Abstract
The ability of HIV-1 to use dendritic cells (DCs) for transport and to transfer virus to activated T cells in the lymph node may be crucial in early HIV-1 pathogenesis. We have characterized primary DCs for the receptors involved in viral envelope attachment and observed that C-type lectin receptor (CLR) binding was predominant in skin DCs, whereas binding to emigrating and tonsil DCs was CD4-dependent. No one CLR was solely responsible for envelope binding on all skin DC subsets. DC-SIGN (DC-specific ICAM-3–grabbing nonintegrin) was only expressed by CD14+CDlalo dermal DCs. The mannose receptor was expressed by CD1ahi and CD14+CDlalo dermal DCs, and langerin was expressed by Langerhans cells. The diversity of CLRs able to bind HIV-1 in skin DCs may reflect their ability to bind a range of microbial glycoproteins.
Similar content being viewed by others
Main
Dendritic cells (DCs) are critical for initiating immune responses due to their ability to take up antigen in the peripheral tissues, migrate to the secondary lymphoid organs and present processed antigens to recirculating naïve T cells1. The ability of DCs to capture HIV and present it to CD4+ T lymphocytes in vitro—which results in explosive foci of viral replication—suggests that HIV-1 may use genital mucosa DCs for uptake and transport to their major cell target, CD4+ T lymphocytes in draining lymph nodes in vivo2,3,4. Indeed, Langerhans cells (LCs) in the squamous epithelia of genital mucosa (or skin) are infected by HIV-1 in ex vivo models of transmission5,6. Tracking of SIV entry into the vaginal epithelium of macaque monkeys suggested LCs are the initial infectable targets7,8, although HIV replication was also detected soon after transmission in resting CD4+ T lymphocytes in the lamina propria, beneath the columnar epithelium of the endocervix and in the tonsils9,10. DCs in the lamina propria deep in the genital or anal mucosa epithelium are also among the first leukocytes that encounter HIV and, in animal models, can carry infectious virus to the lymph node without becoming productively infected themselves11.
HIV enters CD4+ T lymphocytes and macrophages via CD4 in conjunction with CCR5 (R5 isolates) or CXCR4 (X4 isolates)12. However, on other cells—such as DCs—HIV can efficiently bind to additional receptors independently of CD413,14,15,16,17. Studies of monocyte-derived DCs (MDDCs) have emphasized the importance of mannose C-type lectin receptors (MCLRs), particularly the DC-specific ICAM-3–grabbing nonintegrin (DC-SIGN), for HIV gp120 binding15. DC-SIGN was originally described, from a placental cDNA library, as an MCLR that is able to bind gp12018. Later, it was reported to be the major receptor for HIV gp120 on MDDCs and to facilitate HIV transfer from MDDCs to CD4+ T lymphocytes15. A more recent comparison of gp120 binding to MDDCs differentiated in vitro with blood DCs isolated ex vivo showed marked differences in HIV gp120 binding16. Multiple MCLRs were most important for gp120 binding to MDDCs, whereas gp120 binding to blood DCs was CD4-dependent16.
Therefore, to determine the relative contribution of CD4 and MCLRs to viral binding on a broader range of different DC subsets, especially DCs at mucosal sites, we examined CD4 and MCLR expression, the mechanism of gp120 binding to these receptors and HIV entry in a variety of DCs from different microenvironments. We compared skin (epidermal and dermal), lymphoid and blood DCs and to in vitro–derived MDDCs and monocyte-derived Langerhan's cells (MDLCs), generated from monocytes like MDCC, but with the addition of transforming growth factor-β (TGF-β).
We show here that CD4 and multiple MCLRs mediate gp120 binding to DCs in peripheral tissues and that the predominant MCLR varies with the DC phenotype and changes during migration. Our finding that HIV uses a spectrum of receptors to attach to key cell types in the body has key implications for antiretroviral therapies aimed at blocking viral uptake and entry. In addition, our results suggest general DC capture mechanisms for microbial antigens via MCLR-glycoprotein interactions in either epithelia, underlying submucosa or dermis.
Results
DC subsets
To study HIV interactions with freshly isolated tissue DCs—which may differ from the more commonly used MDDCs in their repertoire of surface receptors—we obtained fresh (immature) LCs and dermal DCs from human skin as well as DCs from tonsils and blood with minimal culture and enzymatic disruption. We isolated fresh skin DCs from epidermal and dermal skin, rather than the genital tract, as representative immature peripheral DCs. Although there are clear differences between squamous epithelia of the skin and anogenital tract, similar DC populations exist at both sites. In addition, the availability of only small amounts of genital mucosa and consequent low yield of isolated DCs precluded binding studies for several independent donors. These ex vivo DCs were compared to MDDCs and MDLCs in vitro. Epidermal LCs and dermal DCs purified after emigration from cultured skin explants were also used because both simulate the migration of their in vivo counterparts from skin to lymph nodes after inflammation or HIV infection. Both DC subsets have been postulated to transport HIV to lymph nodes3,7,8,19,20.
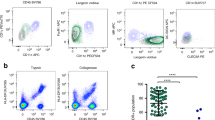
To isolate sufficient numbers of skin and tonsil–derived DCs without destroying the structural and functional integrity of the extracellular receptors meant that certain proteases had to be avoided. Trypsin effectively dissociates epidermal sheets14 and does not cleave either the mannose receptor (MR) or langerin16,21, but it cleaves both CD4 and DC-SIGN16 and therefore affects HIV infectivity assays13. In contrast, we found that collagenase II and collagenase F did not cleave the HIV gp120 binding epitope within domain 1 of CD4—recognized by the monoclonal antibody (mAb) Leu3a—during tissue dissociation and did not affect recognition of DC-SIGN on MDDCs by various mAbs specific for a diverse range of epitopes, including several within the carbohydrate recognition domain (Fig. 1). Therefore, collagenase was routinely used for tissue dissociation to obtain fresh DCs. In subsequent experiments only the DC28 and DC-SIGN1 mAbs were used to identify DC-SIGN.
(a) Effect of collagenase treatment on CD4 and DC-SIGN expression by MDDCs, as a control. MDDCs (1 × 106 cells/ml) were treated with collagenase F (2.5 mg/ml) for 90 min at 37 °C. (b) CD4 expression on immature or emigrant DC subsets. Immature epidermal LCs, dermal DCs and tonsil DCs were dissociated from various tissues by collagenase. For comparison, dermal DC emigrants were obtained 24 h after emigration from dermal explant cultures. Immature LCs and immature or emigrant dermal DCs were stained for the defining surface markers CD1a, HLA-DR and CD45. Samples were gated on CD45 and HLA-DR before CD1a and CD4 analysis. In contrast, tonsil DCs were purified via magnetic columns for expression of HLA-DR and lack of lineage markers (CD3, CD14, CD19 and CD16)16. CD11c was used to further resolve blood DCs into two subsets.
