Abstract
Reducing oxidative stress (ROS) have been demonstrated effective for steroid-induced osteonecrosis of the femoral head (steroid-induced ONFH). Selenium (Se) plays an important role in suppressing oxidative stress and has huge potential in ONFH treatments. However the Se has a narrow margin between beneficial and toxic effects which make it hard for therapy use in vivo. In order to make the deficiency up, a control release of Se (Se@SiO2) were realized by nanotechnology modification. Porous Se@SiO2 nanocomposites have favorable biocompatibility and can reduced the ROS damage effectively. In vitro, the cck-8 analysis, terminal dexynucleotidyl transferase (TdT)-mediated dUTP nick end labeling (TUNEL) stain and flow cytometry analysis showed rare negative influence by porous Se@SiO2 nanocomposites but significantly protective effect against H2O2 by reducing ROS level (detected by DCFH-DA). In vivo, the biosafety of porous Se@SiO2 nanocomposites were confirmed by the serum biochemistry, the ROS level in serum were significantly reduced and the curative effect were confirmed by Micro CT scan, serum Elisa assay (inflammatory factors), Western blotting (quantitative measurement of ONFH) and HE staining. It is expected that the porous Se@SiO2 nanocomposites may prevent steroid-induced ONFH by reducing oxidative stress.
Similar content being viewed by others
Introduction
Steroid as an irreplaceable medicaments is used to treat diseases including rheumatoid arthritis, systemic lupus erythematosus, acute lymphoblastic leukaemia and so on. However, steroid-induced osteonecrosis of the femoral head (ONFH) has been one of the most serious diseases for orthopedists, and a hip replacement is the only treatment option at the terminal stage1. Epidemiology studies in East Asia show that 47.4% of all cases diagnosed as non-traumatic ONFH were directly associated with steroids2. Considering the serious consequences3 and economic costs4 incurred by ONFH, it is necessary to find new treatments. However, although numerous hypotheses for the pathogenesis of this disease, including lipid metabolism disorder, intravascular coagulation, microvascular injury, and intraosseous hypertension5,6,7,8, have been proposed, the exact mechanism of steroid-induced osteonecrosis of the femoral head (ONFH) still remains unclear. Yet, among all the risk factors reported, oxidative stress disorders may be one of the most common one participated9, which may benefit more when intervened.
Oxidative stress is defined as an imbalance between the production of oxidants (free radicals or reactive oxygen species, ROS) and their elimination by protective mechanisms, such as antioxidants10. ROS have been demonstrated to be closely related to ONFH11. Not only the wide influence oxidative stress disorders have in pulmonary, neurodegenerative, autoimmune diseases, as well as in metabolic disorders, cancer, and aging12,13,14. But also the direct evidence that chronic use of methylprednisolone may increase ROS damage15. In addition, it has been hypothesized that osteonecrosis is produced by the ischemic change accompanying the compartment pressure load in the marrow, where degeneration and necrosis may occur simultaneously with oxidative stress16. Besides, antioxidants such as Coenzyme Q10 (CoQ10)17 and hydrogen-rich saline18, have already been proved to be therapeutic for steroid-induced osteonecrosis in rats. While stem cell factor (SCF)19 and grape seed proanthocyanidin proved protective by reducing oxidative stress20. Based on the studies mentioned above, it is widely suspected that oxidative stress leads to osteonecrosis of ONFH21. Effective, selective, multifunctional drugs suppressing oxidative stress have tremendous potential in ONFH treatment, which can be realized by nanocomposites.
The choice of structural composition and compound method shall be very careful. As an essential trace mineral22, selenium (Se) plays an important role in suppressing oxidative stress23,24,25 and has been proved interrelationship with DNA damage and oxidative stress26. Se deficiency may induce oxidative stress and endoplasmic reticulum stress27 in some special cases (such as the use of ECMO)28. In contrast, Se’s essential interrelationship with coenzyme Q10 in cardiovascular diseases29 and its preventive effect in combination with vitamin E for prostate cancers30 suggested a great potential for the prevention of ONFH. Which made Se an ideal composition in ONFH treatment.
Compared with other reported ROS scavengers, Se is more stable and economical than a biological product. However, its toxicity cannot be ignored31 because Se has a narrow margin between beneficial and toxic effects32. After modification by nanotechnology, nano-Se can serve as an antioxidant with reduced risk of selenium toxicity33. The size of nanoparticles plays an important role in their biological activity: as expected, 5–200 nm Nano-Se can directly scavenge free radicals in vitro in a size-dependent fashion34. For further developments of nano-se therapy, porous structure of Se@SiO2 were synthesized. Our previous research showed that porous Se@SiO2 nanocomposites can be used as a delivery system for the controlled-release of Se nanoparticles35, which can slowly release a beneficial amount of Se over a long period of time. Moreover, Se nanocrystals exhibit a higher biological activity and lower toxicity than other forms33,36,37. Thus, porous Se@SiO2 nanocomposites may be a safe and ideal source of Se. Meanwhile, the porous structure Se@SiO2 nanocomposites have made them an ideal deliver system for multifunctional drug therapy which represents a promising, safe and effective way for ONFH treatments. In order to explain the mechanism porous Se@SiO2 nanocomposites have, the combination therapies are not considered in this study.
The following three aspects of porous Se@SiO2 nanocomposites were evaluated: the identification and biosecurity, the ROS-suppressing capacity and the therapeutic effects associated. For mechanism explain, experiments were repeated in vitro and in vivo.
Experimental
Synthesis and characterization of material
Porous Se@SiO2 nanocomposites were prepared according to our previous method35, and characterized by means of a D/max-2550 PC X-ray diffractometer (XRD; Rigaku, Cu-Kα radiation), a transmission electron microscopy (TEM; JEM-2100F). Besides the control release of Se were repeated at PH 7.4. As-synthesized porous Se@SiO2 nanocomposites were dispersed in deionized water for further use.
