Abstract
Background
The risk of colorectal cancer (CRC) in chronic kidney disease (CKD) patients relative to the general population is unknown. The aim of this population-based study was to investigate the risk of CRC in patients with CKD.
Methods
The study cohort included patients aged ≥18 years diagnosed with CKD between 2004 and 2005 (n = 15,975). The comparison cohort (n = 79,875) included five randomly selected age- and gender-matched controls for each patient in the study cohort. All the subjects were followed up from the date of cohort entry until they developed CRC or until the end of 2006.
Results
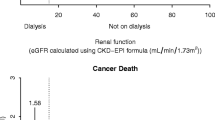
We identified 15,975 patients with a diagnosis of CKD who matched the inclusion criteria. A total of 460 patients developed CRC during the study period, of whom 116 were from the CKD cohort and 344 were from the comparison cohort. After adjusting for potential confounding factors, the CKD patients not undergoing dialysis were independently associated with a greater risk of CRC (hazard ratio, 1.79; 95 % confidence interval [CI] 1.41–2.27). The overall incidence rate of CRC was 341 per 100,000 person-years for CKD patients not undergoing dialysis, compared to 174 per 100,000 person-years. The age-matched hazard ratio of CRC after excluding dialysis patients was 1.64 (95 % CI 1.27–2.11) in patients 50 years and older, and 3.7 (95 % CI 1.83–7.49) in patients younger than 50 years.
Conclusions
This population-based cohort study indicated that CKD patients not requiring dialysis have an increased risk of CRC compared to the general population, independent of comorbidities.


Similar content being viewed by others
References
Levey AS, Coresh J. Chronic kidney disease. Lancet. 2012;379:165–80.
Zhang L, Wang F, Wang L, et al. Prevalence of chronic kidney disease in China: a cross-sectional survey. Lancet. 2012;379:815–22.
Siegel R, Ward E, Brawley O, Jemal A. Cancer statistics, the impact of eliminating socioeconomic and racial disparities on premature cancer deaths. CA Cancer J Clin. 2011;61:212–36.
Giovannucci E. Modifiable risk factors for colon cancer. Gastroenterol Clin North Am. 2002;31:925–43.
Schoen RE, Pinsky PF, Weissfeld JL, et al. Colorectal-cancer incidence and mortality with screening flexible sigmoidoscopy. N Engl J Med. 2012;366:2345–57.
National Health Insurance Research Database, Taiwan. http://www.nhri.org.tw/nhird/en/index.htm. Accessed 24 June 2013.
Quan H, Sundararajan V, Halfon P, et al. Coding algorithms for defining comorbidities in ICD-9-CM and ICD-10 administrative data. Med Care. 2005;43:1130–9.
Efron B, Tibshirani R. An introduction to the bootstrap. New York: Chapman & Hall; 1993.
Sauerbrei W. The use of resampling methods to simplify regression models in medical statistics. Appl Stat. 1999;48:313–29.
Lin HW, Tu YY, Lin SY, et al. Risk of ovarian cancer in women with pelvic inflammatory disease: a population-based study. Lancet Oncol. 2011;12:900–4.
Cunningham D, Atkin W, Lenz HJ, et al. Colorectal cancer. Lancet. 2010;375:1030–47.
Vamvakas S, Bahner U, Heidland A. Cancer in end-stage renal disease: potential factors involved (editorial). Am J Nephrol. 1998;18:89–95.
Iseki K, Osawa A, Fukiyama K. Evidence for increased cancer deaths in chronic dialysis patients. Am J Kidney Dis. 1993;22:308–13.
Lee S, Wasserberg N, Petrone P, et al. The prevalence of colorectal neoplasia in patients with end-stage renal disease: a case-control study. Int J Colorectal Dis. 2008;23:47–51.
Vajdic CM, McDonald SP, McCredie MR, et al. Cancer incidence before and after kidney transplantation. JAMA. 2006;296:2823–31.
Coresh J, Selvin E, Stevens LA, et al. Prevalence of chronic kidney disease in the United States. JAMA. 2007;298:2038–47.
