Abstract
Indolealkylamine (IAA) drugs are 5-hydroxytryptamine (5-HT or serotonin) analogs that mainly act on the serotonin system. Some IAAs are clinically utilized for antimigraine therapy, whereas other substances are notable as drugs of abuse. In the clinical evaluation of antimigraine triptan drugs, studies on their biotransformations and pharmacokinetics would facilitate the understanding and prevention of unwanted drug–drug interactions (DDIs). A stable, principal metabolite of an IAA drug of abuse could serve as a useful biomarker in assessing intoxication of the IAA substance. Studies on the metabolism of IAA drugs of abuse including lysergic acid amides, tryptamine derivatives and β-carbolines are therefore emerging. An important role for polymorphic cytochrome P450 2D6 (CYP2D6) in the metabolism of IAA drugs of abuse has been revealed by recent studies, suggesting that variations in IAA metabolism, pharmaco- or toxicokinetics and dynamics can arise from distinct CYP2D6 status, and CYP2D6 polymorphism may represent an additional risk factor in the use of these IAA drugs. Furthermore, DDIs with IAA agents could occur additively at the pharmaco/toxicokinetic and dynamic levels, leading to severe or even fatal serotonin toxicity. In this review, the metabolism and potential DDIs of these therapeutic and abused IAA drugs are described.
Similar content being viewed by others
INTRODUCTION
Indolealkylamines (IAAs) are chemical derivatives of 5-hydroxytryptamine (5-HT or serotonin), a monoamine neurotransmitter that modulates human mood and behaviors. Structurally, these compounds all possess an indole moiety and a basic nitrogen atom, which are connected by an alkyl chain usually of two carbons in length. Acting on the serotonergic system, some IAA agents such as ergotamine and triptan drugs (e.g. sumatriptan, naratriptan and almotriptan) (Fig. 1) have been successfully developed for antimigraine therapy (1–3).
Many other IAA agents are important as widely abused substances although some show potential in psychopharmacotherapy. This group of IAA agents consists of lysergic acid amides such as d-lysergic acid diethylamide (LSD) and ergine (LSA), tryptamines such as psilocybin, N,N-dimethyltryptamine (DMT), bufotenine, 5-methoxy-N,N-dimethyltryptamine (5-MeO-DMT) and 5-methoxy-N,N-diisopropyltryptamine (5-MeO-DIPT), and β-carbolines such as harman, harmaline and harmine (4–6) (Fig. 2). Tryptamine (e.g. 5-MeO-DMT) and β-carboline (e.g. harmaline) derivatives are sometimes abused together. These substances are readily synthesized in underground laboratories, sold via the internet and abused particularly by teenagers and young adults. As an unscheduled substance, 5-MeO-DMT has even been referred to as the next generation designer drug to replace “ecstasy.” Cases of IAA intoxication have been continuously documented in the United States (7–9). Overdosing or combined abuse of IAA agents may cause severe or even fatal hyperserotonergic toxicity, namely “serotonin syndrome” (10,11). Of note, serotonin toxicity has become an important clinical problem over the last 15 years with the increasing use of psychotropic agents.
A substantial body of research has revealed considerable variations in the metabolic and pharmacokinetic properties for therapeutic triptan agents, and provided adequate data to predict metabolic drug–drug interactions (DDIs) in clinical practice. In contrast, the metabolism of IAA drugs of abuse has not been fully characterized because of legal, ethical and safety issues associated in conducting human tests. For these agents, a stable metabolite, measured by a reliable analytical method, may serve as a better approach for forensic analysis. Many metabolic data were therefore obtained from animal studies, in which the discrepancy is obvious for some drugs (12,13). Furthermore, the specific role of individual drug-metabolizing enzymes including monoamine oxidases (MAO) and cytochrome P450 (P450 or CYP) enzymes (14) remains undefined, and mechanistic understanding of potential DDIs with other abused or therapeutic agents is mostly unknown. Increased knowledge in this area may advance our understanding of individual vulnerability to and/or protection from illicit drugs of abuse (15). This review, therefore, aims to describe our current understanding of the metabolism and potential DDIs of IAA drugs.
METABOLISM AND DRUG–DRUG INTERACTIONS OF THERAPEUTIC INDOLEALKYLAMINE DRUGS
Mechanisms of Indolealkylamine Drugs for Antimigraine Therapy
Ergotamine remains as a useful drug for acute treatment of severe migraine attacks (1,16). It is an ergot alkaloid originally isolated from fungus, and its pharmacological property in relieving migraine headache was shown about 70 years ago. Its antimigraine effect is generally attributed to the actions on 5-HT1B/1D receptors, whereas its side effects may be caused by the nonselective actions on a variety of other receptors including dopamine and 5-HT1A receptors.
In contrast to the complex mode of actions of ergotamine, newer IAA antimigraine drugs, namely triptans, are much more selective for 5-HT1B and 5-HT1D receptors with high affinity (2,3). Sumatriptan is the first of these “new generation” IAA antimigraine agents that are better tolerated by patients. The pharmacokinetics properties of these triptans are quite diverse. For instance, the oral bioavailability of sumatriptan is about 14% whereas naratriptan is 63–74%. The elimination half-life of sumatriptan is 2 h whereas for frovatriptan, it is 25 h (Table I). The sharp difference in elimination of different triptans is at least partly due to the marked difference in the metabolism of these drugs.
Metabolism and Drug–Drug Interactions of Ergotamine and Triptans
Although ergotamine is known to be extensively metabolized in the liver, its metabolic pathways are largely undefined in humans. Nonetheless, there is good evidence from animal studies supporting that CYP3As are the major enzymes responsible for ergotamine metabolism (17). Indeed, CYP3A inhibitory drugs such as erythromycin and troleandomycin are known to decrease ergotamine metabolism and may lead to unwanted DDIs. To prevent such metabolic DDIs and potentially adverse drug effects, concomitant use of ergotamine with CYP3A4 inhibitory drugs should be avoided.
Deamination metabolism is the predominant pathway for sumatriptan (18) and rizatriptan (19), and a major route for almotriptan (20). MAO-A is the principal enzyme responsible for initiating the biotransformation (Table I). Their end metabolites, indole acetic acids, are inactive and can be readily recovered in urine. For instance, 50% of orally administered and 35% of intravenously administered (14)C-rizatriptan was excreted as triazolomethyl-indole acetic acid in human urine (19). As expected, concurrent administration of MAO-A inhibitors such as moclobemide may decrease the clearance of these triptans and increase the systemic exposure (20).