Culture and identification of the cartilage cells
Two male SD rats, weighing 150 g, were sacrificed by CO2 asphyxiation and disinfected in 75% alcohol for 10 min. The head of the femur was exposed under aseptic conditions. Then, the total articular cartilage was isolated, collected, cut into 1 mm3 pieces, and then digested with 0.2% collagenase type II (GIBCO Grand Island, NY, USA) for 30 min, and filtered through a 70-μm cell strainer and washed 3 times with phosphate-buffered saline (PBS) at 300 × g for 5 min. After that, the collected cells were seeded into 100-mm tissue culture dishes and grown in DMEM/F-12 (GIBCO Grand Island, NY, USA) with 10% FBS (GIBCO Grand Island, NY, USA), 100 μg/ML streptomycin and 100 U/ML penicillin (GIBCO Grand Island, NY, USA) in a 37 °C, 5% CO2 environment. The culture medium was changed every 2–3 days. The cells were digested with 0.25% trypsin (GIBCO Grand Island, NY, USA) and passaged when they reached 80–90% confluency. Cells at passage 3 in culture were identified by immunofluorescence staining with collagenase type I (Santa Cruz, CA, USA) and aggrecan (Santa Cruz, CA, USA) before being used for subsequent experiments.
Biocompatibility test and direct flow cytometry analysis
The cartilage cells were diluted into single cell suspensions and seeded into 96-well plates (1 × 104 cells/well) with the culture medium. After 24 hours, the upper medium was exchanged with a medium containing different concentrations of porous Se@SiO2 nanocomposites that were dispersed by ultrasound. After additional 24 hours, a 10% cck-8 (DOJINDO, Japan) solution was added to each well, and the plates were incubated for 1 hour in the incubator. Then, the absorbance was measured at 490 nm using a micro-plate reader. Before a comparison, the absorbances were normalized to control groups without porous Se@SiO2 nanocomposites.
Before the flow cytometry analysis, the cartilage cells were cultured with the porous Se@SiO2 nanocomposites at a concentration of 40 μg/ML based on the results of the cck-8 assay for 24 hours. Then, the cartilage cells were digested and washed twice with blinding buffer (BD, USA) and analyzed directly on an Accuri C6 at the fluorescence channels for FITC, PE/PI, 7AAD and APC. For the apoptosis analysis, the cells were incubated with 5 μL of APC-Annexin V and 5 μL of PI for 15 min at room temperature (25 °C) in the dark, and then 400 μL of 1 × Binding Buffer was added to each tube. The cell suspension was then analyzed on an Accuri C6.
Protection by the porous Se@SiO2 nanocomposites as assessed by suppression of ROS
H2O2 was considered a classical simulation of ROS38 and widely used39,40,41 which was also used in this experiment.
Cartilage cells were plated into 6-well plates (1 × 106 cells/well) and were then pre-stimulated by the porous Se@SiO2 nanocomposites in a culture medium at a concentration of 0 μg/ML, 20 μg/ML, and 40 μg/ML for 24 hours, respectively. Subsequently, the cells in the plates and the EP tubes (collected by digestion for the flow cytometry test) were stimulated with 50 μM H2O2 (Sigma-Aldrich St. Louis, MO, USA) in PBS (1.5 mL/well, 500 μL/EP tube). 30 min later, DCFH-DA at its working concentration was added after 2 washes with PBS (1000 rpm, 5 min for intervention in EP tube). After 15 min of staining at 37 °C, the plates were directly observed with a fluorescence microscope (Leica, German). Cells in the EP tube were analyzed by flow cytometry.
For the cell supernatant tests, DF-12 (1.5 mL/well) was added to the 6-well plates after the H2O2 stimulation. IL-1β, IL-4 and IL-6 were assessed 24 hours later by Elisa Kits (Neobioscience, China).
Protection by the porous Se@SiO2 nanocomposites as assessed by apoptosis tests and cell activity
For the TUNEL assay, the treatment group, with or without a 24-hour pre-stimulation with 40 μg/ML of the porous Se@SiO2 nanocomposites, was stimulated with 200 μM H2O2 in DF-12, while the control group was stimulated with DF-12 for 24 hours. The TUNEL assay was then used to assess DNA fragmentation by a commercially available kit (In Situ Cell Death Detection Kit, fluorescein, Roche, Indianapolis, IN, USA). Briefly, the fixed cells on the slides were washed three times for 5 min with PBS and permeabilized with 0.1% (v/v) Triton X-100 containing 0.1% (w/v) sodium citrate for 2 min. The samples were then incubated in 50 μL of TUNEL reaction mixture for 1 h at 37 °C in a dark and humidified atmosphere. Subsequently, 6-diamidino-2-phenylindole (DAPI) was used for staining of the nuclei. Positive TUNEL staining was observed under a fluorescence microscope. The sperm TUNEL index was evaluated by determining the ratio of the number of TUNEL-positive cells to that of total cells in each of the ten fields of vision.
For the flow cytometry analysis, cells received pre-stimulation or no stimulation with the porous Se@SiO2 nanocomposites in 6-well plates for 24 hours, and then 200 μM and 500 μM H2O2 in DF-12 were each used separately as inducements. After 24 hours, the suspension cells and adherent cells were collected and measured with an annexin V/APC apoptosis detection kit (eBioscience, USA). Briefly, the cells were trypsinized and pelleted by centrifugation, washed once with ice-cold PBS, and resuspended in 1 × Binding Buffer at a concentration of 1 × 106 cells/ML, from which 100 μL of cell suspension (1 × 105 cells) was transferred to a 1.5 mL EP tube. Staining was then completed that is outlined above.
