Abstract
Objective
The increasing global prevalence of obesity and its associated disorders points to an urgent need for the development of novel and effective strategies for the prevention of weight gain. Here, we investigated the potential of α-cedrene, a volatile sesquiterpene compound derived from cedarwood oil, in regulation of obesity and delineated the mechanisms involved.
Methods
For the prevention of obesity, C57BL/6 N mice were fed a high-fat diet (HFD) and were orally administered either with vehicle or α-cedrene for 8 weeks. For the therapy of obesity, obese Sprague Dawley rats, induced by a HFD for 8 weeks, were orally treated either with vehicle or α-cedrene for 12 weeks. To determine whether the action of α-cedrene was Adcy3 dependent, Adcy3 heterozygous null mice (Adcy3+/−) and wild-type controls were fed either HFD or α-cedrene supplemented HFD for 17 weeks.
Results
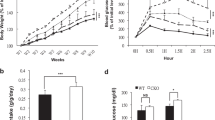
Oral α-cedrene administration prevented or reversed HFD-induced obesity and abnormal metabolic aberrations in rodents, without affecting their food intake. Downregulation of Adcy3 expression by small interfering RNA abrogated the beneficial effects of α-cedrene on the oxygen consumption rate and intracellular lipid accumulation in 3T3-L1 adipocytes. Similarly, in Adcy3+/− mice, the α-cedrene-driven suppression of body weight gain observed in wild-type mice was substantially (~50%) attenuated. Expression of thermogenic and lipid oxidation genes was increased in adipose tissues of α-cedrene-treated mice, with concomitant downregulation of adipogenic gene expression. These beneficial molecular changes elicited by α-cedrene were blunted in adipose tissues of Adcy3+/− mice.
Conclusions
Our results highlight the potential of α-cedrene for antiobesity interventions and suggest that the antiobesity effect of α-cedrene is mediated by Adcy3 in adipose tissues.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Crowley VE, Yeo GS, O’Rahilly S. Obesity therapy: altering the energy intake-and-expenditure balance sheet. Nat Rev Drug Discov. 2002;1:276–86.
Cao H. Adipocytokines in obesity and metabolic disease. J Endocrinol. 2014;220:T47–59.
Haslam DW, James WPT. Obesity. Lancet. 2005;366:1197–209.
Jackson VM, Breen DM, Fortin JP, Liou A, Kuzmiski JB, Loomis AK, et al. Latest approaches for the treatment of obesity. Expert Opin Drug Dis. 2015;10:825–39.
Barja-Fernandez S, Leis R, Casanueva FF, Seoane LM. Drug development strategies for the treatment of obesity: how to ensure efficacy, safety, and sustainable weight loss. Drug Des Dev Ther. 2014;8:2391–2400.
Jackson VM, Price DA, Carpino PA. Investigational drugs in Phase II clinical trials for the treatment of obesity: implications for future development of novel therapies. Expert Opin Investig. Drugs. 2014;23:1055–66.
Zheng W, Thorne N, McKew JC. Phenotypic screens as a renewed approach for drug discovery. Drug Discov Today. 2013;18:1067–73.
Swinney DC. Phenotypic vs. target-based drug discovery for first-in-class medicines. Clin Pharmacol Ther. 2013;93:299–301.
Swinney DC, Anthony J. How were new medicines discovered? Nat Rev Drug Discov. 2011;10:507–19.
Vernochet C, Mourier A, Bezy O, Macotela Y, Boucher J, Rardin MJ, et al. Adipose-specific deletion of TFAM increases mitochondrial oxidation and protects mice against obesity and insulin resistance. Cell Metab. 2012;16:765–76.
Rogne M, Tasken K. Compartmentalization of cAMP signaling in adipogenesis, lipogenesis, and lipolysis. Horm Metab Res. 2014;46:833–40.
Carmen GY, Victor SM. Signalling mechanisms regulating lipolysis. Cell Signal. 2006;18:401–8.
Madsen L, Kristiansen K. The importance of dietary modulation of cAMP and insulin signaling in adipose tissue and the development of obesity. Ann N Y Acad Sci. 2010;1190:1–14.
Harms M, Seale P. Brown and beige fat: development, function and therapeutic potential. Nat Med. 2013;19:1252–63.
Yin W, Mu J, Birnbaum MJ. Role of AMP-activated protein kinase in cyclic AMP-dependent lipolysis in 3T3-L1 adipocytes. J Biol Chem. 2003;278:43074–80.
Omar B, Zmuda-Trzebiatowska E, Manganiello V, Goransson O, Degerman E. Regulation of AMP-activated protein kinase by cAMP in adipocytes: Roles for phosphodiesterases, protein kinase B, protein kinase A, Epac and lipolysis. Cell Signal. 2009;21:760–6.
