Abstract
Introduction
The Cleveland-Cusco Connection (CCC) elective was created during the COVID-19 pandemic to continue global health (GH) education for Case Western Reserve University (CWRU) and Universidad Nacional de San Antonio Abad del Cusco (UNSAAC) medical students. The CCC elective was held over Zoom and aimed to promote international collaboration, knowledge about health systems, and perspectives in GH with synchronous and asynchronous learning.
Methods
Peruvian and US medical students participated in six monthly sessions consisting of student presentations and large and small group discussions. The elective was led collaboratively by CWRU and UNSAAC students. We evaluated students’ experience using pre- and post-course surveys.
Results
Nineteen students (76%) completed the post-course survey. The median rating for meeting each course objective was “somewhat effective” on a 5-point scale ranging from “very ineffective” to “very effective.” All respondents would recommend the course to a friend. Common barriers included language challenges, fatigue from other coursework, and technology issues. Seven students’ pre- and post-course surveys could be linked. The number of students who agreed with the statements assessing course objectives increased for all questions between the pre- and post-test, with only the number agreeing that they understood the Peruvian healthcare system increasing significantly (p < 0.05).
Discussion
The CCC elective provides a valuable GH educational opportunity via a virtual platform. Students reported that learning from their peers was effective and enjoyable.
Conclusion
Virtual GH electives like the CCC may offer benefits in terms of cost, equity, and flexibility and merit further investigation.
Similar content being viewed by others
Introduction
Global health is the study, research, and practice of medicine focused on improving health and achieving health equity for all persons worldwide [1]. In the modern era, health issues transcend borders and national governments, and it is paramount that healthcare professionals understand global issues to improve healthcare delivery worldwide. Global health education (GHE) has traditionally utilized various modalities, such as didactic lectures, workshops, and international field experiences, including clinical electives and mission trips [2,3,4]. There are several drawbacks to international field experiences, including the high costs of participating in overseas placements; estimated mission trip costs range from $12,600 to $84,000 per trip [2]. Students and physicians are responsible for many costs on these trips, which Rovers et al. estimated at $1764 and $2066, respectively, for a week-long trip to the Dominican Republic [3]. Additionally, international travel for global health (GH) experiences has raised ethical concerns. Short-term mission trips have been critiqued for disrupting or undermining existing health services, having underqualified volunteers practice beyond their training, not having sufficient pre-departure preparation, perpetuating a white savior mentality, and being unsustainable [4,5,6,7]. Travel is dependent on many unpredictable factors, such as political stability, security threats, natural disasters, and epidemics [8, 9]. The travel restrictions imposed by the COVID-19 pandemic have created an impetus for GH programs to develop, adapt, and incorporate virtual methods of GH education.
Virtual GHE offers several benefits to instructors and students. Not only does it provide flexibility and access to a wealth of online resources, but a virtual elective conducted synchronously via videoconferencing maintains the opportunity for collaborative, face-to-face peer interaction. Additionally, these virtual partnerships can be longitudinal and substantially less costly than short-term international trips [10, 11]. Studies have shown pedagogical support for e-learning in medical education and student preference for this method [12, 13].
While virtual partnerships in GH are gaining attention, these programs remain under-investigated. Previous virtual GH programs at medical schools have described curricula covering a variety of topics using different web-based applications and educational methods [14,15,16]. There is also curricular guidance laid out in the Virtual Education Partnership and Curricular Kit for transitioning GH education to virtual formats [17]. As the nature of these virtual GH partnerships is diverse, we aim to describe our unique peer-teaching-based virtual GH elective between US and Peruvian medical students based in Cleveland and Cusco.
