Abstract
Purpose. To evaluate the feasibility of using a serially passaged culture of human nasal epithelial cell monolayers on a permeable support for in vitro drug transport studies. The optimum conditions for passaged culture as well as the correlation between the transepithelial electrical resistance (TEER) value and drug permeability (Papp) were evaluated.
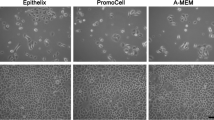
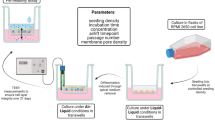
Methods. Fresh human nasal epithelial cells were collected from normal inferior turbinates and were subcultured repeatedly in serum-free bronchial epithelial cell growth media (BEGM) in petri dishes. The subcultured cells of each passage were seeded onto permeable supports at 5 × 105 cells/cm2 and grown in Dulbecco's modified Eagle medium (DMEM). Morphologic characteristics were observed by scanning electron microscopy (SEM). To verify the formation of tight junctions, actin staining and transmission electron microscopy (TEM) studies were conducted. In the drug transport study, [14C]mannitol and budesonide were selected as the paracellular and the transcellular route markers, respectively.
Results. Serially passaged cells were successfully cultured on a permeable support and showed significantly high TEER values up to passage 4. After 14 days of seeding, SEM showed microvilli, and protrusions of cilia and mucin granules were detected by TEM. The paracellular marker [14C]mannitol showed a nearly constant permeability coefficient (Papp) when the TEER value exceeded 500 Ω·cm2 regardless of the passage number. However, as expected, budesonide showed a higher permeability coefficient compared to [14C]mannitol and was less affected by the TEER value.
Conclusions. Human nasal epithelial cell monolayers were successfully subcultured on a permeable support up to passage 4. These cell culture methods may be useful in high-throughput screening of in vitro nasal transport studies of various drugs.
Similar content being viewed by others
References
E. Marttin, J. C. Verhoef, C. Cullander, S. G. Romeijn, and J. F. Nagelkerke. F. W. Merkus, Confocal laser scanning microscopic visualization of the transport of dextrans after nasal administration to rats: effects of absorption enhancers. Pharm. Res. 14:631-637 (1997).
S. J. Hersey and R. T. Jackson. Effect of bile salts on nasal permeability in vitro. J. Pharm. Sci. 76:876-879 (1987).
P. M. Reardon, C. H. Gochoco, K. L. Audus, G, Wilson, and P. L. Smith. In vitro nasal transport across ovine mucosa: Effects of ammonium glycyrrhizinate on electrical properties and permeability of growth hormone releasing peptidem, mannitol, and lucifer yellow. Pharm. Res. 10:553-561 (1993).
Y. Maitani, K. Ishigaki, K. Takayama, and T. Nagai. In vitro nasal transport across rabbit mucosa: effect of oxygen bubbling, pH and hypertonic pressure on permeability of lucifer yellow, diazepam and 17 β-estradiol. Int. J. Pharm. 146:11-19 (1997).
M. C. Schmidt, D. Simmen, M. Hilbe, P. Boderke, G. Ditzinger, J. Sandow, S. Lang, W. Rubas, and H. P. Merkle. Validation of excised bovine nasal mucosa as in vitro model to study drug transport and metabolic pathways in nasal epithelium. J. Pharm. Sci. 89:396-407 (2000).
C. Wadell, E. Bjork, and O. Camber. Nasal drug delivery–evaluation of an in vitro model using porcine nasal mucosa. Eur. J. Pharm. Sci. 7:197-206 (1999).
U. Werner and T. Kissel. Development of a human nasal cell culture model and its suitability for transport and metabolism studies under in vivo conditions. Pharm. Res. 12:565-571 (1995).
U. Werner and T. Kissel. In-vitro cell culture models of the nasal epithelium: a comparative histochemical investigation of their suitability for drug transport studies. Pharm. Res. 13:978-988 (1996).
D. Schmidt, U. Hubsch, H. Wurzer, W. Heppt, and M. Aufderheide. Development of an in vitro human nasal epithelial (HNE) cell model. Toxicol. Lett. 88:75-79 (1996).
M. C. Schmidt, H. Peter, S. R. Lang, G. Ditzinger, and H. P. Merkle. In vitro cell models to study nasal mucosal permeability and metabolism. Adv. Drug Deliv. Rev. 29:51-79 (1998).
T. Kissel and U. Werner. Nasal delivery of peptides: an in vitro cell culture model for the investigation of transport and metabolism in human nasal epithelium. J. Control. Release 53:195-203 (1998).
