Abstract
Efflux pumps are a serious challenge for the development of antibacterial agents. Overcoming efflux requires an in-depth understanding of efflux pump functions, specificities and the development of inhibitors. However, the complexities of efflux networks have limited such studies. To address these challenges, we generated Efflux KnockOut-35 (EKO-35), a highly susceptible Escherichia coli strain lacking 35 efflux pumps. We demonstrate the use of this strain by constructing an efflux platform comprising EKO-35 strains individually producing efflux pumps forming tripartite complexes with TolC. This platform was profiled against a curated diverse compound collection, which enabled us to define physicochemical properties that contribute to transport. We also show the E. coli drug efflux network is conditionally essential for growth, and that the platform can be used to investigate efflux pump inhibitor specificities and efflux pump interplay. We believe EKO-35 and the efflux platform will have widespread application for the study of drug efflux.

This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
Data availability
All supporting data are included in this published article and the Supplementary information. Source data are provided with this paper. EKO-35 and EKO-35-Pore genomic raw sequence data were deposited in GenBank (BioProject ID PRJNA838981). The reference E. coli genome was obtained from NCBI (accession no. CP009273.1). Mass spectrometry proteomics data have been deposited to the ProteomeXchange Consortium via the PRIDE partner repository with the dataset identifier PXD033975. Source data are provided with this paper.
References
Tommasi, R., Brown, D. G., Walkup, G. K., Manchester, J. I. & Miller, A. A. ESKAPEing the labyrinth of antibacterial discovery. Nat. Rev. Drug Discov. 14, 529–542 (2015).
Zhao, S. et al. Defining new chemical space for drug penetration into Gram-negative bacteria. Nat. Chem. Biol. 16, 1293–1302 (2020).
Krishnamoorthy, G. et al. Synergy between active efflux and outer membrane diffusion defines rules of antibiotic permeation into Gram-negative bacteria. mBio 8, e01172–17 (2017).
Piddock, L. J. V. Multidrug-resistance efflux pumps - not just for resistance. Nat. Rev. Microbiol. 4, 629–636 (2006).
Teelucksingh, T., Thompson, L. K. & Cox, G. The evolutionary conservation of Escherichia coli drug efflux pumps supports physiological functions. J. Bacteriol. 202, e00367–20 (2020).
Saier, M. H. Jr. et al. Evolutionary origins of multidrug and drug-specific efflux pumps in bacteria. FASEB J. 12, 265–274 (1998).
Nishino, K. & Yamaguchi, A. Analysis of a complete library of putative drug transporter genes in Escherichia coli. J. Bacteriol. 183, 5803–5812 (2001).
Saier, M. H. Jr. A functional-phylogenetic classification system for transmembrane solute transporters. Microbiol. Mol. Biol. Rev. 64, 354–411 (2000).
Sun, J., Deng, Z. & Yan, A. Bacterial multidrug efflux pumps: mechanisms, physiology and pharmacological exploitations. Biochem. Biophys. Res. Commun. 453, 254–267 (2014).
Alcalde-Rico, M., Hernando-Amado, S., Blanco, P. & Martínez, J. L. Multidrug efflux pumps at the crossroad between antibiotic resistance and bacterial virulence. Front. Microbiol. 7, 1483 (2016).
Weston, N., Sharma, P., Ricci, V. & Piddock, L. J. V. Regulation of the AcrAB-TolC efflux pump in Enterobacteriaceae. Res. Microbiol. 169, 425–431 (2018).
Krishnamoorthy, G. et al. Breaking the permeability barrier of Escherichia coli by controlled hyperporination of the outer membrane. Antimicrob. Agents Chemother. 60, 7372–7381 (2016).
Datsenko, K. A. & Wanner, B. L. One-step inactivation of chromosomal genes in Escherichia coli K-12 using PCR products. Proc. Natl Acad. Sci. USA 97, 6640–6645 (2000).
