Abstract
OBJECTIVE: To investigate patient preferences for a patient-centered or a biomedical communication style.
DESIGN: Randomized study.
SETTING: Urgent care and ambulatory medicine clinics in an academic medical center.
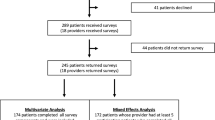
PARTICIPANTS: We recruited 250 English-speaking adult patients, excluding patients whose medical illnesses prevented evaluation of the study intervention.
INTERVENTION: Participants watched one of three videotaped scenarios of simulated patient-physician discussions of complementary and alternative medicine (CAM). Each participant watched two versions of the scenario (biomedical vs. patient-centered communication style) and completed written and oral questionnaires to assess outcome measurements.
MEASUREMENTS AND MAIN RESULTS: Main outcome measures were 1) preferences for a patient-centered versus a biomedical communication style; and 2) predictors of communication style preference. Participants who preferred the patient-centered style (69%; 95% confidence interval [CI], 63 to 75) tended to be younger (82% [51/62] for age < 30; 68% [100/148] for ages 30–59; 55% [21/38] for age > 59; P<.03), more educated (76% [54/71] for postcollege education; 73% [94/128] for some college; 49% [23/47] for high school only; P=.003), use CAM (75% [140/188] vs. 55% [33/60] for non-users; P=.006), and have a patient-centered physician (88% [74/84] vs. 30% [16/54] for those with a biomedical physician; P<.0001). On multivariate analysis, factors independently associated with preferring the patient-centered style included younger age, use of herbal CAM, having a patient-centered physician, and rating a “doctor’s interest in you as a person” as “very important.”
CONCLUSIONS: Given that a significant proportion of patients prefer a biomedical communication style, practicing physicians and medical educators should strive for flexible approaches to physician-patient communication.
Similar content being viewed by others
References
Lipkin M, Putnam SM, Lazare A. The Medical Interview: Clinical Care, Education, and Research. New York, NY: Springer-Verlag; 1995.
Stewart MA. Effective physician-patient communication and health outcomes: a review. CMAJ. 1995;152:1423–33.
Platt FW, Gaspar DL, Coulehan JL, et al. “Tell me about yourself”: the patient-centered interview. Ann Intern Med. 2001;134:1079–85.
Williams S, Weinman J, Dale J. Doctor-patient communication and patient satisfaction: a review. Fam Pract. 1998;15:480–92.
Kinnersley P, Stott N, Peters TJ, Harvey I. The patient-centredness of consultations and outcome in primary care. Br J Gen Pract. 1999;49:711–16.
Kinmonth AL, Woodcock A, Griffin S, Spiegal N, Campbell MJ. Randomised controlled trial of patient centred care of diabetes in general practice: impact on current wellbeing and future disease risk. The Diabetes Care from Diagnosis Research Team. BMJ. 1998;317:1202–8.
Rosenberg EE, Lussier MT, Beaudoin C. Lessons for clinicians from physician-patient communication literature. Arch Fam Med. 1997;6:279–83.
Safran DG, Taira DA, Rogers WH, Kosinski M, Ware JE, Tarlov AR. Linking primary care performance to outcomes of care. J Fam Pract. 1998;47:213–20.
Rao JK, Weinberger M, Kroenke K. Visit-specific expectations and patient-centered outcomes: a literature review. Arch Fam Med. 2000;9:1148–55.
Maisiak R, Austin JS, West SG, Heck L. The effect of person-centered counseling on the psychological status of persons with systemic lupus erythematosus or rheumatoid arthritis: a randomized, controlled trial. Arthritis Care Res. 1996;9:60–6.
Kaplan SH, Greenfield S, Ware JE Jr. Assessing the effects of physician-patient interactions on the outcomes of chronic disease. Med Care. 1989;27(3 suppl):S110-S127.
Levinson W, Roter DL, Mullooly JP, Dull VT, Frankel RM. Physician-patient communication. The relationship with malpractice claims among primary care physicians and surgeons. JAMA. 1997;277:553–9.
Jackson JL, Kroenke K, Chamberlin J. Effects of physician awareness of symptom-related expectations and mental disorders. A controlled trial. Arch Fam Med. 1999;8:135–42.