Qiu L, LeBel RP, Storm DR, Chen X. Type 3 adenylyl cyclase: a key enzyme mediating the cAMP signaling in neuronal cilia. Int J Physiol Pathophysiol Pharmacol. 2016;8:95–108.
Cooper DMF. Regulation and organization of adenylyl cyclases and cAMP. Biochem J. 2003;375:517–29.
Hanoune J, Defer N. Regulation and role of adenylyl cyclase isoforms. Annu Rev Pharmacol Toxicol. 2001;41:145–74.
Pierre S, Eschenhagen T, Geisslinger G, Scholich K. Capturing adenylyl cyclases as potential drug targets. Nat Rev Drug Discov. 2009;8:321–35.
Pavan B, Biondi C, Dalpiaz A. Adenylyl cyclases as innovative therapeutic goals. Drug Discov Today. 2009;14:982–91.
Nordman S, Abulaiti A, Hilding A, Langberg EC, Humphreys K, Ostenson CG, et al. Genetic variation of the adenylyl cyclase 3 (AC3) locus and its influence on type 2 diabetes and obesity susceptibility in Swedish men. Int J Obes (Lond). 2008;32:407–12.
Wang HR, Wu M, Zhu WG, Shen J, Shi XM, Yang J et al. Evaluation of the association between the AC3 genetic polymorphisms and obesity in a chinese Han population. PLoS ONE. 2010;5:e13851.
Wu L, Shen C, Ahmed MS, Ostenson CG, Gu HF. Adenylate cyclase 3: a new target for anti-obesity drug development. Obes Rev. 2016;17:907–14.
The right form for ref. 25 is:Pitman JL, Wheeler MC, Lloyd DJ, Walker JR, Glynne RJ, Gekakis N. A gain-of-function mutation in adenylate cyclase 3 protects mice from diet-induced obesity. PLoS ONE. 2014;9:e110226.
Tong T, Shen Y, Lee HW, Yu R, Park T. Adenylyl cyclase 3 haploinsufficiency confers susceptibility to diet-induced obesity and insulin resistance in mice. Sci Rep. 2016;6:34179.
Liang Y, Li Z, Liang S, Li Y, Yang L, Lu M, et al. Hepatic adenylate cyclase 3 is upregulated by Liraglutide and subsequently plays a protective role in insulin resistance and obesity. Nutr Diabetes. 2016;6:e191.
Li Z, Liang Y, Xia N, Lai Y, Pan H, Zhou S, et al. Liraglutide reduces body weight by upregulation of adenylate cyclase 3. Nutr Diabetes. 2017;7:e265.
James WPT, Caterson ID, Coutinho W, Finer N, Van Gaal LF, Maggioni AP, et al. Effect of sibutramine on cardiovascular outcomes in overweight and obese subjects. N Engl J Med. 2010;363:905–17.
Mashiko S, Ishihara A, Iwaasa H, Moriya R, Kitazawa H, Mitobe Y, et al. Effects of a novel Y5 antagonist in obese mice: combination with food restriction or sibutramine. Obesity. 2008;16:1510–5.
Shen Y, Song SJ, Keum N, Park T. Olive leaf extract attenuates obesity in high-fat diet-fed mice by modulating the expression of molecules involved in adipogenesis and thermogenesis. Evid Based Complement Alternat Med. 2014;2014:971890.
Kym PR, Iyengar R, Souers AJ, Lynch JK, Judd AS, Gao J, et al. Discovery and characterization of aminopiperidinecoumarin melanin concentrating hormone receptor 1 antagonists. J Med Chem. 2005;48:5888–91.
Heal DJ, Gosden J, Smith SL. What is the prognosis for new centrally-acting anti-obesity drugs? Neuropharmacology. 2012;63:132–46.
Hansen HH, Hansen G, Tang-Christensen M, Larsen PJ, Axel AMD, Raben A, et al. The novel triple monoamine reuptake inhibitor tesofensine induces sustained weight loss and improves glycemic control in the diet-induced obese rat: comparison to sibutramine and rimonabant. Eur J Pharmacol. 2010;636:88–95.
Buettner R, Scholmerich J, Bollheimer LC. High-fat diets: modeling the metabolic disorders of human obesity in rodents. Obesity. 2007;15:798–808.
Forgacs AL, Kent MN, Makley MK, Mets B, DelRaso N, Jahns GL, et al. Comparative metabolomic and genomic analyses of TCDD-elicited metabolic disruption in mouse and rat liver. Toxicol Sci. 2012;125:41–55.
