Abstract
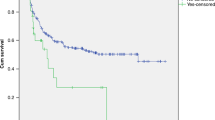
Transplantation-associated thrombotic microangiopathy (TA-TMA) is a serious complication of allogeneic haematopoietic stem cell transplantation (allo-HSCT) with high mortality rate. We retrospectively studied the frequency, clinical and genetic associations and prognostic effect of TA-TMA, in a total of 425 consecutive adult patients, who underwent allo-HSCT for a malignant haematological condition between 2007 and 2013 at our single centre. TA-TMA developed in 19% of the patients. Unrelated donor type (P<0.001), acute GvHD grades II–IV (P<0.001), myeloablative conditioning regimens (P=0.003), tacrolimus-based GvHD prophylaxis (P=0.003), CMV infection (P=0.003) and carriership for HLA-DRB1*11 (P=0.034) were associated with the development of TA-TMA. Survival was adversely affected by the presence of TA-TMA (P<0.001). Among patients with TA-TMA, the outcome of HLA-DRB1*11 carriers was significantly better compared with non-carriers (P=0.003). As a new finding, our observations suggest that the presence of HLA-DRB1*11 antigen contributes to the development of TA-TMA and affects the outcome.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Uderzo CC, Jodele S, Missiry ME, Ciceri F, Busca AB, Bacigalupo A et al. Transplant-associated thrombotic microangiopathy (TA-TMA) and consensus based diagnostic and therapeutic recommendations: which TA-TMA patients to treat and when? J Bone Marrow Res 2014; 2: 152.
Batts ED, Lazarus HM . Diagnosis and treatment of transplantation-associated thrombotic microangiopathy: real progress or are we still waiting? Bone Marrow Transplant 2007; 40: 709–719.
Laskin BL, Goebel J, Davies SM, Jodele S . Small vessels, big trouble in the kidneys and beyond: hematopoietic stem cell transplantation-associated thrombotic microangiopathy. Blood 2011; 118: 1452–1462.
George JN, Li X, McMinn JR, Terrell DR, Vesely SK, Selby GB . Thrombotic thrombocytopenic purpura-hemolytic uremic syndrome following allogeneic HPC transplantation: a diagnostic dilemma. Transfusion 2004; 44: 294–304.
Kojouri K, George JN . Thrombotic microangiopathy following allogeneic hematopoietic stem cell transplantation. Curr Opin Oncol 2007; 19: 148–154.
Stavrou E, Lazarus HM . Thrombotic microangiopathy in haematopoietic cell transplantation: an update. Mediterr J Hematol Infect Dis 2010; 2: e2010033.
Oran B, Donato M, Aleman A, Hosing C, Korbling M, Detry MA et al. Transplant-associated microangiopathy in patients receiving tacrolimus following allogeneic stem cell transplantation: risk factors and response to treatment. Biol Blood Marrow Transplant 2007; 13: 469–477.
Ruutu T, Hermans J, Niederwieser D, Gratwohl A, Kiehl M, Volin L et al. Thrombotic thrombocytopenic purpura after allogeneic stem cell transplantation: a survey of the European Group for Blood and Marrow Transplantation (EBMT). Br J Haematol 2002; 118: 1112–1119.
Cho BS, Yahng SA, Lee SE, Eom KS, Kim YJ, Kim HJ et al. Validation of recently proposed consensus criteria for thrombotic microangiopathy after allogeneic hematopoietic stem-cell transplantation. Transplantation 2010; 90: 918–926.
Willems E, Baron F, Seidel L, Frère P, Fillet G, Beguin Y . Comparison of thrombotic microangiopathy after allogeneic hematopoietic cell transplantation with high-dose or nonmyeloablative conditioning. Bone Marrow Transplant 2010; 45: 689–693.
Labrador J, López-Corral L, López-Godino O, Vázquez L, Cabrero-Calvo M, Pérez-López R et al. Risk factors for thrombotic microangiopathy in allogeneic hematopoietic stem cell recipients receiving GVHD prophylaxis with tacrolimus plus MTX or sirolimus. Bone Marrow Transplant 2014; 49: 684–690.
Shayani S, Palmer J, Stiller T, Liu X, Thomas SH, Khuu T et al. Thrombotic microangiopathy associated with sirolimus level after allogeneic hematopoietic cell transplantation with tacrolimus/sirolimus-based graft-versus-host disease prophylaxis. Biol Blood Marrow Transplant 2013; 19: 298–304.
