Abstract
Background
Minimally invasive esophagectomy (MIE) may lead to early restoration of health-related quality of life, but few prospective comparative studies have been performed. This exploratory study compared recovery between totally minimally invasive esophagectomy (MIE), laparoscopically assisted esophagectomy (LAE) and open surgery (OE).
Methods
A prospective study in 2 specialist centers recruited consecutive patients undergoing OE, LAE, or MIE for high-grade dysplasia or cancer. Patients completed validated questionnaires, the Multi-Dimensional Fatigue Inventory (MFI-20), modified Katz Scale, and modified Lawton and Brody Scale (assessing activities of daily living) before and 6 weeks and 3 and 6 months after surgery.
Results
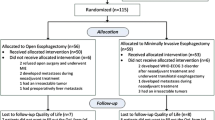
A total of 97 patients (26 women; median age 64 years) were scheduled for surgery that was abandoned in 11 due to occult low-volume metastatic disease. In the remaining 86 (OE = 19, LAE = 31, and MIE = 36), there were 4 in-hospital deaths (4 %), and 54 postoperative complications (OE = 12, LAE = 19, and MIE = 23). Overall questionnaire compliance was high (77 %) and baseline scores similar in all groups, although clinical differences between groups were observed with earlier tumors and more squamous cell cancers selected for MIE. Following surgery fatigue levels increased dramatically and activity levels reduced in all groups. These gradually recovered to baseline following MIE and LAE within 6 months, but the ability to perform activities of daily living and most parameters of fatigue had not returned to baseline levels in the OE group.
Conclusions
This exploratory prospective nonrandomized study of recovery after different types of surgery for esophageal cancer showed possible small benefits to MIE. A much larger study is needed to confirm these findings.


Similar content being viewed by others
References
The National Oesophago-Gastric Cancer Audit. http://www.augis.org/clinical_audits/clinical_audits_og_cancer.htm. Accessed 8 Jan 2013.
Luketich JD, Alvelo-Rivera M, Buenaventura PO, Christie NA, McCaughan JS, Litle VR, et al. Minimally invasive esophagectomy: outcomes in 222 patients. Ann Surg. 2003;238:486–94.
Smithers BM, Gotley DC, Martin I, Thomas JM. Comparison of the outcomes between open and minimally invasive esophagectomy. Ann Surg. 2007;245:232–40.
Nagpal K, Ahmed K, Vats A, Yakoub D, James D, Ashrafian H, et al. Is minimally invasive surgery beneficial in the management of esophageal cancer? A meta-analysis. Surg Endosc. 2010;24:1621–9.
Parameswaran R, Blazeby JM, Hughes R, Mitchell K, Berrisford RG, Wajed SA. Health-related quality of life after minimally invasive oesophagectomy. Br J Surg. 2010;97:525–31.
Wang H, Feng M, Tan L, Wang Q. Comparison of the short-term quality of life in patients with esophageal cancer after subtotal esophagectomy via video-assisted thoracoscopic or open surgery. Dis Esophagus. 2010;23:408–14.
Weeks JC, Nelson H, Gelber S, Sargent D, Schroeder G; Clinical Outcomes of Surgical Therapy (COST) Study Group. Short-term quality-of-life outcomes following laparoscopic-assisted colectomy vs open colectomy for colon cancer: a randomized trial. JAMA. 2002;287:321–8.
King PM, Blazeby JM, Ewings P, Longman RJ, Kipling RM, Franks PJ, et al. The influence of an Enhanced Recovery Programme on clinical outcomes, costs and quality of life after surgery for colorectal cancer. Colorectal Dis. 2006;8:506–13.
Guillou PJ, Quirke P, Thorpe H, Walker J, Jayne DG, Smith AM, et al. Short-term endpoints of conventional versus laparoscopic-assisted surgery in patients with colorectal cancer (MRC CLASICC trial): multicentre, randomised controlled trial. Lancet. 2005;365:1718–26.
Kleinbeck SV, Eells KR. Monitoring postdischarge ambulatory surgical recovery costs and outcomes. Surg Serv Manage. 1997;3:33–5.
Oberle K, Allen M, Lynkowski P. Follow-up of same day surgery patients. A study of patient concerns. AORN J. 1994;59:1016–5.
Zalon ML. Correlates of recovery among older adults after major abdominal surgery. Nurs Res. 2004;53:99–106.
