse reactions, and caution is required when treating patients with pre-existing cardiac or CNS disorders.
Similar content being viewed by others
References
Abo A, Pick E, Hall A, Totty N, Teaham C, et al. Activation of the NADPH oxidase involves the small GTP-binding protein p21rac1. Nature 353: 668–670, 1991
Badaro R, Falcoff E, Badaro FS, et al. Treatment of visceral leishmaniasis with pentavalent antimony and interferon gamma. New England Journal of Medicine 322: 16–21, 1990
Bernhisel-Broadbent J, Camargo EE, Jaffe HS, Lederman HM. Recombinant human interferon-γ as adjunct therapy for Aspergillus infection in a patient with chronic granulomatous disease. Journal of Infectious Diseases 163: 908–911, 1991
Billiau A, Dijkmans R. Interferon-γ: mechanism of action and therapeutic potential. Biochemical Pharmacology 40: 1433–1439, 1990
Bonnem EM, Oldham RK. Gamma-interferon: physiology and speculation on its role in medicine. Journal of Biological Response Modifiers 6: 275–301, 1987
Chen AB, Baker DL, Ferraiolo BL. Points to consider in correlating bioassays and immunoassays in the quantitation of peptides and proteins. In Garzone et al. (Eds) Peptides, peptoids, and proteins, pp. 54–71, Harvey Whitney Books, Cincinnati, Ohio, 1991
Chen SA, Izu AE, Baughman RA, Ferraiolo BL, Mordenti J, et al. Pharmacokinetic disposition of recombinant human interferon-gamma following intravenous, subcutaneous and intramuscular administration in normal, male volunteers. Abstract 116-17. Journal of Interferon Research 10: S125, 1990
Curnette JT. Classification of chronic granulomatous disease. Hematology/Oncology Clinics of North America 2: 241–253, 1988
Dinauer MC, Orkin SH. Molecular genetics of chronic granulomatous disease. Immunodeficiency Reviews 1: 5.5-69, 1988
Dijkmans R, Billiau A. Interferon: a master key in the immune system. Current Opinion in Immunology 1: 269–274, 1988
Dorenbaum A, Kline MW, Abramson SL, Hanson CG, Rosenblatt HM, et al. Osteomyelitis in a patient with chronic granulomatous disease following dose reduction of recombinant interferon gamma. Abstract 502. Journal of Allergy and Clinical Immunology 87: 265, 1991
Ezekowitz RAB, Newburger PE. New perspectives in chronic granulomatous disease. Journal of Clinical Immunology 8: 419–425, 1988
Ezekowitz RAB, Orkin SH, Newburger PE. Recombinant interferon gamma augments phagocyte superoxide production and x-chronic granulomatous disease gene expression in x-linked variant chronic granulomatous disease. Journal of Clinical Investigation 80: 1009–1016, 1987
Ezekowitz RAB, Dinauer MC, Jaffe HS, Orkin SH, Newburger PE. Partial correction of the phagocyte defect in patients with x-linked chronic granulomatous disease by subcutaneous interferon gamma. New England Journal of Medicine 319: 146–151, 1988
Ezekowitz RAB, Sieff CA, Dinauer MC, Nathan DG, Orkin SH, et al. Restoration of phagocyte function by interferon-γ in x-linked chronic granulomatous disease occurs at the level of a progenitor cell. Blood 76: 2443–2448, 1990
Gallin JI. Phagocytic cells: disorders of function, In Gallin et al. (Eds) Inflammation: basic principles and clinical correlates, pp. 493–512, Raven Press, New York, 1988
Gallin JI, Malech HL. Update on chronic granulomatous diseases of childhood. Journal of the American Medical Association 263: 1533–1537, 1990
Gallin JI, Buescher ES, Selgimann BE, et al. Recent advances in chronic granulomatous disease. Annals of Internal Medicine 99: 657–674, 1983
Izermans JNM, Marquet RL. Interferon-gamma: a review. Immunobiology 179: 456–473, 1989
International Chronic Granulomatous Disease Cooperative Study Group (ICGDCSG). A controlled trial of interferon gamma to prevent infection in chronic granulomatous disease. New England Journal of Medicine 324: 509–516, 1991
