Abstract
In some organs, adult stem cells are uniquely poised to serve as cancer cells of origin. It is unclear, however, whether tumorigenesis is influenced by the activation state of the adult stem cell. Hair follicle stem cells (HFSCs) act as cancer cells of origin for cutaneous squamous cell carcinoma and undergo defined cycles of quiescence and activation. The data presented here show that HFSCs are unable to initiate tumours during the quiescent phase of the hair cycle, indicating that the mechanisms that keep HFSCs dormant are dominant over the gain of oncogenes (such as Ras) or the loss of tumour suppressors (such as p53). Furthermore, Pten activity is necessary for quiescence-based tumour suppression, as its deletion alleviates tumour suppression without affecting proliferation. These data demonstrate that stem cell quiescence is a form of tumour suppression in HFSCs, and that Pten plays a role in maintaining quiescence in the presence of tumorigenic stimuli.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Accession codes
References
Lowry, W. E. & Richter, L. Signaling in adult stem cells. Front. Biosci. 12, 3911–3927 (2007).
Fuchs, E. The tortoise and the hair: slow-cycling cells in the stem cell race. Cell 137, 811–819 (2009).
Lapouge, G. et al. Identifying the cellular origin of squamous skin tumors. Proc. Natl Acad. Sci. USA 108, 7431–7436 (2011).
White, A. C. et al. Defining the origins of Ras/p53-mediated squamous cell carcinoma. Proc. Natl Acad. Sci. USA 108, 7425–7430 (2011).
Barker, N. et al. Crypt stem cells as the cells-of-origin of intestinal cancer. Nature 457, 608–611 (2009).
Visvader, J. E. Cells of origin in cancer. Nature 469, 314–322 (2011).
Paus, R., Muller-Rover, S. & Botchkarev, V. A. Chronobiology of the hair follicle: hunting the ‘hair cycle clock’. J. Invest. Dermatol. Symp. Proc. 4, 338–345 (1999).
Greco, V. et al. A two-step mechanism for stem cell activation during hair regeneration. Cell Stem Cell 4, 155–169 (2009).
Trempus, C. S. et al. CD34 expression by hair follicle stem cells is required for skin tumor development in mice. Cancer Res. 67, 4173–4181 (2007).
Finch, J. S., Albino, H. E. & Bowden, G. T. Quantitation of early clonal expansion of two mutant 61st codon c-Ha-ras alleles in DMBA/TPA treated mouse skin by nested PCR/RFLP. Carcinogenesis 17, 2551–2557 (1996).
Andreasen, E. & Borum, K. The influence of the mouse hair cycle on 9, 10-dimethyl-1, 2-benzanthracene-induced skin tumors. Acta Pathol. Microbiol. Scand. Suppl. 39, 76–77 (1956).
Klinken-Rasmussen, L. Effect of croton oil applied to mouse skin originally painted with suboptimal doses of carcinogen during the growth and resting phases of the hair follicles. Acta Pathol. Microbiol. Scand. Suppl. 39, 78–79 (1956).
Miller, S. J. et al. Mouse skin is particularly susceptible to tumor initiation during early anagen of the hair cycle: possible involvement of hair follicle stem cells. J. Invest. Dermatol. 101, 591–594 (1993).
Lavker, R. M. et al. Hair follicle stem cells: their location, role in hair cycle, and involvement in skin tumor formation. J. Invest. Dermatol. 101, 16S–26S (1993).
Grachtchouk, M. et al. Basal cell carcinomas in mice arise from hair follicle stem cells and multiple epithelial progenitor populations. J. Clin. Invest. 121, 1768–1781 (2011).
Mancuso, M. et al. Hair cycle-dependent basal cell carcinoma tumorigenesis in Ptc1neo67/ + mice exposed to radiation. Cancer Res. 66, 6606–6614 (2006).
Li, S. et al. A keratin 15 containing stem cell population from the hair follicle contributes to squamous papilloma development in the mouse. Mol. Carcinog. 52, 751–759 (2012).
Groszer, M. et al. Negative regulation of neural stem/progenitor cell proliferation by the Pten tumor suppressor gene in vivo. Science 294, 2186–2189 (2001).
Jaks, V. et al. Lgr5 marks cycling, yet long-lived, hair follicle stem cells. Nature Genet. 40, 1291–1299 (2008).