U. A. Remigius, J. Mark, W. Tom, A. Patrick, K. Renaat, and V. Norbert. In-vitro nasal drug delivery studies: comparison of derivatised, fibrillar and polymerized collagen matrix-based human nasal primary culture systems for nasal drug delivery studies. J. Pharm. Pharmacol. 53:1447-1456 (2001).
R. U. Agu, H. V. Dang, M. Jorissen, T. Willems, R. Kinget, and N. Verbeke. Nasal absorption enhancement strategies for therapeutic peptides: an in vitro study using cultured human nasal epithelium. Int. J. Pharm. 237:179-191 (2002).
H. V. Dang, R. U. Agu, M. Jorissen, T. Willems, R. Kinget, and N. Verbeke. Characterization of human nasal primary culture systems to investigate peptide metabolism. Int. J. Pharm. 238:247-256 (2002).
T. E. Gray, K. Guzman, C. W. Davis, L. H. Abdullah, and P. Nettesheim. Mucociliary differentiation of serially passaged normal human tracheobronchial epithelial cells. Am. J. Respir. Cell Mol. Biol. 14:104-112 (1996).
R. Wu, J. Yankaskas, E. Cheng, M. R. Knowles, J. T. Gatzy, and R. C. Boucher. Growth and differentiation of human nasal epithelial cells in culture. Am. Rev. Respir. Dis. 132:311-320 (1985).
D. P. Chopra, J. Sullivan, J. J. Wille, and K. M. Siddiqui. Propagation of differentiating normal human tracheobronchial epithelial cells in serum-free medium. J. Cell. Physiol. 130:173-181 (1987).
H. J. Roh, E. K. Goh, S. G. Wang, K. M. Chon, J. H. Yoon, and Y. S. Kim. Serially passaged normal human nasal epithelial cells: morphology and mucous secretory differentiation. Korean. J. Rhinol. 6:107-112 (1999).
D. J. Thornton, T. Gray, P. Nettesheim, M. Howard, J. S. Koo, and J. K. Sheehan. Characterization of mucins from cultured normal human tracheobronchial epithelial cells. Am. J. Physiol. Lung Cell. Mol. Physiol. 278:L1118-L1128 (2000).
E. K. Anderberg, T. Lindmark, P. Artursson, and S. Caprate. Dilatations in human intestinal tight junctions and enhances drug absorption by the paracellular route. Pharm. Res. 10:857-864 (1993).
L. A. Lapierre. The molecular structure of the tight junction. Adv. Drug Deliv. Rev. 41:255-264 (2000).
J. L. Madara, J. Stafford, D. Barenberg, and S. Carson. Functional coupling of tight junctions and microfilaments in T84 monolayers. Am. J. Physiol. 254:G416-G423 (1988).
C. Mattinger, T. Nyugen, D. Schafer, and K. Hormann. Evaluation of serum-free culture conditions for primary human nasal epithelial cells. Int. J. Hyg. Environ. Health 205:235-238 (2002).
C. S. Rhee, Y. G. Min, C. H. Lee, T. Y. Kwon, C. H. Lee, W. J. Yi, and K. S. Park. Ciliary beat frequency in cultured human nasal epithelial cells. Ann. Otol. Rhinol. Laryngol. 110:1011-1016 (2001).
N. R. Mathias and K. J. Kim. T. W. Robison., V. H. L. Lee. Development and characterization of rabbit tracheal epithelial cell monolayer models for drug transport studies. Pharm. Res. 12:1499-1505 (1995).
A. N. O. Dodoo, S. S. Balnsal, D. J. Barlow, F. Bennet, R. C. Hider, A. B. Lansley, M. J. Lawrence, and C. Marriott. Use of alveolar cell monolayers of varying electrical resistance to measure pulmonary peptide transport. J. Pharm. Sci. 89:223-231 (2000).
K. A. Foster, M. L. Avery, M. Yazdanian, and K. L. Audus. Characterization of the Calu-3 cell line as a tool to screen pulmonary drug delivery. Int. J. Pharm. 208:1-11 (2000).
J. C. Kidney and D. Proud. Neutrophil transmigration across human airway epithelial monolayers: mechanisms and dependence on electrical resistance. Am. J. Respir. Cell Mol. Biol. 23:389-395 (2000).
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Yoo, JW., Kim, YS., Lee, SH. et al. Serially Passaged Human Nasal Epithelial Cell Monolayer for in Vitro Drug Transport Studies. Pharm Res 20, 1690–1696 (2003). https://doi.org/10.1023/A:1026112107100
Issue Date:
DOI: https://doi.org/10.1023/A:1026112107100