Abstract
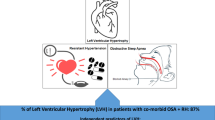
Uncontrolled blood pressure (BP) is linked to increased risk of obstructive sleep apnea (OSA). However, few studies have assessed the impact of this relationship among blacks with metabolic syndrome (MetS). Data for this study were collected from 1035 blacks (mean age=62±13 years) enrolled in the Metabolic Syndrome Outcome study. Patients with a score ⩾6 on the Apnea Risk Evaluation System were considered at risk for OSA. Of the sample, 77.1% were low-to-high OSA risk and 92.3% were hypertensive, of which 16.8% had uncontrolled BP levels. Analysis also showed that 60.4% were diabetic, 8.9% had a stroke history, 74.3% had dyslipidemia, 69.8% were obese and 30.9% had a history of heart disease. Logistic regression analyses were employed to investigate associations between uncontrolled BP and OSA risk, while adjusting for known covariates. Findings showed that uncontrolled BP independently increased the odds of OSA risk twofold (odds ratio=2.02, 95% confidence interval=1.18–3.48, P<0.05). In conclusion, our findings show that uncontrolled BP was associated with a twofold greater risk of OSA among blacks, suggesting that those with MetS and who have uncontrolled BP should be screened for the presence of OSA.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Grundy SM, Brewer HB Jr, Cleeman JI, Smith SC Jr, Lenfant C . Definition of metabolic syndrome: Report of the National Heart, Lung and Blood Institute/American Heart Association Conference on scientific issues related to definition. Circulation 2004; 109: 433–438.
Reaven GM . Pathophysiology of insulin resistance in human disease. Physiol Rev 1995; 75: 473–486.
Meis SB, Schuster D, Gaillard T, Osei K . Metabolic Syndrome in nondiabetic, obese, first-degree relatives of African American patients with type 2 diabetes: African American triglycerides-HDL-C and insulin resistance paradox. Ethn Dis 2006; 16: 830–836.
DeFronzo RA, Ferrannini E . Insulin resistance. A multifaceted syndrome responsible for NIDDM, obesity, hypertension, dyslipidemia and atherosclerotic cardiovascular disease. Diabetes Care 1991; 14: 173–194.
Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults. Executive Summary of The Third Report of The National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, And Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III). JAMA 2001; 285: 2486–2497.
Olafiranye O, Akinboboye O, Mitchell JE, Ogedegbe G, Jean-Louis G . Obstructive sleep apnea and cardiovascular disease in blacks: a call to action from the Association of Black Cardiologists. Am Heart J 2013; 165: 469–476.
Jean-Louis G, Zizi F, Brown DB, Ogedegbe G, Borer JS, McFarlane SI . Obstructive sleep apnea and cardiovascular disease: evidence and underlying mechanisms. Minerva Pneumol 2009; 48: 277–293.
Relchmuth KJ, Austin D, Skatrud JB, Young T . Association of sleep apnea and Type II Diabetes: a population-based study. Am J Respir Crit Care Med 2005; 172: 1590–1595.
Calvin AD, Albuquerque FN, Lopez-Jimenez F, Somer VK . Obstructive sleep apnea, inflammation and metabolic syndrome. Metab Syndr Relat Disord 2009; 7: 271–277.
Lettieri CJ, Eliasson AH, Greenburg DL . Persistence of obstructive sleep apnea after surgical weight loss. J Clin Sleep Med 2008; 4: 333–338.
Palmer LJ, Buxbaum SG, Larkin E, Patel SR, Elston C, Tishler PV et al. A whole-genome scan for obstructive sleep apnea and obesity. Am J Hum Genet 2003; 72: 340–350.
Ronksley PE, Hemmelgarn BR, Heitman SJ, Hanly PJ, Faris PD, Quan H et al. Obstructive sleep apnea is associated with diabetes in sleepy subjects. Thorax 2009; 64: 834–839.
Barcelo A, Barbe F, De la Pena M, Martinez P, Soriano JB, Pierola J et al. Insulin resistance and daytime sleepiness in patients with sleep apnea. Thorax 2008; 63: 946–995.
Demede M, Pandey A, Zizi F, Bachmann R, Donat M, McFarlane SI et al. Resistant hypertension and obstructive sleep apnea in the primary-care setting. Int J Hypertens 2011; 20: 1–5.
Levendowski DJ, Morgan T, Montague J, Melzer V, Berka C, Westbrook PR . Prevalence of probable obstructive sleep apnea risk and severity in a population of dental patients. Sleep Breath 2008; 12: 303–309.
Levendowski DJ, Olmstead EM, Popovich D, Carper D, Berka C, Westbrook PR . Assessment of obstructive sleep apnea risk and severity in truck drivers: validation of a screening questionnaire. Sleep Diagn Ther 2007; 2: 20–26.
Calhoun DA, Jones D, Textor S, Goff DC, Murphy TP, Toto RD et al. Resistant hypertension: diagnosis, evaluation, and treatment a scientific statement from the American Heart Association Professional Education Committee of the Council for High Blood Pressure Research. Circulation 2008; 51: 1403–1419.
Persell SD . Prevalence of resistant hypertension in the United States, 2003-2008. Hypertension 2011; 57: 1076–1080.
de la Sierra A, Segura J, Banegas JR, Gorostidi M, de la Cruz JJ, Armario P et al. Clinical features of 8295 patients with resistant hypertension classified on the basis of ambulatory blood pressure monitoring. Hypertension 2011; 57: 898–902.