The other major pathway for almotriptan metabolism is hydroxylation, which is catalyzed mainly by CYP3A4 and CYP2D6 (20). In addition to deamination inactivation, rizatriptan undergoes N-oxygenation, 6-hydroxylation and N-demethylation (19). The N-monodesmethyl-rizatriptan, formed to a minor degree, exhibits similar pharmacological activity as the parent drug at the 5-HT1B/1D receptors. In contrast, 6-hydroxy-rizatriptan and the N-oxide produced by phase I drug-metabolizing enzymes are not active at the 5-HT1B/1D receptors.
N-Demethylation is the main metabolic pathway for zolmitriptan (Fig. 3), eletriptan and frovatriptan. CYP1A2 is the major enzyme mediating N-demethylation of zolmitriptan (21) and frovatriptan (22,23), and CYP3A4 is the primary enzyme catalyzing N-demethylation of eletriptan (24). In vitro studies have also revealed that CYP3A4 inhibitors can significantly reduce eletriptan N-demethylation (22,23). Because zolmitriptan is primarily excreted via this oxidative metabolic route, CYP1A2 inhibitors and inducers are expected to significantly alter the clearance and systemic exposure of zolmitriptan (21). In contrast, the CYP1A2 inhibitor fluvoxamine has been shown to have minor effects on frovatriptan pharmacokinetics, primarily because frovatriptan is significantly eliminated by renal clearance (22).
In contrast to the inactive N-desmethyl-frovatriptan, the N-demethylated metabolites from zolmitriptan and eletriptan are both active at the 5-HT1B/1D sites. In particular, the N-desmethyl-zolmitriptan acts on 5-HT1B/1D receptors with an affinity about two- to six-fold of that of zolmitriptan and its steady state concentration is also higher than the parent drug. Therefore, N-desmethyl-zolmitriptan may have important contribution to the overall zolmitriptan drug effects. This active metabolite undergoes selective MAO-A-mediated deamination metabolism, resulting in an inactive indole acetic acid derivative (21) (Fig. 3). Because zolmitriptan is extensively N-demethylated and N-desmethyl-zolmitriptan is primarily excreted via deamination, potent MAO-A inhibitors are anticipated to alter the pharmacokinetics of N-desmethyl-zolmitriptan in humans. Indeed, concurrent use of selective MAO-A inhibitor, moclobemide, has been shown to cause 1.5- to 3-fold increase in the systemic exposure (AUC) and peak drug concentration (Cmax) of N-desmethyl-zolmitriptan (25).
Additionally, some N-demethylated triptan metabolites may be further hydroxylated or N-acetylated (e.g. frovatriptan), and a small portion of the parent triptans may be converted to N-oxide (e.g. zolmitriptan by CYP1A2; Fig. 3). These information may aid our understanding of the pharmacokinetics of triptans and in predicting their unwanted metabolic DDIs.
METABOLISM AND DRUG–DRUG INTERACTIONS OF INDOLEALKYLAMINE DRUGS OF ABUSE
Widespread Abuse of Indolealkylamine Drugs
Since the discovery of hallucinogenic properties for LSD (Fig. 2), which include the alteration and distortion of human perceptions, this agent has been used by millions of people in the United States and elsewhere for quasi-religious and recreational purposes. Other psychedelic IAA drugs of abuse include psilocybin, DMT, bufotenine, 5-MeO-DMT, 5-MeODIPT, harman, harmine, harmaline and ibogaine (Fig. 2) that are all 5-HT analogs.
Many IAAs have been found to be the psychoactive ingredients of a wide range of plant, fungus and animal preparations, which have been used in social and religious cultures in history. 5-MeO-DMT and bufotenine are the major ingredients of the venom of psychoactive toads such as Colorado River Bufo alvarius (26,27). 5-MeO-DMT is also the psychoactive agent in numerous plant preparations including Virola snuffs. Harmaline, harmine, tetrahydroharmine and DMT are important active constituents of the beverage Ayahuasca (28). Several methylated IAAs have been detected as endogenous compounds in humans. 5-MeO-DMT can be synthesized in human pineal gland and has been detected in both pineal gland and urine (29–31). The methylated IAAs are also present in retina at relatively high levels (32). Derived from 5-HT through methylation (methylated IAAs) and Pictet–Spengler condensation (β-carbolines), the presence of these psychedelic IAAs in humans is certainly clear. Although their biological roles and association with psychiatric diseases are still obscure, increased understanding of their metabolic pathways (33,34) would be helpful in answering these questions.
Presently, IAA drugs are readily synthesized in clandestine laboratories and sold via the internet. Studies by Monitoring the Future programs (35) have revealed that, in every year since 1991 to 2006, more than 8.3% of 12th-graders have used hallucinogens. The abuse of hallucinogenic substance other than LSD remains over 8.0% since 2001. Additionally, nearly 50% of teenagers surveyed since 2001 said that it was “fairly easy” or “very easy” to get hallucinogens other than LSD. As a presently unscheduled hallucinogen, 5-MeO-DMT has been suggested as the next generation designer drug to replace “ecstasy” and it is often used in combination with harmaline (also an unscheduled substance in the USA). Intoxications due to IAA drugs have been frequently reported in hospitals in recent years (7–9).
These psychoactive IAA agents have also shown some therapeutic value in treating mental health disorders. For instance, ayahuasca may be utilized for the treatment of alcoholism, serotonergic defects and substance abuse (28), and ibogaine for cocaine addiction (36). Indeed, IAAs act on a variety of 5-HT receptors, serotonin transporter, or MAO enzyme that are highly favorable molecular targets for treating depression, anxiety, schizophrenia, and other psychiatric disturbances (37). Nevertheless, medical use of these agents remains a challenge because IAA drug responses exhibit considerable variability in humans (38), and concerns about their safety and abuse liability persist (28,39).
Mechanisms of Action of Indolealkylamine Drugs of Abuse
LSD was thought initially to act through 5-HT antagonism in the central nervous system or through mimicry of 5-HT actions by interacting with the 5-HT receptor. After 5-HT was firmly established as a neurotransmitter, it was found that LSD inhibited the activity of serotonergic neurons. With the delineation of 5-HT receptor subtypes and the extension of serotonergic actions to other hallucinogenic agents, Glennon et al. (40) established an excellent correlation between the hallucinogenic potency and the affinity of IAAs for 5-HT2 receptors. Collective evidence from biochemical, physiological and behavioral tests suggests that these hallucinogens likely act on a common site of 5-HT2A and other 5-HT2 receptors in the central nervous system (5).