The Peru Health Outreach Project (PHOP) is a student-run global health initiative at the Case Western Reserve University (CWRU) School of Medicine and the Cleveland Clinic Lerner College of Medicine of CWRU (CCLCM). Since 2009, an interdisciplinary team of students, healthcare professionals, and volunteers have planned and participated in 2-to-4-week health education trips to medically underserved areas in Peru with local partnerships. In 2018, PHOP established a partnership with the Universidad Nacional de San Antonio Abad del Cusco (UNSAAC), a medical school in Cusco. With the onset of the COVID-19 pandemic, the annual PHOP trip was canceled in 2020. In order to continue GHE and adapt to the constraints of the pandemic, the PHOP leadership designed the Cleveland-Cusco Connection (CCC) elective and built a longitudinal, student-led, virtual bidirectional GH partnership between the CWRU and UNSAAC medical schools. The goals of the elective were to promote medical foreign language skills, foster international collaboration, improve student knowledge about health systems, and broaden perspectives in GH. We aim to describe the structure and evaluation of this virtual elective to inform the development of future virtual GH partnerships.
Methods
Participants
The CCC elective was designed by CWRU and UNSAAC medical students and faculty members at CCLCM of CWRU. The course was open to first and second year CWRU medical students and UNSAAC medical students of all years. The course was limited to 30 participants in total to ensure robust small group discussions with limited faculty facilitators. There were no prerequisites, although we recommended that students have at least basic language skills in Spanish (for CWRU students) and English (for UNSAAC students). In addition to the faculty leaders of the course, residents, fellows, and attending physicians with backgrounds in GH were recruited to facilitate the small group discussions.
CCC Elective Structure
The CCC elective was held over Zoom and consisted of six monthly sessions, each lasting 1.5 h. Sessions were held in the evening to accommodate student and facilitators’ schedules. Before each session, students completed pre-readings, which consisted of peer-reviewed articles, newspaper articles, and videos or documentaries. Sessions began with student presentations providing background information on the session topic, followed by small group discussions in breakout rooms where students discussed prepared questions. There were approximately six students and one physician facilitator in each small group, which were crafted to ensure that a combination of CWRU and UNSAAC students with an equal representation of language abilities was in each group. We encouraged students to speak in both Spanish and English during small group discussions or have a group member translate verbally or using the Zoom chat function. After the small group sessions, students returned to the main Zoom room for a brief large group discussion and concluding points. Session topics included diabetes case discussion, the US and Peruvian healthcare systems, medical training and the healthcare workforce in the US and Peru, barriers to care, public health outreach programs, and the evolving COVID-19 pandemic.
A typical session consisted of short student presentations, and small group discussions, and concluded with a brief large group discussion/wrap-up. We structured the time in various ways during different sessions based on student feedback and faculty and student leaders’ ideas to improve interactivity; for some sessions, we did the entirety of the student presentations at the beginning, and for others, we interspersed presentations with small group discussions. We also incorporated different forms of collaboration, including having groups take notes about their discussions in a shared Google Doc so they could see what other groups discussed in real time, a method called “jigsaw learning” [18]. We sent out short, anonymous feedback forms after each session and adapted the session structure accordingly throughout the elective.
Each session was led by three to six student leaders, consisting of both UNSAAC and CWRU students, on a rotating basis to include all students. Session leaders participated in two meetings with CCC student and faculty leaders to prepare for the session. Student leaders used the preparatory meetings to decide on the session topics and discuss the session’s learning objectives, structure, pre-readings, introductory presentations, and discussion questions. Student leaders reviewed their presentations with the faculty leaders and received feedback during the second meeting.
Students were assigned two reflection assignments during the elective, one about their experiences working with people of different backgrounds, and a final reflection on what they would take away from the course. Students were given a month to complete each reflection, which were expected to be between 300 and 600 words long. A faculty leader of the course reviewed each reflection for completeness and provided a brief response to each student’s reflection. To receive credit for the elective, students were required to attend at least five of the six sessions, serve as a leader for one session, and complete the two writing assignments. Only CWRU students were eligible to receive credit due to administrative barriers; UNSAAC students received a certificate of completion.
