Abstract
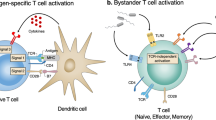
Inflammation induced during infection can both promote and suppress immunity. This contradiction suggests that inflammatory cytokines affect the immune system in a context-dependent manner. Here we show that nonspecific bystander inflammation conditions naive CD4+ T cells for enhanced peripheral Foxp3 induction and reduced effector differentiation. This results in inhibition of immune responses in vivo via a Foxp3-dependent effect on antigen-specific naive CD4+ T cell precursors. Such conditioning may have evolved to allow immunity to infection while limiting subsequent autoimmunity caused by release of self-antigens in the wake of infection. Furthermore, this phenomenon suggests a mechanistic explanation for the idea that early tuning of the immune system by infection affects the long-term quality of immune regulation.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
References
Yoshimura, A., Naka, T. & Kubo, M. SOCS proteins, cytokine signalling and immune regulation. Nat. Rev. Immunol. 7, 454–465 (2007).
Schmitz, M.L., Weber, A., Roxlau, T., Gaestel, M. & Kracht, M. Signal integration, crosstalk mechanisms and networks in the function of inflammatory cytokines. Biochim. Biophys. Acta 1813, 2165–2175 (2011).
Scott-Browne, J.P. et al. Expansion and function of Foxp3-expressing T regulatory cells during tuberculosis. J. Exp. Med. 204, 2159–2169 (2007).
Haribhai, D. et al. A requisite role for induced regulatory T cells in tolerance based on expanding antigen receptor diversity. Immunity 35, 109–122 (2011).
Bilate, A.M. & Lafaille, J.J. Induced CD4+Foxp3+ regulatory T cells in immune tolerance. Annu. Rev. Immunol. 30, 733–758 (2012).
Janeway, C.A. Jr. & Medzhitov, R. Innate immune recognition. Annu. Rev. Immunol. 20, 197–216 (2002).
van Duin, D., Medzhitov, R. & Shaw, A.C. Triggering TLR signaling in vaccination. Trends Immunol. 27, 49–55 (2006).
Thompson, L.J., Valladao, A.C. & Ziegler, S.F. Cutting edge: de novo induction of functional Foxp3+ regulatory CD4 T cells in response to tissue-restricted self antigen. J. Immunol. 186, 4551–4555 (2011).
Srivastava, S., Koch, M.A., Pepper, M. & Campbell, D.J. Type I interferons directly inhibit regulatory T cells to allow optimal antiviral T cell responses during acute LCMV infection. J. Exp. Med. 211, 961–974 (2014).
Coffman, R.L., Sher, A. & Seder, R.A. Vaccine adjuvants: putting innate immunity to work. Immunity 33, 492–503 (2010).
Boyman, O. Bystander activation of CD4+ T cells. Eur. J. Immunol. 40, 936–939 (2010).
Christen, U. & von Herrath, M.G. Do viral infections protect from or enhance type 1 diabetes and how can we tell the difference? Cell. Mol. Immunol. 8, 193–198 (2011).
Mills, K.H. TLR-dependent T cell activation in autoimmunity. Nat. Rev. Immunol. 11, 807–822 (2011).
Bach, J.F. Infections and autoimmune diseases. J. Autoimmun. 25 (suppl.), 74–80 (2005).
Headley, M.B. et al. TSLP conditions the lung immune environment for the generation of pathogenic innate and antigen-specific adaptive immune responses. J. Immunol. 182, 1641–1647 (2009).
Durrant, D.M. & Metzger, D.W. Emerging roles of T helper subsets in the pathogenesis of asthma. Immunol. Invest. 39, 526–549 (2010).
Saff, R.R., Spanjaard, E.S., Hohlbaum, A.M. & Marshak-Rothstein, A. Activation-induced cell death limits effector function of CD4 tumor-specific T cells. J. Immunol. 172, 6598–6606 (2004).
Takahashi, R. et al. SOCS1 is essential for regulatory T cell functions by preventing loss of Foxp3 expression as well as IFN-γ and IL-17A production. J. Exp. Med. 208, 2055–2067 (2011).
Lu, L.F. et al. Foxp3-dependent microRNA155 confers competitive fitness to regulatory T cells by targeting SOCS1 protein. Immunity 30, 80–91 (2009).