Isolation of immature and emigrant skin DCs
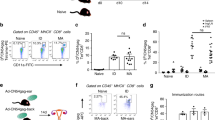
Both leukocyte (lymphocytes and DCs) and nonleukocyte populations (keratinocytes and fibroblasts from surrounding connective tissue) are present in dissociated human skin. The methods we used to prepare epidermis and dermis for flow cytometric analysis of epidermal LCs and dermal DCs differed. In dissociated epidermal preparations, clumping of contaminating keratinocytes interfered with HIV gp120 binding assays, so LCs were sorted by CD1a expression to a purity of >95% (Fig. 2a). After dissociation of dermal tissue and in order to distinguish HLA-DR+ dermal DC subpopulations from fibroblasts and other stromal cells during analysis and characterize the DCs with greater resolution, leukocytes were identified by the pan-leukocyte marker CD45. Two subpopulations of fresh dermal DCs were defined: CD1ahiCD14−CD16− and CD1aloCD14+CD16−. The latter included cells expressing little or no CD1a (Fig. 2bA–C). The identification of both CD1ahiCD14− and CD1aloCD14+ dermal DC subsets was consistent with previously characterized dermal DC subsets22. Contamination of the dermal DC subsets with peripheral blood monocytes was not observed, as shown by the absence of erythrocyte contamination and lack of CD14+CD16+ monocyte populations. As contaminating CD45− dermal cells (mostly fibroblasts) did not bind gp120 and could be excluded from flow cytometric analysis, unfractionated dissociated cell suspensions were used in binding studies. The dermal CD4+ T lymphocytes provided an internal control to measure gp120 binding when CD4-blocking mAbs and mannan were present.
(a) Epidermal LCs were obtained from split-skin collagenase F digestion and purified by successive magnetic and flow cytometric sorting and stained for CD1a expression. (b) (A–C) Phenotyping of immature dermal DCs after collagenase dissociation. DCs were gated to exclude lymphocytes and were also gated with (A–C) CD45 and (B,C) HLA-DR. Quadrants were set to discriminate between CD1ahi and CD1alo populations; the dotted line represents the CD1a isotype control. (A) CD1ahiHLA-DR+++, CD1aloHLA-DR+++ (B) CD1ahiCD14−, CD1aloCD14+ and (C) CD1ahiCD16−, CD1aloCD16−. (D) CD1ahi and CD1alo dermal DCs 24 h after emigrating from epidermal stripped split skin. (c) Blood DC purification. Blood DCs were purified by depletion of lineage+ cells (CD3+CD14+CD19+CD16+ by magnetic sorting), the (A) lineage-depleted and (B) lineage-negative–enriched fractions are shown. The lineage-negative fraction was stained for HLA-DR and CD11c as described16. (C) After lineage-negative gating in B (gate R19), HLA-DR and CD11c were used to resolve the two main DC subpopulations. The cells were subsequently flow cytometrically sorted into the CD11c+ (gate R17) and CD11c− (gate R16) blood DC subsets for HIV infection studies.
Early emigrant DCs (sampled within 24 h of skin culture) from epidermal and dermal sheets3,23 also contained CD1aloCD14+ and CD1ahiCD14− populations (Fig. 2bD and data not shown) that were similar to the subsets of immature LCs and dermal DCs identified in dissociated skin preparations. After longer periods of emigration (>48 h), CD1a was down-regulated, so the mature DCs could only be detected and quantified by their high HLA-DR expression. Thus, relatively pure populations of LCs and the two subsets of dermal DCs could be distinguished by flow cytometric analysis, which enabled us to subsequently study gp120 binding. In comparison, blood DCs could be resolved into two populations according to CD11c expression (Fig. 2cC).
HIV gp120 binding to DC subsets
To evaluate the ability of various DC subsets to bind HIV env, we incubated the cells with biotinylated soluble HIV gp120 (Figs. 3 and 4). Specificity was determined with CD4 mAbs and/or the high mannose ligand mannan, which blocks binding of gp120 to C-type lectins. We observed heterogeneity in HIV gp120 binding patterns across the range of DC subtypes, both in the amount of gp120 bound as well as the nature of the receptors. Anti-CD4 completely blocked binding of gp120 to the CD11c+CD123− and CD11c−CD123+ blood and tonsil DCs (Fig. 3a). In contrast, binding of gp120 to immature CDlahi dermal DC subsets, as well as to immature or epidermal LCs, MDLCs and MDDCs, was blocked by incubation with mannan. Anti-CD4 had little effect on gp120 binding. Thus, gp120 binding to these immature DC and LC subtypes occurred predominantly via MCLRs (Fig. 3a). Regarding the amount of gp120 bound, fresh (immature) LCs consistently bound approximately sixfold more gp120 than immature dermal DCs and MDDCs (Fig. 4dA). Immature (fresh) CD1ahi and CD1alo dermal DCs, LCs, MDDCs and MDLCs in turn bound higher amounts of gp120 than either mature DCs migrating out of skin or MDDCs and MDLCs matured in vitro (Fig. 4dB,eB,fB). The amount of gp120 binding to dermal DCs and LCs decreased progressively with time after emigration. Thus in immature LCs and dermal DCs, gp120 was bound predominantly by MCLRs; however, gp120 was predominantly bound by CD4 in emigrating equivalent DCs and tonsil and blood DCs. (Fig. 3a,b).
(a) Relative contributions of CD4 and MCLRs to HIV gp120 binding on representative immature and emigrating skin DCs, DCs generated in vitro and CD11c+ and CD11c− tonsil and blood DCs. To determine the relative blinding of biotinylated gp120 to MCLR and/or CD4, DCs (1 × 106 cells/ml) were incubated with no inhibitors (1), 5 mg/ml of mannan (MCLR block) (2), 10 μg/ml of Leu3a (CD4 block) (3) or both mannan and Leu3a (MCLR and CD4 block) (4). Percentage binding contributions were calculated as described16. (b) HIV gp120 binding to CD4 and MCLR on dermal DCs isolated at various times after emigration from skin explant cultures. Relative binding contributions were calculated as in a.