Johnston HC, Shigeoka AO, Hurley DC, Pysher TJ. Nocardia pneumonia in a neonate with chronic granulomatous disease. Pediatric Infectious Disease Journal 8: 526–528, 1989
Lomax KJ, Burch-Whitman C, Tiffany HC, et al. Analysis of chronic granulomatous disease kindreds reveals distinct genetic lesions affecting the same gene product. Clinical Research 36: 413, 1988
Mordenti J, Chen SA, Ferraiolo BL. Pharmacokinetics of interferon-gamma. In Kung et al. (Eds) Protein therapeutics: pharmacokinetics and pharmacodynamics, Stockton Press, New York, in press, 1992
Murray HW, Scavuzzo D, Jacobs JL, et al. In vitro and in vivo activation of human mononuclear phagocytes by gamma interferon: studies with normal and AIDS monocytes. Journal of Immunology 138: 2457–2462, 1987
Murray HW. Interferon-gamma, the activated macrophage, and host defense against microbial challenge. Annals of Internal Medicine 108: 595–608, 1988
Murray HW. Gamma interferon, cytokine-induced macrophage activation, and antimicrobial host defence. In vitro, in animal models, and in humans. Diagnostic Microbiology and Infectious Diseases 13: 411–421, 1990
Murray HW, Rubin BY, Rothermel CD. Killing of intracellular Leishmania donovani by lymphokine-stimulated human mononuclear phagocytes. Evidence that interferon-γ is the activating lymphokine. Journal of Clinical Investigation 72: 1506–1510, 1983
Murray HW, Rubin BY, Carriero SM, Harris AM, Jaffee EA. Human mononuclear phagocyte antiprotozoal mechanisms: oxygen-dependent vs oxygen-independent activity against intracellular Toxoplasma gondii. Journal of Immunology 134: 1983–1988, 1985
Nathan CF, Horowitz CR, de la Harpe J, et al. Administration of recombinant interferon to cancer patients enhances monocyte secretion of hydrogen peroxide. Proceedings of the National Academy of Sciences (USA) 82: 8686–8690, 1985
Nathan CF, Kaplan G, Levis WR, et al. Local and systemic effects of intradermal recombinant interferon-γ in patients with lepromatous leprosy. New England Journal of Medicine 315: 6–15, 1986
Newburger PE, Ezekowitz RAB. Cellular and molecular effects of recombinant interferon gamma in chronic and granulomatous disease. Hematology/Oncology Clinics of North America 2: 267–276, 1988
Newburger PE, Ezekowitz RAB, Whitney C, Wright J, Orkin SH. Induction of phagocyte cytochrome b heavy chain gene expression by interferon γ. Proceedings of the National Academy of Sciences (USA) 85: 5215–5219, 1988
Nunoi H, Rotrosen D, Gallin JI, Malech HL. Two forms of autosomal chronic granulomatous disease lack distinct neutrophil cytosol factors. Science 242: 1298–1301, 1988
Ockenhouse CF, Schulman S, Shear HL. Induction of crisis forms in the human malaria parasite Plasmodium falciparum by γ-interferon-activated, monocyte-derived macrophages. Journal of Immunology 133: 1601–1608, 1984
Ohno Y, Buescher ES, Roberts R, et al. Re-evaluation of cytochrome 6 and flavin adenine dinucleotide in neutrophils from patients with chronic granulomatous disease and description of a family with probable autosomal recessive inheritance of cytochrome b deficiency. Blood 67: 1132–1138, 1986
Orkin SH. X-linked chronic granulomatous disease: more than two years later. Molecular Biology and Medicine 6: 1–5, 1989
Perussia B, Kobayashi M, Rossi ME, Anegon I, Trinchieri G. Immune interferon enhances functional properties of human granulocytes: role of Fc receptors and effect of lymphotoxin, tumor necrosis factor and granulocyte-macrophage colonystimulating factor. Journal of Immunology 138: 765–774, 1987
Reed BR, Chen AB, Gibson UEM, Chen S, Baughman R, et al. Parenteral administration of recombinant interferon-gamma results in route-dependent processing in normal human subjects. Abstract 12-7. Journal of Interferon Research 10: S5, 1990
