Abstract
Objective
The intestinal immune response could play an important role in obesity-related comorbidities. We aim to study the profile of duodenal cytokines and chemokines in patients with morbid obesity (MO), its relation with insulin resistance (IR) and the intake of metformin, and with the evolution of MO after sleeve gastrectomy (SG).
Research design and methods
Duodenal levels of 24 cytokines and 9 chemokines were analyzed in 14 nonobese and in 54 MO who underwent SG: with lower IR (MO-lower-IR), with higher IR (MO-higher-IR), and with type 2 diabetes treated with metformin (MO-metf-T2DM).
Results
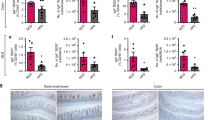
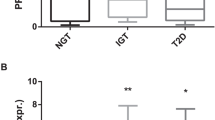
MO-lower-IR had higher levels of cytokines related to Th1, Th2, Th9, Th17, Th22, M1 macrophages, and chemokines involved in the recruitment of macrophages and T-lymphocytes (p < 0.05), and total (CD68 expression) and M1 macrophages (ITGAX expression) (p < 0.05) when compared with nonobese patients, but with a decrease in M2 macrophages (MRC1 expression) (p < 0.05). In MO-higher-IR, these chemokines and cytokines decreased and were similar to those found in nonobese patients. In MO-metf-T2DM, only IL-4 (Th2) and IL-22 (Th22) increased their levels with regard to MO-higher-IR (p < 0.05). In MO-higher-IR and MO-metf-T2DM, there was a decrease of CD68 expression (p < 0.05) while ITGAX and MRC1 were similar with regard to MO-lower-IR. We found an association between CXCL8, TNFβ and IL-2 with the evolution of body mass index (BMI) after SG (p < 0.05).
Conclusions
There is an association between a higher IR and a lower duodenal immune response in MO, with a slight increase in those patients with metformin treatment. Intestinal immune response could be involved in the evolution of BMI after SG.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Barbarroja N, López-Pedrera R, Mayas MD, García-Fuentes E, Garrido-Sánchez L, Macías-González M, et al. The obese healthy paradox: is inflammation the answer? Biochem J. 2010;430:141–9.
Zeyda M, Stulnig TM. Obesity, inflammation, and insulin resistance-a mini-review. Gerontology. 2009;55:379–86.
Lumeng CN, Bodzin JL, Saltiel AR. Obesity induces a phenotypic switch in adipose tissue macrophage polarization. J Clin Investig. 2007;117:175–84.
Winer DA, Winer S, Shen L, Wadia PP, Yantha J, Paltser G, et al. B cells promote insulin resistance through modulation of T cells and production of pathogenic IgG antibodies. Nat Med. 2011;17:610–7.
Molofsky AB, Nussbaum JC, Liang HE, Van Dyken SJ, Cheng LE, Mohapatra A, et al. Innate lymphoid type 2 cells sustain visceral adipose tissue eosinophils and alternatively activated macrophages. J Exp Med. 2013;210:535–49.
Raphael I, Nalawade S, Eagar TN, Forsthuber TG. T cell subsets and their signature cytokines in autoimmune and inflammatory diseases. Cytokine. 2015;74:5–17.
Martinez FO, Sica A, Mantovani A, Locati M. Macrophage activation and polarization. Front Biosci. 2008;13:453–61.
Crane MJ, Daley JM, van Houtte O, Brancato SK, Henry WL Jr, Albina JE. The monocyte to macrophage transition in the murine sterile wound. PLoS ONE. 2014;9:e86660.
Monteiro-Sepulveda M, Touch S, Mendes-Sá C, André S, Poitou C, Allatif O, et al. Jejunal T cell inflammation in human obesity correlates with decreased enterocyte insulin signaling. Cell Metab. 2015;22:113–24.
Ding S, Lund PK. Role of intestinal inflammation as an early event in obesity and insulin resistance. Curr Opin Clin Nutr Metab Care. 2011;14:328–33.
Winer DA, Luck H, Tsai S, Winer S. The intestinal immune system in obesity and insulin resistance. Cell Metab. 2016;23:413–26.
Hard GC. Some biochemical aspects of the immune macrophage. Br J Exp Pathol. 1970;51:97–105.
Lopes EC, Heineck I, Athaydes G, Meinhardt NG, Souto KE, Stein AT. Is bariatric surgery effective in reducing comorbidities and drug costs? A systematic review and meta-analysis. Obes Surg. 2015;25:1741–9.