Snippert, H. J. et al. Lgr6 marks stem cells in the hair follicle that generate all cell lineages of the skin. Science 327, 1385–1389 (2010).
Zhang, J. et al. BMP signaling inhibits hair follicle anagen induction by restricting epithelial stem/progenitor cell activation and expansion. Stem Cells 24, 2826–2839 (2006).
Gu, T. et al. CREB is a novel nuclear target of PTEN phosphatase. Cancer Res. 71, 2821–2825 (2011).
Vivanco, I. et al. Identification of the JNK signaling pathway as a functional target of the tumor suppressor PTEN. Cancer Cell 11, 555–569 (2007).
Tran, L. M. et al. Determining PTEN functional status by network component deduced transcription factor activities. PLoS ONE 7, e31053 (2012).
Rozenberg, J. et al. Inhibition of CREB function in mouse epidermis reduces papilloma formation. Mol. Cancer Res. 7, 654–664 (2009).
Ji, J. et al. Elevated coding mutation rate during the reprogramming of human somatic cells into induced pluripotent stem cells. Stem Cells 30, 435–440 (2012).
Plikus, M. V. New activators and inhibitors in the hair cycle clock: targeting stem cells’ state of competence. J. Invest. Dermatol. 132, 1321–1324 (2012).
Ahmed, M. I., Mardaryev, A. N., Lewis, C. J., Sharov, A. A. & Botchkareva, N. V. MicroRNA-21 is an important downstream component of BMP signalling in epidermal keratinocytes. J. Cell Sci. 124, 3399–3404 (2011).
Wang, T. et al. TGF-beta-induced miR-21 negatively regulates the antiproliferative activity but has no effect on EMT of TGF-beta in HaCaT cells. Int. J. Biochem. Cell Biol. 44, 366–376 (2012).
Zhong, X., Chung, A. C., Chen, H. Y., Meng, X. M. & Lan, H. Y. Smad3-mediated upregulation of miR-21 promotes renal fibrosis. J. Am. Soc. Nephrol. 22, 1668–1681 (2011).
Yao, Q. et al. Micro-RNA-21 regulates TGF-beta-induced myofibroblast differentiation by targeting PDCD4 in tumor-stroma interaction. Int. J. Cancer 128, 1783–1792 (2011).
Kim, Y. J., Hwang, S. J., Bae, Y. C. & Jung, J. S. MiR-21 regulates adipogenic differentiation through the modulation of TGF-beta signaling in mesenchymal stem cells derived from human adipose tissue. Stem Cells 27, 3093–3102 (2009).
Ma, X. et al. Loss of the miR-21 allele elevates the expression of its target genes and reduces tumorigenesis. Proc. Natl Acad. Sci. USA 108, 10144–10149 (2011).
Zhu, H. et al. MicroRNA expression abnormalities in limited cutaneous scleroderma and diffuse cutaneous scleroderma. J. Clin. Immunol. 32, 514–522 (2012).
Darido, C. et al. Targeting of the tumor suppressor GRHL3 by a miR-21-dependent proto-oncogenic network results in PTEN loss and tumorigenesis. Cancer Cell 20, 635–648 (2011).
Narducci, M. G. et al. MicroRNA profiling reveals that miR-21, miR486 and miR-214 are upregulated and involved in cell survival in Sezary syndrome. Cell Death Dis. 2, e151 (2011).
Oshimori, N. & Fuchs, E. Paracrine TGF-beta signaling counterbalances BMP-mediated repression in hair follicle stem cell activation. Cell Stem Cell 10, 63–75 (2012).
Sugawara, K., Schneider, M. R., Dahlhoff, M., Kloepper, J. E. & Paus, R. Cutaneous consequences of inhibiting EGF receptor signaling in vivo: normal hair follicle development, but retarded hair cycle induction and inhibition of adipocyte growth in Egfr(Wa5) mice. J. Dermatol. Sci. 57, 155–161 (2010).
Lowry, W. E. et al. Defining the impact of beta-catenin/Tcf transactivation on epithelial stem cells. Genes Dev. 19, 1596–1611 (2005).
Kimura-Ueki, M. et al. Hair cycle resting phase is regulated by cyclic epithelial FGF18 signaling. J. Invest. Dermatol. 132, 1338–1345 (2012).