Rex JH, Bennett JE, Gallin JI, Malech HL, DeCarlo ES, et al. In vivo interferon-γ therapy augments the in vitro ability of chronic granulomatous disease neutrophils to damage Aspergillus hyphae. Journal of Infectious Diseases 163: 849–852, 1991
Rosenblatt HM, Smith W, Parikh N, Dombrowski M, Anderson DC. Effects of interferon-gamma (IFN-γ) on surface antigen expression in children with chronic granulomatous disease (CGD). Abstract 705. Journal of Allergy and Clinical Immunology 87: 316, 1991
Rothermel CD, Rubin BY, Jaffe EA, Murray HW. Oxygen-independent inhibition of intracellular Chlamydia psittaci growth by human monocytes and interferon-γ-activated macrophages. Journal of Immunology 137: 689–692, 1986
Sechler JMG, Malech HL, White CJ, Gallin JI. Recombinant human interferon-γ reconstitutes defective phagocyte function in patients with chronic granulomatous disease of childhood. Proceedings of the National Academy of Sciences (USA): 4874-4878, 1988
Segal AW. The electron transport chain of the microbicidal oxidase of phagocytic cells and its involvement in the molecular pathology of chronic granulomatous disease. Biochemical Society Transactions 17: 427–434, 1989
Segal AW, Cross AR, Garcia RC. Absence of cytochrome b-245 in chronic granulomatous disease: a multicenter European evaluation of its incidence and relevance. New England Journal of Medicine 308: 245–251, 1983
Volpp BD, Nauseef WM, Clark RA. Two cytosolic neutrophil oxidase components absent in autosomal chronic granulomatous disease. Science 242: 1295–1297, 1988
Weening RS, Adriannsz LH, Weemaes CMR, Lutter R, Roos D. Clinical differences in chronic granulomatous disease patients with cytochrome-b-negative neutrophils and patients with cytochrome-b-positive neutrophils. Journal of Pediatrics 107: 102–104, 1985
Weening RS, Verhoeven AJ, de Boer M, Roos D. Developments in the treatment of patients with chronic granulomatous disease. Acta Paediatrica Hungarica 29: 223–227, 1988
Zavala F, Veber F, Descamps-Latscha B. Altered expression of neutrophil peripheral benzodiazepine receptor in x-linked chronic granulomatous disease. Blood 76: 184–188, 1990a
Zavala F, Veber F, Taupin V, Nguyen AT, Descamps-Latscha B. Reconstitution of peripheral benzodiazepine receptor expression in x-linked chronic granulomatous disease by interferon-γ. Lancet 336: 758–759, 1990b
Author information
Authors and Affiliations
Additional information
Various sections of the manuscript reviewed by: G. Berton, Istituto di Patologia Generale, Universita degli Studi di Verona, Verona, Italy; L.A. Boxer, Department of Pediatrics, C.S. Mott Children’s Hospital, University of Michigan Hospitals, Ann Arbor, Michigan, USA; R. Dijkmans, SCK/CEN (VITO), Laboratory of Genetics and Biotechnology, Boeretang, Belgium; J. French, Department of Medicine, The Rayne Institute, University College and Middlesex School of Medicine, London, England; A. Kemp, Department of Microbiology and Infectious Diseases, Royal Children’s Hospital, Melbourne, Victoria, Australia; A. Mantovani, Istituto Di Ricerche Farmacologiche, Mario Negri Institute, Milan, Italy; H.W. Murray, Division of Infectious Diseases, The New York Hospital — Cornell Medical Center, New York, New York, USA; M. Takagi, Department of Pediatrics, Shinshu University School of Medicine, Matsumoto, Japan; R.S. Weening, Department of Pediatrics, Academic Medical Centre, University of Amsterdam, Amsterdam, The Netherlands.
An erratum to this article is available at http://dx.doi.org/10.1007/BF03257490.
Rights and permissions
About this article
Cite this article
Todd, P.A., Goa, K.L. Interferon Gamma-1b. Drugs 43, 111–122 (1992). https://doi.org/10.2165/00003495-199243010-00008
Published:
Issue Date:
DOI: https://doi.org/10.2165/00003495-199243010-00008