For the cck-8 assay, the cartilage cells were diluted into single cell suspensions and seeded into 96-well plates (1 × 104cells/well) with a culture medium. After 24 hours, the upper medium of the experiment group was exchanged with a medium with 40 μg/mL of the porous Se@SiO2 nanocomposites, while the control group had a replacement of a medium without the porous Se@SiO2 nanocomposites. After a 24-hour stimulation, different concentrations of H2O2 were used for stimulation. After additional 24 hours, a 10% cck-8 (DOJINDO, Japan) solution was added to each well, and the plates were incubated for 1–2 hours in the incubator. Then, the absorbance was measured at 490 nm using a micro-plate reader.
Animal experiments
Animal preparation
This study was performed following the National Institutes of Health guidelines for the use of experimental animals, and all animal protocols were approved by the Institutional Animal Care and Use Committee of Shanghai Jiaotong University. Male Sprague-Dawley (SD) rats (weight 250–300 g; age of 12 months; SPF class) were obtained from the experimental animal center of Shanghai Jiao Tong University. The rats were bred and maintained under a 12/12-hour light-dark cycle with free access to food and water. The room temperature was set to 18 °C–25 °C, and the relative humidity was set to 40–60%.
Testing changes in ROS levels in serum after stimulation by the porous Se@SiO2 nanocomposites in vivo
Prior to the experiments on the ONFH model, the porous Se@SiO2 nanocomposites were directly injected into adult rats intraperitoneally at doses of 0 mg/kg, 1 mg/kg, 2 mg/kg and 4 mg/kg. 24 hours later, the serum from each group was cultured as outlined in a previous study42, and the ROS (Nanjing Jiancheng, China) was measured with an Elisa kit.
ONFH animal model establishment, treatments and sample collection
According to a previous study43, an early stage SANFH model was induced using a combination of lipopolysaccharides (LPS) and methylprednisolone (MPS). 36 rats were randomly divided into a control group (group A), model group (group B) and porous Se@SiO2 nanocomposite group (group C), each consisting of 12 rats. Male SD rats from group B and group C were intravenously injected with LPS (10 μg/kg body weight). After 24 hours, three injections of MPS (20 mg/kg body weight) were administered intramuscularly every 24 h for 5 days. To prevent infection, each rat was intramuscularly injected with 100,000 U of penicillin. Based on the toxicity study data of selenium nanoparticles in rats37 and control release capacity of porous Se@SiO2 nanocomposite35. The rats in group C were injected intraperitoneally with 1 mg/kg of the porous Se@SiO2 nanocomposites per day for 14 days, beginning 4 weeks after the MPS administration. The model group (group A) was fed and housed under identical conditions but received saline injections.
The rats in all groups were sacrificed by an overdose of anesthesia at 8 weeks after the first MPS injection, and the femoral heads and blood samples were harvested. Blood samples from all groups were collected in containers without anticoagulant, thus allowing clot formation. The blood was centrifuged at 1,200× g for 10 minutes. The serum was stored at −80 °C until further analysis. The left femoral heads of all rats were preserved in a −70 °C cryogenic freezer immediately after sacrifice, and the proteins were isolated for Western blot analysis. The right femoral heads were collected and immediately fixed with 10% formalin (0.1 M phosphate buffer, pH 7.4) at 4 °C for 24 hours. Then, the samples were used for Micro CT scanning and HE staining tests following previous protocols44.
Evaluation techniques
Micro CT procedure
According to a previous study44, a Micro CT (GE Healthcare Biosciences, Piscataway, NJ, USA) was used to detect changes in the excised femoral head sample and the trabecular bone. Bone volume (BV), bone surface (BS), trabecular thickness (Tb.N), trabecular number (Tb.Sp) and trabecular separation (Tb.Th) were calculated.
Western blot analysis
The protein expression levels of IL-1β45, collagen II46, MMP-1347 and aggrecan48 in the femoral head tissues obtained from rats in the different groups were detected by Western blot analysis. The Western blot protocol and semi-quantitative analysis were carried out following the protocols of a previous study43. Antibodies, obtained from Santa Cruz Biotechnology (Santa Cruz, CA, USA), against the following were used: IL-1β, collagen type II, MMP-13, aggrecan, and GAPDH.
Hematoxylin-eosin staining
According to a previous study49, the femoral heads harvested from the animals were fixed with 4% formalin and were then washed with PBS buffer. Sequentially, they were decalcified with 10% EDTA and neutralized with sodium sulfate buffer for approximately 4 weeks. After decalcification, the tissues were embedded in paraffin and cut in the coronal plane into 4-μm thick sections with a microtome. Then, H-E staining was processed for the micro-structure observation.
Serum Biochemistry
Serum from each groups were tested. The activities of blood serum marker enzymes, such as alanine transaminase (ALT), alkaline phosphatase (ALP), aspartate transaminase (AST), creatinine, and urea, were measured using a Roche kit (Penzberg, Germany) and analyzed spectrophotometrically using the Hitachi Analytical Instrument (Roche Diagnostic GmbH, Mannheim, Germany).
Statistical analysis
Quantitative data are expressed as the mean ± SD. Data were analyzed using SPSS 21.0 software (IBM, Armonk, NY, USA). For comparisons of means among multiple groups, one-way ANOVAs followed by LSD tests was performed. Differences were considered statistically significant when P < 0.05.
