Abstract
Childhood trauma (ChT) is a risk factor for psychosis. Negative lifestyle factors such as rumination, negative schemas, and poor diet and exercise are common in psychosis. The present study aimed to perform a network analysis of interactions between ChT and negative lifestyle in patients and controls. We used data of patients with early-stage psychosis (n = 500) and healthy controls (n = 202). Networks were constructed using 12 nodes from five scales: the Brief Core Schema Scale (BCSS), Brooding Scale (BS), Dietary Habits Questionnaire, Physical Activity Rating, and Early Trauma Inventory Self Report-Short Form (ETI). Graph metrics were calculated. The nodes with the highest predictability and expected influence in both patients and controls were cognitive and emotional components of the BS and emotional abuse of the ETI. The emotional abuse was a mediator in the shortest pathway connecting the ETI and negative lifestyle for both groups. The negative others and negative self of the BCSS mediated emotional abuse to other BCSS or BS for patients and controls, respectively. Our findings suggest that rumination and emotional abuse were central symptoms in both groups and that negative others and negative self played important mediating roles for patients and controls, respectively.
Trial Registration: ClinicalTrials.gov identifier: CUH201411002.
Similar content being viewed by others
Introduction
Network analysis has been employed to investigate a) psychotic experiences1, potential pathways between psychotic symptoms and environmental risk factors or childhood trauma (ChT)2, and transdiagnostic experiences surrounding auditory verbal hallucinations3 in b) general population samples as well as interactions among a wide array of psychotic symptoms4 or among positive, negative, and depressive symptoms5, prediction of treatment responses6, negative symptom systems7, and pathways linking psychotic symptoms with ChT8 or post-traumatic stress9 in psychosis or schizophrenia. To date, only one study on the issue of trauma in psychosis8 has used a network approach; that study was based on data from patients but not from healthy controls.
Rumination is a repetitive and negatively valenced thinking style characterized by “the tendency to repetitively analyze one’s problems, concerns, and feelings of distress without taking action to make positive changes”10. Several studies have explored the relationships of rumination with depression11, negative symptoms12, positive symptoms13, and suicidality14 in psychosis. People with psychosis reported extreme negative evaluations of both self and others15. Furthermore, individuals with psychosis showing suicidal ideation held more negative evaluations of self and others than did those without suicidal ideation16. Moreover, in individuals with psychosis, negative beliefs following trauma were closely associated with psychotic experiences17. Patients with schizophrenia tend to have poor diets, characterized by high intake of saturated fat and low consumption of fiber and fruit18, and to have lower levels of physical activity compared with the general population19. One study reported that physical abuse was linked to elevated systolic blood pressure, whereas emotional abuse and neglect in women were linked to overweight in patients with schizophrenia20. Also in a non-clinical population, individuals with adverse childhood experiences were at increased risk of poor health outcomes such as physical inactivity, overweight or obesity, and diabetes21. Taken together, these findings suggest that in individuas with psychosis, ChT is associated with rumination, negative schemas, poor diet, and reduced physical activity, which can be grouped as a “negative life style”.
Our first aim was to understand how from a network perspective, ChT and negative life style interact in a given network and what are the central and bridge symptoms. The second aim was to determine whether the network characteristics of the two domains would remain the same or be altered after including positive (P) and negative symptoms (N) of psychosis as a third domain in the network. Therefore, in the present study, networks consisting of two or three domains were estimated and analyzed in patients with early-stage psychosis. The characteristics of these networks were compared to those of healthy controls.
Method
Study sample
Data were collected as part of the longitudinal multicenter Korean Early Psychosis Study (KEPS), which has been described in detail elsewhere22. The sample comprised 500 patients with early-stage psychosis and 202 healthy controls. The inclusion criteria required that subjects be between 19 and 58 years of age and meet the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV)23 criteria for schizophrenia spectrum disorders (schizophrenia, schizoaffective disorder, schizophreniform disorder, psychotic disorder not otherwise specified [NOS]), brief psychotic disorder, or delusional disorder. Individuals who had been treated with antipsychotics for < 2 years were considered to be in early-stage psychosis. Written informed consents were obtained from all the participants and also from legal guardians of the participants. All experimental protocols were approved by the Ethics Committee of the Jeonbuk National University Hospital (approval number CUH 2014-11-002). All procedures were performed in accordance with relevant guidelines.
