Abstract
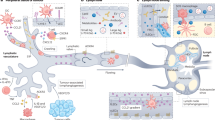
Glioblastoma are malignant highly vascularized brain tumours, which feature large oedema resulting from tumour-promoted vascular leakage. The pro-permeability factor Semaphorin3A (Sema3A) produced within glioblastoma has been linked to the loss of endothelial barrier integrity. Here, we report that extracellular vesicles (EVs) released by patient-derived glioblastoma cells disrupt the endothelial barrier. EVs expressed Sema3A at their surface, which accounted for in vitro elevation of brain endothelial permeability and in vivo vascular permeability, in both skin and brain vasculature. Blocking Sema3A or its receptor Neuropilin1 (NRP1) hampered EV-mediated permeability. In vivo models using ectopically and orthotopically xenografted mice revealed that Sema3A-containing EVs were efficiently detected in the blood stream. In keeping with this idea, sera from glioblastoma multiforme (GBM) patients also contain high levels of Sema3A carried in the EV fraction that enhanced vascular permeability, in a Sema3A/NRP1-dependent manner. Our results suggest that EV-delivered Sema3A orchestrates loss of barrier integrity in glioblastoma and may be of interest for prognostic purposes.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 50 print issues and online access
$259.00 per year
only $5.18 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Yan K, Yang K, Rich JN . The evolving landscape of glioblastoma stem cells. Curr Opin Neurol 2013; 26: 701–707.
Yuan X, Curtin J, Xiong Y, Liu G, Waschsmann-Hogiu S, Farkas DL et al. Isolation of cancer stem cells from adult glioblastoma multiforme. Oncogene 2004; 23: 9392–9400.
Galan-Moya EM, Le Guelte A, Fernandes EL, Thirant C, Dwyer J, Bidere N et al. Secreted factors from brain endothelial cells maintain glioblastoma stem-like cell expansion through the mTOR pathway. EMBO Rep 2011; 12: 470–476.
Galan-Moya EM, Treps L, Oliver L, Chneiweiss H, Vallette FM, Bidere N et al. Endothelial secreted factors suppress mitogen deprivation-induced autophagy and apoptosis in glioblastoma stem-like cells. PLoS One 2014; 9: e93505.
Calabrese C, Poppleton H, Kocak M, Hogg TL, Fuller C, Hamner B et al. A perivascular niche for brain tumor stem cells. Cancer Cell 2007; 11: 69–82.
Batchelor TT, Sorensen AG, di Tomaso E, Zhang WT, Duda DG, Cohen KS et al. AZD2171, a pan-VEGF receptor tyrosine kinase inhibitor, normalizes tumor vasculature and alleviates edema in glioblastoma patients. Cancer Cell 2007; 11: 83–95.
Chinot OL, Wick W, Mason W, Henriksson R, Saran F, Nishikawa R et al. Bevacizumab plus radiotherapy-temozolomide for newly diagnosed glioblastoma. N Engl J Med 2014; 370: 709–722.
Gilbert MR, Dignam JJ, Armstrong TS, Wefel JS, Blumenthal DT, Vogelbaum MA et al. A randomized trial of bevacizumab for newly diagnosed glioblastoma. N Engl J Med 2014; 370: 699–708.
Le Guelte A, Galan-Moya EM, Dwyer J, Treps L, Kettler G, Hebda JK et al. Semaphorin 3 A elevates endothelial cell permeability through PP2A inactivation. J Cell Sci 2012; 125: 4137–4146.
Maione F, Molla F, Meda C, Latini R, Zentilin L, Giacca M et al. Semaphorin 3 A is an endogenous angiogenesis inhibitor that blocks tumor growth and normalizes tumor vasculature in transgenic mouse models. J Clin Invest 2009; 119: 3356–3372.