Kobielak, K., Stokes, N., de la Cruz, J., Polak, L. & Fuchs, E. Loss of a quiescent niche but not follicle stem cells in the absence of bone morphogenetic protein signaling. Proc. Natl Acad. Sci. USA 104, 10063–10068 (2007).
Brownstein, M. H., Mehregan, A. H. & Bilowski, J. B. Trichilemmomas in Cowden’s disease. Jama 238, 26 (1977).
Lazarov, M. et al. CDK4 coexpression with Ras generates malignant human epidermal tumorigenesis. Nat. Med. 8, 1105–1114 (2002).
Agrawal, N. et al. Exome sequencing of head and neck squamous cell carcinoma reveals inactivating mutations in NOTCH1. Science 333, 1154–1157 (2011).
Stransky, N. et al. The mutational landscape of head and neck squamous cell carcinoma. Science 333, 1157–1160 (2011).
Kubo, Y., Urano, Y., Hida, Y. & Arase, S. Lack of somatic mutation in the PTENgene in squamous cell carcinomas of human skin. J. Dermatol. Sci. 19, 199–201 (1999).
Al-Zaid, T. et al. Trichilemmomas show loss of PTEN in Cowden syndrome but only rarely in sporadic tumors. J. Cutan. Pathol. 39, 493–499 (2012).
Kurose, K., Zhou, X. P., Araki, T. & Eng, C. Biallelic inactivating mutations and an occult germline mutation of PTEN in primary cervical carcinomas. Genes Chromosom. Cancer 29, 166–172 (2000).
Tuveson, D. A. et al. Endogenous oncogenic K-ras(G12D) stimulates proliferationand widespread neoplastic and developmental defects. Cancer Cell 5, 375–387 (2004).
Jonkers, J. et al. Synergistic tumor suppressor activity of BRCA2 and p53 in a conditional mouse model for breast cancer. Nature Gen. 29, 418–425 (2001).
Jackson, E. L. et al. Analysis of lung tumor initiation and progression using conditional expression of oncogenic K-ras. Genes Dev. 15, 3243–3248 (2001).
Horenstein, M. G. & Bacheler, C. J. Follicular density and ratios in scarring and nonscarring alopecia. Am. J. Dermatopathol. 35, 818–826 (2013).
Chin, M. H., Pellegrini, M., Plath, K. & Lowry, W. E. Molecular analyses of human induced pluripotent stem cells and embryonic stem cells. Cell Stem Cell 7, 263–269 (2010).
Wang, D. et al. Quantitative functions of Argonaute proteins in mammalian development. Genes Dev. 26, 693–704 (2012).
Acknowledgements
We would like to acknowledge the technical support of W. Kim; the management of the animal facilities (DLAM); the FACS core (EEBSCRC); the TPCL (Department of Pathology, UCLA); the gene expression core (Department of Pathology, UCLA) and X. Gaeta for a critical reading of the manuscript. This work was supported by grants from CIRM (TG2-01169), CRCC, The JCCF, and NIH (UCLA Tumour Biology Program, Ruth L. Kirschstein Institutional National Research Service Award # T32 CA009056, UCLA; and 5R01AR057409-03). WEL holds the Maria Rowena Ross Term Chair in Cell Biology.
Author information
Authors and Affiliations
Contributions
Technical support: J.H., A.L. and S.G. Experimentation: A.C.W., J.K.K., C.Y.D., K.V.T., Z.Z. and M.G. Experimental design: A.C.W., R.Y., P.S. and W.E.L. Manuscript preparation: A.C.W. and W.E.L. Financial support: W.E.L.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Integrated supplementary information
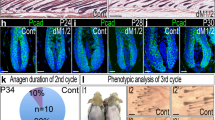
Supplementary Figure 1 (a) K15-CrePR;KrasG12D HFSCs demonstrate hyperplasia when treated with mifepristone during telogen to anagen transition for three days.