HIV gp120 binding to (a,b) MDDCs, (c) MDLCs and (d–f) cutaneous DCs. Open histograms represent the negative controls (no HIV gp120); shaded histograms represent HIV gp120 binding. Absolute mean fluorescence intensity (MFI) values are shown. Experiments are representative of three independent donors. (aB–cB,C) The expression of HIV receptors CD4 and MCLRs are shown as histogram overlays. The isotope control IgG1 was included for comparison. As MDDC binding was variable between donors, two distinct gp120 binding phenotypes are shown in a and b. (d–f) In skin DCs, HIV gp120 binding is compared in immature (A) and emigrant (B) DCs. For skin DCs, expression of the HIV gp120 receptors is shown in Fig. 5.
gp120 binding to MCLRs on tissue DCs
We next examined CD4 and DC-SIGN expression by LCs and the DC subsets to determine the predominant receptor that binds HIV gp120 (Fig. 5). Both CD4 and DC-SIGN can bind gp120 with high affinity. Thus, if expressed at moderate or high amounts on DCs, they are likely to be important in HIV binding and entry. In addition, we measured the expression of two cell surface lectins—langerin and MR—to determine whether these can also function as attachment factors for HIV. We found that tonsil and blood DCs, whether of the myeloid (CD11c+) or plasmacytoid (CD11c−CD123+) subsets, did not express DC-SIGN, langerin or MR on their surface (data not shown), which was consistent with complete inhibition of gp120 binding by anti-CD4 (Fig. 3a).
(a,b) Langerin, MMR, DC-SIGN expression and HIV gp120 binding, as demonstrated by flow cytometry, for freshly isolated (immature) and emigrant LCs and dermal DCs. (c,d) Comparison of CD4 expression and gp120 binding by (c) dermal lymphocytes (gated for expression of CD3 and CD45) and (d) dermal DCs.
Epidermal LCs also failed to express surface MR or DC-SIGN, but did express high amounts of the LC-specific marker langerin and low amounts of CD4 (Figs. 1b and 5a). There was little down-regulation of langerin expression in epidermal LC emigrants (Fig. 5a) and CD4 expression remained low to negative, similar to freshly derived LCs (Fig. 1b). Because gp120 binding to LCs could be inhibited by mannan, but not by anti-CD4, we expressed langerin in quail QT6 cells to determine whether it could efficiently bind gp120 (Fig. 6). We found that langerin efficiently bound both HIV-1 and HIV-2 gp120 proteins in a mannan inhibitable manner (Fig. 6b,c). Thus, langerin could function as an attachment factor for the HIV env protein, and the high amounts of gp120 bound by LCs correlated with the high amounts of langerin expression on freshly isolated cells. Because the anti-langerin DCGM4 antibody did not inhibit gp120 binding to langerin expressed on quail QT6 cells or LCs, we were unable to specifically block gp120 interactions with langerin on LCs to determine whether other proteins might also support gp120 binding (data not shown). There was an 90% reduction in gp120 binding by LC emigrants over 24 h, whereas langerin expression was maintained on the bulk of the population. This suggested that another unidentified MCLR was was binding gp120 on immature LCs and was down-regulated on LC emigrants (Fig. 5a). However, a small subset of LCs did down-regulate langerin expression. Thus, LCs bind gp120 via surface langerin and possibly another unidentified MCLR or MCLRs.
(a) HIV gp120 binding to stable MR transfectant Rat-6 cells and inhibition with mannan. Gates were set on untransfected cells to show MR expression by the transfectants. (b,c) HIV-1 and HIV-2 gp120 binding to various transfectants and inhibition of binding to MCLRs with mannan. (b) CD4, DC-SIGN, DC-SIGNR, langerin and mock quail QT6 receptor transfectants (pcDNA3) were incubated with HIV-1 HXBc2 gp120 with or without prior exposure to mannan. (c) HIV-2 VCP gp120 binding to CXCR4, DC-SIGN, DC-SIGNR, langerin and mock quail QT6 receptor transfectants with or without preincubation with mannan. VCP, a CD4-independent HIV-2 gp12050, can bind directly to CXCR4 (unpublished data).
For comparison with LCs, MDLCs were produced from monocytes under identical conditions to MDDCs with the additional incubation of MDDCs with TGF-β. We found that in vitro–derived MDLCs also expressed langerin but, unlike immature LCs, some residual expression of the MCLRs MR and DC-SIGN was also observed (Fig. 4cB). Binding of gp120 was also substantially lower in MDLCs than LCs (Fig. 4c,d). Therefore, with respect to MCLR expression, MDLCs are incomplete in vitro models of immature LCs in vivo.
DC-SIGN is expressed on dermal cells in tissue sections24. We confirmed this with freshly isolated skin DCs, but found that DC-SIGN expression was restricted to the CD1alo CD14 subset (Fig. 5b and Table 1). DC-SIGN was not detected on the CD1ahi dermal DCs or on the LC population (which also expresses high amounts of CD1a) (Fig. 5a,b and Table 1). In contrast, the MR was expressed on both CD1ahi and CD1alo subsets, although CD1ahi DCs expressed the highest amounts (Fig. 5b and Table 1). The pattern of MR expression correlated well with the pattern of gp120 binding to the dermal DC subsets, with the CD1ahi population showing higher amounts of gp120 binding (Figs. 4e,f and 5b). However, there was a small subpopulation of CD1alo CD14+ dermal DCs that also bound high amounts of gp120, and this correlated with coexpression of both DC-SIGN and MR (Figs. 4f and 5b). Like langerin, specific binding of gp120 to the MR-transfected Rat-6 cell line confirmed the ability of this MCLR to bind HIV gp120 and that this binding could be inhibited by mannan (Fig. 6a). Thus, binding of gp120 to dermal DCs correlates with both DC-SIGN and MR expression, and the expression of these attachment factors varies between the two DC subsets.
We next compared dermal DCs to MDDCs because previous investigations have suggested that the closest in vivo counterpart to MDDCs are dermal DCs25. However, we found that in contrast to the CD1ahi and CDlalo dermal DC subsets, MDDCs showed a relatively homogeneous phenotype with high DC-SIGN and MR expression (Fig. 4aB,bB). High expression of MR on MDDCs is consistent with the failure of anti–DC-SIGN to completely prevent binding of gp120 to these cells. Nevertheless we did observe heterogeneity of gp120 binding between MDDC preparations from different donors. In a relatively low gp120-binding MDDC phenotype, we observed low CD4 and MR expression but high DC-SIGN expression. In contrast, a high gp120-binding MDDC phenotype showed twofold greater CD4 and MR expression, although DC-SIGN expression was similar to the low gp120-binding phenotype (Fig. 4aB,bB). Hence the repertoire of MCLRs expressed on MDDCs in vitro most closely resembles the minor CD1aloCD14+ dermal DC subset.
gp120 binding to MCLRs on tissue DC migrants
As it has been proposed that migratory DCs transport HIV from distal mucosal sites to more proximal secondary lymphoid organs, we monitored gp120 binding and MCLR expression on dermal DCs that emigrated from skin explants. We found that emigration and maturation of dermal DCs resulted in a rapid down-regulation of both DC-SIGN and MR to almost undetectable amounts (Fig. 5b). This observation was independently confirmed when low levels of DC-SIGN and MR mRNA transcripts were demonstrated in sorted 24-h HLA-DRhi dermal emigrants (data not shown). Down-regulation of both MCLRs correlated with a lower amount of gp120 binding and with an increasing dependence on CD4 for gp120 binding (Figs. 3a,b and 5b,d). In addition, the switch from predominant MCLR to CD4–gp120-binding corresponded to increasing gp120 binding via CD4 and increasing CD4 expression on the emigrant populations (Fig. 5d). CD4 expression on dermal T cells also correlated well with gp120 binding and acted as an internal positive control (Fig. 5c).