Results
A series of tests demonstrated that the nanocomposites used in the following experiments were the porous Se@SiO2 nanocomposites. The phase structure of the resulting nanocomposites was examined by the XRD pattern, as shown in Fig. 1a. Several well-defined characteristic peaks, such as (100), (011), (110) and (012), exhibited the hexagonal phase, referenced by the standard Se phase (JCPDS card no. 65-1876). In addition, the XRD pattern of the Se@SiO2 nanocomposites showed a steady increase in the low angle region, which is due to amorphous silica. It can be observed in Fig. 1b that the homogeneous nanocomposites have a diameter of about 55 nm, which many very small nanoparticles (less than 5 nm) were interspersed from the center to the surface. The dispersed nanoparticles have an interplanar spacing of 0.218 nm, matching the spacing for the (110) crystal planes of the standard hexagonal Se (Fig. 1b inset), which further confirmed that the small nanoparticles dispersed in the silica were Se nanocrystals. After treatment with hot water, the porous Se@SiO2 nanocomposites were formed (Fig. 1c,d). Our previous characterization of BET showed that the Se@SiO2 nanocomposites are porous35. The PVP (pyrrolidinovalerophenone) had permeated into the silica shells, and the channels were distributed in the Se@SiO2 nanocomposites, leading to the slow release of very small nanoparticles from the porous Se@SiO2 nanocomposites. Meanwhile, the release capacity were re-confirmed (Fig. S1).
The characterization of the Se@SiO2 nanocomposites: (a) XRD pattern of the Se@SiO2 nanocomposites and the standard hexagonal phase of Se (JCPDS card no: 65-1876). (b) TEM image of as-prepared Se@SiO2 nanocomposites (inset: HRTEM of a Se@SiO2 nanocomposite). (c) Low magnification and (d) high magnification of the porous Se@SiO2 nanocomposites.
Cells were identified as cartilage cells by staining with aggrecan and collagenase type I (Fig. 2a,b). Co-culturing with the porous Se@SiO2 nanocomposites was demonstrated to have no significant influence on the flow cytometry (Figs S2 and S3) and proved to be safe by flow cytometry at a concentration of 40 μg/ML (Figs 2c, S4). The porous Se@SiO2 nanocomposites showed no significant cytostatic action under a concentration of 40 μg/ML compared with the control group (Fig. 2d).
Identification of cartilage cells and confirmation of biosafety of the porous Se@SiO2 nanocomposites: (a) Immunofluorescence staining of aggrecan (200×). (b) Immunofluorescence staining of collagenase type I (200×). (c) Normalized cck-8 absorbance at 490 nm of cells cultured with different porous Se@SiO2 nanocomposite concentrations. Obviously toxicity only occurs over 100 μg/ML. (d) Flow cytometry of cartilage cells stimulated with 40 μg/ML of the porous Se@SiO2 nanocomposites for 24 hours. No significant differences indicated (P > 0.05).
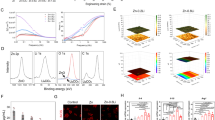
The fluorescence microscopic observation indicated that pre-stimulation with the porous Se@SiO2 nanocomposites might significantly decrease the expression of the ROS (Fig. 3) after H2O2 exposure, which was re-confirmed and quantitatively analyzed by flow cytometry analysis (Fig. S5). Pre-stimulation with the porous Se@SiO2 nanocomposites could significantly reduce the expression of IL-1β, IL-4 and IL-6 in a concentration-dependent manner (Fig. S6, P < 0.05).
DCFH staining was used for ROS detection in cartilage cells pre-stimulated with and without the porous Se@SiO2 nanocompositesv (40 μg/ML for 24 hours pre-stimulation). ROS expression was indicated by the fluorescence intensity of DCFH (FITC). Pre-stimulated with the porous Se@SiO2 nanocomposites can significantly decrease ROS expression.
After 24 hours of stimulation with 200 μM H2O2, the cells pre-stimulated with 40 μg/ML of the porous Se@SiO2 nanocomposites demonstrated less damage than the control groups. The apoptosis analysis showed that the porous Se@SiO2 nanocomposites significantly decreased the apoptosis rates caused by H2O2 (Fig. 4a,b, *P < 0.05), which was re-confirmed by the flow cytometry analysis (Fig. S7, *P < 0.05) and the cck-8 assay (Fig. 4c, *P < 0.05) at different H2O2 concentrations.
(a) Staining of cartilage cells with DAPI, TUNEL and MERGE. (b) Statistical graph and analysis of TUNEL staining, Pre-stimulated with the porous Se@SiO2 nanocomposites can significantly decrease apoptosis rates induced by H2O2. *P < 0.05. (c) Normalized by control group the cell activity decreased along with the increasing H2O2 concentrations. Significant protection of the porous Se@SiO2 nanocomposites as reflected by the cck-8 assay P < 0.05.
After 24 hours through the intraperitoneal injection of the porous Se@SiO2 nanocomposites, the ROS levels in the serum were significantly decreased (Fig. S8, *P < 0.05 in comparison with the other groups). 8 weeks after the steroid injection, the weight of the rats was maintained at 426 ± 32 g, with no significant differences detected among the groups.
The porous Se@SiO2 nanocomposite treatment was performed for 4 weeks after the steroid exposure to avoid the possible influence of the model inducement. Under this situation, the protective role of the porous Se@SiO2 nanocomposites in the early stage of ONFH were evaluated.
A CT scan indicated the therapeutic effects of the Porous Se@SiO2nanocomposite treatment (Fig. 5), and the data analyses on the levels of the microstructural parameters showed significant differences (Fig. S9).
Serum ALT, ALP, AST, creatinine, and urea in each group had no significant differences (Table S1).
IL-1β and MMP-13 were classical damage indexes in cartilage reaches that can objectively evaluate the necrosis situation. While collagen type II and aggrecan were both constructional and functional protein in cartilage. The changes of these four protein assessed by Western blot analysis can fully reflect the specific situation. Western blot analysis for both subchondral bone and cartilage showed that the expression of IL-1β, collagen type II, MMP-13 and aggrecan increased in the model group. After the Porous Se@SiO2nanocomposite injection, expression significantly decreased (Figs 6 and 7, P < 0.05), except for collagen II expression in cartilage (Fig. 6). The blot is representative of subchondral bone, normalized to GAPDH, and statistical analysis was performed (n = 12, *P < 0.05) (b, d); the blot is representative of cartilage, normalized to GAPDH, and statistical analysis was performed (n = 12, *P < 0.05).