Measures
The severity of psychiatric symptoms was assessed using the Positive and Negative Syndrome Scale (PANSS)24. For self-rating scales, the Brief Core Schema Scale (BCSS)15, Brooding Scale (BS)25, Early Trauma Inventory Self Report-Short Form (ETI)26, Dietary Habits Questionnaire (DHQ)27 and Physical Activity Rating (PAR)28 were employed. The DHQ is a 20-item self-administered questionnaire consisting of three subcategories: five items for diet regularity, six items for balanced diet, and nine items for unhealthy diet and eating habits. This scale was developed based on dietary guidance published by the Korean Ministry for Health, Welfare and Family Affairs (2010)29. The total score is categorized as indicating poor (20–49), usual (50–79), or good (80–100) diet. The PAR is a questionnaire that rates the individual’s level of physical activity, with scores ranging from 0 (avoids walking or exercise) to 7 (runs more than 10 miles per week or spends more than 3 h per week in comparable physical activity). As all scores for each parameter exhibited skewed distributions based on the Shapiro–Wilk test, they were normalized using nonparanormal transformation30,31.
Network estimation
Networks were constructed using 12 nodes: negative self, positive self, negative others, and positive others from the BCSS; emotional and cognitive components from the BS; DHQ; PAR; and general trauma, emotional abuse, physical abuse, and sexual abuse from the ETI). We fitted a Gaussian graphical model (GGM) to the data. The GGM networks were regularized via a graphical lasso (GLASSO) algorithm32 in combination with the extended Bayesian information criterion (EBIC) model. A tuning hyperparameter γ for the EBIC was set to 0.533. The edges were calculated by partial correlations. We used the R-packages ‘bootnet (estimateNetwork (https://CRAN.R-project.org/package=bootnet. R package version 1.4.3))’ and ‘qgraph’ (https://rdocumentation.org/packages/qgraph/versions/1.6.9. R package version 1.6.9) to estimate and visualize all networks34.
Network analysis
Global network metrics
Global network metrics consisting of network density, global strength, averaged clustering coefficient, modularity index (Q), and characteristic path length were calculated using the R packages ‘qgraph’ and ‘igraph’ (https://cran.r-project.org/package=igraph. R package version 1.2.7).
Local network metrics
Although strength is regarded as the most reliably estimated centrality index it does not necessarily indicate the degree to which a node can be predicted by the remaining intranetwork nodes. To examine node predictability, we estimated the proportion of each node’s variance accounted for by its connections to other nodes in the network, using the ‘mgm’ package (https://cran.r-project.org/package=mgm. R package version 1.2-12). In addition, as strength centrality uses the sum of absolute weights, whether positive or negative, which might distort interpretation, we estimated expected influence (EI), i.e., the sum of all edges of a node35. To detect symptoms that bridged the two domains (ChT and negative life style) or three domains (ChT, negative life style and P and N on the PANSS), bridge EI was calculated. Bridge EI is the sum of the values (+ or −) of all edges that connect a node to all nodes that are not part of the same community36. Bridge symptoms that play a primary role in connecting two or more psychiatric symptoms or domains37 were defined as those items scoring higher than the 80th percentile for the bridge EI metric. We also computed the shortest pathways38 from each subscale of the ETI to negative life style or to P and N within the network. To determine the EI, bridge EI, and shortest pathway, the R-packages ‘mgm’, ‘qgraph’, ‘networktools’39, and ‘igraph’ were used, respectively.
Network comparison
We investigated network structures and global strength using the Network Comparison Test (NCT) in the R package. For global network metrics (network density, averaged clustering coefficient, modularity index [Q], and characteristic path length), the ‘NetworkToolbox’ package (https://cran.r-project.org/package=NetworkToolbox. R package version 1.4.2) was used to explore whether the overall level of network connectivity was equal among the networks.
Network accuracy and stability
The accuracy and stability of the network were examined using the R package ‘bootnet(https://CRAN.R-project.org/package=bootnet. R package version 1.4.3)’. First, we bootstrapped (1,000 iterations) the 95% confidence intervals around the edge weights to assess the accuracy of the edge weights. Second, we used the case-dropping subset bootstrap (1,000 iterations) to examine the stability of the order of the node centrality indices. A correlation stability coefficient (CS-coefficient), a measure that quantifies the stability of node centrality indices, was also calculated. Finally, we tested for significant differences in edge weights and node centralities using the bootstrapped difference tests. In addition, using the R-package “netPower (https://github.com/mihaiconstantin/netpaw. R package version 1.0.0)”, we calculated power with current conditions which was 80%, an acceptable level.