The pharmacological and toxicological effects of 5-MeO-DMT, however, were believed to act through the 5-HT1A receptor, as supported by results summarized by Winter et al. (41). Furthermore, the inhibition of MAO enzyme or 5-HT uptake was thought to be important for the actions of β-carbolines such as harmaline in its induction of hypothermia (42,43). The hallucinogenic effects of harmaline are likely produced from binding to 5-HT2A and 5-HT2C receptors, and the tremorgenic properties are due to the interactions with benzodiazepine receptors (44–46). Because harmaline stimulates locus coeruleus neuronal activity, it was even proposed as an endogenous ligand for imidazoline receptors (47).
Hallucinations (e.g. colorful and luminous patterns) are characteristics for IAA intoxication in humans (26). Distorted perception of time or auditory effects may also occur. In animals, IAA drugs (e.g. harmaline that is discussed above) are known to cause a variety of drug effects including physiological (e.g. body temperature), biochemical (e.g. monoamine neurotransmitters), and behavioral (e.g. discriminative control) changes. Despite some exceptions (48), there is a strong correlation between the discriminative stimulus effects in non-verbal species and subjective effects in humans (49–51).
There are significant variations of drug effects for individual IAA agents in humans (4,26–28,38). Some individuals can be adversely affected by IAA drugs including LSD, 5-MeO-DMT, bufotenine, and harmaline, some may not have any response, and yet others would use them with impunity. Meanwhile, depending upon the doses, 5-MeO-DMT may induce hypothermic or hyperthermic effects in animals (52,53). Unfortunately, a clear understanding of the molecular basis and the vulnerability to IAA substances is still lacking.
Metabolism of Indolealkylamine Drugs of Abuse
Metabolism of d-Lysergic Acid Diethylamide
LSD is extensively metabolized in laboratory animals and only a trivial fraction of the parent drug is excreted in urine. Major metabolites of LSD detected in the rat and guinea pig urines were the 13- and 14-hydroxy-LSD (HO-LSD) and their corresponding glucuronic acid conjugates (54). Other metabolites included 2-oxo-LSD, lysergic acid ethylamide (LSE) and N-desmethyl-LSD (nor-LSD). In the isolated perfused rat liver, aromatic hydroxylation was shown as the principal metabolic pathway (55). However, studies on LSD metabolism in rat liver microsomes indicated that nor-LSD and LSE were the major metabolites, followed by 13-hydroxy-LSD (56). The metabolism of LSD was more complex in rhesus monkey because the urine consisted of at least nine metabolites. In contrast to the metabolism in rats and guinea pigs, aromatic hydroxylation was a minor metabolic pathway in rhesus monkey (54). Thus, significant difference in LSD metabolism between humans and laboratory animals has been observed.
Indeed, at least four metabolites have been identified in urine from human users of LSD, which include 2-oxo-3-hydroxy-LSD (2-oxo-3-HO-LSD), nor-LSD, 13- and 14-hydroxy-LSD glucuronides (57) (Fig. 4). Although other metabolites such as LSE were produced as major metabolites from LSD incubated with human liver microsomes (58), 2-oxo-3-HO-LSD was shown to be the main human urinary metabolite, which may be present at 4- to 41-times higher concentration than urinary LSD (59). This metabolite therefore holds promise as a biomarker for LSD use in the forensic toxicology laboratories.
The detection of 2-oxo-LSD in human body fluids indicates that 2-oxo-3-HO-LSD may be formed in two steps via the 2-oxo-LSD intermediate. Recent studies on LSD metabolism in human liver microsomes and hepatocytes not only confirmed the formation of 2-oxo-3-HO-LSD but also identified a 2,3-dihydroxy-LSD metabolite (60). This finding suggests that 2-oxo-3-HO-LSD could be produced through dehydrogenation of the 2,3-dihydroxy-LSD intermediate, which is presumably formed from LSD 2,3-epoxide.
Due to limited studies on LSD metabolism in humans, further well-controlled studies are warranted to validate whether 2-oxo-3-HO-LSD is indeed the major metabolite (59) and to delineate the particular mechanisms that are involved in the formation of this metabolite (60). Furthermore, almost nothing is known regarding the contribution of specific drug-metabolizing enzyme to the production of individual LSD metabolites in humans. Advance in these areas could facilitate forensic detection, as well as the prediction and prevention of potential metabolic DDIs between LSD and other substances.
Metabolism of Tryptamine Derivatives
Like tryptamine itself (31,61), tryptamine derivatives including DMT, bufotenine and 5-MeO-DMT are excreted primarily via oxidative deamination and a predominant role for MAO-A is certain in this metabolic pathway (62–66). However, there are some discrepancies among animal studies reported in the literature. Sitaram’s group (13,67,68) showed that DMT and 5-MeO-DMT were metabolized through deamination, N-demethylation, O-demethylation, and N-oxygenation, and found that N-oxides were the major metabolites in rat tissues. In contrast, oxidative deamination and O-demethylation (followed by glucuronidation or deamination) were shown to be the major pathways for (14)C-labeled 5-MeO-DMT in rats (12). Our in vitro studies using human liver microsomes, hepatocytes and recombinant enzymes agreed with the importance of deamination for 5-MeO-DMT metabolism, while 5-MeO-DMT was shown to be O-demethylated primarily by CYP2D6 (33,69) (Fig. 5), a P450 enzyme that has enormous genetic variations and is well recognized for its clinical importance (70).
5-MeO-DMT O-demethylation is potentially an activation process because the metabolite bufotenine is a biologically active agent. Although the psychedelic activity for bufotenine has been questioned (4,26,71), the confusion probably arises due to its poor lipid solubility. A variety of biochemical studies (71,72) supported the hypothesis that bufotenine was a potent ligand at the 5-HT2A receptor with an affinity up to ten-fold higher than 5-MeO-DMT. Vogel and Evans (73) estimated that bufotenine was about three times more potent than 5-MeO-DMT within the brain. Other studies also indicated that bufotenine was psychoactive in humans, as summarized by Ott (26,27). It is interesting to note that bufotenine (the metabolite) is currently listed as a Schedule I controlled substance, whereas 5-MeO-DMT (its parent compound) is not. On the other hand, bufotenine may be converted to 5-MeO-DMT in vivo by methyltransferase (Fig. 5).