Evaluation
The protocol was determined to meet the criteria for exemption by the CWRU Institutional Review Board. UNSAAC medical school does not have an IRB. At the beginning of the course, students were emailed a survey containing Likert scale questions about their understanding of US and Peruvian healthcare systems, public health programs, and barriers to healthcare. We asked students to rate their language ability using a simplified version of the Interagency Language Roundtable Scale [19], which included the following categories: (1) none; (2) understands simple words; (3) capable of using simple phrases; (4) able to have simple dialogue; (5) conversational and able to use conjugations, including past, present, and future; and (6) native fluency. All surveys and the consent information were provided in both English and Spanish languages and were voluntary, with statements indicating that surveys would not be identifiable and would not impact course credit. Students entered the first four letters of their favorite actor and color to create an identifier to link pre- and post-course surveys.
We sent out short, anonymous feedback forms after each session asking how well the session met the learning objectives, how comfortable students felt participating in the session, and their suggestions for improving future sessions. We sent out the survey link in the Zoom chat feature before the session ended and in an email after the session. Course leaders made continuous adjustments to the session structure based on this feedback throughout the year.
Immediately after the course ended, we sent an anonymous, voluntary survey assessing self-rated language proficiency and 5-point Likert scale questions measuring achievement of course objectives, with a scale ranging from “strongly disagree” or “very ineffective” to “strongly agree” or “very effective” (Appendix 1). The survey took approximately 10 min to complete, and we sent out several reminder emails for students to complete the survey. We asked for students’ assessment of additional goals of the course, any barriers they encountered, and their experience with the course. We included open-ended questions about the aspects of the course they found most and least valuable. For students whose pre- and post-course surveys could be linked by a unique identifier, we assessed changes in agreement by dichotomizing responses from 5-point Likert scale questions into “agree” or “neutral/disagree” and using McNemar’s test. We specified the level of significance to be p < 0.05. Descriptive statistics are reported for the post-course Likert scale questions, and selected qualitative responses are included. Analyses were conducted in Microsoft Excel and JMP Pro 15.1.0 statistical software (SAS Institute, Cary, NC).
Results
Forty-six students applied for the course, and the first 30 students to apply were enrolled in the elective. Of the 30 students who enrolled, 25 participated (83%). Reasons provided for dropping the course included being too busy and not having sufficient language skills. Nineteen students (76%) responded to the post-course survey, including 10 UNSAAC students and nine CWRU students. Eleven students (58%) identified as female, and eight students (42%) identified as male (Table 1).
There was a range of foreign language competencies among respondents. The majority of respondents reported that their language ability was limited to simple phrases (n = 4) or simple dialogue with complete sentences (n = 5), while six students reported having conversational skills. Three UNSAAC students self-identified as having native fluency in English. One CWRU student indicated that their Spanish competency was limited to understanding scattered words (Table 1).
Post-course Survey
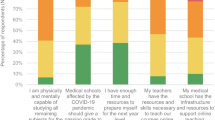
The median rating for each course objective was “somewhat effective” on the 5-point Likert scale from “very ineffective” to “very effective” (Fig. 1). The objective of “presenting and leading discussions about complex medical topics in an interactive virtual platform” received the largest number of “very effective” ratings (n = 8, 42%).
Effectiveness of course in meeting specific objectives. Participants responded to statements describing course objects using a five-point scale ranging from “very ineffective” to “very effective.” Dashed lines represent Case Western Reserve University respondents (N = 9), solid fill indicates Universidad Nacional de San Antonio Abad del Cusco respondents (N = 10)
Regarding the course experience, the median ratings for statements indicating that the elective helped students understand healthcare from a different perspective, that they felt engaged, that they felt comfortable linguistically, and that leading a session was effective for their learning was “agree” (Fig. 2). Students responded with a median rating of “strongly agree” for statements indicating that they felt comfortable participating in small groups, that they learned a great deal from other students, and that they felt comfortable using the virtual platform. The only statement with a median rating of “neither agree nor disagree” was if students felt comfortable participating in the large group. All respondents said they would recommend the elective to a friend.