Results
Participants’ demographic and clinical characteristics
The proportion of males was lower (p = 0.027) and the mean age was younger (p < 0.001) in patients compared to controls. The scores on the negative self and negative others of the BCSS, the emotional and cognitive components on the BS, the general trauma, emotional abuse, physical abuse, and sexual abuse on the ETI, and the DHQ were significantly higher in patients compared to controls. Notably, although the DHQ score was significantly higher in patients, scores ranging from 50 to 79 are categorized as usual; hence, there was no actual difference between the two groups. The PAR score was significantly lower in patients (Table S1).
Global network metrics
Comparisons between the two groups revealed no significant differences in all global network metrics except the average clustering coefficient (Table S2).
Local network metrics
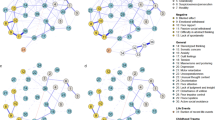
The nodes showing the highest predictability in both groups were cognitive and emotional components of the BS (Figs. 1 and S1 and Table S3). The node with highest EI in both groups was emotional abuse of the ETI (Figs. 2 and S2). In patients, the shortest pathway from each subscale node of the ETI to the BS nodes always connected through the emotional abuse node (Fig. 3a). However, in controls, it always connected via the negative self and/or emotional abuse nodes. In patients, the connection order for the BS nodes was emotional and cognitive components, whereas it was the reverse in controls. With respect to the shortest pathway from each subscale node of the ETI to the BCSS nodes, emotional abuse played the same mediating role in both groups (except for sexual abuse in the controls, which connected directly to negative self). However, the connection order for the BCSS nodes was negative others and negative self in patients and the reverse in controls (Fig. 3b). When P and N of the PANSS were included in the network, the shortest pathway from each subscale node of the ETI to the P or N node always connected through the negative others node (Fig. 4). The bridge symptoms between the two domains were emotional abuse, negative others and emotional component in patients and emotional abuse, negative self and sexual abuse in controls (Fig. 5). The bridge symptoms among the three domains in patients were the same as in the two-domain model (Fig. S3).
Estimated network structures of (a) patients and (b) controls. Graph features represent the following: edge thickness = strengths of the regularized partial correlations (positive in blue and negative in red); shaded area in the node perimeter = predictability. Abbreviation: BCSS, Brief Core Schema Scales; BS, Brooding Scale; Co, Cognitive subscale of the BS; DHQ, Dietary Habits Questionnaire; Em, Emotional subscale of the BS; EMO, Emotional abuse of the ETI; ETI, Early Trauma Inventory Self Report-Short Form; GT, General Traumatic experiences of the ETI; NO, Negative-Others of the BCSS; NS, Negative-Self of the BCSS; PAR, Physical Activity Rating; PHY, Physical abuse of the ETI; PO, Positive-Others of the BCSS; PS, Positive-Self of the BCSS; SEXU, Sexual abuse of the ETI. The R-packages ‘mgm (version 1.2-12 and URL https://CRAN.R-project.org/package=mgm)’ ‘qgraph (version 1.6.9 and URL https://CRAN.R-project.org/package=qgraph)’ and ‘igraph (version 1.2.7 and URL https://CRAN.R-project.org/package=igraph)’ were used to estimate and visualize all networks.
Expected influence for patients (red) and controls (blue). Abbreviation: Co, Cognitive subscale of the BS; DHQ, Dietary Habits Questionnaire; Em, Emotional subscale of the BS; EMO, Emotional abuse of the ETI; GT, General Traumatic experiences of the ETI; NO, Negative-Others of the BCSS; NS, Negative-Self of the BCSS; PAR, Physical Activity Rating; PHY, Physical abuse of the ETI; PO, Positive-Others of the BCSS; PS, Positive-Self of the BCSS; SEXU, Sexual abuse of the ETI The R-packages ‘mgm (version 1.2-12 and URL https://CRAN.R-project.org/package=mgm)’ and ‘qgraph (version 1.6.9 and URL https://CRAN.R-project.org/package=qgraph)’ were used.