Haxhinasto, S., Mathis, D. & Benoist, C. The AKT-mTOR axis regulates de novo differentiation of CD4+Foxp3+ cells. J. Exp. Med. 205, 565–574 (2008).
Delgoffe, G.M. et al. The mTOR kinase differentially regulates effector and regulatory T cell lineage commitment. Immunity 30, 832–844 (2009).
Yamane, H. & Paul, W.E. Early signaling events that underlie fate decisions of naive CD4+ T cells toward distinct T-helper cell subsets. Immunol. Rev. 252, 12–23 (2013).
Wei, J. et al. Antagonistic nature of T helper 1/2 developmental programs in opposing peripheral induction of Foxp3+ regulatory T cells. Proc. Natl. Acad. Sci. USA 104, 18169–18174 (2007).
Bettelli, E. et al. Reciprocal developmental pathways for the generation of pathogenic effector TH17 and regulatory T cells. Nature 441, 235–238 (2006).
Wang, Y. et al. Timing and magnitude of type I interferon responses by distinct sensors impact CD8 T cell exhaustion and chronic viral infection. Cell Host Microbe 11, 631–642 (2012).
Barchet, W. et al. Virus-induced interferon-α production by a dendritic cell subset in the absence of feedback signaling in vivo. J. Exp. Med. 195, 507–516 (2002).
Matsumoto, M. & Seya, T. TLR3: interferon induction by double-stranded RNA including poly(I:C). Adv. Drug Deliv. Rev. 60, 805–812 (2008).
Liu, Y. et al. FoxA1 directs the lineage and immunosuppressive properties of a novel regulatory T cell population in EAE and MS. Nat. Med. 20, 272–282 (2014).
Dumont, F.J. & Coker, L.Z. Interferon-α/β enhances the expression of Ly-6 antigens on T cells in vivo and in vitro. Eur. J. Immunol. 16, 735–740 (1986).
Taniguchi, T. & Takaoka, A. A weak signal for strong responses: interferon-α/β revisited. Nat. Rev. Mol. Cell Biol. 2, 378–386 (2001).
Knutson, K.L. & Disis, M.L. Tumor antigen-specific T helper cells in cancer immunity and immunotherapy. Cancer Immunol. Immunother. 54, 721–728 (2005).
Zhou, G., Drake, C.G. & Levitsky, H.I. Amplification of tumor-specific regulatory T cells following therapeutic cancer vaccines. Blood 107, 628–636 (2006).
Zhou, G. & Levitsky, H.I. Natural regulatory T cells and de novo-induced regulatory T cells contribute independently to tumor-specific tolerance. J. Immunol. 178, 2155–2162 (2007).
Zhou, L. et al. TGF-β-induced Foxp3 inhibits TH17 cell differentiation by antagonizing RORγt function. Nature 453, 236–240 (2008).
Miyao, T. et al. Plasticity of Foxp3+ T cells reflects promiscuous Foxp3 expression in conventional T cells but not reprogramming of regulatory T cells. Immunity 36, 262–275 (2012).
Longhi, M.P. et al. Dendritic cells require a systemic type I interferon response to mature and induce CD4+ Th1 immunity with poly IC as adjuvant. J. Exp. Med. 206, 1589–1602 (2009).
González-Navajas, J.M., Lee, J., David, M. & Raz, E. Immunomodulatory functions of type I interferons. Nat. Rev. Immunol. 12, 125–135 (2012).
Teijaro, J.R. et al. Persistent LCMV infection is controlled by blockade of type I interferon signaling. Science 340, 207–211 (2013).
Wilson, E.B. et al. Blockade of chronic type I interferon signaling to control persistent LCMV infection. Science 340, 202–207 (2013).
Stelekati, E. et al. Bystander chronic infection negatively impacts development of CD8+ T cell memory. Immunity 40, 801–813 (2014).
Osokine, I. et al. Type I interferon suppresses de novo virus-specific CD4 Th1 immunity during an established persistent viral infection. Proc. Natl. Acad. Sci. USA 111, 7409–7414 (2014).
Bach, J.F. The effect of infections on susceptibility to autoimmune and allergic diseases. N. Engl. J. Med. 347, 911–920 (2002).
Dunn, G.P., Koebel, C.M. & Schreiber, R.D. Interferons, immunity and cancer immunoediting. Nat. Rev. Immunol. 6, 836–848 (2006).