Gutierrez-Repiso C, Garcia-Serrano S, Moreno-Ruiz FJ, Alcain-Martinez G, Rodriguez-Pacheco F, Garcia-Fuentes E. Jejunal gluconeogenesis associated with insulin resistance level and its evolution after Roux-en-Y gastric bypass. Surg Obes Relat Dis. 2017;13:623–30.
García-Fuentes E, García-Almeida JM, García-Arnés J, Rivas-Marín J, Gallego-Perales JL, González-Jiménez B, et al. Morbidly obese individuals with impaired fasting glucose have a specific pattern of insulin secretion and sensitivity: effect of weight loss after bariatric surgery. Obes Surg. 2006;16:1179–88.
Rodriguez-Pacheco F, Garcia-Serrano S, Garcia-Escobar E, Gutierrez-Repiso C, Garcia-Arnes J, Valdes S, et al. Effects of obesity/fatty acids on the expression of GPR120. Mol Nutr Food Res. 2014;58:1852–60.
Bisgaard LS, Mogensen CK, Rosendahl A, Cucak H, Nielsen LB, Rasmussen SE, et al. Bone marrow-derived and peritoneal macrophages have different inflammatory response to oxLDL and M1/M2 marker expression - implications for atherosclerosis research. Sci Rep. 2016;6:35234.
Escamilla A, Bautista MJ, Zafra R, Pacheco IL, Ruiz MT, Martínez-Cruz S, et al. Fasciola hepática induces eosinophil apoptosis in the migratory and biliary stages of infection in sheep. Vet Parasitol. 2016;216:84–88.
Wynn TA. Type 2 cytokines: mechanisms and therapeutic strategies. Nat Rev Immunol. 2015;15:271–82.
Mantovani A, Biswas SK, Galdiero MR, Sica A, Locati M. Macrophage plasticity and polarization in tissue repair and remodelling. J Pathol. 2013;229:176–85.
Hussaarts L, García-Tardón N, van Beek L, Heemskerk MM, Haeberlein S, van der Zon GC, et al. Chronic helminth infection and helminth-derived egg antigens promote adipose tissue M2 macrophages and improve insulin sensitivity in obese mice. FASEB J. 2015;29:3027–39.
Ye J, McGuinness OP. Inflammation during obesity is not all bad: evidence from animal and human studies. Am J Physiol Endocrinol Metab. 2013;304:E466–E477.
Kuhn KA, Manieri NA, Liu TC, Stappenbeck TS. IL-6 stimulates intestinal epithelial proliferation and repair after injury. PLoS ONE. 2014;9:e114195.
Obermeier F, Hausmann M, Kellermeier S, Kiessling S, Strauch UG, Duitman E, et al. IL-15 protects intestinal epithelial cells. Eur J Immunol. 2006;36:2691–9.
Araújo JR, Tomas J, Brenner C, Sansonetti PJ. Impact of high-fat diet on the intestinal microbiota and small intestinal physiology before and after the onset of obesity. Biochimie. 2017;141:97–106.
Moreno-Navarrete JM, Sabater M, Ortega F, Ricart W, Fernández-Real JM. Circulating zonulin, a marker of intestinal permeability, is increased in association with obesity-associated insulin resistance. PLoS ONE. 2012;7:e37160.
Cani PD, Bibiloni R, Knauf C, Waget A, Neyrinck AM, Delzenne NM, et al. Changes in gut microbiota control metabolic endotoxemia-induced inflammation in high-fat diet-induced obesity and diabetes in mice. Diabetes. 2008;57:1470–81.
Sallusto F, Lanzavecchia A, Mackay CR. Chemokines and chemokine receptors in T-cell priming and Th1/Th2-mediated responses. Immunol Today. 1998;19:568–74.
Dickensheets HL, Donnelly RP. IFN-gamma and IL-10 inhibit induction of IL–1 receptor type I and type II gene expression by IL–4 and IL–13 in human monocytes. J Immunol. 1997;159:6226–33.
Licona-Limón P, Henao-Mejia J, Temann AU, Gagliani N, Licona-Limón I, Ishigame H, et al. Th9 cells drive host immunity against gastrointestinal worm infection. Immunity. 2013;39:744–57.
Kaplan MH. Th9 cells: differentiation and disease. Immunol Rev. 2013;252:104–15.
Dalmas E, Venteclef N, Caer C, Poitou C, Cremer I, Aron-Wisnewsky J, et al. T cell-derived IL-22 amplifies IL-1β-driven inflammation in human adipose tissue: relevance to obesity and type 2 diabetes. Diabetes. 2014;63:1966–77.
Zheng Y, Valdez PA, Danilenko DM, Hu Y, Sa SM, Gong Q, et al. Interleukin-22 mediates early host defense against attaching and effacing bacterial pathogens. Nat Med. 2008;14:282–9.