Students’ self-reported experience with the CCC course. Participants responded to statements describing different aspects of the experience of the course using a five-point scale ranging from “strongly disagree” to “strongly agree.” Dashed lines represent Case Western Reserve University respondents (N = 9), solid fill indicates Universidad Nacional de San Antonio Abad del Cusco respondents (N = 10)
Students’ qualitative responses indicated that they learned a great deal from the small group discussions. One CWRU student reflected that having “small group discussions with the Peruvian students to hear about each other's experiences directly” was the most valuable part of the elective. An UNSAAC student echoed this, emphasizing the value of the “cultural and linguistic exchange” that occurred. Students indicated their preference for small group discussions on the post-session feedback forms as well. In response to this feedback, we shortened the time allotted to student presentations and large group discussions to allow more time for small group discussions in later sessions.
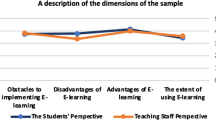
Students reported encountering several barriers during the CCC elective. UNSAAC students reported encountering more barriers overall, with the most common being language challenges (eight out of 10 UNSAAC respondents, 80%) and technology issues (n = 3, 30%) (Fig. 3). Students described problems with Internet instability and being unable to re-join discussion rooms if they lost and regained connection. One student reported having difficulty understanding the technical English used during presentations. CWRU students also encountered language challenges (four out of nine CWRU respondents, 44%), with one student reporting: “I can understand Spanish pretty well, but I have a hard time coming up with it on my own to speak.” Another noted that English dominated in the small group discussions and they “wanted to practice [their] Spanish but when most students spoke English it made [them] feel less comfortable with trying to speak [their] non-native language.” Some students from both institutions also reported feeling fatigued from other coursework (n = 5, 26%), that there was too much pre-work (n = 4, 21%), and that they had conflicts with session times (n = 2, 11%).
Pre- and Post-course Surveys
We were able to link responses from seven participants (28%) who used the same identifier on the pre- and post-course survey. Two of these students were from UNSAAC and five were from CWRU. The number of students who agreed with all five statements assessing course objectives increased between the pre- and post-course survey (Table 2). There was a statistically significant increase only for the course objective regarding the understanding of the Peruvian healthcare system (p < 0.05, shown with *). Students’ self-rated language ability improved one point on the 6-point scale, from a median of “able to have simple dialogue” to “conversational and able to use multiple conjugations.”
Discussion
The CCC elective provided a unique virtual learning experience for medical students in the USA and Peru who are interested in global health. Steenhoff et al. outline seven guiding principles for global child health partnerships including equity, inclusivity, sustainability, mutual benefit, prevention of adverse impact, social justice, and humility [20] which should be considered when designing and evaluating virtual partnerships. We aimed to incorporate these principles in our partnership, and post-elective survey feedback demonstrates that both Peruvian and US medical students reported mutual benefits from this virtual GHE partnership. As virtual GHE continues to develop, it is crucial to continuously monitor and evaluate the strengths of a course and areas for improvement to ensure partnerships are aligned with the principles outlined above. We found that the Zoom platform allowed for synchronous sessions in which students could engage in discussion-based learning in break-out rooms. Having the chance to converse about personal experiences within each country’s education and healthcare systems forged an open environment that encouraged students to engage in cultural exchange. Previous virtual GH partnerships have recommended keeping group sizes small and ensuring there is faculty support and facilitation of small groups [15, 21]. We found support for this paradigm within our cohort and limited group sizes to six students and ensured there was a physician facilitator for each group.
Another strength of the course was the flexibility of the elective structure. Students had input about session topics, which created a more personalized learning experience and an environment in which students oversaw their own learning. This flexibility allowed students to focus on timely topics, which led to an interesting session on the COVID-19 pandemic. Additionally, after receiving feedback that the small group discussions were more valuable, we dedicated more time towards them in lieu of students’ presentations or large group discussions. This adaptability provided the opportunity for students to participate in the development of the curriculum, which may benefit students interested in medical education.