Grivennikov, S.I., Greten, F.R. & Karin, M. Immunity, inflammation, and cancer. Cell 140, 883–899 (2010).
Trinchieri, G. Cancer and inflammation: an old intuition with rapidly evolving new concepts. Annu. Rev. Immunol. 30, 677–706 (2012).
Conroy, H., Marshall, N.A. & Mills, K.H. TLR ligand suppression or enhancement of Treg cells? A double-edged sword in immunity to tumours. Oncogene 27, 168–180 (2008).
Virgin, H.W., Wherry, E.J. & Ahmed, R. Redefining chronic viral infection. Cell 138, 30–50 (2009).
Koch, M.A. et al. T-bet+ Treg cells undergo abortive Th1 cell differentiation due to impaired expression of IL-12 receptor-β2. Immunity 37, 501–510 (2012).
Lyons, A.B. Analysing cell division in vivo and in vitro using flow cytometric measurement of CFSE dye dilution. J. Immunol. Methods 243, 147–154 (2000).
Mellor, A.L. et al. Cutting edge: CpG oligonucleotides induce splenic CD19+ dendritic cells to acquire potent indoleamine 2,3-dioxygenase-dependent T cell regulatory functions via IFN Type 1 signaling. J. Immunol. 175, 5601–5605 (2005).
Floess, S. et al. Epigenetic control of the foxp3 locus in regulatory T cells. PLoS Biol. 5, e38 (2007).
Acknowledgements
We thank D. Campbell, J. Hamerman and E. Bettelli for helpful discussion, and S. Ma and Aru K. for technical assistance. We thank A. Abbas, M. Orr and A. Marshak-Rothstein for mice and materials. Supported by American Cancer Society postdoctoral fellowship 121930-PF-12-071-01-LIB and National Institute of Allergy and Infectious Diseases (NIAID) grant T32 AI007411 (L.J.T.) and the Juvenile Diabetes Research Foundation Cooperative Center for Cellular Therapy and US National Institutes of Health grant CA182783 (S.F.Z.).
Author information
Authors and Affiliations
Contributions
L.J.T. and S.F.Z. developed the study. L.J.T. and J.-F.L. designed and performed the experiments. A.C.V., T.D.T. and Z.L.U. performed in vitro experiments. L.J.T. and S.F.Z. wrote the manuscript, and all authors contributed to manuscript editing.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Integrated supplementary information
Supplementary Figure 1 Bystander inflammation conditioned Treg cells have normal functional suppressive activity and ex vivo phenotype.
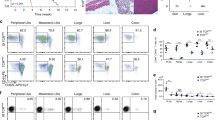
WT Balb/c mice were treated with polyI:C (pIC) or PBS (ctr) via i.p. injection for two consecutive days. (a) Splenocytes were assessed for frequency (left panel) and total number (right panel) of intracellular Foxp3+ CD4 T cells seven days after the first injection. Each symbol represents an individual mouse. P-values by student’s two-tailed t-test, *p<0.05, **p<0.01. (b-d) In vitro T cell suppression assay with TREG isolated from ctr and pIC-treated mice. Activation of effector CD4+ T cells as shown by (b) proliferation, (c) CD25 expression (mean florescence intensity, MFI), and (d) intracellular T-bet expression. Bar graph depicts mean plus SEM, data representative of two independent experiments, n=2 mice per group. (e) Splenocytes from pbs- and pIC-treated mice were stimulated ex vivo and intracellular cytokine expression was assessed. (f) Diagram depicting experimental approach for acute primary airway inflammation. Following intranasal treatment with pIC or PBS, mice were primed intranasally with TSLP and OVA, then challenged with OVA one week later, see Materials and Methods for detailed description. (g) Total pulmonary neutrophil counts from mice treated as described in main figure 1, each symbol represents an individual mouse.
Supplementary Figure 2 Diminished efficacy of immunization that follows nonspecific inflammation.
(a) Experimental schematic for data described in Figure 2. Briefly, Balb/c mice were treated with pbs or pIC for 2 consecutive days, then on the fourth day after the first treatment, mice were immunized with subcutaneous Ova/IFA. Approximately one week later mice were challenged with Ova either in the in the context of direct intranasal challenge or A20 lymphoma expressing Ova (A20-tGO). See Materials and Methods for detailed description. (b) Mean time of tumor onset, as determined by initial identification of measurable tumor mass following subcutaneous inoculation. Incidence of tumor-bearing mice as a fraction of the total mice in each group is shown below. P-value by one-tailed Mann-Whitney U-test.