5-MeO-DIPT is also an abused tryptamine derivative, which contains N,N-diisopropyl groups, rather than the N,N-dimethyl groups within 5-MeO-DMT. The metabolism of 5-MeODMT vs. 5-MeO-DIPT can be compared (74). Analyses of urine samples collected from 5-MeO-DIPT users (75–77) suggested that this drug was mainly excreted via metabolism, in particular, O- and N-dealkylation and deamination (Fig. 6). Because isotope-labeled 5-MeO-DIPT was not used and 5-HO-indole acetic acid is intrinsically present in human urine, it is unclear which pathway is the predominant route. Nonetheless, extensive studies using human liver microsomes and recombinant enzymes (74,78,79) revealed that CYP2D6 was responsible for 5-MeO-DIPT O-dealkylation, while CYP1A2, 3A4, 2C19 enzymes mediated its N-dealkylation. The critical role for CYP2D6 in 5-MeO-DIPT O-dealkylation might provide a reasonable explanation for the sharp difference in urinary 5-hydroxy-N,N-diisopropyltryptamine (5-HO-DIPT) level that was observed between Caucasian and Japanese drug users (75,77), if that Caucasian 5-MeO-DIPT user were to have deficient CYP2D6 activity and the Japanese user have regular CYP2D6 activity. Furthermore, 5-MeO-DIPT was mainly O-dealkylated in human liver microsomes, whereas it was primarily N-dealkylated in rat liver microsomes (78,79). The sharp species difference in region-selective metabolism of 5-MeO-DIPT, which is not unusual in drug metabolism (80), may add complexity in the extrapolation of animal data to humans.
Different from the tryptamine derivatives discussed above, psilocybin and psilocin are 4-substituted IAA drugs that have been found in many psychedelic mushrooms worldwide. Psilocin was readily detected in the blood and urine from human subjects taken psilocybin (81). The dephosphorylation of psilocybin to produce psilocin (Fig. 7) appears to be an activation process. Identification of other metabolites including 4-hydroxyindole acetic acid (4-HO-IAA) and 4-hydroxyindole acetaldehyde suggested that psilocin underwent deamination oxidation. Additionally, the 4-hydroxy group of psilocin may be conjugated to form an O-glucuronide (Fig. 7). In spite of these information, limited studies on the metabolism of psilocybin and psilocin have been reported, and specific enzymes that catalyze the formation of individual metabolites remain unknown.
Metabolism of β-Carbolines and Ibogaine
β-Carbolines were shown to be good substrates for N-methyltransferase and the corresponding cation products were highly neurotoxic (82,83). In contrast, hydroxylation and O-demethylation of β-carboline alkaloids, followed by glucuronidation and sulfation, are expected to be detoxification processes that may play an important role in protection against brain damage.
The metabolism of harmine is relatively well understood, which includes two major oxidative pathways, O-demethylation and 6-hydroxylation (Fig. 8). Hydroxylation could also occur at the 3- or 4-position of harmine (84). Hydroxyl β-carboline metabolites such as harmol are readily conjugated through glucuronidation and sulfation. The formation of harmol from harmine exhibited three- to four-fold higher Vmax in phenobarbitone-induced mouse liver microsomes (85). Our recent study revealed that harmine O-demethylation was catalyzed by human CYP2D6, 1A1, 1A2, 2C9 and 2C19 enzymes (86). Furthermore, we found that CYP2D6 was a major enzyme mediating the O-demethylation of harmaline and pinoline (33,86), suggesting an important role for CYP2D6 in O-demethylation of these β-carbolines, although its role in their total clearance has not been determined yet. Given the fact that defect of CYP2D6 can significantly alter the pharmacokinetics of CYP2D6 substrate drugs, distinct pharmacokinetics may occur for these β-carbolines due to different CYP2D6 status. Indeed, a recent study (87) disclosed that there were two phenotypes in harmine pharmacokinetics, fast and slow metabolism, in humans. Further investigation will determine whether this is because of CYP2D6 polymorphism, and whether this would be translated into significant difference in drug responses.
Little is known for many other β-carbolines regarding the specific enzymes that contribute to their biotransformation, although some of them have been shown to undergo aromatic hydroxylations. The depletion of harman in mouse liver microsomes was enhanced about 4- and 11-fold when pretreated with phenobarbitone and 3-methylcholanthrene, respectively. The major metabolite was found to be 6-hydroxyharman the formation of which was likely mediated by P450 enzymes (88), but it is unclear which particular isozyme is involved. Interestingly, species difference was also shown in the metabolism of tetrahydroharman (1-methyl-1,2,3,4-tetrahydro-β-carboline). In vitro and in vivo studies demonstrated that tetrahydroharman was hydroxylated at the 5-, 6- and 7-positions in rats (89), whereas it was mainly hydroxylated at the 6- and 7-positions in humans (90,91). Furthermore, 6-hydroxytetrahydroharman was present in both free and conjugated forms, and 7-hydroxytetrahydroharman mainly exist as a conjugated form in the urine from humans administered with deuterated tetraharman.
Ibogaine is an indole alkaloid initially isolated from a rain forest shrub, Tabernanthe Iboga, which is native to Africa. It is a schedule I substance in the United States while its potential as a pharmacotherapeutic agent in treating cocaine and opiate addictions has been explored recently (36). Even in a Phase I trial containing a limited number of human subjects, ibogaine exhibited considerable variability in the pharmacokinetics of parent drug and its major metabolite, noribogaine (92). CYP2D6 was subsequently identified as the predominant enzyme that catalyzed the formation of noribogaine from ibogaine (93). Furthermore, noribogaine is pharmacologically active and has a similar pharmacodynamic profile as the parent drug with higher affinities to the opioid receptors and serotonin transporter. An important contribution of noribogaine to the overall ibogaine drug effects and the involvement of CYP2D6 polymorphism would also add complexity in the use of ibogaine.