Jiang, Y. et al. Multigene editing in the Escherichia coli genome via the CRISPR-Cas9 system. Appl. Environ. Microbiol. 81, 2506–2514 (2015).
Baba, T. et al. Construction of Escherichia coli K-12 in-frame, single-gene knockout mutants: the Keio collection. Mol. Syst. Biol. https://doi.org/10.1038/msb4100050 (2006).
Krin, E., Danchin, A. & Soutourina, O. Decrypting the H-NS-dependent regulatory cascade of acid stress resistance in Escherichia coli. BMC Microbiol. 10, 273 (2010).
Hyatt, D. et al. Prodigal: prokaryotic gene recognition and translation initiation site identification. BMC Bioinf. 11, 119 (2010).
Jumper, J. et al. Highly accurate protein structure prediction with AlphaFold. Nature 596, 583–589 (2021).
Rest, M. E., van der, van der Rest, M. E., Frank, C. & Molenaar, D. Functions of the membrane-associated and cytoplasmic malate dehydrogenases in the citric acid cycle of Escherichia coli. J. Bacteriol. 182, 6892–6899 (2000).
Wang-Kan, X. et al. Lack of AcrB efflux function confers loss of virulence on Salmonella enterica serovar Typhimurium. mBio. https://doi.org/10.1128/mBio.00968-17 (2017).
Cox, G. et al. A common platform for antibiotic dereplication and adjuvant discovery. Cell Chem. Biol. 24, 98–109 (2017).
Zgurskaya, H. I., Krishnamoorthy, G., Ntreh, A. & Lu, S. Mechanism and function of the outer membrane channel TolC in multidrug resistance and physiology of Enterobacteria. Front. Microbiol. 2, 189 (2011).
Kitagawa, M. et al. Complete set of ORF clones of Escherichia coli ASKA library (a complete set of E. coli K-12 ORF archive): unique resources for biological research. DNA Res. 12, 291–299 (2005).
Grinter, R. et al. Protease-associated import systems are widespread in Gram-negative bacteria. PLoS Genet. 15, e1008435 (2019).
Horiyama, T. & Nishino, K. AcrB, AcrD, and MdtABC multidrug efflux systems are involved in enterobactin export in Escherichia coli. PLoS ONE 9, e108642 (2014).
Hews, C. L., Cho, T., Rowley, G. & Raivio, T. L. Maintaining integrity under stress: envelope stress response regulation of pathogenesis in Gram-negative bacteria. Front. Cell. Infect. Microbiol. 9, 313 (2019).
Blanco, P. et al. Bacterial multidrug efflux pumps: much more than antibiotic resistance determinants. Microorganisms 4, 14 (2016).
Deininger, K. N. W. et al. A requirement of TolC and MDR efflux pumps for acid adaptation and GadAB induction in Escherichia coli. PLoS ONE 6, e18960 (2011).
Lewinson, O., Padan, E. & Bibi, E. Alkalitolerance: a biological function for a multidrug transporter in pH homeostasis. Proc. Natl Acad. Sci. USA 101, 14073–14078 (2004).
Holdsworth, S. R. & Law, C. J. Multidrug resistance protein MdtM adds to the repertoire of antiporters involved in alkaline pH homeostasis in Escherichia coli. BMC Microbiol. 13, 113 (2013).
Zhang, Y. et al. The multidrug efflux pump MdtEF protects against nitrosative damage during the anaerobic respiration in Escherichia coli. J. Biol. Chem. 286, 26576–26584 (2011).
El Zahed, S. S., French, S., Farha, M. A., Kumar, G. & Brown, E. D. Physicochemical and structural parameters contributing to the antibacterial activity and efflux susceptibility of small molecule inhibitors of Escherichia coli. Antimicrob. Agents Chemother. 65, e01925–20 (2021).
Smith, D. H. & Davis, B. D. Mode of action of novobiocin in Escherichia coli. J. Bacteriol. 93, 71–79 (1967).