Shortest pathways from GT, EMO, PHY or SEXU to negative life style in (a) patients (a-1, a-2, a-3 and a-4) and (b) controls (b-1, b-2, b-3 and b-4). Thicker solid lines represent stronger connections; Dashed lines represent background connections existent within the network that are less relevant when investigating shortest paths. Abbreviation: same as in the Fig. 1. The R-packages ‘networktools (version 1.4.0 and URL https://CRAN.R-project.org/package=networktools)’ and ‘igraph (version 1.2.7 and URL https://CRAN.R-project.org/package=igraph)’ were used.
Shortest pathways from GT, EMO, PHY or SEXU to P (a-1, a-2, a-3 and a-4) or N (b-1, b-2, b-3 and b-4) in patients. Thicker solid lines represent stronger connections; Dashed lines represent background connections existent within the network that are less relevant when investigating shortest paths. Abbreviation: same as in the Fig. 1. The R-packages ‘networktools (version 1.4.0 and URL https://CRAN.R-project.org/package=networktools)’ and ‘igraph (version 1.2.7 and URL https://CRAN.R-project.org/package=igraph)’ were used.
Bridge symptoms between two domains (childhood trauma and negative life style) in (a) patients and (b) controls. Abbreviation: same as in the Fig. 1. The R-packages ‘mgm (version 1.2–12 and URL https://CRAN.R-project.org/package=mgm)’ and ‘qgraph (version 1.6.9 and URL https://CRAN.R-project.org/package=qgraph)’ were used.
Network accuracy and stability
The results of the edge weight bootstrap analysis (Fig. S4) showed substantial overlap among the 95% CIs of the edge weights. However, some of the strongest edges showed non-overlapping CI values. The CS coefficients for node strength and bridge EI were \(\ge\) 0.25 in both groups (Table S4 and S5). The results of bootstrapped difference tests for EI, bridge EI, edge weights and strength centralities are presented in Figs. S1–S9.
Discussion
This childhood adversity can affect many aspects of personal development. Assuming that ChT may lead to negative life style factors such as rumination, negative schemas, poor diet, and reduced physical exercise, we conducted network analysis to explore dynamic interactions between ChT and negative life style in individuals with early-stage psychosis. Our results revealed several central symptoms within a network, which could ultimately prove to be important targets for clinical intervention.
In terms of global network metrics, only the average clustering coefficient differed significantly between the patient and control groups. As a higher clustering coefficient value means a more connected neighborhood around one particular node, this suggests that the 12 symptoms studied in patients were much more highly connected in a triangular fashion, producing greater negative impact on one another. Given that clustering coefficients tend to decline with the age40, our finding may be due to the age difference between the groups. However, no test controlling for covariates is available at present.
With respect to local network metrics, in both groups, the node with the highest predictability was rumination, which indicates that variance in rumination was highly predicted by its relationships with other symptoms in the network. Numerous factors may trigger rumination including negative affect, childhood adversity41, stable individual traits, and failure to achieve a goal42. Rumination has also been regarded as a common pathway leading to the development of mental disorders43. emotional abuse was the most influential central symptom in both groups, although its EI value was slightly higher in patients compared to controls. Emotional abuse and emotional neglect have been considered the most frequent forms of severe trauma in patients with schizophrenia44. Few studies have addressed the specificity of childhood adversity effects; emotional and physical abuses were correlated with dissociative symptoms in patients with schizophrenia44; emotional neglect was associated with psychotic experiences in a general population cohort45; and physical and sexual abuses were associated with positive symptoms in first-episode psychosis46. Therefore, these findings suggest that, from the perspective of “factors that are influenced and influential”, rumination and emotional abuse are key central factors that should be targeted for psychosocial intervention in patients with psychosis.