Potential Drug–Drug Interactions of Indolealkylamine Drugs of Abuse
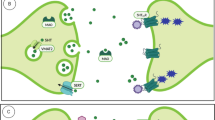
DDIs occur at the pharmacokinetic level when one drug (perpetrator) alters the absorption, distribution, metabolism or excretion of another drug (victim) and at the pharmacodynamic level when the perpetrator and victim drugs work on the common targets (e.g. receptors) of action. Severe or fatal adverse reactions could be induced when pharmacokinetic and pharmacodynamic DDIs arise together additively. This may be true for IAA drugs that are abused concomitantly, in particular, through the use of a tryptamine derivative (e.g. 5-MeO-DMT) and a β-carboline (e.g. harmaline). First, harmaline itself possesses psychotropic activities, which not only inhibits MAO-mediated 5-HT degradation but also acts directly on 5-HT receptors (46). Concomitant use of such MAO inhibitor and 5-HT agonist would potentiate serotonergic neurotransmission (Fig. 9). Second, by inhibiting MAO-A activity, harmaline is anticipated to reduce 5-MeO-DMT metabolic disposition, leading to an increased and prolonged exposure to 5-MeO-DMT. Additionally, the inhibition of MAO-A activity may shunt 5-MeO-DMT deamination to O-demethylation and results in elevated levels of the psychoactive metabolite bufotenine, the formation of which will depend on CYP2D6 status. A contribution of both 5-HT2A and 5-HT1A receptors to the overall 5-MeO-DMT drug effects is possible, and increased levels of bufotenine may even convert 5-MeO-DMT (5-HT1A) dominant effects to bufotenine (5-HT2A agonist) dominant effects. Such complex DDIs among IAA drugs and the involvement of CYP2D6 pharmacogenetics could represent additional risk factors in IAA abuse.
Serotonergic neurotransmission. Hyperserotonergic effects may be induced when a tryptamine derivative (5-HT receptor agonist) and a β-carboline (monoamine oxidase inhibitor) are used concurrently. In particular, the β-carboline can reduce the degradation of 5-HT neurotransmitter and inhibit the metabolism of tryptamine derivative
The dominant role of CYP2D6 in ibogaine O-demethylation metabolism also suggests that ibogaine may be subject to metabolic DDIs with CYP2D6 inhibitors (93). Of note, some selective serotonin reuptake inhibitors (SSRIs) such as paroxetine and fluoxetine are potent inhibitors of CYP2D6. These SSRIs have been known to cause DDIs with other psychotropic drugs metabolized by CYP2D6. Quinidine is another known potent inhibitor of CYP2D6 with an inhibitory potency in the nanomolar range. A single oral dose of 50 mg of quinidine strikingly altered the metabolism and disposition of CYP2D6 substrate drugs including debrisoquine, dextromethorphan and codeine (94–96). Similarly, the potential of metabolic DDIs is increased (93) for ibogaine with CYP2D6 inhibitory medications including SSRIs.
Nevertheless, quantitative prediction of DDIs with IAA drugs of abuse is extremely difficult because the precise contribution of specific drug-metabolizing enzyme to the overall clearance of an IAA drug (e.g. 5-MeO-DMT) or even the enzymes involved (e.g. LSD) remains unknown. Secondly, other factors including drug transporters and/or the target receptors or enzymes may be affected simultaneously by the drugs. Thus, theoretical predictions of DDIs with IAA drugs can be quite complex, and would require clinical verification.
CONCLUSION
Acting on the serotonergic system, IAA drugs represent a major class of abused hallucinogens. Some IAA drugs however show potential in psychopharmacotherapy and others have been developed as antimigraine agents. Studies on the metabolism of triptans provide useful information to predict adverse metabolic DDIs in clinical practice. In contrast, there are limited metabolic data for IAA drugs of abuse. Increased knowledge in this area could provide better understanding of the hazards of IAA drugs of abuse, including the potential of metabolic variability and adverse interactions with other abused or therapeutic drugs.
References
S. D. Silberstein, and D. C. McCrory. Ergotamine and dihydroergotamine: history, pharmacology, and efficacy. Headache. 43(2):144–166 (2003).
S. S. Jhee, T. Shiovitz, A. W. Crawford, and N. R. Cutler. Pharmacokinetics and pharmacodynamics of the triptan antimigraine agents: a comparative review. Clin. Pharmacokinet. 40(3):189–205 (2001).
C. Dahlof. Integrating the triptans into clinical practice. Curr. Opin. Neurol. 15(3):317–322 (2002).
A. T. Shulgin, and A. Shulgin. TIKAL The Continuation, Transform, Berkeley, CA, 1997.
G. K. Aghajanian, and G. J. Marek. Serotonin and hallucinogens. Neuropsychopharmacology. 21(2 Suppl):16S–23S (1999).
R. A. Glennon. Arylalkylamine drugs of abuse: an overview of drug discrimination studies. Pharmacol. Biochem. Behav. 64(2):251–256 (1999).
D. E. Brush, S. B. Bird, and E. W. Boyer. Monoamine oxidase inhibitor poisoning resulting from Internet misinformation on illicit substances. J. Toxicol. Clin. Toxicol. 42(2):191–195 (2004).
H. Long, L. S. Nelson, and R. S. Hoffman. Alpha-methyltryptamine revisited via easy Internet access. Vet. Hum. Toxicol. 45(3):149 (2003).
A. A. Muller. New drugs of abuse update: Foxy Methoxy. J. Emerg. Nurs. 30(5):507–508 (2004).
E. W. Boyer, and M. Shannon. The serotonin syndrome. N. Engl. J. Med. 352(11):1112–1120 (2005).
G. K. Isbister, and N. A. Buckley. The pathophysiology of serotonin toxicity in animals and humans: implications for diagnosis and treatment. Clin. Neuropharmacol. 28(5):205–214 (2005).
S. Agurell, B. Holmstedt, and J. E. Lindgren. Metabolism of 5-methoxy-N,-N dimethyltryptamine-14 C in the rat. Biochem. Pharmacol. 18(10):2771–2781 (1969).
B. R. Sitaram, L. Lockett, R. Talomsin, G. L. Blackman, and W. R. McLeod. In vivo metabolism of 5-methoxy-N,N-dimethyltryptamine and N,N-dimethyltryptamine in the rat. Biochem. Pharmacol. 36(9):1509–1512 (1987).
F. P. Guengerich. 2 in drug metabolism and toxicity. AAPS J. 8(1):E101–E111 (2006).
J. L. Rutter. Symbiotic relationship of pharmacogenetics and drugs of abuse. AAPS J. 8(1):E174–E184 (2006).
P. Tfelt-Hansen, P. R. Saxena, C. Dahlof, et al. Ergotamine in the acute treatment of migraine: a review and European consensus. Brain. 123(Pt 1):9–18 (2000).