Hematoxylin-eosin staining were used for structural observation of the femur head. Serious destruction of the femur head was induced for 8 weeks after methylprednisolone administration. After the Porous Se@SiO2 nanocomposite injection, fewer necrotic areas (cavity beneath the cartilage surface) were detected (Fig. 8).
Discussion
Briefly, after Porous Se@SiO2 pre-stimulation before H2O2 exposure, ROS level were significantly decreased (Figs 3, S5), thus IL-1β, IL-4 and IL-6 levels were tested lower by Elisa (Fig. S6) and apoptosis rates decreased according to TUNEL staining (Fig. 4b) and flow cytometry analysis (Fig. S7). The cell activity were protected (Fig. 4c). In vivo, ONFH rat models were successfully established and Porous Se@SiO2 nanocomposites proved safe (Table S1) and effective by Micro CT scanning (Figs 5, S9), serum Elisa assay (Fig. S8), Western blotting (Figs 6 and 7) and HE staining (Fig. 8). The Porous Se@SiO2 nanocomposites proved medicative to steroid-induced ONFH by reducing oxidative stress.
Still, the mechanism of ONFH are still unclear, but ROS and ROS suppressing treatments indicated the close relationship oxidative stress have to ONFH. A newly reported review of hyperbaric oxygen therapy in the treatment of osteonecrosis of the femoral head confirmed the therapeutic function antioxidants have in ONFH50. Thus by decreasing the ROS levels, other elements should also have the capacity to retard the progress of ONFH. However, antioxidants, such as coenzyme Q10 (CoQ10), may lead to nausea, upset stomach or loss of appetite. In addition, hydrogen-rich saline is not stable enough, and stem cell factor (SCF) and grape seed proanthocyanidin are costly as standard treatments. Compare to which, thanks to the SiO2-coated structure, significant advantages Porous Se@SiO2 nanocomposites have in both economic and stability (room temperature store) are convinced.
Moreover, porous structure gave Se@SiO2 nanocomposites potentials to be multifunctional (combined with drugs) and made them slow-released. Controlled-release systems play special roles in disease treatment51,52. Compared to normal Se nanoparticles, Se in the Se@SiO2 nanocomposites is limited by SiO2. Accompanying the entrance of PVP into an aqueous solution, trace Se can be released into the solution35. By controlled-release, the porous Se@SiO2 nanocomposites may have advantages in biosafety (Fig. 2d) and in vivo stability. Because the process of ONFH is long and progressive53, the controlled-release capacity benefits the sustaining of the ROS inhibition. So, SiO2-coated ultrasmall Se particles may help to delay the onset or reduce the serious outcome of the ONFH.
The advantages and characteristics porous Se@SiO2 nanocomposites have made them an ideal therapy to ONFH. The possible mechanism may be the ROS suppressing. Nano-materials that can mediate the ROS expression are not unique; some function by direct contact, and some function by anti-bacterial properties54, while others help to maintain structural stability and improve bio-safety55, even help to induce the cell apoptosis program via the ROS56. However, the porous Se@SiO2 nanocomposites may not only reduce the expression of the ROS directly but also provide essential elements that help to comprise the intracellular pool against oxidative stress57,58. Accumulating evidence supports the idea that Se nanoparticles have antioxidant effects59. These effects have been shown to increase the activities of both GPX and glutathione S-transferase and induce less oxidative stress34,59. The same consequences were observed in this study, in which the porous Se@SiO2 nanocomposite simulation significantly decreased the ROS levels and improved the cells’ tolerance to H2O2 (Fig. 4), with the ROS levels in serum demonstrating the same consequence in vivo (Fig. S7). It also has been reported that by inhibiting the activation of the PI3K/AKT and ERK signaling pathways and endoplasmic reticulum stress, Se can suppress oxidative-stress-enhanced vascular smooth muscle cell calcification60, further reducing the levels of IL-1β, TNF- α, oxidative stress, and NF- κ B activation61. On the contrary, a diet with a Se deficiency weakens antioxidant capacity62. However, despite the acute side effects associated with toxicity63, pre-stimulation with porous Se@SiO2 nanocomposites did help to reduce the expression of IL-1β, IL-4, and IL-6 after exposure to H2O2 in a concentration-dependent manner (Fig. S5). This change matched the decreased IL-1β level in the femoral head (Figs 6 and 7).
This improvement was reflected not only by Micro CT (Fig. 5) and the histological images (Fig. 8) but also by the protein levels of tissue biopsies (Figs 6 and 7). In the CT imaging, a low attenuation section in the femoral head refers to collapse and necrosis. Observed in 3-dimensional images, after treatment by the porous Se@SiO2 nanocomposites, the percentage of low attenuation area was reduced. By a quantitative comparison (Fig. S8), significant differences were detected among these groups confirmed the curative effects. Meanwhile, the tissue biopsy directly showed the improvement in the femur head structure in treatment group (Fig. 8). Thus, it is receivable that after porous Se@SiO2 nanocomposite treatment, anatomic integrity of femoral head was maintained.
Western blot investigation showed a significant increase in IL-1β and MMP-13, which indicates that damage had occurred in the cartilage and subchondral bone, which decreased after the porous Se@SiO2 nanocomposite treatment. The expression of aggrecan and collagen type II indicated a compositional variation after steroid inducement, as their variation combined the structural and functional changes in the femoral head, which were also significantly recovered after the porous Se@SiO2 nanocomposite treatment. These results confirmed the local phenomenon and possible mechanism that ONFH may started with IL-1β and MMP-13 damages, influenced the structural and functional protein aggrecan and collagen type II and finally leads to necrosis (Fig. 6). By suppressing IL-1β and MMP-13, porous Se@SiO2 nanocomposites can significantly reduce the damage of ONFH.
