Abstract
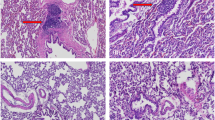
The aim of this study was to test the efficacy of transplantation of bone marrow-derived mesenchymal stem cells (BMSCs) expressing human platelet-derived growth factor A (hPDGF-A) and human beta-defensin2 (hBD2) in accelerating wound healing of combined radiation-wound injury. Recombinant adenovirus vector simultaneously expressing hPDGF-A and hBD2 was constructed and packaged into virus particles that were used to infect rat BMSCs. The expressions of the exogenous in BMSCs were determined by reverse transcriptase (RT)-PCR and western –blot, whereas the functions were determined by cell counting kit (CCK), wound-healing assay on monolayer cells and Kleihauer-Betke (K-B) test. The recombinant adenovirus-infected BMSCs (1 × 107) were subcutaneously transplanted into the wound bed and wound healing was observed for the indicated duration. Rats with combined total body ionizing radiation (6 Gy) and full-thickness skin excision (2% of total body surface area) wound injury were treated with normal BMSCs (group N), BMSCs infected with recombinant adenovirus expressing hPDGF-A and hBD2 (group T) or phosphate-buffered saline (PBS) (group S). The mean wound healing time, percentage of residual wound area (n=8), blind pathological observation (n=3 per time point for each group) and the amount of bacteria under the scar (the same sample was used in the pathological study, n=3) were used for evaluating wound healing. Collagen was visualized by Sirius red staining. Exogenous hPDGF-A and hBD2 were expressed in BMSCs as indicated by RT-PCR and western blot. Faster wound healing of scratched monolayer cells was demonstrated in hPDGF-A/hBD2 gene-modified BMSCs (T-MSCs) when compared with the corresponding control (P<0.01), and conditioned culture medium from T-MSCs showed stimulative effect on BMSC proliferation and in vitro antibiotic effect in the presence of trypsin. Neutralizing antibody interfering in vitro demonstrated that secreted hPDGF-A was the main factor stimulating cell proliferation. In an in vivo test, the radiation-wound combined injury exhibited shorter healing time (21 days). Histologically, there was better granulation formation/maturation and skin-dependent regeneration, as well as more collagen deposition (P<0.01) in rats of group T than in other groups. The deposition and remodeling of collagen in wounds were ranked in the following order: group T>group N>group S. Significantly less bacterial colony formation in the cultured under-scar samples in the rats of group T was observed (P<0.01) at day 7 and thereafter when compared with control. After transplantation, the BMSCs expressed exogenous genes in the wound for at least 2 weeks, as indicated by the reporter gene. Topical transplantation of gene-modified BMSCs promoted wound healing, which may be the benefit of the secretion of antibacterial hBD2 and mitogenic hPDGF-A, resulting in better granulation formation/maturation and skin appendage regeneration in wound. These data demonstrated the potential application of this combination of cell therapy and gene therapy on refractory wound healing.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
References
Pierce GF, Tarpley JE, Allman RM, Goode PS, Serdar CM, Morris B et al. Tissue repair processes in healing chronic pressure ulcers treated with recombinant platelet-derived growth factor BB. Am J Pathol 1994; 145: 1399–1410.
Loots MA, Lamme EN, Zeegelaar J, Mekkes JR, Bos JD, Middelkoop E . Differences in cellular infiltrate and extracellular matrix of chronic diabetic and venous ulcers versus acute wounds. J Invest Dermatol 1998; 111: 850–857.
Supp DM, Wilson-Landy K, Boyce ST . Human dermal microvascular endothelial cells form vascular analogs in cultured skin substitutes after grafting to athymic mice. FASEB J 2002; 16: 797–804.
Robson MC . Wound infection. A failure of wound healing caused by an imbalance of bacteria. Surg Clin North Am 1997; 77: 637–650.
Robson MC, Heggers JP . Bacterial quantification of open wounds. Mil Med 1969; 134: 19–24.
Robson MC, Stenberg BD, Heggers JP . Wound healing alterations caused by infection. Clin Plast Surg 1990; 17: 485–492.
Cooper R, Lawrence JC . Micro-organisms and wounds. J Wound Care 1996; 5: 233–236.
Rasulov MF, Vasilchenkov AV, Onishchenko NA, Krasheninnikov ME, Kravchenko VI, Gorshenin TL et al. First experience of the use bone marrow mesenchymal stem cells for the treatment of a patient with deep skin burns. Bull Exp Biol Med 2005; 139: 141–144.
McFarlin K, Gao X, Liu YB, Dulchavsky DS, Kwon D, Arbab AS et al. Bone marrow-derived mesenchymal stromal cells accelerate wound healing in the rat. Wound Repair Regen 2006; 14: 471–478.