In situ expression of MCLRs
Individual MCLR expression by skin DCs isolated from dissociated tissue was compared, by immunofluorescent staining and confocal microscopy, with in situ expression of the MCLRs in tissue sections (Fig. 7). Both MR and DC-SIGN expression was restricted to dermal cells (Fig. 7b,c). However langerin expression was restricted to epidermal LCs in a typical dendritiform distribution and extended to the most superficial layers of the epidermis (Fig. 7a). MR expression was consistently more abundant than DC-SIGN staining, and this was consistent with expression by both dermal DC subsets and tissue macrophages (in serial sections, 469 ± 228 MR+ and 239 ± 113 DC-SIGN+ cells were identified, respectively, per mm2). Thus, the DC MCLR expression revealed by direct immunohistochemistry correlated with that observed on DCs isolated by enzymatic digestion of the epidermis and dermis.
Cryostat sections of skin were stained with primary mAbs, then washed and stained with goat anti–mouse IgG. Cellular nuclei were detected by propidium iodide after immunofluorescent staining. Representative samples are shown. (a) Langerin staining on epidermal LCs. Arrows indicate langerin staining on LC cytoplasmic processes. (b) MR staining on dermal cells. (c) DC-SIGN staining on dermal cells. Arrows indicate representative MR+ and DC-SIGN+ cells. (a–c) Magnification: × 200. (a) Inset are magnified a further × 4.
Inhibition of HIV entry by mannan or anti-CD4
Inhibition of gp120 binding with mannan or anti-CD4 (mAb Leu3a) identified the predominant receptors for soluble gp120 binding to DCs. As gp120 binding may not fully represent the binding of infectious HIV, it was essential to observe the effects of these inhibitors on binding and entry of infectious HIV. We determined this directly by analysis of HIV entry 24 h after viral inoculation using qualitative polymerase chain reaction (PCR) analysis specific for complete HIV reverse transcripts (Fig. 8). Immature MDDC and blood DC subsets (CD11c+CD123− or CD11c−CD123+) were chosen as easily available representatives of the two classes for MCLR- and CD4-dependent binding, respectively. In MDDCs, mannan and anti-CD4 were equivalent in inhibiting the accumulation of full-length HIV transcripts (Fig. 8c). In contrast, blocking of MCLR on blood DCs by mannan had no effect on HIV DNA, whereas saturating amounts of anti-CD4 almost completely inhibited entry and reverse transcription (Fig. 8a,b). Therefore, on blood DCs, both gp120 binding and HIV entry and infection are mediated by CD4 alone. In MDDCs, MCLRs are crucial for both gp120 binding and HIV infection, but the role played by CD4 is more prominent in the latter.
CD11c+ blood DCs (a), CD11c− blood DCs (b) or MDDCs (c) were either treated with anti-CD4 (CD4 block) or mannan (CLR block). Cells were next infected with an identical stock of DNase-treated HIV-1 strain AD8 for 2 h, then washed and cultured for 24 h. Cells were collected and subjected to quantitative real-time PCR to quantify HIV-1 proviral DNA (gag) and cell numbers by cellular CCR5 DNA. HIV gag copies per CCR5 DNA copies = HIV DNA copies × cell−1. The amount of HIV DNA copies per cell type were standardized to 100%. The 100% amounts were (a) CD123 blood DCs = 8347 copies/106 cells; (b) CD11c blood DCs = 1725 copies/106 cells; (c) MDDCs = 13610 copies/106 cells. Data are representative of three separate experiments with cells from different blood donors.
Discussion
Interactions of HIV with DCs have been studied mostly with DCs generated in vitro. However, blood, skin and lymphoid tissue contain multiple DC subsets26, and these may differ in their ability to take up HIV or become infected16,17. In characterizing HIV-1 and gp120 binding by DC subsets we found marked differences in the mechanisms of HIV binding. Two groups of DC subsets were defined by the predominant receptors used to bind gp120. Blood and tonsil DCs, whether within the myeloid (CD11c+) or plasmacytoid (CD11c−CD123+) subsets, bound gp120 almost exclusively via CD4. In contrast, uncultured or immature skin DCs bound gp120 predominantly via MCLRs, with CD4 playing only a minor role. When these DCs migrated out of skin, this pattern of binding changed from predominantly MCLR- to CD4-dependent. Rapid down-regulation of these antigen-binding receptors during maturation and migration was consistent with the paradigm of DC specialization for antigen capture and processing in the periphery, but presentation of antigen and stimulation of T cells in the lymph node1,27,28. Although MCLRs were mainly responsible for gp120 binding in immature DCs, no one MCLR was expressed on all DC subsets. We identified MR, DC-SIGN and langerin as the predominant MCLRs expressed on different DCs or LCs and, using transfected cells, independently confirmed that HIV gp120 can bind to these MCLRs.
The ability of HIV to efficiently interact with LCs and our finding that langerin, the MCLR that is highly expressed on LCs, avidly binds the HIV env protein is of particular importance because LCs are restricted to the epidermis and may be the first leukocytes encountered in squamous epithelium and infected by HIV during sexual transmission5,6,7. Several lines of evidence support the idea that langerin plays a key role in the ability of LCs to interact with HIV. First, langerin is expressed on LCs and appears to be restricted or largely restricted to epidermal LCs21. Second, we found that HIV gp120 binding to LCs correlated with langerin expression on the freshly isolated DCs. Third, gp120 binding to LCs could be inhibited by mannan, which implicates one or more MCLRs as the primary attachment factor. Fourth, langerin expressed on cell lines efficiently binds gp120 and could not be inhibited by mannan. Fifth, LCs did not express DC-SIGN, in agreement with published data24, nor did they express MR, which also binds gp120. A trypsin-resistant receptor has previously been shown to be responsible for gp120 uptake in LCs14, and gp120 exposure induces the formation of Birbeck granules at the plasma membrane29. It is not likely that HIV-1 langerin-mediated binding to dermal DCs occurs because we did not observe langerin expression on immature or on 24-h emigrant dermal DC populations. In our immunohistochemical studies, langerin was restricted to epidermal sections, which was consistent with published observations21.
The importance of langerin and MR in binding gp120 on LCs and dermal DCs, respectively, requires further definition. Just as DC-SIGN is not the only attachment factor for HIV on immature MDDCs, gp120 binding to LCs may depend on other unidentified MCLRs. Loss of MCLR-dependent gp120 binding by emigrating mature LCs, despite continued langerin expression, supports this view. The development of specific inhibitors will be required to fully characterize the role that langerin plays in viral interactions in vivo. In addition to langerin, MR can efficiently bind gp120 when expressed in cell lines. Its pattern of expression on dermal DCs suggests that it may be the principal viral attachment protein on these cells, but identification of its potential role in HIV transmission will require the development of effective and specific blocking ligands or mAbs.