Freireich EJ, Gehan EA, Rall DP, Schmidt LH, Skipper HE. Quantitative comparison of toxicity of anticancer agents in mouse, rat, hamster, dog, monkey, and man. Cancer Chemother Rep. 1966;50:219–44.
Kim TH, Yoo SD, Lee HS, Lee KM, Seok SH, Kim MG, et al. In vivo absorption and disposition of alpha-cedrene, a sesquiterpene constituent of cedarwood oil, in female and male rats. Drug Metab Pharmacokinet. 2015;30:168–73.
Livera G, Xie F, Garcia MA, Jaiswal B, Chen J, Law E, et al. Inactivation of the mouse adenylyl cyclase 3 gene disrupts male fertility and spermatozoon function. Mol Endocrinol. 2005;19:1277–90.
Wong ST, Trinh K, Hacker B, Chan GCK, Lowe G, Gaggar A, et al. Disruption of the type III adenylyl cyclase gene leads to peripheral and behavioral anosmia in transgenic mice. Neuron. 2000;27:487–97.
Pluznick JL, Zou DJ, Zhang XH, Yan QS, Rodriguez-Gil DJ, Eisner C, et al. Functional expression of the olfactory signaling system in the kidney. Proc Natl Acad Sci USA. 2009;106:2059–64.
Dodge-Kafka KL, Bauman A, Mayer N, Henson E, Heredia L, Ahn J, et al. cAMP-stimulated protein phosphatase 2A activity associated with muscle A kinase-anchoring Protein (mAKAP) signaling complexes inhibits the phosphorylation and activity of the cAMP-specific phosphodiesterase PDE4D3. J Biol Chem. 2010;285:11078–86.
Taylor SS, Kim C, Cheng CY, Brown SHJ, Wu H, Kannan N. Signaling through cAMP and cAMP-dependent protein kinase: diverse strategies for drug design. BBA Proteins Proteom. 2008;1784:16–26.
Habinowski SA, Witters LA. The effects of AICAR on adipocyte differentiation of 3T3-L1 cells. Biochem Biophys Res Commun. 2001;286:852–6.
Rosen ED, Spiegelman BM. PPAR gamma: a nuclear regulator of metabolism, differentiation, and cell growth. J Biol Chem. 2001;276:37731–4.
Catania C, Binder E, Cota D. mTORC1 signaling in energy balance and metabolic disease. Int J Obes. 2011;35:751–61.
Inoki K, Zhu TQ, Guan KL. TSC2 mediates cellular energy response to control cell growth and survival. Cell. 2003;115:577–90.
McGarry JD, Brown NF. The mitochondrial carnitine palmitoyltransferase system - from concept to molecular analysis. Eur J Biochem. 1997;244:1–14.
Greenberg AS, Coleman RA, Kraemer FB, McManaman JL, Obin MS, Puri V, et al. The role of lipid droplets in metabolic disease in rodents and humans. J Clin Invest. 2011;121:2102–10.
Cao WH, Daniel KW, Robidoux J, Puigserver P, Medvedev AV, Bai X, et al. p38 mitogen-activated protein kinase is the central regulator of cyclic AMP-dependent transcription of the brown fat uncoupling protein 1 gene. Mol Cell Biol. 2004;24:3057–67.
Tong T, Ryu SE, Min Y, de March CA, Bushdid C, Golebiowski J, et al. Olfactory receptor 10J5 responding to alpha-cedrene regulates hepatic steatosis via the cAMP-PKA pathway. Sci Rep. 2017;7:9471.
Kim SH, Yoon YC, Hwang JT, Sung MJ, Kim MS, Hur HJ, et al. Tangeretin synergistically enhances odorant-induced increases in cAMP and calcium levels and CREB phosphorylation in non-neuronal 3T3-L1 cells. Appl Biol Chem. 2016;59:103–8.
Choi Y, Hur CG, Park T. Induction of olfaction and cancer-related genes in mice fed a high-fat diet as assessed through the mode-of-action by network identification analysis. PLoS ONE. 2013;8:e56610.
Acknowledgements
This work was supported by the National Research Foundation of Korea Grant (funded by the Korean Government; NRF-2016R1A2B4016189) and the grant of the Korea Health Technology R&D Project through the Korea Health Industry Development Institute (KHIDI), funded by the Ministry of Health & Welfare, Republic of Korea (grant number: HI17C2243).
Author contributions
TT and TP designed the study; TT and TP conducted the experiments; TT analyzed the data; TT, RY, and TP wrote the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Tong, T., Yu, R. & Park, T. α-Cedrene protects rodents from high-fat diet-induced adiposity via adenylyl cyclase 3. Int J Obes 43, 202–216 (2019). https://doi.org/10.1038/s41366-018-0176-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-018-0176-0