Purpose
Sacral resection is a potentially curative procedure for patients with sacral tumours,
both malignant tumours and aggressive benign neoplasms.
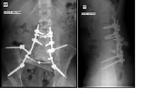
Lumbo-pelvic fixation is performed to restore axial and pelvic stability where resection involves more than 50% of the sacroiliac joint,
usually with a combination of metalwork and fibular strut grafts.
(1,
2) An example of this construct is shown in Figure 1.
Lumbo-pelvic stabilisation is technically challenging due to the high mechanical demand in this region.
Although 24 cases of this surgery have been reported in...
Methods and Materials
We performed a retrospective review of our orthopaedic oncology database in order to identify all patients with sacral neoplasia who had undergone total or partial sacrectomy requiring lumbo-pelvic reconstruction.
Postoperative imaging was jointly assessed by two experienced musculoskeletal radiologists,
with consensus decision when there was a difference in interpretation.
MR imaging was performed on a 1.0 Tesla MR scanner and CT imaging was performed on a 4 slice scanner.
Standard radiographic projections of the lumbar spine and pelvis were obtained as clinically indicated.
The size...
Results
We identified 7 patients who had undergone sacral resection of a tumour involving the proximal sacrum,
with lumbo-pelvic reconstruction.
All patients were seen and treated after 2004.
The patient details and tumour types are shown in figure 2.
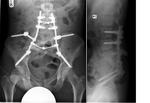
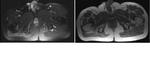
Mean tumour size on preoperative imaging was 10.7cm maximum diameter (range 6-16cm).
5 patients underwent total sacrectomy and 2 partial sacrectomy involving proximal sacrum and sacroiliac joint.
6 patients demonstrated adequate resection margins on histopathological examination,
although resection was deemed marginal for patient 4.
Postoperative follow up...
Conclusion
This procedure carries a high rate of complications including postoperative infection,
metalwork and graft failure and disease recurrence.
Sacral surgery carries a particularly high rate of infection,
attributed to the number of surgeons carrying out each operation,
the large surgical exposure and long duration of surgery as well as the proximity to bowel.
(3) Rod fracture has only been described in two cases in the literature,
although considerably more common in our series.
(4,
5)
Non-union of strut graft/ bone interface was also common occurrence...
References
1. Gokaslan ZL,
Romsdahl MM,
Kroll SS,
Walsh GL,
Gillis TA,
Wildrick DM,
et al.
Total sacrectomy and Galveston L-rod reconstruction for malignant neoplasms.
Technical note.
J Neurosurg.
1997 Nov;87(5):781-7.
2. Zhang ZY,
Fu CF,
Yang YX,
Wang LQ,
Cui Y,
Liu Y.
Long-term outcomes following en bloc resection for sacral tumor: a retrospective analysis of 93 cases.
Orthopedics. Aug;34(8):e403-7.
3. Sciubba DM,
Nelson C,
Gok B,
McGirt MJ,
McLoughlin GS,
Noggle JC,
et al.
Evaluation of factors associated with postoperative infection following sacral tumor...
Personal Information
M.
Thomas1,
A.M.
Davies1,
A.J.
Stirling2,
R.J.
Grimer3,
M.
Grainger2,
S.
L.
J.
James1
1 Department of Radiology,
The Royal Orthopaedic Hospital NHS Foundation Trust,Bristol Road South,Northfield,Birmingham,B31 2AP
2 Department of Spinal Surgery,
The Royal Orthopaedic Hospital NHS Foundation Trust,Bristol Road South,Northfield,Birmingham,B31 2AP
3 Department of Orthopaedic Oncology,
The Royal Orthopaedic Hospital NHS Foundation Trust,Bristol Road South,Northfield,Birmingham,B31 2AP
CORRESPONDING AUTHOR: Marianna Thomas.
Email address:
[email protected]