It was thought that DC-SIGN mediates DC capture and transmission of HIV to susceptible target cells15. Although this may be true in DC-SIGN transfectants and certain MDDCs in vitro, we have demonstrated the involvement of multiple viral attachment factors in vivo. In general, we found that binding of gp120 to immature skin DCs was inhibited by mannan, thus implicating one or more MCLRs. However, MCLR expression varied markedly between DC subsets. A diverse range of real or potential CLRs have been described on DCs17, but it is not known whether these interact efficiently with HIV env, in the same way as DC-SIGN, DC-SIGNR, MR and langerin. In addition, whether these receptors are expressed at sufficient amounts to function as viral attachment factors in vivo remains to be determined. This could be important because relatively high amounts of transfected DC-SIGN are needed to mediate efficient virus binding, even though DC-SIGN binds to env with high affinity30.
The pattern of cellular expression of DC-SIGN is somewhat controversial17,24,31,32,33,34. Termed “DC-specific”24, DC-SIGN is also expressed on brain microvascular endothelial cells35, certain tissue macrophages, can be induced on monocyte-derived macrophages under certain conditions17,31,34 and can even be found on rare CD14+ cells, resembling monocytes in blood (unpublished observations). In addition, it is clear that DC-SIGN is not a pan-DC marker because we found that its expression was restricted to a subset of CD14+ dermal DCs in our study of five tissue DC subsets. These findings also directly support histological findings in skin33.
The MR is now shown to be expressed on immature dermal DCs, but its expression on in vivo blood DCs is not generally accepted. Well characterized and stringently sorted lineage-negative CD11c+CD123− and CD11c−CD123+ blood DCs did not express MR on either subset36,37,38, which is consistent with our observations. Although there may be a rare MR+ leukocyte in blood, it is unclear whether this can be classified functionally as a DC.
The ability of DCs to efficiently initiate HIV-1 infection in T cells results from their specializations for antigen uptake and as potent costimulators for CD4+ T cells. DCs efficiently capture HIV and can transmit virus to adjoining CD4+ T cells after antigen-specific activation. There has been some disagreement about the relative contribution of “trans-infection” mediated by HIV bound to DCs and DC infection required before transfer to CD4+ T cells2,6,11,12,13,39,40. DC-SIGN is particularly adept at HIV binding and transfer from certain MDDCs preparations and some other cell lines to T lymphocytes in vitro15, especially at high cellular concentrations of DC-SIGN. Therefore the observation of low and/or lack of DC-SIGN expression on freshly isolated DCs and DCs 24 h after emigration from the skin is not consistent with current DC-SIGN–mediated HIV-transfer models. In addition, the cultured blood DCs and emigrant skin DCs initially used in HIV-1 transfer experiments do not express DC-SIGN or other MCLRs2,16,41.
This proposed “trans-infection” mechanism of retention and carriage of HIV before transfer to T lymphocytes and to the draining lymph node may be more complicated in vivo because the cells expressing MCLR are also potent antigen-processing cells27. It is likely that HIV is internalized via MCLR before emigration and maturation, especially as antigen uptake and processing is enhanced by DEC20542 and by the MCLRs MR28 and DC-SIGN43. It seems unlikely that the mechanism of long-term carriage found in vitro with transfected cells15 will exist in potent antigen-processing cells that express MCLR. Internalization of HIV after fusion with the DC membrane via CD4 and CCR5 is supported by the selection of R5 HIV variants observed in initial HIV infection in vivo and in studies that infect skin DCs in situ, either in skin blisters or abraded skin5,6. Binding, internalization and transfer by MCLRs without subsequent fusion via CD4-CCR5 would not select R5 strains from mixed infection with R5 and X4 strains in vitro or in vivo.
The presence of an array of attachment factors on different DC subsets could favor enhancement of infection by cis mechanisms31. Indeed, DC-SIGN can enhance infection of CD4+ and CCR5+ cells, particularly when CD4 or coreceptor expression is limiting. This is because high-affinity mechanisms for HIV capture on DCs will increase the probability of CD4-CCR5 binding and subsequent virus entry31. In MDDCs, we observed efficient blocking of infectious HIV entry into DCs by both mannan and anti-CD4. The more effective blocking by anti-CD4 compared to soluble gp120 binding is probably due to the initial high-affinity binding of C type lectins to HIV gp120 and then cis transfer to the CD4-CCR5–mediated fusion mechanism31. The latter only operates for whole virus and is permissive to inhibition at two stages: CLR binding inhibited by mannan and CD4 binding inhibited by anti-CD4. Conversely, predominant inhibition of soluble gp120 binding by mannan reflects the absence of CD4-CCR5–mediated fusion, but demonstrates the key role played by MCLRs in the initial concentration of HIV on the DC membrane, particularly in skin DCs where CD4 is expressed at lower concentrations. These data suggest efficient entry into skin DCs requires initial binding to an attachment factor such as DC-SIGN, langerin or MR.
Our HIV studies may have also elucidated a more fundamental property of epithelial DCs. In contrast to blood, tonsil and emigrating DCs, the diverse and extensive expression of MCLRs on immature LCs and dermal DCs may be a specialized adaptation that allows binding of oligosaccharides from a diverse array of microbial pathogens invading the epithelia. HIV is able to bind to these DC subsets via the abundant oligosaccharide gp120 and uses this specialized adaptation for fusion and transport within DCs to the draining lymph node.
In summary, HIV gp120 binds predominantly to MCLRs in skin DCs, probably langerin and other species in epidermal LCs and MR or MR–DC-SIGN in the two dermal DC subsets. Emigration and maturation of these DCs from cultured skin explants leads to a switch from predominantly binding via MCLRs to binding via CD4, which is similar to the exclusive binding via CD4 in tonsil and blood DCs (which do not express MCLRs). Similarly, infectious HIV enters blood DCs exclusively via the CD4-CCR pathway but both MCLRs and CD4 mediate such entry into MCLRs expressing MDDCs. The relative importance of these MCLRs and the definition of other receptors, particularly on LCs, requires further work. In addition, their roles in determining the route of intracellular trafficking should be examined. The diversity of MCLRs that we have demonstrated to mediate HIV binding and internalization and infection of DCs in anogenital skin and mucosa suggests that a combination of antiretroviral agents incorporating these new targets may be required to prevent sexual transmission of HIV.
Methods
Generation and culture of MDDCs.