Casazza A, Fu X, Johansson I, Capparuccia L, Andersson F, Giustacchini A et al. Systemic and targeted delivery of semaphorin 3 A inhibits tumor angiogenesis and progression in mouse tumor models. Arterioscler Thromb Vasc Biol 2011; 31: 741–749.
Acevedo LM, Barillas S, Weis SM, Gothert JR, Cheresh DA . Semaphorin 3 A suppresses VEGF-mediated angiogenesis yet acts as a vascular permeability factor. Blood 2008; 111: 2674–2680.
Casazza A, Laoui D, Wenes M, Rizzolio S, Bassani N, Mambretti M et al. Impeding macrophage entry into hypoxic tumor areas by Sema3 A/Nrp1 signaling blockade inhibits angiogenesis and restores antitumor immunity. Cancer Cell 2013; 24: 695–709.
Skog J, Wurdinger T, van Rijn S, Meijer DH, Gainche L, Sena-Esteves M et al. Glioblastoma microvesicles transport RNA and proteins that promote tumour growth and provide diagnostic biomarkers. Nat Cell Biol 2008; 10: 1470–1476.
Vader P, Breakefield XO, Wood MJ . Extracellular vesicles: emerging targets for cancer therapy. Trends Mol Med 2014; 20: 385–393.
Colombo M, Raposo G, Thery C . Biogenesis, secretion, and intercellular interactions of exosomes and other extracellular vesicles. Annu Rev Cell Dev Biol 2014; 30: 255–289.
Kucharzewska P, Christianson HC, Welch JE, Svensson KJ, Fredlund E, Ringner M et al. Exosomes reflect the hypoxic status of glioma cells and mediate hypoxia-dependent activation of vascular cells during tumor development. Proc Natl Acad Sci USA 2013; 110: 7312–7317.
Shao H, Chung J, Balaj L, Charest A, Bigner DD, Carter BS et al. Protein typing of circulating microvesicles allows real-time monitoring of glioblastoma therapy. Nat Med 2012; 18: 1835–1840.
Thirant C, Galan-Moya EM, Dubois LG, Pinte S, Chafey P, Broussard C et al. Differential proteomic analysis of human glioblastoma and neural stem cells reveals HDGF as a novel angiogenic secreted factor. Stem Cells 2012; 30: 845–853.
Gavard J, Gutkind JS . VEGF controls endothelial-cell permeability by promoting the beta-arrestin-dependent endocytosis of VE-cadherin. Nat Cell Biol 2006; 8: 1223–1234.
Crescitelli R, Lasser C, Szabo TG, Kittel A, Eldh M, Dianzani I et al. Distinct RNA profiles in subpopulations of extracellular vesicles: apoptotic bodies, microvesicles and exosomes. J Extracell Vesicles 2013; 2: 20677.
Olsson AK, Dimberg A, Kreuger J, Claesson-Welsh L . VEGF receptor signalling - in control of vascular function. Nat Rev Mol Cell Biol 2006; 7: 359–371.
Pan Q, Chanthery Y, Liang WC, Stawicki S, Mak J, Rathore N et al. Blocking neuropilin-1 function has an additive effect with anti-VEGF to inhibit tumor growth. Cancer Cell 2007; 11: 53–67.
Piao Y, Liang J, Holmes L, Zurita AJ, Henry V, Heymach JV et al. Glioblastoma resistance to anti-VEGF therapy is associated with myeloid cell infiltration, stem cell accumulation, and a mesenchymal phenotype. Neuro Oncol 2012; 14: 1379–1392.
Chen X, Zhang L, Zhang IY, Liang J, Wang H, Ouyang M et al. RAGE expression in tumor-associated macrophages promotes angiogenesis in glioma. Cancer Res 2014; 74: 7285–7297.
Maione F, Capano S, Regano D, Zentilin L, Giacca M, Casanovas O et al. Semaphorin 3A overcomes cancer hypoxia and metastatic dissemination induced by antiangiogenic treatment in mice. J Clin Invest 2012; 122: 1832–1848.