However, in this experiment with the porous Se@SiO2 nanocomposites injection, only its possible function in the early stage of ONFH was tested, and the potential preventive effects of the porous Se@SiO2 nanocomposites, according to the basic function of ROS inhibition, were not demonstrated. For preventive treatment, it has to be proved that the porous Se@SiO2 nanocomposites have no influence on the therapeutic effects of the steroids. Another study system will be needed and will be reported in the future.
Conclusions
In summary, the porous Se@SiO2 nanocomposites could reduce the ROS levels, protect cells from H2O2-induced apoptosis and reduce inflammation by inhibiting oxidative stress. Same effects were observed in vivo and eventually demonstrated the significant protective effect in disease management.
The porous Se@SiO2 nanocomposites have advantages of stability, economy, and enormous multifunctional potentials compared to other methods. Therefore, make porous Se@SiO2 nanocomposites an ideal way to protect the femoral head from osteonecrosis after steroid inducement.
Additional Information
How to cite this article: Deng, G. et al. Treatment of steroid-induced osteonecrosis of the femoral head using porous Se@SiO2 nanocomposites to suppress reactive oxygen species. Sci. Rep. 7, 43914; doi: 10.1038/srep43914 (2017).
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
Issa, K., Pivec, R., Kapadia, B. H., Banerjee, S. & Mont, M. A. Osteonecrosis of the femoral head: the total hip replacement solution. Bone Joint J 95-b, 46–50 (2013).
Ikeuchi, K. et al. Epidemiology of nontraumatic osteonecrosis of the femoral head in Japan. Mod Rheumatol 25, 278–81 (2015).
Zalavras, C. G. & Lieberman, J. R. Osteonecrosis of the femoral head: evaluation and treatment. J Am Acad Orthop Surg 22, 455–64 (2014).
Watters, T. S. et al. Cost-effectiveness analysis of free vascularized fibular grafting for osteonecrosis of the femoral head. J Surg Orthop Adv 20, 158–67 (2011).
Matsui, M. et al. Experimental steroid-induced osteonecrosis in adult rabbits with hypersensitivity vasculitis. Clin Orthop Relat Res 61–72 (1992).
Saito, S., Inoue, A. & Ono, K. Intramedullary haemorrhage as a possible cause of avascular necrosis of the femoral head. The histology of 16 femoral heads at the silent stage. J Bone Joint Surg Br 69, 346–51 (1987).
Kawai, K., Tamaki, A. & Hirohata, K. Steroid-induced accumulation of lipid in the osteocytes of the rabbit femoral head. A histochemical and electron microscopic study. J Bone Joint Surg Am 67, 755–63 (1985).
Wang, G. J., Sweet, D. E., Reger, S. I. & Thompson, R. C. Fat-cell changes as a mechanism of avascular necrosis of the femoral head in cortisone-treated rabbits. J Bone Joint Surg Am 59, 729–35 (1977).
Puppel, K., Kapusta, A. & Kuczynska, B. The etiology of oxidative stress in the various species of animals, a review. J Sci Food Agric 95, 2179–84 (2015).
Nakamura, K., Nakajima, Y. & Nakamura, Y. Characterization of two similar differential tumor markers based on phosphofructokinase activity arising from the influence of cancer patient serum. Cancer Detect Prev 13, 239–50 (1988).
Ichiseki, T. et al. Osteonecrosis development in a novel rat model characterized by a single application of oxidative stress. Arthritis Rheum 63, 2138–41 (2011).
Latini, A. et al. D-2-hydroxyglutaric acid induces oxidative stress in cerebral cortex of young rats. Eur J Neurosci 17, 2017–22 (2003).
Warwick, E., Scourfield, A. & Quint, J. Systemic manifestations of chronic obstructive pulmonary disease. Br J Hosp Med (Lond) 76, 324–9 (2015).
Mizushima, N., Levine, B., Cuervo, A. M. & Klionsky, D. J. Autophagy fights disease through cellular self-digestion. Nature 451, 1069–75 (2008).
Torres, R. L. et al. Effects of acute and chronic administration of methylprednisolone on oxidative stress in rat lungs. J Bras Pneumol 40, 238–43 (2014).
Murata, M., Kumagai, K., Miyata, N., Osaki, M. & Shindo, H. Osteonecrosis in stroke-prone spontaneously hypertensive rats: effect of glucocorticoid. J Orthop Sci 12, 289–95 (2007).
Komurcu, E. et al. Preventive effects of coenzyme Q10 (CoQ10) on steroid-induced osteonecrosis in rats. Acta Orthop Traumatol Turc 48, 217–22 (2014).
Huang, S. L., Jiao, J. & Yan, H. W. Hydrogen-rich saline attenuates steroid-associated femoral head necrosis through inhibition of oxidative stress in a rabbit model. Exp Ther Med 11, 177–182 (2016).
Yang, L. et al. Stem cell factor (SCF) protects osteoblasts from oxidative stress through activating c-Kit-Akt signaling. Biochem Biophys Res Commun 455, 256–61 (2014).
Song, Q. et al. Beneficial effect of grape seed proanthocyanidin extract in rabbits with steroid-induced osteonecrosis via protecting against oxidative stress and apoptosis. J Orthop Sci 20, 196–204 (2015).
Qi, X. & Zeng, Y. Biomarkers and pharmaceutical strategies in steroid-induced osteonecrosis of the femoral head: a literature review. J Int Med Res 43, 3–8 (2015).
