Abstract
Introduction
Previous studies have suggested that the use of regional anesthesia can reduce recurrence risk after oncologic surgery. The purpose of this study was to assess the effect of epidural anesthesia on recurrence-free (RFS) and overall survival (OS) after hepatic resection for colorectal liver metastases (CLM).
Methods
After approval of the institutional review board, the records of all adult patients who underwent elective hepatic resection between January 2006 and October 2011 were retrospectively reviewed. Patients were categorized according to use of perioperative epidural analgesia versus intravenous analgesia. Univariate and multivariate analyses were performed to identify factors influencing RFS and OS.
Results
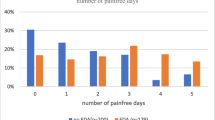
Of 510 total patients, 390 received epidural analgesia (EA group) and 120 patients received intravenous analgesia (IVA group). Compared with the IVA group, more patients in the EA group underwent associated surgical procedures with consequently longer operative times (p < 0.001). In addition, the EA group received more intraoperative fluids and had higher urine output volumes (p ≤ 0.001). Five-year RFS was longer in the EA group (34.7 %) compared with the IVA group (21.1 %). On multivariate analysis, the receipt of epidural analgesia was an independent predictor of improved RFS (p = 0.036, hazard ratio [HR] 0.74; 95 % confidence interval [CI] 0.56–0.95), but not OS (p = 0.102, HR 0.72; 95 % CI 0.49–1.07).
Conclusions
This study suggests an association between epidural analgesia and improved RFS, but not OS, after CLM resection. These results warrant further prospective, randomized studies on the benefits of regional anesthesia on oncologic outcomes after hepatic resection for CLM.


Similar content being viewed by others
References
Lau WY, Lai EC Hepatic resection for colorectal liver metastases. Singapore Med J. 2007;48(7):635–9.
Koshariya M, Jagad RB, Kawamoto J, et al. An update and our experience with metastatic liver disease. Hepatogastroenterology. 2007;54(80):2232–9.
Tavare AN, Perry NJ, Benzonana LL, et al. Cancer recurrence after surgery: direct and indirect effects of anesthetic agents. Int J Cancer. 2011;130(6)1237–50.
De Oliveira GS Jr, Schink JC, Buoy C, et al. The association between allogeneic perioperative blood transfusion on tumour recurrence and survival in patients with advanced ovarian cancer. Transfus Med. 2012;22(2):97–103.
Cata JP, Wang H, Gottumukkala V, et al. Inflammatory response, immunosuppression, and cancer recurrence after perioperative blood transfusions. Br J Anaesth. 2013;110(5):690–701.
Gottschalk A, Sharma S, Ford J, et al. Review article: the role of the perioperative period in recurrence after cancer surgery. Anesth Analg. 2010;110(6):1636–43.
Unic-Stojanovic D, Babic S, Jovic M Benefits, risks and complications of perioperative use of epidural anesthesia. Medicinski Arhiv. 2012;66(5):340–3.
Manion SC, Brennan TJ Thoracic epidural analgesia and acute pain management. Anesthesiology. 2011;115(1):181–8.
Liu SS, Wu CL Effect of postoperative analgesia on major postoperative complications: a systematic update of the evidence. Anesth Analg. 2007;104(3):689–702.
Rigg JR, Jamrozik K, Myles PS, et al. Epidural anaesthesia and analgesia and outcome of major surgery: a randomised trial. Lancet. 2002;359(9314):1276–82.
Capmas P, Billard V, Gouy S, et al. Impact of epidural analgesia on survival in patients undergoing complete cytoreductive surgery for ovarian cancer. Anticancer Res. 2012;32(4):1537–42.
Myles PS, Peyton P, Silbert B, et al. Perioperative epidural analgesia for major abdominal surgery for cancer and recurrence-free survival: randomised trial. BMJ. 2011;342:d1491.
Tsui BC, Rashiq S, Schopflocher D, et al. Epidural anesthesia and cancer recurrence rates after radical prostatectomy. Can J Anaesth. 2010;57(2):107–12.
Gottschalk A, Ford JG, Regelin CC, et al. Association between epidural analgesia and cancer recurrence after colorectal cancer surgery. Anesthesiology. 2010;113(1):27–34.
Chang SB, Palavecino M, Wray CJ, et al. Modified Makuuchi incision for foregut procedures. Arch Surg. 2010;145(3):281–4.
Strasberg SM. Nomenclature of hepatic anatomy and resections: a review of the Brisbane 2000 system. J Hepatobiliary Pancreat Surg. 2005;12(5):351–5.
Pang YY. The Brisbane 2000 terminology of liver anatomy and resections. HPB. 2000;2:333-39. HPB (Oxford). 2002;4(2):99; author reply 99–100.