Braun, M., Killmann, H., Maier, E., Benz, R. & Braun, V. Diffusion through channel derivatives of the Escherichia coli FhuA transport protein. Eur. J. Biochem. 269, 4948–4959 (2002).
Srikumar, R., Kon, T., Gotoh, N. & Poole, K. Expression of Pseudomonas aeruginosa multidrug efflux pumps MexA-MexB-OprM and MexC-MexD-OprJ in a multidrug-sensitive Escherichia coli strain. Antimicrob. Agents Chemother. 42, 65–71 (1998).
Ramaswamy, V. K., Vargiu, A. V., Malloci, G., Dreier, J. & Ruggerone, P. Molecular rationale behind the differential substrate specificity of bacterial RND multi-drug transporters. Sci. Rep. 7, 8075 (2017).
Rosenberg, E. Y., Ma, D. & Nikaido, H. AcrD of Escherichia coli is an aminoglycoside efflux pump. J. Bacteriol. 182, 1754–1756 (2000).
Sulavik, M. C. et al. Antibiotic susceptibility profiles of Escherichia coli strains lacking multidrug dfflux pump genes. Antimicrob. Agents Chemother. 45, 1126–1136 (2001).
Lomovskaya, O. et al. Identification and characterization of inhibitors of multidrug resistance efflux pumps in Pseudomonas aeruginosa: novel agents for combination therapy. Antimicrob. Agents Chemother. 45, 105–116 (2001).
Anes, J., Sivasankaran, S. K., Muthappa, D. M., Fanning, S. & Srikumar, S. Exposure to sub-inhibitory concentrations of the chemosensitizer 1-(1-naphthylmethyl)-piperazine creates membrane destabilization in multi-drug resistant Klebsiella pneumoniae. Front. Microbiol. 10, 92 (2019).
Misra, R., Morrison, K. D., Cho, H. J. & Khuu, T. Importance of real-time assays to distinguish multidrug efflux pump-inhibiting and outer membrane-destabilizing activities in Escherichia coli. J. Bacteriol. 197, 2479–2488 (2015).
Lee, A. et al. Interplay between efflux pumps may provide either additive or multiplicative effects on drug resistance. J. Bacteriol. 182, 3142–3150 (2000).
Tal, N. & Schuldiner, S. A coordinated network of transporters with overlapping specificities provides a robust survival strategy. Proc. Natl Acad. Sci. USA 106, 9051–9056 (2009).
Vega, D. E. & Young, K. D. Accumulation of periplasmic enterobactin impairs the growth and morphology of Escherichia coli tolC mutants. Mol. Microbiol. 91, 508–521 (2014).
Zwama, M., Yamaguchi, A. & Nishino, K. Phylogenetic and functional characterisation of the Haemophilus influenzae multidrug efflux pump AcrB. Commun. Biol. 2, 340 (2019).
Brown, D. G., May-Dracka, T. L., Gagnon, M. M. & Tommasi, R. Trends and exceptions of physical properties on antibacterial activity for Gram-positive and Gram-negative pathogens. J. Med. Chem. 57, 10144–10161 (2014).
Takatsuka, Y., Chen, C. & Nikaido, H. Mechanism of recognition of compounds of diverse structures by the multidrug efflux pump AcrB of Escherichia coli. Proc. Natl Acad. Sci. USA 107, 6559–6565 (2010).
Johnson, J. W. et al. Antibacterial activity of metergoline analogues: revisiting the ergot alkaloid scaffold for antibiotic discovery. ACS Med. Chem. Lett. 13, 284–291 (2022).
Kearse, M. et al. Geneious Basic: an integrated and extendable desktop software platform for the organization and analysis of sequence data. Bioinformatics 28, 1647–1649 (2012).
Patel, J. B. et al. M07-A10: Methods for Dilution Antimicrobial Susceptibility Tests for Bacteria That Grow Aerobically; Approved Standard 10th edn (Clinical Laboratory Standards Institute, 2015).