Noss A. Household Income: 2012. American Community Survey Briefs, 2013; 1–2. Table H-9 Race of Head of Household by Median and Mean Income, US Census Bureau. U.S. Department of Commerce: Economics and Statistics Administration. (https://www.census.gov/prod/2013pubs/acsbr12-02.pdf).
Parish JM, Adam T, Facchiano L . Relationship of metabolic syndrome and obstructive sleep apnea. J Clin Sleep Med 2007; 3: 467–472.
Drager LF, Togerio SM, Polotsky VY, Lorenzi-Filho G . Obstructive sleep apnea: a cardiometabolic risk in obesity and the metabolic syndrome. J Am Coll Cardiol 2013; 62: 569–576.
Walia HK, Li H, Rueschman M, Bhatt DL, Patel SR, Quan SF et al. Association of severe obstructive sleep apnea and elevated blood pressure despite antihypertensive medication use. J Clin Sleep Med 2014; 10: 835–843.
Logan AG, Perlikowski SM, Mente A . High prevalence of obstructive sleep apnea in drug resistant hypertension. J Hypertens 2001; 19: 2271–2277.
Sumner AE . Ethnic differences in triglyceride levels and high-density lipoprotein lead to underdiagnosis of the metabolic syndrome in black children and adults. J Pediatr 2009; 155: S7–e7.
Pedrosa RP, Drager LF, Gonzaga CC, Sousa MG, de Paula LK, Amaro AC et al. Obstructive sleep apnea: the most common secondary cause of hypertension associated with resistant hypertension. Hypertension 2011; 58: 811–817.
Logan AG, Tkacova R, Pelikowski SM, Tisle A, Floras JS, Bradley TD . Refractory hypertension and sleep apnea: effects of CPAP on blood pressure and baroreflex. Eur Respir J 2003; 21: 241–247.
Davies RJO, Stradling JR . The relationship between neck circumference, radiographic pharyngeal anatomy, and the obstructive sleep apnea syndrome. Eur Respir J 1990; 3: 509–514.
Pillar G, Shehadeh N . Abdominal fat and sleep apnea: the chicken or the egg? Diabetes Care 2008; 31: 303–309.
Kostolglou-Athanassiou I, Athanassiou P . Metabolic syndrome and sleep apnea. Hippokrata 2008; 12: 81–86.
Schwartz AR, Patil SP, Laffan AM, Polotsky V, Smith PL . Obesity and obstructive sleep apnea: pathogenic mechanisms and therapeutic approaches. Proc Am Thorac Soc 2008; 5: 185–192.
Lettieri CJ, Eliasson AH, Greenburgh DL . Persistence of obstructive sleep apnea after surgical weight loss. J Clin Sleep Med 2008; 4: 333–338.
Young T, Peppard PE, Gottlieb DJ . Epidemiology of obstructive sleep apnea. Am J Respir Crit Care Med 2002; 165: 1217–1239.
Schein ASO, Kerkhoff AC, Coronel CC, Plentz RDM, Sbruzzi G . Continuous positive airway pressure reduces blood pressure in patients with obstructive sleep apnea; a systematic review and meta-analysis with 1000 patients. J Hypertens 2014; 32: 1762–1773.
Levine DM, Green LW, Deeds SG, Chwalow J, Russell RP, Finlay J . Health education for hypertensive patients. JAMA 1979; 241: 1700–1703.
Gonzalez-Fernandez RA, Rivera M, Torres D, Quiles J, Jackson A . Usefulness of a systemic hypertension in-hospital educational program. Am J Cardiol 1990; 65: 1384–1386.
Farquhar JW, Fortmann SP, Flora JA, Taylor CB, Haskell WL, Williams PT et al. Effects of communitywide education on cardiovascular disease risk factors: the Stanford Five-City Project. JAMA 1990; 264: 359–365.
Hill MN, Bone LR, Hilton SC, Roary MC, Kelen GD, Levine DM . A clinical trial to improve high blood pressure care in young urban black men: recruitment, follow-up, and outcomes. Am J Hypertens 1999; 12: 548–554.
Sclar DA, Chin A, Skaer TL, Okamoto MP, Nakahiro RK, Gill MA . Effect of health education in promoting prescription refill compliance among patients with hypertension. Clin Ther 1991; 13: 489–495.
Tomaszewski M, White C, Patel P, Masca N, Damani R, Hepworth J et al. High rates of non-adherence to antihypertensive treatment revealed by high-performance liquid chromatography-tandem mass spectrometry (HP LC-MS/MS) urine analysis. Heart 2014; 100: 855–861.
Weaver TE, Kribbs NB, Pack AI, Kline LR, Chugh DH, Maislin G et al. Night-to-night variability in CPAP use over the first three months of treatment. Sleep 1997; 20: 278–283.
Weaver TE, Grunstein RR . Adherence to continuous positive airway pressure therapy: the challenge to effective treatment. Proc Am Thorac Soc 2008; 5: 173–178.
Acknowledgements
This work was supported by funding from the NIMHD (R01MD004113, R01MD007716), the NINDS (U54NS081765) and the NHLBI (K24HL111315).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Seixas, A., Ravenell, J., Williams, N. et al. Uncontrolled blood pressure and risk of sleep apnea among blacks: findings from the metabolic syndrome outcome (MetSO) study. J Hum Hypertens 30, 149–152 (2016). https://doi.org/10.1038/jhh.2015.78
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jhh.2015.78