Blazer DG, 3rd, Kishi Y, Maru DM, et al. Pathologic response to preoperative chemotherapy: a new outcome end point after resection of hepatic colorectal metastases. J Clin Oncol. 2008;26(33):5344–51.
Shindoh J, Loyer EM, Kopetz S, et al. Optimal morphologic response to preoperative chemotherapy: an alternate outcome end point before resection of hepatic colorectal metastases. J Clin Oncol. 2012;30(36):4566–72.
Brouquet A, Zimmitti G, Kopetz S, et al. Multicenter validation study of pathologic response and tumor thickness at the tumor-normal liver interface as independent predictors of disease-free survival after preoperative chemotherapy and surgery for colorectal liver metastases. Cancer. 2013;119(15):2778–88.
Dindo D, Demartines N, Clavien PA Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 2004;240(2):205–13.
Fong Y, Fortner J, Sun RL, et al. Clinical score for predicting recurrence after hepatic resection for metastatic colorectal cancer: analysis of 1001 consecutive cases. Ann Surg. 1999;230(3):309–18.
Are C, Gonen M, Zazzali K, et al. The impact of margins on outcome after hepatic resection for colorectal metastasis. Ann Surg 2007;246(2):295–300.
Sessler DI Does regional analgesia reduce the risk of cancer recurrence? A hypothesis. Eur J Cancer Prev. 2008;17(3):269–72.
Beilin B, Shavit Y, Trabekin E, et al. The effects of postoperative pain management on immune response to surgery. Anesth Analg. 2003;97(3):822–7.
Shavit Y, Lewis JW, Terman GW, et al. Opioid peptides mediate the suppressive effect of stress on natural killer cell cytotoxicity. Science. 1984;223(4632):188–90.
Singleton PA, Moss J Effect of perioperative opioids on cancer recurrence: a hypothesis. Future Oncol. 2010;6(8):1237–42.
Welden B, Gates G, Mallari R, Garrett N Effects of anesthetics and analgesics on natural killer cell activity. AANA J. 2009;77(4):287–92.
Afsharimani B, Cabot PJ, Parat MO Morphine use in cancer surgery. Front Pharmacol. 2011;2:46.
Warschkow R, Steffen T, Luthi A, et al. Epidural analgesia in open resection of colorectal cancer: is there a clinical benefit? a retrospective study on 1,470 patients. J Gastrointest Surg. 2011;15(8):1386–93.
Biki B, Mascha E, Moriarty DC, et al. Anesthetic technique for radical prostatectomy surgery affects cancer recurrence: a retrospective analysis. Anesthesiology. 2008;109(2):180–7.
Cummings KC 3rd, Xu F, Cummings LC, Cooper GS. A comparison of epidural analgesia and traditional pain management effects on survival and cancer recurrence after colectomy: a population-based study. Anesthesiology. 2012;116(4):797–806.
Gupta A, Bjornsson A, Fredriksson M, et al. Reduction in mortality after epidural anaesthesia and analgesia in patients undergoing rectal but not colonic cancer surgery: a retrospective analysis of data from 655 patients in central Sweden. Br J Anaesth. 2011;107(2):164–70.
Ismail H, Ho KM, Narayan K, Kondalsamy-Chennakesavan S. Effect of neuraxial anaesthesia on tumour progression in cervical cancer patients treated with brachytherapy: a retrospective cohort study. Br J Anaesth. 2010;105(2):145–9.
Wuethrich PY, Hsu Schmitz SF, Kessler TM, et al. Potential influence of the anesthetic technique used during open radical prostatectomy on prostate cancer-related outcome: a retrospective study. Anesthesiology. 2010;113(3):570–6.
Binczak M, Tournay E, Billard V, et al. Major abdominal surgery for cancer: does epidural analgesia have a long-term effect on recurrence-free and overall survival? Ann Fr Anesth Reanim. 2013;32(5):e81–8.
Holler JP, Ahlbrandt J, Burkhardt E, et al. Peridural analgesia may affect long-term survival in patients with colorectal cancer after surgery (PACO-RAS-Study): an analysis of a cancer registry. Ann Surg. 2013;258(6):989–93.
Acknowledgments
This research was supported in part by the National Institutes of Health through MD Anderson’s Cancer Center Support Grant, CA016672.
Disclosure
The authors report no conflicts of interest relevant to this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zimmitti, G., Soliz, J., Aloia, T.A. et al. Positive Impact of Epidural Analgesia on Oncologic Outcomes in Patients Undergoing Resection of Colorectal Liver Metastases. Ann Surg Oncol 23, 1003–1011 (2016). https://doi.org/10.1245/s10434-015-4933-1
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-015-4933-1