With regard to the shortest pathway between ChT and negative life style, the results suggest that emotional abuse played the same mediating role between the two in both groups. However, a key difference was that in controls, this pathway always led through negative self following emotional abuse and then connected to rumination or negative others. More importantly, in the network including P and N, the pathway for patients was always through negative others following emotional abuse and was then connected to P or N. Thus, these findings suggest that, although emotional abuse was an important meditator in both groups, negative others and negative self were more crucial as differentiating meditators for patients and controls, respectively. Several studies have demonstrated a mediating role of negative beliefs about others between trauma and psychotic symptoms17 and a close association of negative views of others with paranoia47. It is noteworthy that the ‘negative self’ schema is also closely associated with persecutory delusions48 and auditory verbal hallucinations49. In a community sample, previous evidence indicated that early trauma led to reduced self-esteem50 or negative self-referential processing51. Taken together, our findings suggest that patients with early-stage psychosis may benefit from psychotherapeutic treatment targeting negative others. One systematic review of schema therapy indicated initial significant results in terms of reducing early maladaptive schemas and improving symptoms related to personality disorders, but evidence for other mental disorders is currently sparse52. The question of why negative others or negative self was a more important meditator in patients than in controls needs to be clarified in future studies. The relative importance of negative others vs. negative self in patients vs. controls was supported by the findings about bridge symptoms. Interestingly, when P and N were included in the network, three bridge symptoms (emotional abuse, negative others, and emotional component of the BS) remained the same. As bridge symptoms connect different domains within a network, the activation of these bridge symptoms might be expected to distribute the activation toward other domains. This emphasizes the importance of intervening in negative others to reduce P and N in patients with psychosis. Importantly, the CS coefficients for node strength and bridge EI were above the recommended 0.25 cutoff in both groups, making their interpretation acceptable.
A few limitations associated with the current study need to be acknowledged. First, we used cross-sectional data to examine the association between ChT and negative life style, which did not allow us to identify potentially causal relations. Second, sex covariate was not controlled for. Given high impact of sexual abuse in female, our results should be limitedly interpreted. Third, as ChT was assessed with self-rating scale, its validity is weak. Lastly, to validate our findings, replication study should be pursued in future. Despite these caveats, the strength of our study lay in the use of a network approach to examine interrelationships between ChT and negative life style in patients and controls. In summary, we found that rumination and emotional abuse were central symptoms in both groups, and negative others and negative self played important mediating roles for patients and controls, respectively. These findings highlight the importance of targeting central or mediating symptoms to improve patients’ recovery. Future research focusing specifically on these symptoms could be invaluable when designing interventions for patients exposed to ChT.
Data availability
The data supporting the findings are fully available without restriction. Relevant data are available from the corresponding author upon request.
References
Murphy, J., McBride, O., Fried, E. & Shevlin, M. Distress, impairment and the extended psychosis phenotype: A network analysis of psychotic experiences in an US general population sample. Schizophr. Bull. 44(4), 768–777 (2018).
Isvoranu, A. M., Borsboom, D., van Os, J. & Guloksuz, S. A network approach to environmental impact in psychotic disorder: Brief theoretical framework. Schizophr. Bull. 42(4), 870–873 (2016).
Wigman, J. T., de Vos, S., Wichers, M., van Os, J. & Bartels-Velthuis, A. A. A transdiagnostic network approach to psychosis. Schizophr. Bull. 43(1), 122–132 (2017).
van Rooijen, R., Ploeger, A. & Kret, M. E. The dot-probe task to measure emotional attention: A suitable measure in comparative studies?. Psychon. Bull. Rev. 24(6), 1686–1717 (2017).
van Rooijen, G. et al. A state-independent network of depressive, negative and positive symptoms in male patients with schizophrenia spectrum disorders. Schizophr. Res. 193, 232–239 (2018).
Esfahlani, F. Z., Sayama, H., Visser, K. F. & Strauss, G. P. Sensitivity of the positive and negative syndrome scale (PANSS) in detecting treatment effects via network analysis. Innov. Clin. Neurosci. 14(11–12), 59 (2017).
Levine, S. Z. & Leucht, S. Identifying a system of predominant negative symptoms: Network analysis of three randomized clinical trials. Schizophr. Res. 178(1–3), 17–22 (2016).
Isvoranu, A. M. et al. A network approach to psychosis: Pathways between childhood trauma and psychotic symptoms. Schizophr. Bull. 43(1), 187–196 (2016).
Hardy, A., O’Driscoll, C., Steel, C., Van Der Gaag, M. & Van Den Berg, D. A network analysis of post-traumatic stress and psychosis symptoms. Psychol. Med. 51, 1–8 (2020).
Nolen-Hoeksema, S. & Morrow, J. A prospective study of depression and posttraumatic stress symptoms after a natural disaster: The 1989 Loma Prieta Earthquake. J. Pers. Soc. Psychol. 61(1), 115 (1991).
Thomas, N., Ribaux, D. & Phillips, L. J. Rumination, depressive symptoms and awareness of illness in schizophrenia. Behav. Cogn. Psychother. 42(2), 143 (2014).