Rodriguez R, Nakamura R, Palmer JM, Parker P, Shayani S, Nademanee A et al. A phase II pilot study of tacrolimus/sirolimus GVHD prophylaxis for sibling donor hematopoietic stem cell transplantation using 3 conditioning regimens. Blood 2010; 115: 1098–1105.
Rosenthal J, Pawlowska A, Bolotin E, Cervantes C, Maroongroge S, Thomas SH et al. Transplant-associated thrombotic microangiopathy in pediatric patients treated with sirolimus and tacrolimus. Pediatr Blood Cancer 2011; 57: 142–146.
Khaled SK, Palmer J, Stiller T, Senitzer D, Maegawa R, Rodriguez R et al. A phase II study of sirolimus, tacrolimus and rabbit anti-thymocyte globulin as GVHD prophylaxis after unrelated-donor PBSC transplant. Bone Marrow Transplant 2013; 48: 278–283.
Platzbecker U, von Bonin M, Goekkurt E, Radke J, Binder M, Kiani A et al. Graft-versus-host disease prophylaxis with everolimus and tacrolimus is associated with a high incidence of sinusoidal obstruction syndrome and microangiopathy: results of the EVTAC trial. Biol Blood Marrow Transplant 2009; 15: 101–108.
Changsirikulchai S, Myerson D, Guthrie KA, McDonald GB, Alpers CE, Hingorani SR . Renal thrombotic microangiopathy after hematopoietic cell transplant: role of GVHD in pathogenesis. Clin J Am Soc Nephrol 2009; 4: 345–353.
Cho BS, Min CK, Eom KS, Kim YJ, Kim HJ, Lee S et al. Clinical impact of thrombotic microangiopathy on the outcome of patients with acute graft-versus-host disease after allogeneic hematopoietic stem cell transplantation. Bone Marrow Transplant 2008; 41: 813–820.
Worel N, Greinix HT, Leitner G, Mitterbauer M, Rabitsch W, Rosenmayr A et al. ABO-incompatible allogeneic hematopoietic stem cell transplantation following reduced-intensity conditioning: close association with transplant-associated microangiopathy. Transfus Apher Sci 2007; 36: 297–304.
Zheng XL . ADAMTS13 and von Willebrand factor in thrombotic thrombocytopenic purpura. Annu Rev Med 2015; 66: 211–225.
Kennedy GA, Kearey N, Bleakley S, Butler J, Mudie K, Durrant S . Transplantation-associated thrombotic microangiopathy: effect of concomitant GVHD on efficacy of therapeutic plasma exchange. Bone Marrow Transplant 2010; 45: 699–704.
Scully M, Brown J, Patel R, McDonald V, Brown CJ, Machin S . Human leukocyte antigen association in idiopathic thrombotic thrombocytopenic purpura: evidence for an immunogenetic link. J Thromb Haemost 2010; 8: 257–262.
John ML, Hitzler W, Scharrer I . The role of human leukocyte antigens as predisposing and/or protective factors in patients with idiopathic thrombotic thrombocytopenic purpura. Ann Hematol 2012; 91: 507–510.
Coppo P, Busson M, Veyradier A, Wynckel A, Poullin P, Azoulay E et al. HLA-DRB1*11: a strong risk factor for acquired severe ADAMTS13 deficiency-related idiopathic thrombotic thrombocytopenic purpura in Caucasians. J Thromb Haemost 2010; 8: 856–859.
Przepiorka D, Weisdorf D, Martin P, Klingemann HG, Beatty P, Hows J et al. 1994 Consensus Conference on Acute GVHD Grading. Bone Marrow Transplant 1995; 15: 825–828.
Ho VT, Cutler C, Carter S, Martin P, Adams R, Horowitz M et al. Blood and Marrow Transplant Clinical Trials Network Toxicity Committee Consensus Summary: thrombotic microangiopathy after hematopoietic stem cell transplantation. Biol Blood Marrow Transplant 2005; 11: 571–575.
Fine JP, Gray RJ . A proportional hazards model for the subdistribution of a competing risk. J Am Stat Assoc 1999; 94: 496–509.
Kharfan-Dabaja MA, Pidala J, Anasetti C . Thrombotic microangiopathy after GVHD prophylaxis with tacrolimus/sirolimus: a call for use of consensus definition in reporting. Blood 2010; 115: 4316–4317.
