Abstract
The rapid restoration of coronary flow to the jeopardized myocardium has become an essential part of therapy after acute myocardial infarction. Despite an open infarct-related artery, breakdown of or obstruction to coronary microvasculature can markedly reduce blood flow to the infarct zone. This effect is known as the no-reflow phenomenon. Advances in imaging modalities have improved visualization of no reflow, showing its frequency to be higher than was estimated by clinical judgment alone. This phenomenon is important because it correlates with infarct size and provides useful prognostic information. No reflow is associated with reduced left ventricular ejection fraction, left ventricular remodeling, and poor clinical outcomes, placing patients with this effect in a high-risk group among reperfused patients. The focus of reperfusion therapy is shifting towards improved myocardial perfusion, which could promote functional recovery of viable muscle, reduce infarct expansion, and increase the delivery of blood-borne components, thereby accelerating the healing process. Various pharmacologic interventions and catheter-based devices to retrieve embolic materials have been proposed. Further studies to improve understanding of the pathophysiology of microvascular dysfunction will, however, help in the further development of preventive and therapeutic strategies. In this article, I discuss in depth the data available on the no-reflow phenomenon.
Key Points
-
Successful restoration of epicardial coronary artery patency with reperfusion therapy after acute myocardial infarction does not necessarily translate into improved tissue perfusion, resulting in the no-reflow phenomenon
-
As well as correlating closely with myocardial infarction size, the no-reflow phenomenon can provide valuable prognostic indications
-
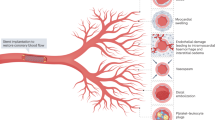
At least two mechanisms lead to microvascular obstruction: capillary occlusion and microemboli to coronary resistance vessels
-
Contrast perfusion defects on myocardial contrast echocardiography, indicating no reflow, are often associated with sluggish coronary flow and sustained ST-segment elevation
-
Reduction of embolic particle concentration with antiplatelet therapy and removal of thrombus and plaque burden with catheter-based interventions can improve coronary blood flow
-
Several pharmacologic interventions have been tested to reduce the no-reflow phenomenon and some of them are available for clinical use
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Ito H et al. (1996) Clinical implications of the 'no reflow' phenomenon. A predictor of complications and left ventricular remodeling in reperfused anterior wall myocardial infarction. Circulation 93: 223–228
Kloner RA et al. (1974) The “no-reflow” phenomenon after temporary coronary occlusion in the dog. J Clin Invest 54: 1496–1508
Kloner RA et al. (1980) Ultrastructural evidence of microvascular damage and myocardial cell injury after coronary artery occlusion: which comes first? Circulation 62: 945–952
Komamura K et al. (1994) Progressive decreases in coronary vein flow during reperfusion in acute myocardial infarction: clinical documentation of the no reflow phenomenon after successful thrombolysis. J Am Coll Cardiol 24: 370–377
Manciet LH et al. (1994) Microvascular compression during myocardial ischemia: mechanistic basis for no-reflow phenomenon. Am J Physiol 266: H1541–H1550
Topol EJ et al. (2000) Recognition of the importance of embolization in atherosclerotic vascular disease. Circulation 101: 570–580
Fuster V et al. (1992) The pathogenesis of coronary artery disease and the acute coronary syndromes (1). N Engl J Med 326: 242–250
Iwakura K et al. (2001) Predictive factors for development of the no-reflow phenomenon in patients with reperfused anterior wall acute myocardial infarction. J Am Coll Cardiol 38: 472–477
Coggins MP et al. (2001) Noninvasive prediction of ultimate infarct size at the time of acute coronary occlusion based on the extent and magnitude of collateral-derived myocardial blood flow. Circulation 104: 2471–2477
Iwakura K et al. (2003) Association between hyperglycemia and the no-reflow phenomenon in patients with acute myocardial infarction. J Am Coll Cardiol 41: 1–7
Malmberg K et al. (1999) Glycometabolic state at admission: important risk marker of mortality in conventionally treated patients with diabetes mellitus and acute myocardial infarction: long-term results from the Diabetes and Insulin-Glucose Infusion in Acute Myocardial Infarction (DIGAMI) study. Circulation 99: 2626–2632
Tanaka A et al. (2002) No-reflow phenomenon and lesion morphology in patients with acute myocardial infarction. Circulation 105: 2148–2152