Halari, R. et al. Rumination and negative symptoms in schizophrenia. J. Nerv. Ment. Dis. 197(9), 703–706 (2009).
Badcock, J. C., Paulik, G. & Maybery, M. T. The role of emotion regulation in auditory hallucinations. Psychiatry Res. 185(3), 303–308 (2011).
Ahrens, B. & Linden, M. Is there a suicidality syndrome independent of specific major psychiatric disorder? Results of a split half multiple regression analysis. Acta Psychiatr. Scand. 94(2), 79–86 (1996).
Fowler, D. et al. The Brief Core Schema Scales (BCSS): Psychometric properties and associations with paranoia and grandiosity in non-clinical and psychosis samples. Psychol. Med. 36(6), 749–759 (2006).
Fialko, L. et al. Understanding suicidal ideation in psychosis: Findings from the Psychological Prevention of Relapse in Psychosis (PRP) trial. Acta Psychiatr. Scand. 114(3), 177–186 (2006).
Kilcommons, A. M. & Morrison, A. P. Relationships between trauma and psychosis: An exploration of cognitive and dissociative factors. Acta Psychiatr. Scand. 112(5), 351–359 (2005).
Dipasquale, S. et al. The dietary pattern of patients with schizophrenia: A systematic review. J. Psychiatr. Res. 47(2), 197–207 (2013).
Daumit, G. L. et al. Physical activity patterns in adults with severe mental illness. J. Nerv. Ment. Dis. 193(10), 641–646 (2005).
Rajkumar, R. P. The impact of childhood adversity on the clinical features of schizophrenia. Schizophr. Res. Treat. (2015).
Hughes, K. et al. The effect of multiple adverse childhood experiences on health: A systematic review and meta-analysis. The Lancet Public Health 2(8), e356–e366 (2017).
Kim, S. W. et al. Design and methodology of the Korean early psychosis cohort study. Psychiatry Investig. 14(1), 93 (2017).
DSM, IV. Diagnostic and Statistical Manual of Mental Disorders. (American Psychiatric Association, 1994).
Kay, S. R., Fiszbein, A. & Opler, L. A. The positive and negative syndrome scale (PANSS) for schizophrenia. Schizophr. Bull. 13(2), 261 (1987).
Kim, J. H. et al. The development of the brooding scale. Psychiatry Investig. 16(6), 443 (2019).
Bremner, J. D., Bolus, R. & Mayer, E. A. Psychometric properties of the early trauma inventory—Self report. J. Nerv. Ment. Dis. 195(3), 211 (2007).
Jhon, M. et al. Gender-specific risk factors for low bone mineral density in patients taking antipsychotics for psychosis. Hum. Psychopharmacol. Clin. Exp. 33(1), e2648 (2018).
Jackson, A. S. et al. Prediction of functional aerobic capacity without exercise testing. Med. Sci. Sports Exerc. 22(6), 863–870 (1990).
Ministry for Health, Welfare and Family Affairs. Dietary Reference Intakes For Koreans. Sejong, Korea: Ministry for Health, Welfare and Family Affairs. (2010).
Epskamp, S., Borsboom, D. & Fried, E. I. Estimating psychological networks and their accuracy: A tutorial paper. Behav. Res. Methods 50(1), 195–212 (2018).
Liu, H., Lafferty, J. & Wasserman, L. The nonparanormal: Semiparametric estimation of high dimensional undirected graphs. J. Mach Learn. Res. 10(10), 2295–2328 (2009).
Friedman, J., Hastie, T. & Tibshirani, R. Sparse inverse covariance estimation with the graphical lasso. Biostatistics 9(3), 432–441 (2008).
Boccaletti, S., Latora, V., Moreno, Y., Chavez, M. & Hwang, D. U. Complex networks: Structure and dynamics. Phys. Rep. 424(4–5), 175–308 (2006).
Glück, T. M., Knefel, M. & Lueger-Schuster, B. A network analysis of anger, shame, proposed ICD-11 post-traumatic stress disorder, and different types of childhood trauma in foster care settings in a sample of adult survivors. Eur. J. Psychotraumatol. 8(sup3), 1372543 (2017).
Robinaugh, D. J., Millner, A. J. & McNally, R. J. Identifying highly influential nodes in the complicated grief network. J. Abnorm. Psychol. 125(6), 747 (2016).