Monocytes were purified and converted to immature and mature MDDCs as described16. To generate MDLCs, 10 ng/ml of TGF-β1 (R&D Systems, Minneapolis, MN) was included as well as interleukin 4 and granulocyte-macrophage colony-stimulating factor. MDLC differentiation was assessed by the expression of the LC markers E-cadherin (clone 36, BD Transduction Laboratories, San Diego, CA) and langerin (clone DCGM4, Immunotech, Marseille, France).
Isolation and culture of blood and tonsil DCs.
Tonsils were obtained with methods approved by the Melbourne University and the Royal Children's Hospital Research ethics committee. Tonsil tissue was dissociated as described44. Cells were sorted according to density with countercurrent elutriation as described16. Crossover elutriator fractions (equivalent proportions of lymphocyte-monocyte populations, as determined by forward scatter–side scatter) were subjected to lineage cell depletion by successive magnetic and flow cytometric sorting under identical conditions to blood DCs as described16.
Isolation of skin-derived DCs.
Skin was obtained by methods approved by the Melbourne University and the Mercy Hospital Research ethics committee (Mercy Hospital, Melbourne, Victoria, Australia). Split skin explants were incubated in 2.5 mg/ml of dispase II (Roche Biochemicals, Basel, Switzerland) in RPMI-1640 at 4 °C for a minimum of 6 h and subsequently split into epidermal and dermal sections. Epidermal and dermal sheets were cultured in RF-10 (0.5 cm2 of skin/ml of media).
Generation of intact binding epitopes.
Tissue was cut into small sections with a sterile scalpel blade and resuspended in 2.5 mg/ml of collagenase F (Sigma, St. Louis, MI) + 50 μg/ml of DNase in sterile RPMI-1640 supplemented with 5% (v/v) fetal calf serum (FCS). Cells were rocked for 1 h at room temperature, then manually disrupted with a sterile glass Pasteur pipette. Cells were passed over a Ficoll-Paque gradient (Pharmacia-Biotech, Uppsala, Sweden). LCs were labeled with fluorescein isothiocyanate (FITC)–anti-CD1a (Pharmingen, San Diego CA), followed by goat anti-mouse magnetic microbeads (Miltenyi Biotech, Auburn, CA). LCs were enriched to 8% from single cell epidermal suspensions after magnetic sorting and ∼3 × 105 cells at a purity of > 95% were obtained after fluorescent sorting with a MoFlo cell sorter (Cytomation, Fort Collins, CO). Isolation of fresh dermal DCs was done with collagenase as described22. A large number of cells were CD45− and excluded from the analysis by CD45 gating22.
Isolation of emigrant skin–derived DCs.
DCs were also isolated as migratory cells after culture of whole dermal and epidermal skin sheets as described19,22.
Plasmids, cell lines and vaccinia viruses.
HIV-1 HXBc2 and HIV-2/vcp plasmids expressing gp120 under a vaccinia synthetic early-late promoter45 and plasmids expressing CD4 and CXCR446 and DC-SIGN and DC-SIGNR30,47 were used (unpublished data). The langerin coding sequence was amplified from lymph node RNA with a commercially available kit (SuperScript One-Step RT-PCR, Invitrogen, Carlsbad, CA) and primers p5LR (5′-CCGGATCCAGGATGACTGTGGAGAAGGAGGCCCCTGATGCG-3′) and p3LR-AU1 (5′-GGCTCGAGTTATATGTATCTGTAGGTGTCCGGTTCTGATGGGACATAGG-3′) (underlined sequences denote BamHI and XhoI restriction sites, respectively). The PCR product was cloned into pcDNA3 (Invitrogen) with BamHI and XhoI restriction sites. Sequence analysis confirmed that the encoded amino acid sequence was identical to GenBank sequence NM_015717. Primer p3LR-AU1 introduced a COOH-terminal AU-1 antigenic tag, which allowed detection of langerin surface expression by FACS. The MR-transfected Rat-6 cell line has been described48.
Production of HIV gp120 proteins.
Human 293T cells were infected for 1 h at 37 °C with vaccinia virus strain WR at a multiplicity of infection of ten. Infected cells were then calcium phosphate–transfected with the HXBc2 or VCP gp120 expression plasmids for 4 h. After transfection, the medium was replaced with DMEM-10 containing 100 μg/ml of rifampicin (DMEM-10-R). After overnight expression at 37 °C, medium containing gp120 was clarified by low-speed centrifugation for 10 min.
HIV gp120 labeling and binding on fresh and cultured DC.
Because of the complexity of dissociated tissue suspensions and rarity of DC populations, flow cytometry with biotinylated HIV gp120 was used in DC binding studies. HIV-1 isolate envelope BaL gp120 (AIDS Reagent Program) was biotinylated as described16. Inhibition studies, HIV gp120 detection and percentage HIV gp120 calculations were as described16.
Receptor binding assays on MCLR-transfected cell types.
QT6 quail receptor cells were generated by infecting with vTF1.1, transfecting with T7 promoted receptor plasmids and expressing overnight at 37 °C in DMEM-10-R. Cells were resuspended in 200 μl of gp120 containing supernatant in the presence or absence of 100 μg/ml of mannan (Sigma) or 100 mg/ml of anti-langerin (mAb DCGM4). At 4 °C cells were washed with PBS and lysed with 1% (v/v) NP-40, 150 mM NaCl, 50 mM Tris at pH 8.0 and a complete protease inhibitor mixture (Roche Molecular Biochemicals). Lysates were then immunoblotted for bound gp120 with rabbit sera 116946 for HXBc2 or mAb DA6 for VCP.
Flow cytometric analysis.
Cells were labeled with primary murine mAbs as described16. Antibodies used were: phycoerythrin (PE)-IgG1, FITC-IgG1, FITC-CD3, IgG1, PE-CD14, PE-CD11c, PE-CD123, PE-CD4 (Leu3a), pure Leu3a mAb, FITC–goat anti-mouse, PE–goat anti-mouse (Becton Dickinson, San Jose, CA), FITC-CD1a, MR (clone 19), allophycocyanin-CD45, cychrome–HLA-DR (Pharmingen), PE-IgG2b, PE–DC-SIGN1 (R&D Systems, Minneapolis, MN), PE-MR (clone 3.29), langerin (clone DCGM4, Immunotech), anti–DC-SIGN (clone 28, from the AIDS Reagent Program) were used.
Immunohistology.
Cryostat skin sections (10 μm) were cut from Tissue-Tek OCT, mounted onto poly(L)lysine–coated glass slides and stored at −80 °C (Miles, Elkhart, IN). Slides were stained with 5 μg/ml of primary antibodies (unless otherwise stated) for 40 min at room temperature, washed three times with 1% bovine serum albumin (w/v) in PBS, and primary antibodies were detected by incubation with 5 μg/ml of Alexa 488–conjugated goat anti–mouse IgG for 40 min at room temperature (Molecular Probes, Eugene, OR). Nuclear staining was done with 150 ηg/ml propidium iodide (Molecular Probes) and mounted with fluorescent mounting medium (DAKO, Carpinteria, CA) before acquisition with a Zeiss Axioplan 2 confocal microscope at × 200 magnification.