Vredenburgh JJ, Desjardins A, Herndon JE 2nd, Marcello J, Reardon DA, Quinn JA et al. Bevacizumab plus irinotecan in recurrent glioblastoma multiforme. J Clin Oncol 2007; 25: 4722–4729.
Friedman HS, Prados MD, Wen PY, Mikkelsen T, Schiff D, Abrey LE et al. Bevacizumab alone and in combination with irinotecan in recurrent glioblastoma. J Clin Oncol 2009; 27: 4733–4740.
Kreisl TN, Kim L, Moore K, Duic P, Royce C, Stroud I et al. Phase II trial of single-agent bevacizumab followed by bevacizumab plus irinotecan at tumor progression in recurrent glioblastoma. J Clin Oncol 2009; 27: 740–745.
Lai A, Tran A, Nghiemphu PL, Pope WB, Solis OE, Selch M et al. Phase II study of bevacizumab plus temozolomide during and after radiation therapy for patients with newly diagnosed glioblastoma multiforme. J Clin Oncol 2011; 29: 142–148.
Narayana A, Gruber D, Kunnakkat S, Golfinos JG, Parker E, Raza S et al. A clinical trial of bevacizumab, temozolomide, and radiation for newly diagnosed glioblastoma. J Neurosurg 2012; 116: 341–345.
Dwyer J, Hebda JK, Le Guelte A, Galan-Moya EM, Smith SS, Azzi S et al. Glioblastoma cell-secreted interleukin-8 induces brain endothelial cell permeability via CXCR2. PLoS One 2012; 7: e45562.
Le Guelte A, Dwyer J, Gavard J . Jumping the barrier: VE-cadherin, VEGF and other angiogenic modifiers in cancer. Biol Cell 2011; 103: 593–605.
Shao H, Chung J, Lee K, Balaj L, Min C, Carter BS et al. Chip-based analysis of exosomal mRNA mediating drug resistance in glioblastoma. Nat Commun 2015; 6: 6999.
Acknowledgements
We are thankful to present and past members of the team, especially to Héloise Leclair and Armelle Le Guelte. We are grateful to Robin Lombard (Myltenyi Biotech, Paris, France) for technical assistance with the MacsQuant cytometer. We are also grateful to PO Couraud and F Niedergang’s team (Institut Cochin, Paris, France) for helpful discussion and reagents. This research was funded by: Fondation pour la Recherche Médicale, Institut National du Cancer INCA_6508, Ligue nationale contre le cancer comité de Paris, Region Pays-de-la-Loire, Nantes Metropole. LT is supported by doctoral fellowship from Universite Paris Descartes. EMGM, EHW and SA are supported by post-doctoral fellowships from Ligue nationale contre le cancer, Canceropole Ile-de-France and Fondation ARC Association pour la Recherche sur le Cancer, respectively.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on the Oncogene website
Supplementary information
Rights and permissions
About this article
Cite this article
Treps, L., Edmond, S., Harford-Wright, E. et al. Extracellular vesicle-transported Semaphorin3A promotes vascular permeability in glioblastoma. Oncogene 35, 2615–2623 (2016). https://doi.org/10.1038/onc.2015.317
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/onc.2015.317
This article is cited by
-
IGF2BP1 regulates the cargo of extracellular vesicles and promotes neuroblastoma metastasis
Oncogene (2023)
-
Emerging role of extracellular vesicles in the pathogenesis of glioblastoma
Metabolic Brain Disease (2023)
-
Glioma extracellular vesicles for precision medicine: prognostic and theragnostic application
Discover Oncology (2022)
-
The von Willebrand factor stamps plasmatic extracellular vesicles from glioblastoma patients
Scientific Reports (2021)
-
A systematic review of extracellular vesicles as non-invasive biomarkers in glioma diagnosis, prognosis, and treatment response monitoring
Molecular Biology Reports (2021)