Levinson, C. A. et al. Social anxiety and eating disorder comorbidity and underlying vulnerabilities: Using network analysis to conceptualize comorbidity. Int. J. Eat. Disord. 51(7), 693–709 (2018).
Jones, P. J., Ma, R. & McNally, R. J. Bridge centrality: A network approach to understanding comorbidity. Multivar Behav. Res. 1–15 (2019).
Dijkstra, E. W. A note on two problems in connexion with graphs. Numer. Math. 1(1), 269–271 (1959).
Jones, P. J. Networktools: Assorted Tools for Identifying Important Nodes in Networks. R package version 1.1. 0. Computer Software. Retrieved from https://CRAN.Rproject.org/package=networktools (2017).
Masuda, N., Sakaki, M., Ezaki, T. & Watanabe, T. Clustering coefficients for correlation networks. Front. Neuroinform. 12, 7 (2018).
Cui, Y. et al. Psychological factors intervening between childhood trauma and suicidality in first-episode psychosis. Psychiatry Res. 293, 113465 (2020).
Smith, J. M. & Alloy, L. B. A roadmap to rumination: A review of the definition, assessment, and conceptualization of this multifaceted construct. Clin. Psychol. Rev. 29(2), 116–128 (2009).
Kinderman, P. A psychological model of mental disorder. Harv. Rev. Psychiatry 13(4), 206–217 (2005).
Schäfer, I. et al. Dissociative symptoms in patients with schizophrenia: Relationships with childhood trauma and psychotic symptoms. Compr. Psychiatry 53(4), 364–371 (2012).
Croft, J. et al. Association of trauma type, age of exposure, and frequency in childhood and adolescence with psychotic experiences in early adulthood. JAMA Psychiat. 76(1), 79–86 (2019).
Ajnakina, O. et al. Impact of childhood adversities on specific symptom dimensions in first-episode psychosis. Psychol Med 46(2), 317–326 (2016).
Valiente, C., Cantero, D., Sánchez, Á., Provencio, M. & Wickham, S. Self-esteem and evaluative beliefs in paranoia. J. Behav. Ther. Exp. Psychiatry 45(2), 297–302 (2014).
Smith, B. et al. Emotion and psychosis: links between depression, self-esteem, negative schematic beliefs and delusions and hallucinations. Schizophr. Res. 86(1–3), 181–188 (2006).
Scott, M., Rossell, S. L., Meyer, D., Toh, W. L. & Thomas, N. Childhood trauma, attachment and negative schemas in relation to negative auditory verbal hallucination (AVH) content. Psychiatry Res. 290, 112997 (2020).
Turner, H. A., Finkelhor, D. & Ormrod, R. The effects of adolescent victimization on self-concept and depressive symptoms. Child Maltreat. 15(1), 76–90 (2010).
Jopling, E., Tracy, A. & LeMoult, J. Childhood maltreatment, negative self-referential processing, and depressive symptoms during stress. Psychol. Res. Behav. Manag. 13, 79 (2020).
Taylor, C. D., Bee, P. & Haddock, G. Does schema therapy change schemas and symptoms? A systematic review across mental health disorders. Psychol. Psychother. Theory Res. Pract. 90(3), 456–479 (2017).
Acknowledgements
The corresponding author would like to thank all participants in the study, as well as his father for guidance. The authors report no biomedical financial interests or potential conflicts of interest.
Funding
Korean Mental Health Technology R&D Project, Ministry of Health and Welfare, Republic of Korea (HL19C0015); Korea Health Technology R&D Project through the Korea Health Industry Development Institute (KHIDI) funded by the Ministry of Health and Welfare, Republic of Korea (HI18C2383).
Author information
Authors and Affiliations
Contributions
Y.C.C. contributed to the conceptualization, funding, supervision, writing review & editing; Y.H.P., L.L., L.B., K.W., J.S. and T.B.N. did data analysis and writing a draft. K.S., L.B., K.J., Y.J., L.K., W.S., L.S., K.S., K.S., K.E. contributed to the data acquisition. Y.J., F.Z.R. did write review & editing.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Chung, YC., Yun, JY., Nguyen, T.B. et al. Network analysis of trauma in patients with early-stage psychosis. Sci Rep 11, 22749 (2021). https://doi.org/10.1038/s41598-021-01574-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-021-01574-y
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.