HIV-1 infection and blocking.
For inhibition studies, DCs were preincubated with either 10 μg/ml of mAb Leu3a or 5 mg/ml of mannan for 40 min at 4 °C. Equal number of DCs (1 × 105) were sorted with a MoFlo and infected with 150 μl of HIV AD8 viral supernatant (TCID50 = 3.05 × 107/ml) that had been treated with RNAse-free DNAse for 30 min at 37 °C (Roche Biochemicals). After 2 h of infection, cells were washed three times with 1% (v/v) human sera, 2 mM EDTA in 1 × PBS and resuspended in 200 μl of RPMI 1640 with 10% FCS. Immediately after infection and after designated culture times, the DCs were washed and lysed as described6 for quantitative PCR analysis.
Quantitative PCR.
Real-time PCR was done with molecular beacons as described49. HIV-1 primers—SL19 5′-TCTCTAGCAGTGGCGCCCGAACA-3′, SL20 5′-TCTCCTTCTAGCCTCCGCTAGTC-3′–and the matching molecular beacon—5′-FAM-CGGGAGTACTCACCAGTCGCCGCCCCTCGCCCTCCCG-DABCYL-3′—that cross the primer binding site and LTR detect full-length provirus. Primers for CCR5—LK46 5′-GCTGTGTTTGCGTCTCTCCCAGGA-3′, LK47 5′-CTCACAGCCCTGTGCCTCTTCTTC-3′— and the molecular beacon recognizing the sequence 5′-GAGAACGGTGAATGAAGAGCAGACAG-3′ were used to quantify genomic copies. Amplifications were done with a Perkin Elmer 7700 (Perkin Elmer, Branchburg, NJ). HIV copy numbers were used to calculate the percentage of HIV entry and entry inhibition and therefore inhibition is defined as:

Accession codes
References
Banchereau, J. & Steinman, R.M. Dendritic cells and the control of immunity. Nature 392, 245–252 (1998).
Cameron, P.U. et al. Dendritic cells exposed to human immunodeficiency virus type-1 transmit a vigorous cytopathic infection to CD4+ T cells. Science 257, 383–387 (1992).
Pope, M. et al. Conjugates of dendritic cells and memory T lymphocytes from skin facilitate productive infection with HIV-1. Cell 78, 389–398 (1994).
Pinchuk, L.M., Polacino, P.S., Agy, M.B., Klaus, S.J. & Clark, E.A. The role of CD40 and CD80 accessory cell molecules in dendritic cell-dependent HIV-1 infection. Immunity 1, 317–325 (1994).
Kawamura, T. et al. Candidate microbicides block HIV-1 infection of human immature langerhans cells within epithelial tissue explants. J. Exp. Med. 192, 1491–1500 (2000).
Reece, J.C. et al. HIV-1 selection by epidermal dendritic cells during transmission across human skin. J. Exp. Med. 187, 1623–1631 (1998).
Hu, J., Gardner, M.B. & Miller, C.J. Simian immunodeficiency virus rapidly penetrates the cervicovaginal mucosa after intravaginal inoculation and infects intraepithelial dendritic cells. J. Virol. 74, 6087–6095 (2000).
Spira, A.I. et al. Cellular targets of infection and route of viral dissemination after an intravaginal inoculation of simian immunodeficiency virus into rhesus macaques. J. Exp. Med. 183, 215–225 (1996).
Zhang, Z. et al. Sexual transmission and propagation of SIV and HIV in resting and activated CD4+ T cells. Science 286, 1353–1357 (1999).
Stahl-Hennig, C. et al. Rapid infection of oral mucosal-associated lymphoid tissue with simian immunodeficiency virus. Science 285, 1261–1265 (1999).
Masurier, C. et al. Dendritic cells route human immunodeficiency virus to lymph nodes after vaginal or intravenous administration to mice. J. Virol. 72, 7822–7829 (1998).
Berger, E.A. et al. A new classification for HIV-1. Nature 391, 240 (1998).
Blauvelt, A. et al. Productive infection of dendritic cells by HIV-1 and their ability to capture virus are mediated through separate pathways. J. Clin. Invest. 100, 2043–2053 (1997).
Dezutter-Dambuyant, C. et al. Interaction of human epidermal Langerhans cells with HIV-1 viral envelope proteins (gp 120 and gp 160s) involves a receptor-mediated endocytosis independent of the CD4 T4A epitope. J. Dermatol. 18, 377–392 (1991).
Geijtenbeek, T.B. et al. DC-SIGN, a dendritic cell-specific HIV-1-binding protein that enhances trans-infection of T cells. Cell 100, 587–597 (2000).
Turville, S.G. et al. HIV gp120 receptors on human dendritic cells. Blood 98, 2482–2488 (2001).
Turville, S.G. et al. Bitter-sweet symphony: defining the role of dendritic cell gp120 receptors in HIV infection. J. Clin. Virol. 22, 229–239 (2001).
Curtis, B.M., Scharnowske, S. & Watson, A.J. Sequence and expression of a membrane-associated C-type lectin that exhibits CD4-independent binding of human immunodeficiency virus envelope glycoprotein gp120. Proc. Natl. Acad. Sci. USA 89, 8356–8360 (1992).
Lenz, A., Heine, M., Schuler, G. & Romani, N. Human and murine dermis contain dendritic cells. Isolation by means of a novel method and phenotypical and functional characterization. J. Clin. Invest. 92, 2587–2596 (1993).
Nestle, F.O., Zheng, X.G., Thompson, C.B., Turka, L.A. & Nickoloff, B.J. Characterization of dermal dendritic cells obtained from normal human skin reveals phenotypic and functionally distinctive subsets. J. Immunol. 151, 6535–6545 (1993).
Valladeau, J. et al. Langerin, a novel C-type lectin specific to Langerhans cells, is an endocytic receptor that induces the formation of Birbeck granules. Immunity 12, 71–81 (2000).
McLellan, A.D., Heiser, A., Sorg, R.V., Fearnley, D.B. & Hart, D.N. Dermal dendritic cells associated with T lymphocytes in normal human skin display an activated phenotype. J. Invest. Dermatol. 111, 841–849 (1998).
Hladik, F. et al. Dendritic cell-T-cell interactions support coreceptor-independent human immunodeficiency virus type 1 transmission in the human genital tract. J. Virol. 73, 5833–5842 (1999).
Geijtenbeek, T.B. et al. Identification of DC-SIGN, a novel dendritic cell-specific ICAM-3 receptor that supports primary immune responses. Cell. 100, 575–585 (2000).
Grassi, F. et al. Monocyte-derived dendritic cells have a phenotype comparable to that of dermal dendritic cells and display ultrastructural granules distinct from Birbeck granules. J. Leukoc. Biol. 64, 484–493 (1998).