Rayman, M. P. The importance of selenium to human health. Lancet 356, 233–41 (2000).
Kahya, M. C., Naziroglu, M. & Cig, B. Melatonin and selenium reduce plasma cytokine and brain oxidative stress levels in diabetic rats. Brain Inj 1–7 (2015).
Ebert, R. et al. Selenium supplementation restores the antioxidative capacity and prevents cell damage in bone marrow stromal cells in vitro . Stem Cells 24, 1226–35 (2006).
Kim, J. H. & Kang, J. C. Oxidative stress, neurotoxicity, and non-specific immune responses in juvenile red sea bream, Pagrus major, exposed to different waterborne selenium concentrations. Chemosphere 135, 46–52 (2015).
Stohs, S. J. & Bagchi, D. Oxidative mechanisms in the toxicity of metal ions. Free Radic Biol Med 18, 321–36 (1995).
Yao, L. et al. Roles of oxidative stress and endoplasmic reticulum stress in selenium deficiency-induced apoptosis in chicken liver. Biometals 28, 255–65 (2015).
McDonald, C. I. et al. The impact of acute lung injury, ECMO and transfusion on oxidative stress and plasma selenium levels in an ovine model. J Trace Elem Med Biol 30, 4–10 (2015).
Alehagen, U. & Aaseth, J. Selenium and coenzyme Q10 interrelationship in cardiovascular diseases–A clinician’s point of view. J Trace Elem Med Biol 31, 157–62 (2015).
Ramamoorthy, V., Rubens, M., Saxena, A. & Shehadeh, N. Selenium and vitamin E for prostate cancer–justifications for the SELECT study. Asian Pac J Cancer Prev 16, 2619–27 (2015).
Sun, H. J. et al. Arsenic and selenium toxicity and their interactive effects in humans. Environ Int 69, 148–58 (2014).
Wang, Y. et al. Inverse relationship between elemental selenium nanoparticle size and inhibition of cancer cell growth in vitro and in vivo . Food Chem Toxicol 85, 71–7 (2015).
Zhang, J., Wang, X. & Xu, T. Elemental selenium at nano size (Nano-Se) as a potential chemopreventive agent with reduced risk of selenium toxicity: comparison with se-methylselenocysteine in mice. Toxicol Sci 101, 22–31 (2008).
Peng, D., Zhang, J., Liu, Q. & Taylor, E. W. Size effect of elemental selenium nanoparticles (Nano-Se) at supranutritional levels on selenium accumulation and glutathione S-transferase activity. J Inorg Biochem 101, 1457–63 (2007).
Liu, X. et al. A novel and facile synthesis of porous SiO2-coated ultrasmall Se particles as a drug delivery nanoplatform for efficient synergistic treatment of cancer cells. Nanoscale 8, 8536–41 (2016).
Wang, H., Zhang, J. & Yu, H. Elemental selenium at nano size possesses lower toxicity without compromising the fundamental effect on selenoenzymes: comparison with selenomethionine in mice. Free Radic Biol Med 42, 1524–33 (2007).
He, Y. et al. Toxicity of selenium nanoparticles in male Sprague-Dawley rats at supranutritional and nonlethal levels. Life Sci 115, 44–51 (2014).
Saita, M. et al. ESR investigation of ROS generated by H2O2 bleaching with TiO2 coated HAp. Dent Mater J 31, 458–64 (2012).
Ding, X., Wang, D., Li, L. & Ma, H. Dehydroepiandrosterone ameliorates H2O2-induced Leydig cells oxidation damage and apoptosis through inhibition of ROS production and activation of PI3K/Akt pathways. Int J Biochem Cell Biol 70, 126–39 (2016).
Singsai, K., Akaravichien, T., Kukongviriyapan, V. & Sattayasai, J. Protective Effects of Streblus asper Leaf Extract on H2O2-Induced ROS in SK-N-SH Cells and MPTP-Induced Parkinson’s Disease-Like Symptoms in C57BL/6 Mouse. Evid Based Complement Alternat Med 2015, 970354 (2015).
Jin, Y. et al. Rhizoma Dioscoreae Nipponicae polysaccharides protect HUVECs from H2O2-induced injury by regulating PPARgamma factor and the NADPH oxidase/ROS-NF-kappaB signal pathway. Toxicol Lett 232, 149–58 (2015).
Wei, P., You, C., Jin, H., Chen, H. & Lin, B. Correlation between serum IL-1beta levels and cerebral edema extent in a hypertensive intracerebral hemorrhage rat model. Neurol Res 36, 170–5 (2014).
Zhang, C., Zou, Y. L., Ma, J., Dang, X. Q. & Wang, K. Z. Apoptosis associated with Wnt/beta-catenin pathway leads to steroid-induced avascular necrosis of femoral head. BMC Musculoskelet Disord 16, 132 (2015).
Jiang, Y. et al. Achyranthes bidentata extract exerts osteoprotective effects on steroid-induced osteonecrosis of the femoral head in rats by regulating RANKL/RANK/OPG signaling. J Transl Med 12, 334 (2014).
Nakamura, H., Yoshino, S., Shiga, H., Tanaka, H. & Katsumata, S. A case of spontaneous femoral neck fracture associated with multicentric reticulohistiocytosis: oversecretion of interleukin-1beta, interleukin-6, and tumor necrosis factor alpha by affected synovial cells. Arthritis Rheum 40, 2266–70 (1997).
Prockop, D. J. Type II collagen and avascular necrosis of the femoral head. N Engl J Med 352, 2268–70 (2005).
Liacini, A. et al. Induction of matrix metalloproteinase-13 gene expression by TNF-alpha is mediated by MAP kinases, AP-1, and NF-kappaB transcription factors in articular chondrocytes. Exp Cell Res 288, 208–17 (2003).
