Abstract
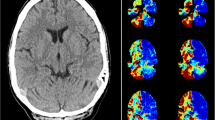
Chronic post-hypoxic myoclonus, also known as Lance-Adams syndrome (LAS), is a rare complication of successful cardiopulmanry resuscitation often accompanied by action myoclonus and cerebellar ataxia. It is seen in patients who have undergone a cardiorespiratory arrest, regained consciousness afterwards, and then developed myoclonus days or weeks after the event. Worldwide, 122 cases have been reported in the literature so far, including 1 case of Chinese. Here we report 2 Chinese LAS patients with detailed neuroimagings. Cranial single photon emission computed tomography (SPECT) of patient 1, a 52-year-old woman, showed a mild hypoperfusion in her left temporal lobe, whereas patient 2, a 54-year-old woman, manifested a mild bilateral decrease of glucose metabolism in the frontal lobes and a mild to moderate decrease of the N-acetyl aspartate (NAA) peak in the bilateral hippocampi by cranial [18F]-fluorodeoxyglucose positron emission tomographic (PET) scan and cranial magnetic resonance spectroscopy (MRS), respectively. We also review the literature on the neuroimaging, pathogenesis, and treatment of LAS.
Similar content being viewed by others
References
Crum, R.M., Anthony, J.C., Bassett, S.S., Folstein, M.F., 1993. Population-based norms for the Mini-Mental State Examination by age and educational level. JAMA, 269(18): 2386–2391. [doi:10.1001/jama.269.18.2386]
Dubinsky, R.M., Hallett, M., Di Chiro, G., Fulham, M., Schwankhaus, J., 1991. Increased glucose metabolism in the medulla of patients with palatal myoclonus. Neurology, 41(4):557–562.
Frucht, S., Fahn, S., 2000. The clinical spectrum of posthypoxic myoclonus. Mov. Disord., 15(Suppl. 1):2–7.
Frucht, S.J., Louis, E.D., Chuang, C., Fahn, S., 2001. A pilot tolerability and efficacy study of levetiracetam in patients with chronic myoclonus. Neurology, 57(6):1112–1114.
Frucht, S.J., Trost, M., Ma, Y., Eidelberg, D., 2004. The metabolic topography of posthypoxic myoclonus. Neurology, 62(10):1879–1881.
Guo, X.H., Yu, S.Y., Liu, J., Wu, W.P., Pu, C.Q., Zhu, K., 2002. Posthypoxic myoclonus treated with 5-hydroxytryptophan: a case report. J. Clin. Neurol., 15(5):313 (in Chinese).
Hallett, M., 2000. Physiology of human posthypoxic myoclonus. Mov. Disord., 15(Suppl. 1):8–13.
Jaw, S.P., Nguyen, B., Vuong, Q.T., Trinh, T.A., Nguyen, M., Truong, D.D., 1996. Effects of GABA uptake inhibitors on posthypoxic myoclonus in rats. Brain Res. Bull., 39(3):189–192. [doi:10.1016/0361-9230(95)02103-5]
Kimbrell, T.A., Ketter, T.A., George, M.S., Little, J.T., Benson, B.E., Willis, M.W., Herscovitch, P., Post, R.M., 2002. Regional cerebral glucose utilization in patients with a range of severities of unipolar depression. Biol. Psychiatry, 51(3):237–252. [doi:10.1016/S0006-3223(01)01216-1]
Kompoliti, K., Goetz, C.G., Vu, T.Q., Carvey, P.M., Leurgans, S., Raman, R., 2001. Estrogen supplementation in the posthypoxic myoclonus rat model. Clin. Neuropharmacol., 24(1):58–61. [doi:10.1097/00002826-200101000-00010]
Kowalczyk, E.E., Koszewicz, M.A., Budrewicz, S.P., Podemski, R., Slotwinski, K., 2006. Lance-Adams syndrome in patient with anoxic encephalopathy in the course of bronchial asthma. Wiad. Lek., 59(7–8):560–562 (in Polish).
Krauss, G.L., Bergin, A., Kramer, R.E., Cho, Y.W., Reich, S.G., 2001. Suppression of post-hypoxic and post-encephalitic myoclonus with levetiracetam. Neurology, 56(3):411–412.
Lance, J.W., Adams, R.D., 1963. The syndrome of intention or action myoclonus as a sequel to hypoxic encephalopathy. Brain, 86(1):111–136. [doi:10.1093/brain/86.1.111]
Lim, L.L., Ahmed, A., 2005. Limited efficacy of levetiracetam on myoclonus of different etiologies. Parkinsonism Relat. Disord., 11(2):135–137. [doi:10.1016/j.parkreldis.2004.07.010]
Matsumoto, R.R., Truong, D.D., Nguyen, K.D., Dang, A.T., Hoang, T.T., Vo, P.Q., Sandroni, P., 2000. Involvement of GABA (A) receptors in myoclonus. Mov. Disord., 15(Suppl. 1):47–52.
Polesin, A., Stern, M., 2006. Post-anoxic myoclonus: a case presentation and review of management in the rehabilitation setting. Brain Inj., 20(2):213–217. [doi:10.1080/02699050500442972]
Reed, L.J., Marsden, P., Lasserson, D., Sheldon, N., Lewis, P., Stanhope, N., Guinan, E., Kopelman, M.D., 1999. FDG-PET analysis and findings in amnesia resulting from hypoxia. Memory, 7(5–6):599–612. [doi:10.1080/096582199387779]
Videbech, P., 2000. PET measurements of brain glucose metabolism and blood flow in major depressive disorder: a critical review. Acta Psychiatr. Scand., 101(1):11–20. [doi:10.1034/j.1600-0447.2000.101001011.x]
Welsh, J.P., Placantonakis, D.G., Warsetsky, S.I., Marquez, R.G., Bernstein, L., Aicher, S.A., 2002a. The serotonin hypothesis of myoclonus from the perspective of neuronal rhythmicity. Adv. Neurol., 89:307–329.
Welsh, J.P., Yuen, G., Placantonakis, D.G., Vu, T.Q., Haiss, F., O’Hearn, E., Molliver, M.E., Aicher, S.A., 2002b. Why do Purkinje cells die so easily after global brain ischemia? Aldolase C, EAAT4, and the cerebellar contribution to posthypoxic myoclonus. Adv. Neurol., 89:331–359.
Werhahn, K.J., Brown, P., Thompson, P.D., Marsden, C.D., 1997. The clinical features and prognosis of chronic posthypoxic myoclonus. Mov. Disord., 12(2):216–220. [doi:10.1002/mds.870120212]
Author information
Authors and Affiliations
Corresponding author
Additional information
The two authors contributed equally to this work
Project supported by the National Natural Science Foundation of China (No. 30600193), the Youth Talent Special Fund of the Health Bureau of Zhejiang Province, China (No. 2004QN012), and the Health Bureau of Zhejiang Province, China (Nos. 2000A114 and 2007A100)
Rights and permissions
About this article
Cite this article
Zhang, Yx., Liu, Jr., Jiang, B. et al. Lance-adams syndrome: a report of two cases. J. Zhejiang Univ. - Sci. B 8, 715–720 (2007). https://doi.org/10.1631/jzus.2007.B0715
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1631/jzus.2007.B0715
Key words
- Lance-Adams syndrome
- Chronic post-hypoxic myoclonus
- Action myoclonus
- Cerebellar ataxia
- Single photon emission computed tomography
- Positron emission tomography
- Magnetic resonance spectroscopy