Hazel, A. J. et al. Conformational dynamics of AcrA govern multidrug efflux pump assembly. ACS Infect. Dis. 5, 1926–1935 (2019).
Rappsilber, J., Mann, M. & Ishihama, Y. Protocol for micro-purification, enrichment, pre-fractionation and storage of peptides for proteomics using StageTips. Nat. Protoc. 2, 1896–1906 (2007).
Cox, J. & Mann, M. MaxQuant enables high peptide identification rates, individualized p.p.b.-range mass accuracies and proteome-wide protein quantification. Nat. Biotechnol. 26, 1367–1372 (2008).
Cox, J. et al. Accurate proteome-wide label-free quantification by delayed normalization and maximal peptide ratio extraction, termed MaxLFQ. Mol. Cell. Proteom. 13, 2513–2526 (2014).
Tyanova, S. et al. The Perseus computational platform for comprehensive analysis of (prote)omics data. Nat. Methods 13, 731–740 (2016).
Cox, J. & Mann, M. 1D and 2D annotation enrichment: a statistical method integrating quantitative proteomics with complementary high-throughput data. BMC Bioinf. 13, S12 (2012).
Acknowledgements
This study was supported by a Natural Sciences and Engineering Research Council of Canada (NSERC) Discovery grant (no. RGPIN-2019-04996) and a Canada Foundation for Innovation (CFI) grant no. JELF 37730 awarded to G.C., a Postgraduate Scholarship (NSERC) awarded to L.K.T., an Ontario Graduate Scholarship awarded to S.Z. and a Canadian Graduate Scholarship awarded to J.A.G. This research was also supported by a Foundation grant from the Canadian Institutes of Health Research (grant no. FRN 143215), infrastructure funding from the CFI, a Research Excellence allocation from the Ontario Research Fund, and a Tier I Canada Research Chair award to E.D.B. We thank K. Klaus and H. Green-Glass for their assistance with aspects of efflux gene inactivation. We also thank T. Bhando for providing the E. coli Pore strain used for the generation of the EKO-35-Pore, H. Zgurskaya for donating the anti-AcrB antibody used in western blotting and C. Murphy and L. Carfrae for assistance with high-throughput susceptibility testing at the Center for Microbial Chemical Biology (CMCB), McMaster University. Last, we thank J. Krieger (Bioinformatics Solutions Inc.) for operating the mass spectrometer for the proteomics experiments and E. Roach (Advanced Analysis Center, University of Guelph) for technical assistance with generation of the scanning electron microscopy images.
Author information
Authors and Affiliations
Contributions
G.C. conceived the research. G.C. and E.D.B. guided the research. G.C., T.T., L.K.T. and C.R.M. designed the experiments. G.C., T.T., L.K.T., S.Z., S.E.G., C.R.M., N.M.K. and J.A.G. performed experiments. L.K.T. and S.Z. analyzed the genome sequence data. L.K.T. prepared the proteomic samples and analyzed the data with guidance from J.G.-M. The high-throughput susceptibility testing was performed by T.T., S.Z., N.M.K., C.R.M. and S.E.G. T.T. and S.Z. analyzed the data. G.C., T.T., L.K.T. and S.Z. wrote the manuscript and all authors commented on and approved the paper.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Chemical Biology thanks Jessica Blair, Karl Hassan and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Plasmid-based complementation of genes harboring nonsynonymous mutations in EKO-35 is detrimental in EKO-35 and wild-type E. coli.
Growth profiling of EKO-35 with ASKA constructs expressing a, pitA b, rspA c, tufA d, yjfC e, wcaC f, gyrB in i, nutrient-rich Lysogeny broth and ii, M9 minimal glucose medium. Solid symbols represent empty vector controls while open symbols represent ASKA expressing constructs. Gene expression was induced with 0.1 mM IPTG and plasmid selection for EKO-35 was achieved using 1 µg/mL in M9 minimal glucose medium and 4 µg/mL in Lysogeny broth. Data points represent mean values of n = 3 biological replicates.