Supplementary Figure 3 Nonspecific bystander inflammation produces ICTN cells that have altered molecular response but retain survival and proliferative ability.
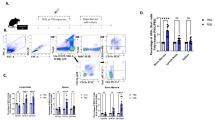
(a) Experimental Schematic; DR mice were given intraperitoneal injection of pbs (ctr) or pIC for two consecutive days, then on the third day spleen and lymph nodes were harvested and purified by magnetic bead enrichment. Cells were then analyzed directly ex vivo or manipulated as described. (b) DR cells were cultured for 16-20 hours with Ova-pulsed APC, cells were fixed and stained for intracellular phospho-AKT (pAKT). For controls, DR cells were cultured with APC with no antigen (not shown). Bar graphs (right panels) depict mean plus SEM of triplicate values of mean florescence intensity (mfi) of pAKT. Data are representative of three independent experiments, n=3 mice per group. (c-d) CFSE-labeled DR cells were cultured for 5 days with OVA-peptide-pulsed APC and cells were assessed by FACS for proliferation by CFSE dilution and survival by viability marker. (b) CFSE dilution of DR cells; representative FACS histogram (left), bar graph depicting mean plus SEM of triplicate values for proliferation index of DR cells as calculated based on CFSE dilution (right). (c) Frequency of viable DR cells by fluorescent viability marker, bar graph depicts mean plus SEM of triplicate values. Data are representative of three independent experiments, n=3 mice per group. P-value by student’s two-tailed t-test, *p<0.01.
Supplementary Figure 4 Enhanced de novo Foxp3+ cell induction from ICTN cells is not dependent on APCs in the microenvironment.
(a) CD4+ T cells from ctr or pIC-treated DR mice were isolated then stimulated for 5 days with plate-bound anti-CD3 and anti-CD28 with no APC. Foxp3 expression was assessed by intracellular staining, representative FACS plot from 3 independent experiments is shown, n=3 mice per group. (b) CD4+ T cells from PBS-treated (ctr) or polyI:C-treated (pIC) DR mice were assessed for methylation of the Foxp3 promoter by bisulfite sequencing analysis. Control cells were obtained by FACS sorting of CD4+ T cells; regulatory T cells, (TREG) were isolated by positive expression of CD25 and GITR, naïve T cells (Tnaive) were CD25-negative, CD62L+, CD44low. Effector TH1 cells (TH1) were obtained by culturing Tnaive cells with plate-bound anti-CD3/CD28 with IL-12 for six days. Bar graph depicts mean plus SEM of values obtained by analysis of samples from three independent experiments, n=3 mice per group. (c) mRNA expression of Tgfbr1 from purified DR cells from control and polyI:C-treated donors. Bar graphs depict fold change in expression of indicated mRNA from polyI:C-treated cells vs controls (set to 1) after normalization to Gapdh mRNA. Mean plus SEM of fold change ratios from three independent experiments, n=3 mice per group. (d) DR cells from ctr (open histogram) or pIC-treated mice (shaded histogram) were cultured for 24 hours with OVA-peptide-pulsed APC and TGFβ, then assessed for intracellular phospho-SMAD2/3. FACS histogram representative of two independent experiments, n=2 mice per group.
Supplementary Figure 5 Enhanced de novo Foxp3+ cell induction from ICTN cells utilizes IFN-I pathways but does not involve IL-10, PDL-1 or IDO.