Kravitz RL, Cope DW, Bhrany V, Leake B. Internal medicine patients’ expectations for care during office visits. J Gen Intern Med. 1994;9:75–81.
Kravitz RL, Callahan EJ, Azari R, Antonius D, Lewis CE. Assessing patients’ expectations in ambulatory medical practice. Does the measurement approach make a difference? J Gen Intern Med. 1997;12:67–72.
Krupat E, Rosenkranz SL, Yeager CM, Barnard K, Putnam SM, Inui TS. The practice orientations of physicians and patients: the effect of doctor-patient congruence on satisfaction. Patient Educ Couns. 2000;39:49–59.
Stewart M, Brown JB, Donner A, et al. The impact of patient-centered care on outcomes. J Fam Pract. 2000;49:796–804.
Levinson W, Roter D. The effects of two continuing medical education programs on communication skills of practicing primary care physicians. J Gen Intern Med. 1993;8:318–24.
Krupat E, Bell RA, Kravitz RL, Thom D, Azari R. When physicians and patients think alike: patient-centered beliefs and their impact on satisfaction and trust. J Fam Pract. 2001;50:1057–62.
Smith RC, Lyles JS, Mettler J, et al. The effectiveness of intensive training for residents in interviewing. A randomized, controlled study. Ann Intern Med. 1998;128:118–26.
Brown JB, Boles M, Mullooly JP, Levinson W. Effect of clinician communication skills training on patient satisfaction. A randomized, controlled trial. Ann Intern Med. 1999;131:822–9.
McKinstry B. Do patients wish to be involved in decision making in the consultation? A cross sectional survey with video vignettes. BMJ. 2000;321:867–71.
Eisenberg DM, Kessler RC, Foster C, Norlock FE, Calkins DR, Delbanco TL. Unconventional medicine in the United States. Prevalence, costs, and patterns of use. N Engl J Med. 1993;328:246–52.
Eisenberg DM, Davis RB, Ettner SL, et al. Trends in alternative medicine use in the United States, 1990–1997: results of a follow-up national survey. JAMA. 1998;280:1569–75.
Wolsko PM, Eisenberg DM, Davis RB, Ettner SL, Phillips RS. Insurance coverage, medical conditions, and visits to alternative medicine providers: results of a national survey. Arch Intern Med. 2002;162:281–7.
Wolsko PM, Eisenberg DM, Davis RB, Phillips RS. Use of mind-body medical therapies. J Gen Intern Med. 2004;19:43–50.
Foster DF, Phillips RS, Hamel MB, Eisenberg DM. Alternative medicine use in older Americans. J Am Geriatr Soc. 2000;48:1560–5.
Ernst E. The risk-benefit profile of commonly used herbal therapies: Ginkgo, St. John’s Wort, Ginseng, Echinacea, Saw Palmetto, and Kava. Ann Intern Med. 2002;136:42–53.
Piscitelli SC, Burstein AH, Chaitt D, Alfaro RM, Falloon J. Indinavir concentrations and St. John’s wort. Lancet. 2000;355:547–8.
Verhoef MJ, Hagen N, Pelletier G, Forsyth P. Alternative therapy use in neurologic diseases: use in brain tumor patients. Neurology. 1999;52:617–22.
Paltiel O, Avitzour M, Peretz T, et al. Determinants of the use of complementary therapies by patients with cancer. J Clin Oncol. 2001;19:2439–48.
Boon H, Brown J, Gavin A. What are the experiences of women with breast cancer as they decide whether to use complementary/alternative medicine? West J Med. 2000;173:39.
Singh N, Squier C, Sivek C, Nguyen MH, Wagener M, Yu VL. Determinants of nontraditional therapy use in patients with HIV infection. A prospective study. Arch Intern Med. 1996;156:197–201.
Burstein HJ, Gelber S, Guadagnoli E, Weeks JC. Use of alternative medicine by women with early-stage breast cancer. N Engl J Med. 1999;340:1733–9.
Holland JC. Use of alternative medicine—a marker for distress? N Engl J Med. 1999;340:1758–9.
