Abstract
Background
Phthalates are used in the manufacturing of consumer products, resulting in ubiquitous human exposure to phthalate mixtures. Previous work has suggested that phthalates display endocrine-disrupting capabilities, and exposure is associated with early delivery.
Objective
To assess mediating effects of hormone concentrations on associations between phthalate mixtures and preterm birth (PTB).
Methods
Repeated urinary phthalates and serum hormones were measured among 1011 women in the PROTECT Puerto Rico birth cohort from 2011–2019. We utilized ridge regression to create phthalate environmental risk scores (ERS), which represent weighted summaries of total phthalate exposure. Mediation analyses were conducted on a subset of 705 women. We additionally conducted fetal sex-specific analyses.
Results
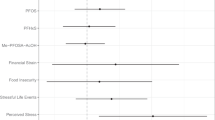
Free thyroxine (FT4) mediated 9.6% of the association between high molecular weight (HMW) ERS at 18 weeks and reduced gestational age at delivery (95%CI:1.07–29.9). Progesterone at 26 weeks mediated 21.1% and 16.2% of the association between HMW ERS at 18 and 22 weeks, and spontaneous PTB, respectively. Among male fetuses, corticotropin releasing hormone (CRH) at 18 weeks mediated 28.2% of the association between low molecular weight ERS and spontaneous PTB.
Significance
We provide introductory evidence of hormone disruption on the causal pathway between phthalate exposure and early delivery. We also show differences by fetal sex, but larger sample size is necessary to validate our findings.
Impact statement
This study provides introductory evidence that an alteration of hormone concentrations occurs on the causal pathway between gestational phthalate mixture exposure and subsequent PTB. In addition to the novel application of repeated biomarker measurements and mixtures methods in causal mediation analyses, we also explored differences between classes of phthalate compounds and between fetal sexes. We show that differential endocrine pathways may be disrupted with exposures to low versus HMW phthalate compounds, and that pregnancies with a male fetus may be more susceptible to endocrine disruption than those with a female fetus.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 print issues and online access
$259.00 per year
only $43.17 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The data dictionary for all variables used in this analysis is publicly available and can be found here: https://arecibo.ece.neu.edu/dictionary/. Any data requested will be made available by contacting the authors, who will forward to request to the PROTECT DMAC database manager. The request will be reviewed with the data owners, who will provide an export of the requested data after approval. All data from the database will be deidentified, individual level, participant data. All data is available now and will remain available until at least January 1, 2025. Any data requester must agree to acknowledge the NIEHS P42 Center grant that supported the collection of this data. Additional files, including analysis code, will also be provided by contacting the first and corresponding authors.
References
Mannisto T, Mendola P, Grewal J, Xie Y, Chen Z, Laughon SK. Thyroid diseases and adverse pregnancy outcomes in a contemporary US cohort. J Clin Endocrinol Metab. 2013;98:2725–33.
Nazarpour S, Ramezani Tehrani F, Simbar M, Azizi F. Thyroid dysfunction and pregnancy outcomes. Iran J Reprod Med. 2015;13:387–96.
Weiss G. Endocrinology of parturition. J Clin Endocrinol Metab. 2000;85:4421–5.
Sykes L, Bennett PR. Efficacy of progesterone for prevention of preterm birth. Best Pr Res Clin Obstet Gynaecol. 2018;52:126–36.
Schettler T. Human exposure to phthalates via consumer products. Int J Androl. 2006;29:134–5.
Rodríguez-Carmona Y, Ashrap P, Calafat AM, Ye X, Rosario Z, Bedrosian LD, et al. Determinants and characterization of exposure to phthalates, DEHTP and DINCH among pregnant women in the PROTECT birth cohort in Puerto Rico. J Expo Sci Environ Epidemiol. 2020;30:56–69.
Frederiksen H, Skakkebæk NE, Andersson AM. Metabolism of phthalates in humans. Mol Nutr Food Res. 2007;51:899–911.
Meeker JD, Hu H, Cantonwine DE, Lamadrid-Figueroa H, Calafat AM, Ettinger AS, et al. Urinary phthalate metabolites in relation to preterm birth in Mexico City. Environ Health Perspect. 2009;117:1587–92.
Gao H, Wang Y-F, Huang K, Han Y, Zhu Y-D, Zhang Q-F, et al. Prenatal phthalate exposure in relation to gestational age and preterm birth in a prospective cohort study. Environ Res. 2019;176:108530.