The CCC elective contributes to the development of virtual GH education within trans-national medical school curricula. However, there are limitations in the course and evaluation methods. First, the small number of students who participated in the course and completed the post-course survey limits generalizability. Few students used the same unique identifier on the pre- and post-course survey, which limited our ability to link the responses and measure change in students’ self-assessed knowledge. We additionally were not able to exclude repeated responses. In future courses, pre- and post-course surveys should use unique identifiers that are easy for participants to remember, use platforms such as REDCap that provide the capability to link surveys, or have students use their names and have data analysis be performed by an individual with no relation to the course. Another limitation was that the survey data were self-reported. Additional evaluation methods including objective measures of knowledge change or evaluation by facilitators could improve the evaluation of future iterations of the course. There are several areas which we hope to improve in the future. Only CWRU students were eligible to receive credit for the course due to administrative barriers. While invitations for UNSAAC faculty leadership and involvement were solicited, the absence of UNSAAC faculty could be due to multiple factors, such as clinical workloads with the COVID-19 pandemic, lack of time and compensation for this volunteer work, and administrative difficulties. However, we were able to include participation of Peruvian leaders through student leaders and a US-based fellow physician who graduated from UNSAAC medical school. UNSAAC students additionally represented a broad range of class years, from second to eighth year students, while CWRU students were all first years. This resulted in UNSAAC students providing more clinical insight from their training, while CWRU students had limited clinical exposure. Future iterations could include more balanced levels of experience between the two groups.
The most frequently encountered barrier was language. CWRU students had lower foreign language skills and there were more CWRU students in attendance, which led to a larger fraction of small group discussions being conducted in English. A greater proportion of UNSAAC students reported encountering language barriers, despite having higher English language proficiency than US students with Spanish, and some CWRU students noted that they would have liked more opportunities to speak in Spanish. Language barriers have been similarly encountered in previous virtual GH partnerships [22,23,24]. There are several ways to address language barriers in future courses, including the use of closed captioning, stratifying small groups by fluency level, requiring a minimum fluency level, alternating the use of each language, recruiting students specifically from language electives, or asking students to take concurrent language courses. Technology issues were another common barrier, which other virtual GH partnerships have similarly encountered [23, 25]. Ravi et al. note that potential solutions include using audio only connections when bandwidth does not support video and using text-based platforms such as Whatsapp to provide alternative methods of communication [25].
Although virtual bi-directional GH partnerships have gained more attention due to the COVID-19 pandemic, they are not merely a tool to utilize when international field experiences are not feasible. The benefits that this type of course offers in terms of cost, equity, and flexibility suggest that medical educators should further explore using virtual methods to deliver GH education. In the future, this type of virtual international partnership could also be utilized to prepare trainees across various health professions and specialties for international field experiences, enhance their learning experience while abroad, and even expose students who might not otherwise be able to travel abroad.
Conclusion
The CCC elective provided an engaging way for medical students in Cleveland and Cusco to participate in global health education during the COVID-19 pandemic. Students reported that the synchronous small group discussions were particularly beneficial for their learning. Further work on virtual GH partnerships is needed to evaluate their effectiveness and investigate their ability to provide equitable learning opportunities to all trainees.
Data Availability
Not applicable.
References
Beaglehole R, Bonita R. What is global health? Glob Health Action. 2010. https://doi.org/10.3402/gha.v3i0.5142.
Maki J, Qualls M, White B, Kleefield S, Crone R. Health impact assessment and short-term medical missions: a methods study to evaluate quality of care. BMC Health Serv Res. 2008;8(1):121.
Rovers J, Andreski M, Becker M, Gray J. Short-term medical service trips: what is the cost of patient care and student training? Int Health. 2019. https://doi.org/10.1093/inthealth/ihz110.
Dell EM, Varpio L, Petrosoniak A, Gajaria A, McCarthy AE. The ethics and safety of medical student global health electives. Int J Med Educ. 2014;10(5):63–72.
Crump JA, Sugarman J. Ethical considerations for short-term experiences by trainees in global health. JAMA. 2008;300(12):1456–8.
Bauer I. More harm than good? The questionable ethics of medical volunteering and international student placements. Trop Dis Travel Med Vaccines. 2017;3(1):5.
Rabelais E, Rosales E. Response to “How Should Academic Medical Centers Administer Students’ ‘Domestic Global Health’ Experiences?” Ethics and Linguistics of “Domestic Global Health” Experience. AMA J Ethics. 2020;22(5):458–61.
Prideaux B. Factors affecting bilateral tourism flows. Ann Tour Res. 2005;32(3):780–801.