Perlman AI, Eisenberg DM, Panush RS. Talking with patients about alternative and complementary medicine. Rheum Dis Clin North Am. 1999;25:815–22.
Sugarman J, Burk L. Physicians’ ethical obligations regarding alternative medicine. JAMA. 1998;280:1623–5.
Eisenberg DM. Advising patients who seek alternative medical therapies. Ann Intern Med. 1997;127:61–9.
Patterson RE, Neuhouser ML, Hedderson MM, et al. Types of alternative medicine used by patients with breast, colon, or prostate cancer: predictors, motives, and costs. J Altern Complement Med. 2002;8:477–85.
Lazar JS, O’Connor BB. Talking with patients about their use of alternative therapies. Prim Care. 1997;24:699–714.
Brown J, Stewart M, McCracken E, McWhinney IR, Levenstein J. The patient-centred clinical method. 2. Definition and application. Fam Pract. 1986;3:75–9.
Roter DL, Stewart M, Putnam SM, Lipkin M Jr, Stiles W, Inui TS. Communication patterns of primary care physicians. JAMA. 1997;277:350–6.
Brown J, Stewart M, Ryan BL. Assessing Communication Between Patients and Physicians: The Measure of Patient-centered Communication (MPCC). London, Ontario: Centre for Studies in Family Medicine; 2001.
Wolf MH, Putnam SM, James SA, Stiles WB. The Medical Interview Satisfaction Scale: development of a scale to measure patient perceptions of physician behavior. J Behav Med. 1978;1:391–401.
Hulley SB. Designing Clinical Research: An Epidemiologic Approach. 2nd ed. Philadelphia, Pa: Lippincott Williams & Wilkins; 2001.
Hosmer DW, Lemeshow S. Applied Logistic Regression. New York, NY: Wiley; 1989.
Krupat E, Yeager CM, Putnam SM. Patient role orientations, doctor-patient fit, and visit satisfaction. Psychol Health. 2000;15:707–19.
Parker PA, Baile WF, de Moor C, Lenzi R, Kudelka AP, Cohen L. Breaking bad news about cancer: patients’ preferences for communication. J Clin Oncol. 2001;19:2049–56.
Benbassat J, Pilpel D, Tidhar M. Patients’ preferences for participation in clinical decision making: a review of published surveys. Behav Med. 1998;24:81–8.
Schmittdiel J, Grumbach K, Selby JV, Quesenberry CP Jr. Effect of physician and patient gender concordance on patient satisfaction and preventive care practices. J Gen Intern Med. 2000;15:761–9.
Dowsett SM, Saul JL, Butow PN, et al. Communication styles in the cancer consultation: preferences for a patient-centred approach. Psychooncology. 2000;9:147–56.
Savage R, Armstrong D. Effect of a general practitioner’s consulting style on patients’ satisfaction: a controlled study. BMJ. 1990;301:968–70.
Hsu J, Schmittdiel J, Krupat E, et al. Patient choice. J Gen Intern Med. 2003;18:319–25.
Roter D, Hall JA. Doctors Talking with Patients/Patients Talking with Doctors: Improving Communication in Medical Visits. Westport, Conn: Auburn House; 1992.
Kaplan RM, Hammel B, Schimmel LE. Patient information processing and the decision to accept treatment. J Soc Behav Pers. 1985;1:113–20.
Greene MG, Adelman R, Charon R, Hoffman S. Ageism in the medical encounter: an exploratory study of the doctor-elderly patient relationship. Lang Commun. 1986;6:113–24.
Waitzkin H. Information giving in medical care. J Health Soc Behav. 1985;26:81–101.
Hall JA, Stein TS, Roter DL, Rieser N. Inaccuracies in physicians’ perceptions of their patients. Med Care. 1999;37:1164–8.
Golin C, DiMatteo MR, Duan N, Leake B, Gelberg L. Impoverished diabetic patients whose doctors facilitate their participation in medical decision making are more satisfied with their care. J Gen Intern Med. 2002;17:857–66.
Tennstedt SL. Empowering older patients to communicate more effectively in the medical encounter. Clin Geriatr Med. 2000;16:61–70, ix.
Brody DS, Miller SM, Lerman CE, Smith DG, Caputo GC. Patient perception of involvement in medical care: relationship to illness attitudes and outcomes. J Gen Intern Med. 1989;4:506–11.