Boss J, Zhai J, Aung MT, Ferguson KK, Johns LE, McElrath TF, et al. Associations between mixtures of urinary phthalate metabolites with gestational age at delivery: a time to event analysis using summative phthalate risk scores. Environ Health. 2018;17:56.
Adibi JJ, Hauser R, Williams PL, Whyatt RM, Calafat AM, Nelson H, et al. Maternal urinary metabolites of Di-(2-Ethylhexyl) phthalate in relation to the timing of labor in a US multicenter pregnancy cohort study. Am J Epidemiol. 2009;169:1015–24.
Cathey AL, Watkins D, Rosario ZY, Velez C, Alshawabkeh AN, Cordero JF, et al. Associations of phthalates and phthalate replacements with CRH and other hormones among pregnant women in Puerto Rico. J Endocr Soc. 2019;3:1127–49.
Johns LE, Ferguson KK, McElrath TF, Mukherjee B, Meeker JD. Associations between repeated measures of maternal urinary phthalate metabolites and thyroid hormone parameters during pregnancy. Environ Health Perspect. 2016;124:1808–15.
Romano ME, Eliot MN, Zoeller RT, Hoofnagle AN, Calafat AM, Karagas MR, et al. Maternal urinary phthalate metabolites during pregnancy and thyroid hormone concentrations in maternal and cord sera: The HOME Study. Int J Hyg Environ Health. 2018;221:623–31.
Sathyanarayana S, Butts S, Wang C, Barrett E, Nguyen R, Schwartz SM, et al. Early prenatal phthalate exposure, sex steroid hormones, and birth outcomes. J Clin Endocrinol Metab. 2017;102:1870–8.
Meeker JD, Cantonwine DE, Rivera-González LO, Ferguson KK, Mukherjee B, Calafat AM, et al. Distribution, variability, and predictors of urinary concentrations of phenols and parabens among pregnant women in puerto rico. Environ Sci Technol. 2013;47:3439–47.
Silva MJ, Samandar E, Preau JL Jr., Reidy JA, Needham LL, Calafat AM. Quantification of 22 phthalate metabolites in human urine. J Chromatogr B. 2007;860:106–12.
Hornung RW, Reed LD. Estimation of average concentration in the presence of nondetectable values. Appl Occup Environ Hyg. 1990;5:46–51.
Dietrich JW, Landgrafe G, Fotiadou EH. TSH and thyrotropic agonists: Key actors in thyroid homeostasis. J Thyroid Res. 2012;2012:351864. https://doi.org/10.1155/2012/351864.
Ruiz RJ, Saade GR, Brown CEL, Nelson-Becker C, Tan A, Bishop S, et al. The effect of acculturation on progesterone/estriol ratios and preterm birth in hispanics. Obstet Gynecol. 2008;111:309–16.
Pettker C, Goldberg J, El-Sayed Y, Copel J. Committee opinion no 700: methods for estimating the due date. Obstet Gynecol. 2017;129:e150–e154.
McElrath TF, Hecht JL, Dammann O, Boggess K, Onderdonk A, Markenson G, et al. Pregnancy disorders that lead to delivery before the 28th week of gestation: an epidemiologic approach to classification. Am J Epidemiol. 2008;168:980–9.
Park SK, Zhao Z, Mukherjee B. Construction of environmental risk score beyond standard linear models using machine learning methods: application to metal mixtures, oxidative stress and cardiovascular disease in NHANES. Environ Health. 2017;16:102.
Aung MT, Song Y, Ferguson KK, Cantonwine DE, Zeng L, McElrath TF, et al. Application of an analytical framework for multivariate mediation analysis of environmental data. Nat Commun. 2020;11:5624.
Eales J, Bethel A, Galloway T, Hopkinson P, Morrissey K, Short RE, et al. Human health impacts of exposure to phthalate plasticizers: An overview of reviews. Environ Int. 2021;158:106903.
Radke EG, Glenn BS, Braun JM, Cooper GS. Phthalate exposure and female reproductive and developmental outcomes: a systematic review of the human epidemiological evidence. Environ Int. 2019;130:104580.
Yaghjyan L, Ghita GL, Dumont-Driscoll M, Yost RA, Chang S-H. Maternal exposure to di-2-ethylhexylphthalate and adverse delivery outcomes: A systematic review. Reprod Toxicol. 2016;65:76–86.