Blazeby JM, Blencowe NS, Titcomb DR, Metcalfe C, Hollowood AD, Barham CP. Demonstration of the IDEAL recommendations for evaluating and reporting surgical innovation in minimally invasive oesophagectomy. Br J Surg. 2011;98:544–51.
Berrisford RG, Wajed SA, Sanders D, Rucklidge MW. Short-term outcomes following total minimally invasive oesophagectomy. Br J Surg. 2008;95:602–10.
Medical Research Council Oesophageal Cancer Working Group. Surgical resection with or without preoperative chemotherapy in oesophageal cancer. Lancet. 2002;359:1727–33.
Medical Research Council. A randomised controlled trial comparing standard chemotherapy followed by resection versus ECX chemotherapy followed by resection in patients with resectable adenocarcinoma of the oesophagus. ISRCTN01852072. 2005.
Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD, et al. The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg. 2009;250:187–96.
Katz S. Assessing self-maintenance: activities of daily living, mobility, and instrumental activities of daily living. J Am Geriatr Soc. 1983;31:721–7.
Lawton MP, Brody EM. Assessment of older people: self-maintaining and instrumental activities of daily living. Gerontologist. 1969;9:179–86.
Smets EM, Garssen B, Bonke B, De Haes JC. The Multidimensional Fatigue Inventory (MFI) psychometric qualities of an instrument to assess fatigue. J Psychosom Res. 1995;39:315–25.
Biere SS, van Berge Henegouwen MI, Maas KW, Bonavina L, Rosman C, Garcia JR, et al. Minimally invasive versus open oesophagectomy for patients with oesophageal cancer: a multicentre, open-label, randomised controlled trial. Lancet. 2012;379:1887–92.
Briez N, Piessen G, Bonnetain F, Brigand C, Carrere N, Collet D, et al. Open versus laparoscopically-assisted oesophagectomy for cancer: a multicentre randomised controlled phase III trial—the MIRO trial. BMC Cancer. 2011;11:310.
Donovan J, Mills N, Smith M, Brindle L, Jacoby A, Peters T, et al. Improving design and conduct of randomised trials by embedding them in qualitative research: ProtecT (prostate testing for cancer and treatment) study. BMJ. 2002;325:766–70.
Metcalfe C, Blazeby JM, Berrisford R et al. ROMIO: Randomised Oesophagectomy: minimally invasive or open. Sydney: Health Technology Assessment Trial Funded; 2012.
Hulscher JB, van Sandick JW, de Boer AG, Wijnhoven BP, Tijssen JG, Fockens P, et al. Extended transthoracic resection compared with limited transhiatal resection for adenocarcinoma of the esophagus. N Engl J Med. 2002;347:1662–9.
Blencowe NS, Strong S, McNair AG, Brookes ST, Crosby T, Griffin SM, et al. Reporting of short-term clinical outcomes after esophagectomy: a systematic review. Ann Surg. 2012;255:658–66.
Reynolds JV, McLaughlin R, Moore J, Rowley S, Ravi N, Byrne PJ. Prospective evaluation of quality of life in patients with localized oesophageal cancer treated by multimodality therapy or surgery alone. Br J Surg. 2006;93:1084–90.
Blazeby JM, Sanford E, Falk SJ, Alderson D, Donovan JL. Health-related quality of life during neoadjuvant treatment and surgery for localized esophageal carcinoma. Cancer. 2005;103:1791–9.
Bege T, Lelong B, Esterni B, Turrini O, Guiramand J, Francon D, et al. The learning curve for the laparoscopic approach to conservative mesorectal excision for rectal cancer: lessons drawn from a single institution’s experience. Ann Surg. 2010;251:249–53.
Itani KM, Hur K, Kim LT, Anthony T, Berger DH, Reda D, et al. Comparison of laparoscopic and open repair with mesh for the treatment of ventral incisional hernia: a randomized trial. Arch Surg. 2010;145:322–8.
International Union Against Cancer. TNM Classification of Malignant Tumours. In: Sobin LH, Gospodarowicz MK, Wittekind C, editors. West Sussex, UK: Wiley-Blackwell; 2009.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Parameswaran, R., Titcomb, D.R., Blencowe, N.S. et al. Assessment and Comparison of Recovery after Open and Minimally Invasive Esophagectomy for Cancer: An Exploratory Study in Two Centers. Ann Surg Oncol 20, 1970–1977 (2013). https://doi.org/10.1245/s10434-012-2848-7
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-012-2848-7