Roter DL, Hall JA, Kern DE, Barker LR, Cole KA, Roca RP. Improving physicians’ interviewing skills and reducing patients’ emotional distress. A randomized clinical trial. Arch Intern Med. 1995;155:1877–84.
Lo B. Resolving Ethical Dilemmas: A Guide for Clinicians. 2nd ed. Philadelphia, Pa: Lippincott Williams & Wilkins; 2000.
Lazare A, Putnam SM, Lipkin M. The three functions of the medical interview. In: Lipkin M, Putnam SM, Lazare A, eds. The Medical Interview: Clinical Care, Education, and Research. New York, NY: Springer-Verlag; 1995:3–19.
Beckman HB, Frankel RM. The effect of physician behavior on the collection of data. Ann Intern Med. 1984;101:692–6.
Burack RC, Carpenter RR. The predictive value of the presenting complaint. J Fam Pract. 1983;16:749–54.
Floyd M, Lang F, Beine KL, McCord E. Evaluating interviewing techniques for the sexual practices history. Use of video trigger tapes to assess patient comfort. Arch Fam Med. 1999;8:218–23.
Gmel G, Lokosha O. Self-reported frequency of drinking assessed with a closed- or open-ended question format: a split-sample study in Switzerland. J Stud Alcohol. 2000;61:450–4.
Ivis FJ, Bondy SJ, Adlaf EM. The effect of question structure on self-reports of heavy drinking: closed-ended versus open-ended questions. J Stud Alcohol. 1997;58:622–4.
Devine DA, Fernald PS. Outcome effects of receiving a preferred, randomly assigned, or non-preferred therapy. J Consult Clin Psych. 1973;41:104–7.
Oberst MT. Methodology in behavioral and psychosocial cancer research. Patients’ perceptions of care. Measurement of quality and satisfaction. Cancer. 1984;53(10 suppl):2366–75.
Brown R, Dunn S, Butow P. Meeting patient expectations in the cancer consultation. Ann Oncol. 1997;8:877–82.
Gerbert B, Berg-Smith S, Mancuso M, et al. Video study of physician selection: preferences in the face of diversity. J Fam Pract. 2003;52:552–9.
Baddeley AD. The Psychology of Memory. New York, NY: Basic Books; 1976.
Capitani E, Della Sala S, Logie RH, Spinnler H. Recency, primacy, and memory: reappraising and standardising the serial position curve. Cortex. 1992;28:315–42.
Yunker RM, Levine MK, Sajid AW. Freestanding emergency centers and the patient population of internists. South Med J. 1986;79:424–7.
Yunker RM, Levine MK, Sajid AW. Free-standing emergency centers and the patient population of family physicians. J Fam Pract. 1985;21:63–9.
Rylko-Bauer B. The development and use of freestanding emergency centers: a review of the literature. Med Care Rev. 1988;45:129–63.
Lo B, Quill T, Tulsky J. Discussing palliative care with patients. ACP-ASIM End-of-life Care Consensus Panel. American College of Physicians-American Society of Internal Medicine. Ann Intern Med. 1999;130:744–9.
Towle A, Godolphin W. Framework for teaching and learning informed shared decision making. BMJ. 1999;319:766–71.
Sheridan SL, Harris RP, Woolf SH. Shared decision making about screening and chemoprevention. A suggested approach from the U.S. Preventive Services Task Force. Am J Prev Med. 2004;26:56–66.
Platt FW, Gordon GH. Field Guide to the Difficult Patient Interview. Philadelphia, Pa: Lippincott Williams & Wilkins; 1999.
Author information
Authors and Affiliations
Corresponding author
Additional information
This work was supported by the Robert Wood Johnson Foundation Initiative on Strengthening the Patient-Provider Relationship.
Rights and permissions
About this article
Cite this article
Swenson, S.L., Buell, S., Zettler, P. et al. Patient-centered communication. J GEN INTERN MED 19, 1069–1079 (2004). https://doi.org/10.1111/j.1525-1497.2004.30384.x
Issue Date:
DOI: https://doi.org/10.1111/j.1525-1497.2004.30384.x