Extended Data Fig. 2 The growth of EKO-35 at acidic and alkaline pH is not restored through plasmid-based complementation of genes in EKO-35 harboring nonsynonymous genomic mutations.
EKO-35 growth is significantly reduced at a, pH 5.0 and is not restored through expression of rspA, pitA, tufa, gyrB, wcaC, and yjfC (P = 6.53 × 10−8, 5.34 × 10−7, 2.52 × 10−8, 3.16 × 10-7, 6.75 × 10−8, 4.80 × 10-8 respectively). Likewise, growth was not restored at b, pH 5.5 (P = 1.00 × 10−7, 1.03 × 10−7, 1.18 × 10−7, 1.45 × 10−6, 4.05 × 10−7, 4.02 × 10−4 respectively). EKO-35 expressing ASKA constructs did not grow at c, 8.5 and d, 9.0. Gene expression was induced with 0.1 mM IPTG and plasmid selection for EKO-35 was achieved using 1 µg/mL chloramphenicol. Data points represent mean values ± s.d. of n = 3 biological end-point readings after 18 h of growth. P-values were calculated by a two-tailed Student’s t-test (****P < 0.0001, ns = not significant) relative to EKO-35 pCA24N.
Extended Data Fig. 3 Plasmid-based complementation of genes in EKO-35 harboring genomic mutations alters biofilm formation in EKO-35 and wild-type E. coli.
Expression of rspA significantly increased biofilm formation in a, wild-type E. coli (P = 2.67 × 10−3) and b, EKO-35 (P = 3.35 × 10−2) in Lysogeny broth, whilst expression of pitA, tufA, gyrB, and yjfC significantly lowered biofilm formation in wild-type E. coli (P = 4.70 × 10−4, 2.98 × 10−5, 6.56 × 10−3, 1.09 × 10−3 respectively) and pitA, tufA, and yjfC in EKO-35 (P = 3.00 × 10−3, 1.65 × 10−1, 8.36 × 10−2, 3.09 × 10−3 respectively). Gene expression was induced using 0.1 mM IPTG and plasmid selection for EKO-35 was achieved using 1 µg/mL chloramphenicol in M9 minimal glucose medium and 4 µg/mL in Lysogeny broth. Data points represent mean values ± s.d. of n = 3 biological end-point readings after 24 h and 48 h of growth in nutrient-rich and -limited media, respectively. P-values were calculated by a two-tailed Student’s t-test (*P < 0.05, **P < 0.01, ***P < 0.001, ****P < 0.0001, ns = not significant).
Extended Data Fig. 4
Plasmid-based complementation of genes harboring nonsynonymous mutations in EKO-35 is detrimental in EKO-35 and wild-type E. coli under low oxygen conditions. Growth profiling of EKO-35 in low oxygen environments with ASKA constructs expressing a, pitA b, rspA c, tufA d, yjfC e, wcaC f, gyrB in i, Lysogeny broth with 10 mM KNO3 (1% oxygen) and ii, M9 minimal glucose medium (5% oxygen). Solid symbols represent empty vector controls while open symbols represent ASKA expressing constructs. Gene expression was induced with 0.1 mM IPTG and plasmid maintenance for EKO-35 was achieved using 1 µg/mL chloramphenicol in M9 minimal glucose medium and 4 µg/mL chloramphenicol in Lysogeny broth. Data points represent mean values of n = 3 biological replicates. P-values were calculated by a two-tailed Student’s t-test (*P < 0.05, **P < 0.01, ***P < 0.001, ****P < 0.0001, ns = not significant).
Extended Data Fig. 5 Assessing the susceptibility of EKO-35 harboring ASKA plasmids expressing rspA, tufA, pitA, wcaC, gyrB, and yjfC.