(a) DR cells from mice treated with pIC, LPS, or gardiquimod were cultured 5 days with Ova-pulsed APCs with or without TGFβ, and intracellular Foxp3 was assessed. Bar graph depicts mean plus SEM of triplicate values of fold difference in % Foxp3+ relative to average control % Foxp3+ in PBS (ctr) DR cells. (b) Total spleen and lymph node cells were harvested from DR mice and incubated with either PBS, 3μg of polyI:C alone (pIC) or with blocking anti-IFNaR antibody (pIC + aIFNaR Ab), or recombinant IFNβ (IFNβ). After 48 hours, naïve CD4+ T cells were purified by MACS and cultured with Ova-pulsed APCs and TGFβ, and 3 days later stained for intracellular Foxp3. Experimental schematic shown (left). Bar graph depicts mean plus SEM of triplicate values of fold difference in % Foxp3+ relative to average control % Foxp3+ in PBS (ctr) DR cells. Data are representative of two independent experiments, n=2 mice per group. (c) WT and IfnarKO DR cells were cultured for 5 days in non-skewing conditions, then stimulated with PMA+Ionomycin and assessed for IFNγ production by intracellular cytokine staining. Bar graph depicts % IFNγ+ DR cells, mean plus SEM for triplicate values. Data are representative of two independent experiments, n=2 mice per group. (d) mRNA expression of Ifnar1 and Ifnar2 from purified DR cells from control and polyI:C-treated donors. Bar graphs depict fold change in expression of indicated mRNA from polyI:C-treated cells vs controls (set to 1) after normalization to Gapdh mRNA. Mean plus SEM of fold change ratios from three independent experiments, n=3 mice per group. (e) DR cells were rested overnight, then stimulated for 30 minutes with recombinant IFNβ and stained for intracellular phospho-STAT1. PBS added for 30 minutes as negative control. FACS histogram representative of two independent experiments. (f-g) DR cells from ctr or pIC-treated mice were cultured with Ova-peptide-pulsed APC and TGFβ in the presence of (f) rat IgG2a isotype control, anti-IL-10, or anti-PDL1 neutralizing antibodies or (g) NaOH vehicle control or 1-MT, and intracellular Foxp3 was assessed. (h-i) WT or IfnarKO DR cells were transferred into WT or IfnarKO Balb/c recipients, and host mice were treated with PBS (ctr) or pIC. Data are representative of two independent experiments, n=2 mice per group. (h) Expression of Ly6C on donor DR cells directly ex vivo. (i) DR cells were cultured with Ova-pulsed APCs in non-skewing conditions and at day 5 cultures were stimulated with PMA+Ionomycin and intracellular IFNγ was assessed. Mean plus SEM of fold change ratios from three independent experiments, n=3 mice per group. P-values by student’s two-tailed t-test, *p<0.05, **p<0.01.
Supplementary Figure 6 Functional Foxp3 is required for ICTN cells to regulate antigen-specific responses.
(a,b) Mean time of tumor onset for data described in (main Fig. 6a,b), respectively. Incidence of tumor-bearing mice as a fraction of the total mice in each group is shown below. (c) RIP-mOva/RAGKO host mice received pIC-primed sf DR cells (sf DR, Donor pIC), or received ctr sf DR cells (sf DR, no tx), and blood glucose was monitored. Graph shows diabetes-free survival. P-value by one-tailed Mann-Whitney U-test, p<0.05. (d) Experimental setup for data described in Fig. 6d-e. Donor DR mice were treated with pIC or PBS as described previously, then CD4+ T cells were isolated and transferred into Rip-mOva/RAGKO host mice. One day after transfer, all host mice were treated with pIC, and assessments conducted as described on day 20.
Supplementary Figure 7 Phenotype and stability of DR cells during transient bystander inflammation.
(a) Experimental schematic; purified DR cells were transferred into wt Balb/c recipients. Host mice were treated with pIC at indicated days prior to harvest of lymphoid tissues, for two consecutive daily treatments. Mice treated on day 0 were treated 6 and 3 hours prior to harvest (first day of treatment indicated for simplicity). Control mice were given PBS injections. (b) Profile of bystander activation markers from donor DR cells from mice treated with pIC at indicated timepoints. (c) Frequency of donor DR cells among total TCRb+ T cells in mice at indicated timepoints after pIC treatment. One of two independent experiments shown.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–7 (PDF 1334 kb)
Rights and permissions
About this article
Cite this article
Thompson, L., Lai, JF., Valladao, A. et al. Conditioning of naive CD4+ T cells for enhanced peripheral Foxp3 induction by nonspecific bystander inflammation. Nat Immunol 17, 297–303 (2016). https://doi.org/10.1038/ni.3329
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ni.3329
This article is cited by
-
A controlled human Schistosoma mansoni infection model to advance novel drugs, vaccines and diagnostics
Nature Medicine (2020)
-
CXCR3 enables recruitment and site-specific bystander activation of memory CD8+ T cells
Nature Communications (2019)