Hart, D.N. Dendritic cells: unique leukocyte populations which control the primary immune response. Blood 90, 3245–3287 (1997).
Romani, N. et al. Presentation of exogenous protein antigens by dendritic cells to T cell clones. Intact protein is presented best by immature, epidermal Langerhans cells. J. Exp. Med. 169, 1169–1178 (1989).
Sallusto, F., Cella, M., Danieli, C. & Lanzavecchia, A. Dendritic cells use macropinocytosis and the mannose receptor to concentrate macromolecules in the major histocompatibility complex class II compartment: downregulation by cytokines and bacterial products. J. Exp. Med. 182, 389–400 (1995).
Dezutter-Dambuyant, C. In vivo and in vitro infection of human Langerhans cells by HIV-1. Adv. Exp. Med. Biol. 378, 447–451 (1995).
Pohlmann, S. et al. DC-SIGN interactions with human immunodeficiency virus type 1 and 2 and simian immunodeficiency virus. J. Virol. 75, 4664–4672 (2001).
Lee, B. et al. cis Expression of DC-SIGN allows for more efficient entry of human and simian immunodeficiency viruses via CD4 and a coreceptor. J. Virol. 75, 12028–12038 (2001).
Soilleux, E.J., Barten, R. & Trowsdale, J. DC-SIGN; a related gene, DC-SIGNR; and CD23 form a cluster on 19p13. J. Immunol. 165, 2937–2942 (2000).
Soilleux, E.J. & Coleman, N. Langerhans cells and the cells of Langerhans cell histiocytosis do not express DC-SIGN. Blood 98, 1987–1988 (2001).
Soilleux, E.J. et al. Constitutive and induced expression of DC-SIGN on dendritic cell and macrophage subpopulations in situ and in vitro. J. Leukoc. Biol. 71, 445–457 (2002).
Mukhtar, M. et al. Primary isolated human brain microvascular endothelial cells express diverse HIV/SIV-associated chemokine coreceptors and DC-SIGN and L-SIGN. Virology 297, 78–88 (2002).
Kato, M. et al. Expression of multilectin receptors and comparative FITC-dextran uptake by human dendritic cells. Int. Immunol. 12, 1511–1519 (2000).
MacDonald, K.P.A. et al. Peripheral blood dendritic cell heterogeneity. Blood doi:10:1182/blood-2002-11-0097 (in the press, 2002).
MacDonald, K.P.A., Munster, D.J., Clark, G.J., Vuckovic, S. & Hart, D.N.J. in Leucocyte Typing VII (ed. Mason, D.) edn. 7 (Oxford University Press, Oxford, 2002).
Cameron, P., Pope, M., Granelli-Piperno, A. & Steinman, R.M. Dendritic cells and the replication of HIV-1. J. Leukoc. Biol. 59, 158–171 (1996).
Granelli-Piperno, A., Finkel, V., Delgado, E. & Steinman, R.M. Virus replication begins in dendritic cells during the transmission of HIV-1 from mature dendritic cells to T cells. Curr. Biol. 9, 21–29 (1999).
Pope, M., Gezelter, S., Gallo, N., Hoffman, L. & Steinman, R.M. Low levels of HIV-1 infection in cutaneous dendritic cells promote extensive viral replication upon binding to memory CD4+ T cells. J. Exp. Med. 182, 2045–2056 (1995).
Mahnke, K. et al. The dendritic cell receptor for endocytosis, DEC-205, can recycle and enhance antigen presentation via major histocompatibility complex class II-positive lysosomal compartments. J. Cell. Biol. 151, 673–684 (2000).
Engering, A. et al. The dendritic cell-specific adhesion receptor DC-SIGN internalizes antigen for presentation to T cells. J. Immunol. 168, 2118–2126 (2002).
Stent, G. et al. Heterogeneity of freshly isolated human tonsil dendritic cells demonstrated by intracellular markers, phagocytosis, and membrane dye transfer. Cytometry 48, 167–176 (2002).
Chakrabarti, S., Sisler, J.R. & Moss, B. Compact, synthetic, vaccinia virus early/late promoter for protein expression. Biotechniques 23, 1094–1097 (1997).
Hoffman, T.L. et al. Stable exposure of the coreceptor-binding site in a CD4-independent HIV-1 envelope protein. Proc. Natl. Acad. Sci. USA 96, 6359–6364 (1999).
Pohlmann, S. et al. DC-SIGNR, a DC-SIGN homologue expressed in endothelial cells, binds to human and simian immunodeficiency viruses and activates infection in trans. Proc. Natl. Acad. Sci. USA 98, 2670–2675 (2001).
Taylor, M.E. & Drickamer, K. Structural requirements for high affinity binding of complex ligands by the macrophage mannose receptor. J. Biol. Chem. 268, 399–404 (1993).
Lewin, S.R. et al. Use of real-time PCR and molecular beacons to detect virus replication in human immunodeficiency virus type 1-infected individuals on prolonged effective antiretroviral therapy. J. Virol. 73, 6099–6103 (1999).
Endres, M.J. et al. CD4-independent infection by HIV-2 is mediated by fusin/CXCR4. Cell 87, 745–756 (1996).
Acknowledgements
Supported by the Australian National Centre for HIV Virology Research (A. L. C.); an Australian Postgraduate Award (to S. T.); an Australian National Health and Medical Research Council grant (to P. U. C.); an NIH MSTP grant (to P. U. C.); a Wellcome trust and ANZ trustees grant (to P. U. C.); the Deutsche Forschungsgemeinschaft (S. P.); NIH grants R0140880 and R0135383 (to R. D.); a Burroughs Wellcome Fund translational research award (to R. W. D.); and an Elizabeth Glaser Scientist award from the Pediatric AIDS Foundation (to R. W. D.). Thanks to R. Berkowicz for tonsils, the staff of the VPSU for normal skin, to M. Taylor and D. Hart for cells and reagents and C. Wolczak for processing the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Turville, S., Cameron, P., Handley, A. et al. Diversity of receptors binding HIV on dendritic cell subsets. Nat Immunol 3, 975–983 (2002). https://doi.org/10.1038/ni841
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ni841
This article is cited by
-
HIV transmitting mononuclear phagocytes; integrating the old and new
Mucosal Immunology (2022)
-
Human anogenital monocyte-derived dendritic cells and langerin+cDC2 are major HIV target cells
Nature Communications (2021)
-
Antiretroviral therapy partially improves the abnormalities of dendritic cells and lymphoid and myeloid regulatory populations in recently infected HIV patients
Scientific Reports (2019)
-
Breaking the Glyco-Code of HIV Persistence and Immunopathogenesis
Current HIV/AIDS Reports (2019)
-
Identification of Siglec-1 null individuals infected with HIV-1
Nature Communications (2016)