Caplan AI . Mesenchymal stem cells. J Orthop Res 1991; 9: 641–650.
Prockop DJ . Marrow stromal cells as stem cells for nonhematopoietic tissues. Science 1997; 276: 71–74.
Haynesworth SE, Baber MA, Caplan AI . Cytokine expression by human marrow-derived mesenchymal progenitor cells in vitro: effects of dexamethasone and IL-1 alpha. J Cell Physiol 1996; 166: 585–592.
Majumdar MK, Thiede MA, Mosca JD, Moorman M, Gerson SL . Phenotypic and functional comparison of cultures of marrow-derived mesenchymal stem cells (MSCs) and stromal cells. J Cell Physiol 1998; 176: 57–66.
Le Blanc K, Tammik C, Rosendahl K, Zetterberg E, Ringden O . HLA expression and immunologic properties of differentiated and undifferentiated mesenchymal stem cells. Exp Hematol 2003; 31: 890–896.
Bacigalupo A . Mesenchymal stem cells and haematopoietic stem cell transplantation. Best Pract Res Clin Haematol 2004; 17: 387–399.
Mustoe TA, Pierce GF, Morishima C, Deuel TF . Growth factor-induced acceleration of tissue repair through direct and inductive activities in a rabbit dermal ulcer model. J Clin Invest 1991; 87: 694–703.
Grotendorst GR, Martin GR, Pencev D, Sodek J, Harvey AK . Stimulation of granulation tissue formation by platelet-derived growth factor in normal and diabetic rats. J Clin Invest 1985; 76: 2323–2329.
Albertson S, Hummel III RP, Breeden M, Greenhalgh DG . PDGF and FGF reverse the healing impairment in protein-malnourished diabetic mice. Surgery 1993; 114: 368–372.
Mustoe TA, Purdy J, Gramates P, Deuel TF, Thomason A, Pierce GF . Reversal of impaired wound healing in irradiated rats by platelet-derived growth factor-BB. Am J Surg 1989; 158: 345–350.
Harder J, Bartels J, Christophers E, Schroder JM . A peptide antibiotic from human skin. Nature 1997; 387: 861.
Chadebech P, Goidin D, Jacquet C, Viac J, Schmitt D, Staquet MJ . Use of human reconstructed epidermis to analyze the regulation of beta-defensin hBD-1, hBD-2, and hBD-3 expression in response to LPS. Cell Biol Toxicol 2003; 19: 313–324.
Chunmeng S, Tianmin C, Yongping S, Xinze R, Yue M, Jifu Q et al. Effects of dermal multipotent cell transplantation on skin wound healing. J Surg Res 2004; 121: 13–19.
Gu DL, Nguyen T, Gonzalez AM, Printz MA, Pierce GF, Sosnowski BA et al. Adenovirus encoding human platelet-derived growth factor-B delivered in collagen exhibits safety, biodistribution, and immunogenicity profiles favorable for clinical use. Mol Ther 2004; 9: 699–711.
Badiavas EV, Falanga V . Gene therapy. J Dermatol 2001; 28: 175–192.
Crombleholme TM . Adenoviral-mediated gene transfer in wound healing. Wound Repair Regen 2000; 8: 460–472.
Javazon EH, Colter DC, Schwarz EJ, Prockop DJ . Rat marrow stromal cells are more sensitive to plating density and expand more rapidly from single-cell-derived colonies than human marrow stromal cells. Stem Cells 2001; 19: 219–225.
Junqueira LC, Cossermelli W, Brentani R . Differential staining of collagens type I, II and III by Sirius red and polarization microscopy. Arch Histol Jpn 1978; 41: 267–274.
Acknowledgements
This study was supported by the National Key Basic Research and Development Plan, China (‘973’ project 2005GB522605) and the Key Scientific Research Project of PLA, China (06G076 and 06H029).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hao, L., Wang, J., Zou, Z. et al. Transplantation of BMSCs expressing hPDGF-A/hBD2 promotes wound healing in rats with combined radiation-wound injury. Gene Ther 16, 34–42 (2009). https://doi.org/10.1038/gt.2008.133
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/gt.2008.133
Keywords
This article is cited by
-
Bone marrow mesenchymal stem cell-derived exosomal miR-144-5p improves rat ovarian function after chemotherapy-induced ovarian failure by targeting PTEN
Laboratory Investigation (2020)
-
Basic concepts, current evidence, and future potential for gene therapy in managing cutaneous wounds
Biotechnology Letters (2019)
-
Application of stem cells in tissue engineering for defense medicine
Military Medical Research (2018)
-
Mesenchymal stem cell therapy for acute radiation syndrome
Military Medical Research (2016)
-
Effect of mesenchymal stem cells and platelet-derived growth factor on the healing of radiation induced ulcer in rats
Tissue Engineering and Regenerative Medicine (2016)