Kotani J et al. (2002) Plaque gruel of atheromatous coronary lesion may contribute to the no-reflow phenomenon in patients with acute coronary syndrome. Circulation 106: 1672–1677
Hori M et al. (1986) Role of adenosine in hyperemic response of coronary blood flow in microembolization. Am J Physiol 250: H509–H518
Okamura A et al. (2005) Detection of embolic particles with the Doppler guide wire during coronary intervention in patients with acute myocardial infarction: efficacy of distal protection device. J Am Coll Cardiol 45: 212–215
Ito H et al. (1992) Lack of myocardial perfusion immediately after successful thrombolysis. A predictor of poor recovery of left ventricular function in anterior myocardial infarction. Circulation 85: 1699–1705
Villanueva FS et al. (1993) Characterization of spatial patterns of flow within the reperfused myocardium by myocardial contrast echocardiography. Implication in determining extent of myocardial salvage. Circulation 88: 2596–2606
Yano A et al. (2004) Myocardial contrast echocardiography with a new calibration method can estimate myocardial viability in patients with myocardial infarction. J Am Coll Cardiol 43: 1799–1806
Zijlstra F et al. (1993) A comparison of immediate coronary angioplasty with intravenous streptokinase in acute myocardial infarction. N Engl J Med 328: 680–684
Simes RJ et al. (1995) Link between the angiographic substudy and mortality outcomes in a large randomized trial of myocardial reperfusion. Importance of early and complete infarct artery reperfusion. GUSTO-I Investigators. Circulation 91: 1923–1928
Ito H et al. (1996) Myocardial perfusion patterns related to thrombolysis in myocardial infarction perfusion grades after coronary angioplasty in patients with acute anterior wall myocardial infarction. Circulation 93:1993–1999
Grines CL et al. (1999) Coronary angioplasty with or without stent implantation for acute myocardial infarction. Stent Primary Angioplasty in Myocardial Infarction Study Group. N Engl J Med 341: 1949–1956
Gibson CM et al. (2000) Relationship of TIMI myocardial perfusion grade to mortality after administration of thrombolytic drugs. Circulation 101: 125–130
Iwakura K et al. (1996) Alternation in the coronary blood flow velocity pattern in patients with no reflow and reperfused acute myocardial infarction. Circulation 94: 1269–1275
Akasaka T et al. (2000) Relation of phasic coronary flow velocity characteristics with TIMI perfusion grade and myocardial recovery after primary percutaneous transluminal coronary angioplasty and rescue stenting. Circulation 101: 2361–2367
Yamamoto K et al. (2002) Two different coronary blood flow velocity patterns in thrombolysis in myocardial infarction flow grade 2 in acute myocardial infarction: insight into mechanisms of microvascular dysfunction. J Am Coll Cardiol 40: 1755–1760
Wehrens X et al. (2000) A comparison of electrocardiographic changes during reperfusion of acute myocardial infarction by thrombolysis or percutaneous transluminal coronary angioplasty. Am Heart J 139: 430–436
Claeys MJ et al. (1999) Determinants and prognostic implications of persistent ST-segment elevation after primary angioplasty for acute myocardial infarction: importance of microvascular reperfusion injury on clinical outcome. Circulation 99: 1972–1977
Wu KC et al. (1998) Prognostic significance of microvascular obstruction by magnetic resonance imaging in patients with acute myocardial infarction. Circulation 97: 765–772
Taylor AJ et al. (2004) Detection of acutely impaired microvascular reperfusion after infarct angioplasty with magnetic resonance imaging. Circulation 109: 2080–2085
Ito H et al (1996) Clinical implications of the 'no reflow' phenomenon. A predictor of complications and left ventricular remodeling in reperfused anterior wall myocardial infarction. Circulation 93: 223–228
Morishima I et al. (2000) Angiographic no-reflow phenomenon as a predictor of adverse long-term outcome in patients treated with percutaneous transluminal coronary angioplasty for first acute myocardial infarction. J Am Coll Cardiol 36: 1202–1209
Kocher AA (2001) Neovascularization of ischemic myocardium by human bone marrow-derived angioblasts prevents cardiomyocyte apoptosis, reduces remodeling and improves cardiac function. Nat Med 7: 430–436
Kunichika H et al. (2004) Effects of glycoprotein IIb/IIIa inhibition on microvascular flow after coronary reperfusion. A quantitative myocardial contrast echocardiography study. J Am Coll Cardiol 43: 276–283
Montalescot G et al. (2001) Platelet glycoprotein IIb/IIIa inhibition with coronary stenting for acute myocardial infarction. N Engl J Med 344: 1895–1903
Stone GW et al. (2005) Distal microcirculatory protection during percutaneous coronary intervention in acute ST-segment elevation myocardial infarction: a randomized controlled trial. JAMA 293: 1063–1072