Strains were profiled against a, benzalkonium chloride, b, novobiocin, c, trimethoprim, d, synthetic 2, e, synthetic 14, f, synthetic 19. MICs were determined i, without and ii, with chloramphenicol to maintain ASKA plasmids. Gene expression was induced with 0.1 mM IPTG. 25 µg/mL and 4 µg/mL chloramphenicol were used to maintain ASKA plasmids in wild-type E. coli and EKO-35, respectively. Strains were assessed in technical duplicate.
Extended Data Fig. 6 Susceptibility and growth profiling of porinated wild-type (WT) K-12, ∆tolC, and EKO-35 strains in LB at 37 °C.
a, Measurement of growth kinetics revealed the pore marginally extended the lag phase of EKO-35-Pore (P = 0.013), and did not significantly impact the generation time of EKO-35-Pore (P = 0.29) compared to the non-porinated parental strains, which was assessed using n = 3 biological replicates. Statistical analysis was performed using a two-tailed Student’s t-test. b, Heatmap depicting vancomycin susceptibility of the porinated strains. Each strain was tested in technical duplicate and MIC values were normalized to 100%, where green represents the highest MIC value, and white represents the lowest value (see key). Susceptibility of the WT K-12, ∆tolC, and EKO-35 strains + /- the pore was assessed for 52 compounds. The physicochemical properties for each compound that resulted in a 4-fold or greater increase in susceptibility compared to the wild-type strain are presented as individual data points in the box plots. The line through the center of each box indicates the median, and whiskers the minimum and maximum values. Physicochemical properties were calculated using DataWarrior (Version 5.5.0): c, Molecular weight (MW); d, Lipophilicity (logP); e, Aqueous solubility (logS); and f, Polar Surface Area (PSA). n for each strain is defined as the number of active compounds that decreased the MIC value by ≥4-fold compared to the WT K-12 strain as listed in panel g. The bounds of the boxes represent 25% (Q1) to 75% (Q3) of the physicochemical substrate ranked ranges, which are also summarized in panel g. g, Summary of the physicochemical property ranges for each strain. Medians are indicated in parentheses.
Extended Data Fig. 7 Heat maps depicting susceptibility levels of strains expressing efflux pump-encoding genes.
Each strain was tested in technical duplicate and MIC values were normalized to 100% for each compound tested, where orange represents the highest MIC value, and white represents the lowest value (see key). Genes encoding a, AcrEF, b, AcrD, c, AcrB, d, MdtEF, e, MdtBC, f, MacAB, g, MacAB, and h, MexCD were chromosomally integrated into the wild-type strain, a single gene deletion mutant, and EKO-35. Susceptibility testing revealed no changes in the resistance levels of the wild-type or single gene deletion backgrounds, except for c, ΔacrB. EKO-35 was highly susceptible to all compounds tested, revealing susceptibility profiles similar to ΔtolC, and integration of efflux genes into this strain conferred resistance to the known substrates.
Extended Data Fig. 8 Heat maps depicting aminoglycoside susceptibility of the wild-type K-12 strain and an ΔacrD mutant expressing the chromosomally integrated acrD gene (araC::acrD).
Susceptibility testing was performed in both MHB and LB. a, Kanamycin in cation-adjusted Mueller Hinton II Broth (MHB II), b, Kanamycin in Lysogeny broth (LB), c, Gentamicin in MHB II, and d, Gentamicin in LB. The cell inoculum used was 104 cells/mL to replicate susceptibility testing conditions used in previous studies. Each strain was assessed using three technical replicates and MIC values were normalized to 100% for each compound tested, where orange represents the highest MIC value, and white represents the lowest value (see key).
Extended Data Fig. 9 EKO-35 and the efflux platform can be used to assess efflux pump inhibitor specificities.