Hu FB, Manson JE, Liu S, et al. Prospective study of adult onset diabetes mellitus (type 2) and risk of colorectal cancer in women. J Natl Cancer Inst. 1999;91:542–7.
Jee SH, Ohrr H, Sull JW, et al. Fasting serum glucose level and cancer risk in Korean men and women. JAMA. 2005;293:194–202.
Khaw KT, Wareham N, Bingham S, et al. Preliminary communication: glycated hemoglobin, diabetes, and incident colorectal cancer in men and women: a prospective analysis from the European prospective investigation into cancer—Norfolk study. Cancer Epidemiol Biomarkers Prev. 2004;13:915–9.
Larsson SC, Giovannucci E, Wolk A. Diabetes and colorectal cancer incidence in the cohort of Swedish men. Diabetes Care. 2005;28:1805–7.
Limburg PJ, Anderson KE, Johnson TW, et al. Diabetes mellitus and subsite-specific colorectal cancer risks in the Iowa Women’s Health Study. Cancer Epidemiol Biomarkers Prev. 2005;14:133–7.
Nilsen TI, Vatten LJ. Prospective study of colorectal cancer risk and physical activity, diabetes, blood glucose and BMI: exploring the hyperinsulinaemia hypothesis. Br J Cancer. 2001;84:417–22.
Schoen RE, Tangen CM, Kuller LH, et al. Increased blood glucose and insulin, body size, and incident colorectal cancer. J Natl Cancer Inst.1999;91:1147–54.
Steenland K, Nowlin S, Palu S. Cancer incidence in the National Health and Nutrition Survey I. Follow-up data: diabetes, cholesterol, pulse and physical activity. Cancer Epidemiol Biomarkers Prev. 1995;4:807–11.
Will JC, Galuska DA, Vinicor F, Calle EE. Colorectal cancer: another complication of diabetes mellitus? Am J Epidemiol. 1998;147:816–25.
Larsson SC, Orsini N, Wolk A. Diabetes mellitus and risk of colorectal cancer: a meta-analysis. J Natl Cancer Inst. 2005;97:1679–87.
Jarvinen HJ, Mecklin JP, Sistonen P. Screening reduces colorectal cancer rate in families with hereditary nonpolyposis colorectal cancer. Gastroenterology. 1995;108:1405–11.
Holley JL. Do dialysis patients need screening colonoscopies and mammograms? Semin Dial. 2011;24:364–5.
Winkelmayer WC, Schneeweiss S, Mogun H, et al. Identification of individuals with CKD from Medicare claims data: a validation study. Am J Kidney Dis. 2005;46:225–32.
Navaneethan SD, Jolly SE, Schold JD, et al. Development and validation of an electronic health record-based chronic kidney disease registry. Clin J Am Soc Nephrol. 2011;6:40–9.
Le Marchand L, Wilkens LR, Kolonel LN, Hankin JH, Lyu LC. Associations of sedentary lifestyle, obesity, smoking, alcohol use, and diabetes with the risk of colorectal cancer. Cancer Res. 1997;57:4787–94.
Levi F, Pasche C, Lucchini F, La Vecchia C. Diabetes mellitus, family history, and colorectal cancer. J Epidemiol Community Health. 2002;56:479–80.
Acknowledgment
This study is based in part on data from the National Health Insurance Research Database provided by the Bureau of National Health Insurance, Department of Health and managed by National Health Research Institutes and supported by the National Science Council of Taiwan under grant number 101-2118-M-031-001-MY2. The interpretation and conclusions contained herein do not represent those of Bureau of National Health Insurance, Department of Health or National Health Research Institutes.
Disclosure
The authors declare no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wu, MY., Chang, TC., Chao, TY. et al. Risk of Colorectal Cancer in Chronic Kidney Disease: A Matched Cohort Study Based on Administrative Data. Ann Surg Oncol 20, 3885–3891 (2013). https://doi.org/10.1245/s10434-013-3065-8
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-013-3065-8