Gick M et al. (2005) Randomized evaluation of the effects of filter-based distal protection on myocardial perfusion and infarct size after primary percutaneous catheter intervention in myocardial infarction with and without ST-segment elevation. Circulation 112: 1462–1469
Mizote I et al. (2005) Distal protection improved reperfusion and reduced left ventricular dysfunction in patients with acute myocardial infarction who had angioscopically defined ruptured plaque. Circulation 112: 1001–1007
Makaryus AN et al. (2006) Efficacy of rheolytic thrombectomy in early versus late myocardial infarction. J Interv Cardiol 19: 135–140
Ali A (2004) Rheolytic thrombectomy in patients with acute MI did not result in a reduction in myocardial infarct size. Presented at Transcatheter Cardiovascular Therapeutics: 2004 September 27 to October 1; Washington, DC
Tsang A et al. (2004) Postconditioning: a form of “modified reperfusion” protects the myocardium by activating the phosphatidylinositol 3-kinase-Akt pathway. Circ Res 95: 230–232
Staat P et al. (2005) Postconditioning the human heart. Circulation 112: 2143–2148
Marzilli M et al. (2000) Beneficial effects of intracoronary adenosine as an adjunct to primary angioplasty in acute myocardial infarction. Circulation 101: 2154–2159
Ross AM et al. (2005) A randomized, double-blinded, placebo-controlled multicenter trial of adenosine as an adjunct to reperfusion in the treatment of acute myocardial infarction (AMISTAD-II). J Am Coll Cardiol 45: 1775–1780
Ito H et al. (1999) Intravenous nicorandil can preserve microvascular integrity and myocardial viability in patients with reperfused anterior wall myocardial infarction. J Am Coll Cardiol 33: 654–660
Ishii H et al. (2005) Impact of a single intravenous administration of nicorandil before reperfusion in patients with ST-segment-elevation myocardial infarction. Circulation 112: 1284–1288
Taniyama Y (1997) Beneficial effect of intracoronary verapamil on microvascular and myocardial salvage in patients with acute myocardial infarction. J Am Coll Cardiol 30: 1193–1199
Umemura S (2006) The effect of verapamil on the restoration of myocardial perfusion and functional recovery in patients with angiographic no-reflow after primary percutaneous coronary intervention. Nucl Med Commun 27: 247–254
Pasceri V (2005) Effects of the nitric oxide donor nitroprusside on no-reflow phenomenon during coronary interventions for acute myocardial infarction. Am J Cardiol 95: 1358–1361
Theroux P (2000) Myocardial cell protection: a challenging time for action and a challenging time for clinical research. Circulation 101: 2874–2876
Theroux P et al. (2000) Inhibition of the sodium-hydrogen exchanger with cariporide to prevent myocardial infarction in high-risk ischemic situations. Main results of the GUARDIAN trial. Guard during ischemia against necrosis (GUARDIAN) Investigators. Circulation 102: 3032–3038
Zeymer U et al. (2001) The Na+/H+ exchange inhibitor eniporide as an adjunct to early reperfusion therapy for acute myocardial infarction. Results of the evaluation of the safety and cardioprotective effects of eniporide in acute myocardial infarction (ESCAMI) trial. J Am Coll Cardiol 38: 1644–1650
Cai Z and Semenza GL (2004) Phosphatidylinositol-3-kinase signaling is required for erythropoietin-mediated acute protection against myocardial ischemia/reperfusion injury. Circulation 109: 2050–2053
Acknowledgements
I thank Dr S Kaul, Oregon Health & Science University, Portland, OR, USA, for valuable discussion and suggestions.
Author information
Authors and Affiliations
Ethics declarations
Competing interests
The author declares no competing financial interests.
Rights and permissions
About this article
Cite this article
Ito, H. No-reflow phenomenon and prognosis in patients with acute myocardial infarction. Nat Rev Cardiol 3, 499–506 (2006). https://doi.org/10.1038/ncpcardio0632
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/ncpcardio0632
This article is cited by
-
Efficacy and safety of intracoronary pro-urokinase combined with low-pressure balloon pre-dilatation during percutaneous coronary intervention in patients with anterior ST-segment elevation myocardial infarction
Journal of Cardiothoracic Surgery (2024)
-
Macrophages in cardiac remodelling after myocardial infarction
Nature Reviews Cardiology (2023)
-
Microvascular bioengineering: a focus on pericytes
Journal of Biological Engineering (2019)
-
Intravital imaging with two-photon microscopy reveals cellular dynamics in the ischeamia-reperfused rat heart
Scientific Reports (2018)
-
Nanoparticle-Mediated Delivery of Irbesartan Induces Cardioprotection from Myocardial Ischemia-Reperfusion Injury by Antagonizing Monocyte-Mediated Inflammation
Scientific Reports (2016)