Jingushi, S. et al. Markers of joint tissue turnover in joint fluids from hips with osteonecrosis of the femoral head. J Orthop Res 18, 728–33 (2000).
Choi, S. E., Hong, S. W. & Yoon, S. O. Proposal of an appropriate decalcification method of bone marrow biopsy specimens in the era of expanding genetic molecular study. J Pathol Transl Med 49, 236–42 (2015).
Uzun, G., Mutluoglu, M., Ersen, O. & Yildiz, S. Hyperbaric oxygen therapy in the treatment of osteonecrosis of the femoral head: a review of the current literature. Undersea Hyperb Med 43, 189–99 (2016).
Robinson, E. et al. Combinatorial release of dexamethasone and amiodarone from a nano-structured parylene-C film to reduce perioperative inflammation and atrial fibrillation. Nanoscale 8, 4267–75 (2016).
Kim, K. et al. Externally controlled drug release using a gold nanorod contained composite membrane. Nanoscale 8, 11949–55 (2016).
Albers, A., Carli, A., Routy, B., Harvey, E. J. & Seguin, C. Treatment with acetylsalicylic acid prevents short to mid-term radiographic progression of nontraumatic osteonecrosis of the femoral head: a pilot study. Can J Surg 58, 198–205 (2015).
Li, J. et al. Oxidative stress-mediated selective antimicrobial ability of nano-VO2 against Gram-positive bacteria for environmental and biomedical applications. Nanoscale 8, 11907–23 (2016).
Zhou, W. et al. Ultrastable BSA-capped gold nanoclusters with a polymer-like shielding layer against reactive oxygen species in living cells. Nanoscale 8, 9614–20 (2016).
Garcia-Hevia, L. et al. Nano-ZnO leads to tubulin macrotube assembly and actin bundling, triggering cytoskeletal catastrophe and cell necrosis. Nanoscale 8, 10963–73 (2016).
Gong, G., Meplan, C., Gautrey, H., Hall, J. & Hesketh, J. E. Differential effects of selenium and knock-down of glutathione peroxidases on TNFalpha and flagellin inflammatory responses in gut epithelial cells. Genes Nutr 7, 167–78 (2012).
Wu, Z. L. et al. Inhibitory effect of selenium against Penicillium expansum and its possible mechanisms of action. Curr Microbiol 69, 192–201 (2014).
Hassanin, K. M., Abd El-Kawi, S. H. & Hashem, K. S. The prospective protective effect of selenium nanoparticles against chromium-induced oxidative and cellular damage in rat thyroid. Int J Nanomedicine 8, 1713–20 (2013).
Liu, H., Li, X., Qin, F. & Huang, K. Selenium suppresses oxidative-stress-enhanced vascular smooth muscle cell calcification by inhibiting the activation of the PI3K/AKT and ERK signaling pathways and endoplasmic reticulum stress. J Biol Inorg Chem 19, 375–88 (2014).
Min-Chang, G., Wei-Hong, T., Zhen, X. & Jie, S. Effects of Selenium-Enriched Protein from Ganoderma lucidum on the Levels of IL-1 beta and TNF- alpha, Oxidative Stress, and NF- kappa B Activation in Ovalbumin-Induced Asthmatic Mice. Evid Based Complement Alternat Med 2014, 182817 (2014).
Zhu, X., Jiang, M., Song, E., Jiang, X. & Song, Y. Selenium deficiency sensitizes the skin for UVB-induced oxidative damage and inflammation which involved the activation of p38 MAPK signaling. Food Chem Toxicol 75, 139–45 (2015).
Shakibaie, M. et al. Acute and subacute toxicity of novel biogenic selenium nanoparticles in mice. Pharm Biol 51, 58–63 (2013).
Acknowledgements
This work was financially supported by the Guide project of Shanghai Committee of Science and Technology (Grant no. 15411968800), the Shanghai Municipal Nature Science Foundation (Grant no. 13ZR1433300), the Shanghai First People’s Hospital pre-medical excellent youth project (Grant no. 061417), the National Natural Science Foundation of China (Grant no. 81371979) and the National Natural Science Foundation of China (Grant no. 21476136).
Author information
Authors and Affiliations
Contributions
Guoying Deng: write the manuscript. Kerun Niu: made the statistical analysis and figures. Feng Zhou: experiment main executor. Buxiao Li, Yingjie Kang: experiment executor. Xijian Liu, Junqing Hu, Bo Li: material synthesis and technical guidance. Qiugen Wang, Chengqing Yi, and Qian Wang: design and progress the experiment.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Deng, G., Niu, K., Zhou, F. et al. Treatment of steroid-induced osteonecrosis of the femoral head using porous Se@SiO2 nanocomposites to suppress reactive oxygen species. Sci Rep 7, 43914 (2017). https://doi.org/10.1038/srep43914
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep43914
This article is cited by
-
Glucocorticoid-induced activation of NOX/ROS/NF-κB signaling in MSCs contributes to the development of GONFH
Apoptosis (2023)
-
Hypoxic condition induced H3K27me3 modification of the LncRNA Tmem235 promoter thus supporting apoptosis of BMSCs
Apoptosis (2022)
-
PARK7 promotes repair in early steroid-induced osteonecrosis of the femoral head by enhancing resistance to stress-induced apoptosis in bone marrow mesenchymal stem cells via regulation of the Nrf2 signaling pathway
Cell Death & Disease (2021)
-
Preincubation with a low-dose hydrogen peroxide enhances anti-oxidative stress ability of BMSCs
Journal of Orthopaedic Surgery and Research (2020)
-
P53 and Parkin co-regulate mitophagy in bone marrow mesenchymal stem cells to promote the repair of early steroid-induced osteonecrosis of the femoral head
Cell Death & Disease (2020)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.