B) Consistent with a lack of phenotype, K15-CrePR;KrasG12D telogen bulges do not exhibit a change in proliferation, as demonstrated by Ki67 staining. C) Expression of KrasG12D during full anagen does not result in hyperplasia. Instead anagen follicles regress back to telogen two weeks post treatment. D) Proliferation is not evident in HFSCs when treated during full anagen, as detected by a lack of Ki67 staining, in either control or KrasG12D expressing settings. E) Pten antibody staining shows low expression in the HFSCs during telogen and the interfollicular epidermis in control tissue. Pten ablation is confirmed by lack of staining in hyperplastic structures formed from induced K15-CrePR;KrasG12D;Ptenff bulges. Some staining is apparent in the dermal sheath cells, directly adjacent to the basal cells of hyperplastic structures. F) K15-CrePR;KrasG12D;Ptenwf hair follicles show no phenotype apart from sebaceous gland hyperplasia, demonstrating that deletion of one Pten allele is insufficient for alleviation of stem cell quiescence based tumor suppression. G) Pten-only deletion does not induce a change in proliferation in the bulge stem cell population. H) Pten expression shows upregulation in the descendants of the hair follicle HFSCs during telogen to anagen transition. The dermal papilla shows high expression as well. I) In contrast to (H), descendants of the HFSCs do not express Pten during telogen to anagen in K15-CrePR;Ptenff skin, confirming Pten knockout. J) Akt is expressed in telogen bulges in control tissues, demonstrating that Akt activity (Fig. 3a) in K15-CrePR;KrasG12D;Ptenff results from phosphorylation rather than a change in protein expression level. Panels B, C, D, E, F, G, and J shown at 20X. A, H, I shown at 40X. Scale bars represent 100μm.
Supplementary Figure 2 Characterization of signaling pathways in telogen K15-CrePR;KrasG12D and K15-CrePR;Ptenff bulges.
A-C) The Akt, Creb and c-Jun pathways are not activated by either KrasG12D or lack of Pten alone during telogen. D) The hyperplasias maintain basal epithelial marker Krt14 (D) and hyperproliferative epidermal marker Krt6 (E). F) Sox9, a marker for hair follicle stem cells, is found throughout hyperplastic structures. A-C shown at 20X, D-F shown at 10X. Scale bars represent 100μm.
Supplementary Figure 3 miRNA analysis on YFP+ K15-CrePR;KrasG12D;Ptenff;LSLYFP cells.
A) Table of miRNAs induced in K15-CrePR;KrasG12D;Ptenff hyperplasias as compared to telogen controls. B) Table of miRNAs shown to be downregulated in K15-CrePR;KrasG12D;Ptenff cells.
Supplementary Figure 4 Signaling pathways and transcription factor activity in K15-CrePR;KrasG12D and K15-CrePR;Ptenff HFSCs in telogen.
p-Smad2 (A), p-Egfr (B), Fgf18 (C) and p-Smad1/5/8 (D) do not show a change in expression pattern in KrasG12D-only telogen follicles, or Pten-only deletion follicles. E) β-catenin, which is localized to the nucleus of hair germ cells during the initiation of a hair cycle (asterisk), is not found in the nucleus in emerging and mature K15-CrePR;KrasG12D;Ptenff hyperplasias. F) At the tumor invasive front arising from K15-CrePR;KrasG12D;p53ff;Ptenff telogen HFSCs, some cells express both epithelial specific Krt5 and mesenchymal specific Vimentin (yellow). Panels A-E are shown at 20X, panel F is at 60X. Scale bars represent 100μm.
Supplementary information
Supplementary Information
Supplementary Information (PDF 719 kb)
Rights and permissions
About this article
Cite this article
White, A., Khuu, J., Dang, C. et al. Stem cell quiescence acts as a tumour suppressor in squamous tumours. Nat Cell Biol 16, 99–107 (2014). https://doi.org/10.1038/ncb2889
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ncb2889
This article is cited by
-
The journey from melanocytes to melanoma
Nature Reviews Cancer (2023)
-
Loss of Epidermal Homeostasis Underlies the Development of Squamous Cell Carcinoma
Stem Cell Reviews and Reports (2023)
-
A stress-induced miR-31–CLOCK–ERK pathway is a key driver and therapeutic target for skin aging
Nature Aging (2021)
-
New insights into the functions of Cox-2 in skin and esophageal malignancies
Experimental & Molecular Medicine (2020)
-
Increased lactate dehydrogenase activity is dispensable in squamous carcinoma cells of origin
Nature Communications (2019)