Cani PD, Osto M, Geurts L, Everard A. Involvement of gut microbiota in the development of low-grade inflammation and type 2 diabetes associated with obesity. Gut Microbes. 2012;3:279–88.
Wang LJ, Cao Y, Shi HN. Helminth infections and intestinal inflammation. World J Gastroenterol. 2008;14:5125–32.
Smith JM, Johanesen PA, Wendt MK, Binion DG, Dwinell MB. CXCL12 activation of CXCR4 regulates mucosal host defense through stimulation of epithelial cell migration and promotion of intestinal barrier integrity. Am J Physiol Gastrointest Liver Physiol. 2005;288:G316–G326.
Veilleux A, Mayeur S, Bérubé JC, Beaulieu JF, Tremblay E, Hould FS, et al. Altered intestinal functions and increased local inflammation in insulin-resistant obese subjects: a gene-expression profile analysis. BMC Gastroenterol. 2015;15:119.
Richard C, Wadowski M, Goruk S, Cameron L, Sharma AM, Field CJ. Individuals with obesity and type 2 diabetes have additional immune dysfunction compared with obese individuals who are metabolically healthy. BMJ Open Diabetes Res Care. 2017;5:e000379.
Cani PD, Amar J, Iglesias MA, Poggi M, Knauf C, Bastelica D, et al. Metabolic endotoxemia initiates obesity and insulin resistance. Diabetes. 2007;56:1761–72.
Sieweke MH, Allen JE. Beyond stem cells: self-renewal of differentiated macrophages. Science. 2013;342:1242974.
Bayer AL, Pugliese A, Malek TR. The IL–2/IL–2R system: from basic science to therapeutic applications to enhance immune regulation. Immunol Res. 2013;57:197–209.
Rotter V, Nagaev I, Smith U. Interleukin-6 (IL-6) induces insulin resistance in 3T3-L1 adipocytes and is, like IL-8 and tumor necrosis factor-alpha, overexpressed in human fat cells from insulin-resistant subjects. J Biol Chem. 2003;278:45777–84.
Lindegaard KK, Jorgensen NB, Just R, Heegaard PM, Madsbad S. Effects of Roux-en-Y gastric bypass on fasting and postprandial inflammation-related parameters in obese subjects with normal glucose tolerance and in obese subjects with type 2 diabetes. Diabetol Metab Syndr. 2015;7:12.
Ruddle NH. Lymphotoxin and TNF: how it all began-a tribute to the travelers. Cytokine Growth Factor Rev. 2014;25:83–89.
Acknowledgements
CIBER Fisiopatología de la Obesidad y Nutrición (CIBEROBN) and CIBER de Diabetes y Enfermedades Metabólicas (CIBERDEM) are initiatives of ISCIII (Spain). We gratefully acknowledge the Imaging platform of the Institute of Biomedical Research in Malaga (IBIMA) (Spain). This work was supported in part by a grant from the Instituto de Salud Carlos III, Spain (PI12/00338) (“Una manera de hacer Europa”). This study has been co-funded by FEDER funds. AHP is supported by a grant from the Ministerio de Educación y Formación Professional (Spain) (FPU14/01972). CSF is supported by a grant from the ISCIII (Spain) (FI16/00241). LGS is supported by the Miguel Servet program from the ISCIII (Spain) (MS13/00188). CR is supported by a grant from BEIPD-COFUND-OPD, (Belgium) (R.EURO.0992-J-F-B-32). EGF is supported by the Nicolas Monardes program from the Consejería de Salud de Andalucía (Spain) (C-0031-2016).
Author information
Authors and Affiliations
Contributions
Conceived and designed the study: EGF. Participated in the selection of patients and samples: EGF, AHP, SGS, MG , CMC, LGS, GAM, BGM, NRS, and LVP. Performed the experiments: AHP, SGS, CSF, AE, and CR. Analyzed the data: AHP, CR, AE, and EGF. Wrote the paper: AHP and EGF. All authors helped to revise the paper and read and approved the final paper. EGF is the guarantor of this paper.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Ho-Plagaro, A., Santiago-Fernandez, C., García-Serrano, S. et al. A lower duodenal immune response is associated with an increase of insulin resistance in patients with morbid obesity. Int J Obes 44, 340–352 (2020). https://doi.org/10.1038/s41366-019-0458-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-019-0458-1
This article is cited by
-
The visceral adipose tissue bacterial microbiota provides a signature of obesity based on inferred metagenomic functions
International Journal of Obesity (2023)