Mishori R, Eastman A, Evert J. Improving the safety and security of those engaged in global health traveling abroad. Glob Health Sci Pract. 2016;4(4):522–8.
Kalbarczyk A, Harrison M, Sanguineti MCD, Wachira J, Guzman CAF, Hansoti B. Practical and ethical solutions for remote applied learning experiences in global health. Ann Glob Health. 2020;86(1):103.
Long C, Meyers N, Nyoni T, Sivaraj D, Muguti GI, Chang J. A new model for educational programming in global health emerges during COVID-19. J Glob Health. 2021;11:03034.
Gruner D, Pottie K, Archibald D, Allison J, Sabourin V, Belcaid I, et al. Introducing global health into the undergraduate medical school curriculum using an e-learning program: a mixed method pilot study. BMC Med Educ. 2015;2(15):142.
Lee S-J, Park J, Lee YJ, Lee S, Kim W-H, Yoon HB. The feasibility and satisfaction of an online global health education course at a single medical school: a retrospective study. Korean J Med Educ. 2020;32(4):307–15.
Wu A, Noël GPJC, Wingate R, Kielstein H, Sakurai T, Viranta-Kovanen S, et al. An international partnership of 12 anatomy departments - improving global health through internationalization of medical education. Ann Glob Health. 2020;86(1):27.
Finlayson AET, Baraco A, Cronin N, Johnson O, Little S, Nuur A, et al. An international, case-based, distance-learning collaboration between the UK and Somaliland using a real-time clinical education website. J Telemed Telecare. 2010;16(4):181–4.
Samuels H, Rojas-Luengas V, Zereshkian A, Deng S, Moodie J, Veinot P, et al. Evaluation of the effectiveness of the Global Medical Student Partnership program in undergraduate medical education. Can Med Educ J. 2020;11(6):e90–8.
Lam SK. VE-PACK - Virtual Education Partnership and Curricular Kit [Internet]. SUGARPREP - Simulation use for global away rotations. 2021. [cited 2021 Aug 21]. Available from: https://sugarprep.org/ve-pack/.
Aronson E, et al. The jigsaw classroom. Oxford, England: Sage; 1978. p. 197.
Interagency Language Roundtable [Internet]. [cited 2021 Aug 16]. Available from: https://www.govtilr.org/Skills/ILRscale2.htm.
Steenhoff AP, Crouse HL, Lukolyo H, Larson CP, Howard C, Mazhani L, et al. Partnerships for global child health. Pediatrics. 2017;140(4). Available from: https://pediatrics.aappublications.org/content/140/4/e20163823.
Ambrose M, Murray L, Handoyo NE, Tunggal D, Cooling N. Learning global health: a pilot study of an online collaborative intercultural peer group activity involving medical students in Australia and Indonesia. BMC Med Educ. 2017;17(1):10.
Murphy R, Clissold E, Keynejad RC. Problem-based, peer-to-peer global mental health e-learning between the UK and Somaliland: a pilot study. Evid Based Ment Health. 2017;20(4):142–6.
Keynejad RC. Global health partnership for student peer-to-peer psychiatry e-learning: Lessons learned. Global Health. 2016;12(1):82.
Keynejad R, Garratt E, Adem G, Finlayson A, Whitwell S, Sheriff RS. Improved attitudes to psychiatry: a global mental health peer-to-peer e-learning partnership. Acad Psychiatry. 2016;40(4):659–66.
Ravi K, Nkuliza D, Patel R, Niyitegeka J, Davidson S, Aruparayil N. Fostering bidirectional trainee-led partnerships through a technology-assisted journal club – the GASOC experience. Trop Doct. 2021;14:00494755211035216.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics Approval
The Case Western Reserve University IRB determined that this study met the criteria for an exemption.
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lenhard, N.K., An, C., Jasthi, D. et al. Establishing a Virtual Global Health Education Partnership: The Cleveland-Cusco Connection. Med.Sci.Educ. 32, 1087–1094 (2022). https://doi.org/10.1007/s40670-022-01626-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40670-022-01626-6