A. S. Moubarak, and C. F. Rosenkrans. Hepatic metabolism of ergot alkaloids in beef cattle by cytochrome P450. Biochem. Biophys. Res. Commun. 274(3):746–749 (2000).
C. M. Dixon, G. R. Park, and M. H. Tarbit. Characterization of the enzyme responsible for the metabolism of sumatriptan in human liver. Biochem. Pharmacol. 47(7):1253–1257 (1994).
K. P. Vyas, R. A. Halpin, L. A. Geer, et al. Disposition and pharmacokinetics of the antimigraine drug, rizatriptan, in humans. Drug Metab. Dispos. 28(1):89–95 (2000).
J. C. Fleishaker, K. K. Ryan, J. M. Jansat, et al. Effect of MAO-A inhibition on the pharmacokinetics of almotriptan, an antimigraine agent in humans. Br. J. Clin. Pharmacol. 51(5):437–441 (2001).
M. J. Wild, D. McKillop, and C. J. Butters. Determination of the human cytochrome P450 isoforms involved in the metabolism of zolmitriptan. Xenobiotica. 29(8):847–857 (1999).
P. Buchan, A. Wade, C. Ward, S. D. Oliver, A. J. Stewart, and S. Freestone. Frovatriptan: a review of drug–drug interactions. Headache. 42(Suppl 2):S63–S73 (2002).
P. Buchan, C. Keywood, A. Wade, and C. Ward. Clinical pharmacokinetics of frovatriptan. Headache. 42(Suppl 2):S54–S62 (2002).
D. C. Evans, D. O'Connor, B. G. Lake, R. Evers, C. Allen, and R. Hargreaves. Eletriptan metabolism by human hepatic CYP450 enzymes and transport by human P-glycoprotein. Drug Metab. Dispos. 31(7):861–869 (2003).
P. Rolan. Potential drug interactions with the novel antimigraine compound zolmitriptan (Zomig, 311C90). Cephalalgia. 17(Suppl 18):21–27 (1997).
J. Ott. Pharmanopo-psychonautics: human intranasal, sublingual, intrarectal, pulmonary and oral pharmacology of bufotenine. J. Psychoactive Drugs. 33(3):273–281 (2001).
J. Ott. Pharmepena-psychonautics: human intranasal, sublingual and oral pharmacology of 5-methoxy-N,N-dimethyl-tryptamine. J. Psychoactive Drugs. 33(4):403–407 (2001).
D. J. McKenna. Clinical investigations of the therapeutic potential of ayahuasca: rationale and regulatory challenges. Pharmacol. Ther. 102(2):111–129 (2004).
N. Narasimhachari, B. Heller, J. Spaide, et al. Urinary studies of schizophrenics and controls. Biol. Psychiatry. 3(1):9–20 (1971).
R. B. Guchhait. Biogenesis of 5-methoxy-N,N-dimethyltryptamine in human pineal gland. J. Neurochem. 26(1):187–190 (1976).
M. M. Airaksinen, and I. Kari. Beta-carbolines, psychoactive compounds in the mammalian body. Part I: occurrence, origin and metabolism. Med. Biol. 59(1):21–34 (1981).
M. Leino, and M. M. Airaksinen. Methoxyindoles of the retina. Med. Biol. 63(4):160–169 (1985).
A. M. Yu, J. R. Idle, T. Herraiz, A. Kupfer, and F. J. Gonzalez. Screening for endogenous substrates reveals that CYP2D6 is a 5-methoxyindolethylamine O-demethylase. Pharmacogenetics. 13(6):307–319 (2003).
N. Takeda, R. Ikeda, K. Ohba, and M. Kondo. Bufotenine reconsidered as a diagnostic indicator of psychiatric disorders. Neuroreport. 6(17):2378–2380 (1995).
L. D. Johnston, P. M. O'Malley, J. G. Bachman, and J. E. Schulenberg. Teen Drug Use Continues Down in 2006, Particularly Among Older Teens; But Use of Prescription-type Drugs Remains High. University of Michigan News and Information Services, Ann Arbor, MI, December 21, 2006. Available: www.monitoringthefuture.org.
D. C. Mash, C. A. Kovera, J. Pablo, et al. Ibogaine: complex pharmacokinetics, concerns for safety, and preliminary efficacy measures. Ann. NY Acad. Sci. 914:394–401 (2000).
B. L. Roth, S. M. Hanizavareh, and A. E. Blum. Serotonin receptors represent highly favorable molecular targets for cognitive enhancement in schizophrenia and other disorders. Psychopharmacology (Berl.). 174(1):17–24 (2004).
H. D. Abraham, A. M. Aldridge, and P. Gogia. The psychopharmacology of hallucinogens. Neuropsychopharmacology. 14(4):285–298 (1996).
H. D. Abraham, and A. M. Aldridge. Adverse consequences of lysergic acid diethylamide. Addiction. 88(10):1327–1334 (1993).
R. A. Glennon, M. Titeler, and J. D. McKenney. Evidence for 5-HT2 involvement in the mechanism of action of hallucinogenic agents. Life Sci. 35(25):2505–2511 (1984).
J. C. Winter, D. J. Fiorella, D. M. Timineri, R. A. Filipink, S. E. Helsley, and R. A. Rabin. Serotonergic receptor subtypes and hallucinogen-induced stimulus control. Pharmacol. Biochem. Behav. 64(2):283–293 (1999).
M. M. Airaksinen, and I. Kari. beta-Carbolines, psychoactive compounds in the mammalian body. Part II: Effects. Med. Biol. 59(4):190–211 (1981).
A. F. Abdel-Fattah, K. Matsumoto, H. A. Gammaz, and H. Watanabe. Hypothermic effect of harmala alkaloid in rats: involvement of serotonergic mechanism. Pharmacol. Biochem. Behav. 52(2):421–426 (1995).
J. Lutes, J. F. Lorden, M. Beales, and G. A. Oltmans. Tolerance to the tremorogenic effects of harmaline: evidence for altered olivo-cerebellar function. Neuropharmacology. 27(8):849–855 (1988).
S. M. Husbands, R. A. Glennon, S. Gorgerat, et al. beta-carboline binding to imidazoline receptors. Drug Alcohol Depend. 64(2):203–208 (2001).
R. A. Glennon, M. Dukat, B. Grella, et al. Binding of beta-carbolines and related agents at serotonin (5-HT(2) and 5-HT(1A)), dopamine (D(2)) and benzodiazepine receptors. Drug Alcohol Depend. 60(2):121–132 (2000).