Marie C, Vendittelli F, Sauvant-Rochat M-P. Obstetrical outcomes and biomarkers to assess exposure to phthalates: A review. Environ Int. 2015;83:116–36.
Yen PM. Physiological and molecular basis of thyroid hormone action. Physiol Rev. 2001;81:1097–142.
Huang PC, Kuo PL, Guo YL, Liao PC, Lee CC. Associations between urinary phthalate monoesters and thyroid hormones in pregnant women. Hum Reprod. 2007;22:2715–22.
Johns LE, Ferguson KK, McElrath TF, Mukherjee B, Seely EW, Meeker JD. Longitudinal profiles of thyroid hormone parameters in pregnancy and associations with preterm birth. PLoS One. 2017;12:1–15.
Sheikh IA, Abu-Elmagd M, Turki RF, Damanhouri GA, Beg MA, Al-Qahtani M. Endocrine disruption: In silico perspectives of interactions of di-(2-ethylhexyl)phthalate and its five major metabolites with progesterone receptor. BMC Struct Biol. 2016;16:1–10.
Zhang S, Sun C, Zhao S, Wang B, Wang H, Zhang J, et al. Exposure to DEHP or its metabolite MEHP promotes progesterone secretion and inhibits proliferation in mouse placenta or JEG-3 cells. Environ Pollut. 2020;257:113593.
Ruge S, Sørensen S, Pedersen JF, Lange AP, Byrjalsen I, Bohn H. Secretory endometrial protein PP14 in women with early pregnancy bleeding. Hum Reprod. 1991;6:885–8.
Okon MA, Laird SM, Tuckerman EM, Li TC. Serum androgen levels in women who have recurrent miscarriages and their correlation with markers of endometrial function. Fertil Steril. 1998;69:682–90.
Dalton CF, Laird SM, Serle E, Saravelos H, Warren MA, Li TC, et al. The measurement of CA 125 and placental protein 14 in uterine flushings in women with recurrent miscarriage; relation to endometrial morphology. Hum Reprod. 1995;10:2680–4.
Tulppala M, Julkunen M, Tiitinen A, Stenman UH, Seppälä M. Habitual abortion is accompanied by low serum levels of placental protein 14 in the luteal phase of the fertile cycle. Fertil Steril. 1995;63:792–5.
McLean M, Bisits A, Davies J, Woods R, Lowry P, Smith R. A placental clock controlling the length of human pregnancy. Nat Med. 1995;1:460–3.
Smith R, Mesiano S, Chan EC, Brown S, Jaffe RB. Corticotropin-releasing hormone directly and preferentially stimulates dehydroepiandrosterone sulfate secretion by human fetal adrenal cortical cells. J Clin Endocrinol Metab. 1998;83:2916–20.
Acknowledgements
We would like to extend our gratitude to all PROTECT study participants and their families. The authors also thank the nurses and research staff who participated in cohort recruitment and follow up, as well as the Federally Qualified Health Centers (FQHC) in Puerto Rico that facilitated participant recruitment, including Morovis Community Health Center, Prymed in Ciales, Camuy Health Services, Inc. and the Delta OBGyn Group in Manati, as well as the Manati Medical Center and the Metro Pavia Hospital in Arecibo.
Funding
This study was supported by the Superfund Research Program of the National Institute of Environmental Health Sciences (NIEHS), National Institutes of Health (NIH; grant number P42ES017198). Additional support was provided from NIEHS grant numbers P30ES017885, R01ES031591, R01ES032202, and T32ES007062, and the Environmental influences on Child Health Outcomes (ECHO) program grant number UH3OD023251. ECHO is a nationwide research program supported by the NIH, Office of the Director to enhance child health.
Author information
Authors and Affiliations
Contributions
AC: Formal analysis, investigation, methodology, visualization, writing—original draft, writing—review and editing; MA: Methodology, writing—review and editing; DW: Supervision, writing—review and editing; ZR: Data curation, resources; CVV: Funding acquisition; AA: Funding acquisition, project administration; JC: Funding acquisition; BM: Conceptualization, methodology, supervision, writing—review and editing; JM: Conceptualization, funding acquisition, project administration, supervision, writing—review and editing.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Cathey, A.L., Aung, M.T., Watkins, D.J. et al. Mediation by hormone concentrations on the associations between repeated measures of phthalate mixture exposure and timing of delivery. J Expo Sci Environ Epidemiol 32, 374–383 (2022). https://doi.org/10.1038/s41370-021-00408-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41370-021-00408-3