Bar charts depicting fractional inhibitory concentration index (FICI) values of a, phenylalanine-arginine-β-naphthylamide (PAβN) in combination with fusidic acid and ciprofloxacin, in addition to FICI values of b, 1-(1-naphthylmethyl)-piperazine (NMP) in combination with fusidic acid and ciprofloxacin. The FICI represents the ΣFIC of each drug. The FIC for each drug was determined by dividing the MIC of each drug in combination, by the MIC of each drug alone. ΣFIC = FICA + FICB = (CA/MICA) + (CB/MICB). Synergy (FICI < 0.5), additive (FICI > 0.5–1.0), indifferent (FICI > 1.0–2.0), and antagonistic (FICI > 2.0), as highlighted on each bar chart. Related to Supplementary Datasets 3 and 4.
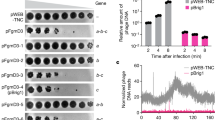
Extended Data Fig. 10 EKO-35 and the efflux platform can be used to assess efflux pump interplay.
Interplay was not observed for novobiocin in a, EKO-35 and b, EKO-35-Pore or for minocycline in c, EKO-35 and d, EKO-35-Pore. pGDP-2 harboring emrE is denoted as pEmrE. All integrated strains were transformed with the empty vector (pGDP-2). Genes encoding AcrB, AcrEF, AcrD, and MdtEF were integrated into the arabinose operon (araC) of EKO-35. Related to Fig. 5 and Supplementary Dataset 5. Data points represent mean MIC values for which the OD600nm value >0.100 ± s.d. of n = 3 biological replicates. P-values were calculated by a two-tailed Student’s t-test (ns = not significant).
Supplementary information
Supplementary Information
Supplementary Figs. 1–5 and Tables 1–13.
Supplementary Data 1
MICs of various compounds against the wild-type K-12, ΔtolC, EKO-35 and the efflux-integrated EKO-35 strains, which were used to calculate fold change.
Supplementary Data 2
MICs of various compounds against the wild-type (WT)-Pore, ΔtolC-Pore, EKO-35-Pore and the efflux-integrated EKO-35-Pore strains, which were used to calculate fold change.
Supplementary Data 3
The FICI for PAβN in combination with different antibiotics using EKO-35 and the efflux platform.
Supplementary Data 4
The FICI for NMP in combination with different antibiotics using EKO-35 and the efflux platform.
Supplementary Data 5
Assessing efflux pump interplay using EKO-35 and the efflux platform.
Supplementary Data 6
Strains and plasmids used in this study.
Supplementary Data 7
Primers and oligonucleotides used in this study.
Source data
Source Data Fig. 1
Statistical source data.
Source Data Fig. 1
Unprocessed western blots.
Source Data Fig. 2
Statistical source data.
Source Data Fig. 3
Statistical source data.
Source Data Fig. 4
Statistical source data.
Source Data Fig. 5
Statistical source data.
Source Data Extended Data Fig. 1
Statistical source data.
Source Data Extended Data Fig. 2
Statistical source data.
Source Data Extended Data Fig. 3
Statistical source data.
Source Data Extended Data Fig. 4
Statistical source data.
Source Data Extended Data Fig. 5
Statistical source data.
Source Data Extended Data Fig. 6
Statistical source data.
Source Data Extended Data Fig. 7
Statistical source data.
Source Data Extended Data Fig. 8
Statistical source data.
Source Data Extended Data Fig. 9
Statistical source data.
Source Data Extended Data Fig. 10
Statistical source data.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Teelucksingh, T., Thompson, L.K., Zhu, S. et al. A genetic platform to investigate the functions of bacterial drug efflux pumps. Nat Chem Biol 18, 1399–1409 (2022). https://doi.org/10.1038/s41589-022-01119-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41589-022-01119-y
This article is cited by
-
Pyridylpiperazine efflux pump inhibitor boosts in vivo antibiotic efficacy against K. pneumoniae
EMBO Molecular Medicine (2023)