E. Ruiz-Durantez, J. A. Ruiz-Ortega, J. Pineda, and L. Ugedo. Stimulatory effect of harmane and other beta-carbolines on locus coeruleus neurons in anaesthetized rats. Neurosci. Lett. 308(3):197–200 (2001).
N. A. Ator, K. A. Grant, R. H. Purdy, S. M. Paul, and R. R. Griffiths. Drug discrimination analysis of endogenous neuroactive steroids in rats. Eur. J. Pharmacol. 241(2–3):237–243 (1993).
C. R. Schuster, and C. E. Johanson. Relationship between the discriminative stimulus properties and subjective effects of drugs. Psychopharmacol. Ser. 4:161–175 (1988).
L. H. Brauer, A. J. Goudie, and H. de Wit. Dopamine ligands and the stimulus effects of amphetamine animal models versus human laboratory data. Psychopharmacology (Berl.). 130(1):2–13 (1997).
A. Dekeyne, and M. J. Millan. Discriminative stimulus properties of antidepressant agents: a review. Behav. Pharmacol. 14(5–6):391–407 (2003).
G. A. Gudelsky, J. I. Koenig, H. Jackman, and H. Y. Meltzer. Suppression of the hypo- and hyperthermic responses to 5-HT agonists following the repeated administration of monoamine oxidase inhibitors. Psychopharmacology (Berl.). 90(3):403–407 (1986).
G. A. Gudelsky, J. I. Koenig, and H. Y. Meltzer. Thermoregulatory responses to serotonin (5-HT) receptor stimulation in the rat. Evidence for opposing roles of 5-HT2 and 5-HT1A receptors. Neuropharmacology. 25(12):1307–1313 (1986).
Z. H. Siddik, R. D. Barnes, L. G. Dring, R. L. Smith, and R. T. Williams. The fate of lysergic acid DI[14C]ethylamide ([14C]LSD) in the rat, guinea pig and rhesus monkey and of [14C]iso-LSD in rat. Biochem. Pharmacol. 28(20):3093–3101 (1979).
Z. H. Siddik, R. D. Barnes, L. G. Dring, R. L. Smith, and R. T. Williams. The metabolism of lysergic acid DI[14C]ethylamide ([14C]LSD) in the isolated perfused rat liver. Biochem. Pharmacol. 28(20):3081–3091 (1979).
T. Inoue, T. Niwaguchi, and T. Murata. Enzymic formation of dehydrogenated and hydroxylated metabolites from lysergic acid diethylamide by rat liver microsomes. Xenobiotica. 10(5):343–348 (1980).
S. A. Reuschel, D. Eades, and R. L. Foltz. Recent advances in chromatographic and mass spectrometric methods for determination of LSD and its metabolites in physiological specimens. J. Chromatogr. B. Biomed. Sci. Appl. 733(1–2):145–159 (1999).
J. Cai, and J. Henion. Elucidation of LSD in vitro metabolism by liquid chromatography and capillary electrophoresis coupled with tandem mass spectrometry. J. Anal. Toxicol. 20(1):27–37 (1996).
A. G. Verstraete, and E. J. Van de Velde. 2-oxo-3-hydroxy-LSD: an important LSD metabolite? Acta. Clin. Belg. Suppl. 1:94–96 (1999).
K. L. Klette, C. J. Anderson, G. K. Poch, A. C. Nimrod, and M. A. ElSohly. Metabolism of lysergic acid diethylamide (LSD) to 2-oxo-3-hydroxy LSD (O-H-LSD) in human liver microsomes and cryopreserved human hepatocytes. J. Anal. Toxicol. 24(7):550–556 (2000).
A. M. Yu, C. P. Granvil, R. L. Haining, et al. The relative contribution of monoamine oxidase and cytochrome p450 isozymes to the metabolic deamination of the trace amine tryptamine. J Pharmacol. Exp. Ther. 304(2):539–546 (2003).
F. Raynaud, and P. Pevet. 5-Methoxytryptamine is metabolized by monoamine oxidase A in the pineal gland and plasma of golden hamsters. Neurosci. Lett. 123(2):172–174 (1991).
O. Suzuki, Y. Katsumata, and M. Oya. Characterization of eight biogenic indoleamines as substrates for type A and type B monoamine oxidase. Biochem. Pharmacol. 30(11):1353–1358 (1981).
R. W. Fuller, H. D. Snoddy, and K. W. Perry. Tissue distribution, metabolism and effects of bufotenine administered to rats. Neuropharmacology. 34(7):799–804 (1995).
S. Szara, and J. Axelrod. Hydroxylation and N-demethylation of N, N-dimethyltryptamine. Experientia. 15(6):216–217 (1959).
E. Sanders-Bush, J. A. Oates, and M. T. Bush. Metabolism of bufotenine-2¢-14C in human volunteers. Life Sci. 19(9):1407–1411 (1976).
B. R. Sitaram, L. Lockett, G. L. Blackman, and W. R. McLeod. Urinary excretion of 5-methoxy-N,N-dimethyltryptamine, N,N-dimethyltryptamine and their N-oxides in the rat. Biochem. Pharmacol. 36(13):2235–2237 (1987).
B. R. Sitaram, R. Talomsin, G. L. Blackman, and W. R. McLeod. Study of metabolism of psychotomimetic indolealkylamines by rat tissue extracts using liquid chromatography. Biochem. Pharmacol. 36(9):1503–1508 (1987).
A. M. Yu, J. R. Idle, and F. J. Gonzalez. Polymorphic cytochrome P450 2D6: humanized mouse model and endogenous substrates. Drug Metab. Rev. 36(2):243–277 (2004).
U. M. Zanger, S. Raimundo, and M. Eichelbaum. Cytochrome P450 2D6: overview and update on pharmacology, genetics, biochemistry. Naunyn. Schmiedebergs. Arch. Pharmacol. 369(1):23–37 (2004).
M. C. McBride. Bufotenine: toward an understanding of possible psychoactive mechanisms. J. Psychoactive Drugs. 32(3):321–331 (2000).
B. L. Roth, M. S. Choudhary, N. Khan, and A. Z. Uluer. High-affinity agonist binding is not sufficient for agonist efficacy at 5-hydroxytryptamine2A receptors: evidence in favor of a modified ternary complex model. J. Pharmacol. Exp. Ther. 280(2):576–583 (1997).