Ruutu T, Barosi G, Benjamin RJ, Clark RE, George JN, Gratwohl A et al. Diagnostic criteria for hematopoietic stem cell transplant-associated microangiopathy: results of a consensus process by an International Working Group. Haematologica 2007; 92: 95–100.
Kennedy GA, Bleakley S, Butler J, Mudie K, Kearey N, Durrant S . Posttransplant thrombotic microangiopathy: sensitivity of proposed new diagnostic criteria. Transfusion 2009; 49: 1884–1889.
Jodele S, Davies SM, Lane A, Khoury J, Dandoy C, Goebel J et al. Diagnostic and risk criteria for HSCT-associated thrombotic microangiopathy: a study in children and young adults. Blood 2014; 124: 645–653.
Goyama S, Takeuchi K, Kanda Y, Nannya Y, Chiba S, Fukayama M et al. Post-transplant endothelial disorder after hematopoietic SCT: a blinded autopsy study. Bone Marrow Transplant 2012; 47: 1243–1245.
Arons E, Adams S, Venzon DJ, Pastan I, Kreitman RJ . Class II human leucocyte antigen DRB1*11 in hairy cell leukaemia patients with and without haemolytic uraemic syndrome. Br J Haematol 2014; 166: 729–738.
Gladman DD, Kung TN, Siannis F, Pellett F . Farewell VT, Lee P. HLA markers for susceptibility and expression in scleroderma. J Rheumatol 2005; 32: 1481–1487.
Reveille JD . Genetic studies in the rheumatic diseases: present status and implications for the future. J Rheumatol Suppl 2005; 72: 10–13.
Pavlovsky L, Israeli M, Sagy E, Berg AL, David M, Shemer A et al. Lichen planopilaris is associated with HLA DRB1*11 and DQB1*03 alleles. Acta Derm Venereol 2015; 95: 177–180.
He X, Yu C, Zhao P, Ding Y, Liang X, Zhao Y et al. The genetics of Henoch-Schönlein purpura: a systematic review and meta-analysis. Rheumatol Int 2013; 33: 1387–1395.
Veneri D, De Matteis G, Solero P, Federici F, Zanuso C, Guizzardi E et al. Analysis of B- and T-cell clonality and HLA class II alleles in patients with idiopathic thrombocytopenic purpura: correlation with Helicobacter pylori infection and response to eradication treatment. Platelets 2005; 16: 307–311.
Theodorou I, Abel L, Mauro F, Duprey B, Magnac C, Payelle-Brogard B et al. High occurence of DRB1 11 in chronic lymphocytic leukaemia families. Br J Haematol 2002; 119: 713–715.
Davidson EJ, Davidson JA, Sterling JC, Baldwin PJ, Kitchener HC, Stern PL . Association between human leukocyte antigen polymorphism and human papillomavirus 16-positive vulval intraepithelial neoplasia in British women. Cancer Res 2003; 63: 400–403.
Climent C, Nazario CM, Umpierre S, Quintero M, Gorbea S . Major histocompatibility complex class II polymorphisms and risk of cervical cancer in Puerto Rican women. P R Health Sci J 2007; 26: 97–101.
Pollack MS, Safai B, Myskowski PL, Gold JW, Pandey J, Dupont B . Frequencies of HLA and Gm immunogenetic markers in Kaposi's sarcoma. Tissue Antigens 1983; 21: 1–8.
Acknowledgements
We thank Tatai Gabor for the data management. This work was supported by grants from OTKA (K104903).
Author contributions
KB, HA, AT, PR, ABat and TM co-ordinated the study; KB, HA, AT and TM wrote the manuscript; KB and HA performed the statistical analysis; PR, ABat, LL, ABar, LG, MR and TM provided patients, collected the clinical data and critically reviewed the manuscript; KR provided the data from HLA registry; ABo, KPK, AS and DI performed and authorised the laboratory work for this study; all authors approved the final version of the paper.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on Bone Marrow Transplantation website
Supplementary information
Rights and permissions
About this article
Cite this article
Balassa, K., Andrikovics, H., Remenyi, P. et al. The potential role of HLA-DRB1*11 in the development and outcome of haematopoietic stem cell transplantation-associated thrombotic microangiopathy. Bone Marrow Transplant 50, 1321–1325 (2015). https://doi.org/10.1038/bmt.2015.161
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bmt.2015.161
This article is cited by
-
Transplant-associated thrombotic microangiopathy: theoretical considerations and a practical approach to an unrefined diagnosis
Bone Marrow Transplantation (2021)