W. H. Vogel, and B. D. Evans. Structure–activity-relationships of certain hallucinogenic substances based on brain levels. Life Sci. 20(10):1629–1635 (1977).
T. Kamata, M. Katagi, H. T. Kamata, et al. Metabolism of the psychotomimetic tryptamine derivative 5-methoxy-N,N-diisopropyltryptamine in humans: identification and quantification of its urinary metabolites. Drug Metab. Dispos. 34(2):281–287 (2006).
R. Meatherall, and P. Sharma. Foxy, a designer tryptamine hallucinogen. J. Anal. Toxicol. 27(5):313–317 (2003).
J. M. Wilson, F. McGeorge, S. Smolinske, and R. Meatherall. A foxy intoxication. Forensic Sci. Int. 148(1):31–36 (2005).
E. Tanaka, T. Kamata, M. Katagi, H. Tsuchihashi, and K. Honda. A fatal poisoning with 5-methoxy-N,N-diisopropyltryptamine, Foxy. Forensic Sci. Int. 163(1–2):152–154 (2006).
S. Narimatsu, R. Yonemoto, K. Masuda, et al. Oxidation of 5-methoxy-N,N-diisopropyltryptamine in rat liver microsomes and recombinant cytochrome P450 enzymes. Biochem. Pharmacol. 75(3):752–760 (2008).
S. Narimatsu, R. Yonemoto, K. Saito, et al. Oxidative metabolism of 5-methoxy-N,N-diisopropyltryptamine (Foxy) by human liver microsomes and recombinant cytochrome P450 enzymes. Biochem. Pharmacol. 71(9):1377–1385 (2006).
F. J. Gonzalez, and A. M. Yu. Cytochrome P450 and xenobiotic receptor humanized mice. Annu. Rev. Pharmacol. Toxicol. 46:41–64 (2006).
T. Passie, J. Seifert, U. Schneider, and H. M. Emrich. The pharmacology of psilocybin. Addict. Biol. 7(4):357–364 (2002).
D. A. Gearhart, E. J. Neafsey, and M. A. Collins. Phenylethanolamine N-methyltransferase has beta-carboline 2N-methyltransferase activity: hypothetical relevance to Parkinson's disease. Neurochem. Int. 40(7):611–620 (2002).
K. Matsubara, K. Aoyama, M. Suno, and T. Awaya. N-Methylation underlying Parkinson’s disease. Neurotoxicol. Teratol. 24(5):593 (2002).
D. J. Tweedie, and M. D. Burke. Metabolism of the beta-carbolines, harmine and harmol, by liver microsomes from phenobarbitone- or 3-methylcholanthrene-treated mice. Identification and quantitation of two novel harmine metabolites. Drug. Metab. Dispos. 15(1):74–81 (1987).
M. D. Burke, and D. G. Upshall. Species and phenobarbitone-induced differences in the kinetic constants of liver microsomal harmine O-demethylation. Xenobiotica. 6(5):321–328 (1976).
A. M. Yu, J. R. Idle, K. W. Krausz, A. Kupfer, and F. J. Gonzalez. Contribution of individual cytochrome P450 isozymes to the O-demethylation of the psychotropic beta-carboline alkaloids harmaline and harmine. J. Pharmacol. Exp. Ther. 305(1):315–322 (2003).
J. C. Callaway. Fast and slow metabolizers of Hoasca. J. Psychoactive Drugs. 37(2):157–161 (2005).
D. J. Tweedie, R. A. Prough, and M. D. Burke. Effects of induction on the metabolism and cytochrome P-450 binding of harman and other beta-carbolines. Xenobiotica. 18(7):785–796 (1988).
O. Beck, B. Jernstrom, M. Martinez, and D. B. Repke. In vitro study of the aromatic hydroxylation of 1-methyltetrahydro-beta-carboline (methtryptoline) in rat. Chem. Biol. Interact. 65(1):97–106 (1988).
H. Tsuchiya, H. Todoriki, and T. Hayashi. Metabolic hydroxylation of 1-methyl-1,2,3,4-tetrahydro-beta-carboline in humans. Pharmacol. Biochem. Behav. 52(4):677–682 (1995).
T. Herraiz, H. Guillen, V. J. Aran, J. R. Idle, and F. J. Gonzalez. Comparative aromatic hydroxylation and N-demethylation of MPTP neurotoxin and its analogs, N-methylated beta-carboline and isoquinoline alkaloids, by human cytochrome P450 2D6. Toxicol. Appl. Pharmacol. 216(3):387–398 (2006).
D. C. Mash, J. K. Staley, M. H. Baumann, R. B. Rothman, and W. L. Hearn. Identification of a primary metabolite of ibogaine that targets serotonin transporters and elevates serotonin. Life Sci. 57(3):PL45–PL50 (1995).
R. S. Obach, J. Pablo, and D. C. Mash. Cytochrome P4502D6 catalyzes the O-demethylation of the psychoactive alkaloid ibogaine to 12-hydroxyibogamine. Drug Metab. Dispos. 26(8):764–768 (1998).
R. Ayesh, S. Dawling, A. Hayler, et al. Comparative effects of the diastereoisomers, quinine and quinidine in producing phenocopy debrisoquine poor metabolisers (PMs) in healthy volunteers. Chirality. 3(1):14–18 (1991).
J. Desmeules, M. P. Gascon, P. Dayer, and M. Magistris. Impact of environmental and genetic factors on codeine analgesia. Eur. J. Clin. Pharmacol. 41(1):23–26 (1991).
J. A. Desmeules, M. K. Oestreicher, V. Piguet, A. F. Allaz, and P. Dayer. Contribution of cytochrome P-4502D6 phenotype to the neuromodulatory effects of dextromethorphan. J. Pharmacol. Exp. Ther. 288(2):607–612 (1999).
Acknowledgements
The project described was supported by Grant number R01DA021172 from the National Institute on Drug Abuse. The author also thanks Drs. Ho-Leung Fung and Robert M. Straubinger for their helpful suggestions and discussions.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This is an open access article distributed under the terms of the Creative Commons Attribution Noncommercial License ( https://creativecommons.org/licenses/by-nc/2.0 ), which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
About this article
Cite this article
Yu, AM. Indolealkylamines: Biotransformations and Potential Drug–Drug Interactions. AAPS J 10, 242–253 (2008). https://doi.org/10.1208/s12248-008-9028-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1208/s12248-008-9028-5