Abstract
Introduction
Preference elicitation methods help to increase patient-centred medical decision making (MDM) by measuring benefit and value. Preferences can be applied in decisions regarding reimbursement, including health technology assessment (HTA); market access, including benefit–risk assessment (BRA); and clinical care. These three decision contexts have different requirements for use and elicitation of preferences.
Objectives
This systematic review identified studies using preference elicitation methods and summarized methodological and practical characteristics within the requirements of the three contexts.
Methods
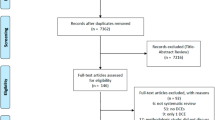
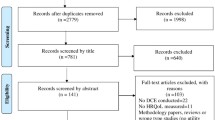
The search terms included those related to MDM and patient preferences. Only articles with original data from quantitative preference elicitation methods were included.
Results
The selected articles (n = 322) included 379 preference elicitation methods, comprising matching methods [MM] (n = 71, 18.7 %), discrete choice experiments [DCEs] (n = 96, 25.3 %), multi-criteria decision analysis (n = 12, 3.2 %) and other methods (n = 200, 52.8 %; i.e. rating scales, which provide estimates inconsistent with utility theory). Most publications of preference elicitation methods had an intended use in clinical decisions (n = 134, 40 %). Fewer preference studies had an intended use in HTA (n = 68, 20 %) or BRA (n = 12, 4 %). In clinical decisions, rating, ranking, visual analogue scales and direct choice are used most often. In HTA, DCEs and MM are both used frequently, and elicitation of preferences in BRA was limited to DCEs.
Conclusion
Relatively simple preference methods are often adequate in clinical decisions because they are easy to administer and have a low cognitive burden. MM and DCE fulfil the requirements of HTA and BRA but are complex for respondents. No preference elicitation methods with a low cognitive burden could adequately inform HTA and BRA decisions.


Similar content being viewed by others
References
Litva A, et al. ‘The public is too subjective’: public involvement at different levels of health-care decision making. Soc Sci Med. 2002;54(12):1825–37.
Coulter A. Patient engagement—what works? J Ambul Care Manag. 2012;35(2):80–9.
Smith M, Higgs J, Ellis E. Factors influencing clinical decision making, in clinical reasoning in the health professions. Oxford: Butterworth-Heinemann; 2008. p. 89–100.
Bridges J, Jones C. Patient-based health technology assessment: a vision of the future. Int J Technol Assess Health Care. 2007;23(1):30–5.
Gagnon M, et al. Introducing patients’ and the public’s perspectives to health technology assessment: a systematic review of international experiences. Int J Technol Assess Health Care. 2011;27(1):31–42.
van Til J, Ijzerman M. Why should regulators consider using patient preferences in benefit–risk assessment? Pharmacoeconomics. 2014;32(1):1–4.
European Medical Agency (2013). The patient’s voice in the evaluation of medicines: how patients can contribute to assessment of benefit and risk. Available from: http://www.ema.europa.eu/docs/en_GB/document_library/Report/2013/10/WC500153276.pdf. Accessed 11 Jul 2013.
Bridges J, et al. Patient preference methods—a patient centered evaluation paradigm. ISPOR Connect. 2007;12(6):4–7.
von Neumann J, Morgenstern O. Theory of games and economic behavior. Princeton: Princeton University Press; 1944.
Carson R, Louviere J. A common nomenclature for stated preference elicitation approaches. Environ Resour Econ. 2011;49(4):539–59.
Ali S, Ronaldson S. Ordinal preference elicitation methods in health economics and health services research: using discrete choice experiments and ranking methods. Br Med Bull. 2012;103:21–44.
Meißner M, Decker R. An empirical comparison of CBC and AHP for measuring consumer preferences. In: International Symposium of Analytical Hierarchy Process; 2009; Pittsburgh.
Green P, Srinivasan V. Conjoint analysis in consumer research: issues and outlook. J Consum Res. 1978;5:103–23.
Louviere J. Conjoint analysis modelling of stated preferences: a review of theory, methods, recent developments and external validity. Journal of Transport Economics and Policy. 1988;22(1):93–119.
Hauber A, Fairchild A, Johnson F. Quantifying benefit–risk preferences for medical interventions: an overview of a growing empirical literature. Appl Health Econ Health Policy. 2013;11(4):319–29.
Dolan J. Multi-criteria clinical decision support. Patient. 2010;3(4):229–48.
Ryan M, et al. Eliciting public preferences for healthcare: a systematic review of techniques. Health Technol Assess. 2001;5(5):186.
Ryan M, Skåtun D, Major K. Using discrete choice experiments to go beyond clinical outcomes when evaluating clinical practice. In: Ryan M, Gerard K, Amaya-Amaya M (eds). Using discrete choice experiments to value health and health care,. Dordrecht: Springer; 2008:101–16.
Esfandiari S, et al. Implant overdentures for edentulous elders: study of patient preference. Gerodontology. 2009;26(1):3–10.
Montgomery AA, Harding J, Fahey T. Shared decision making in hypertension: the impact of patient preferences on treatment choice. Fam Pract. 2001;18(3):309–13.
Gyrd-Hansen D, Kristiansen IS. Preferences for ‘life-saving’ programmes: small for all or gambling for the prize? Health Econ. 2008;17(6):709–20.
Sommers B, et al. Decision analysis using individual patient preferences to determine optimal treatment for localized prostate cancer. Cancer. 2007;110(10):2210–7.
Ubel P, et al. Public preferences for prevention versus cure. Med Decis Mak. 1998;18:141–8.
Hallan S, et al. Quality of life after cerebrovascular stroke: a systematic study of patients’ preferences for different functional outcomes. J Intern Med. 1999;246(3):309–16.
Marti J. Assessing preferences for improved smoking cessation medications: a discrete choice experiment. Eur J Health Econ. 2012;13(5):533–48.
Brundage MD, et al. Using a treatment-tradeoff method to elicit preferences for the treatment of locally advanced non-small-cell lung cancer. Med Decis Mak. 1998;18(3):256–67.
Singh J, et al. Medical decision-making and the patient: understanding preference patterns for growth hormone therapy using conjoint analysis. Med Care. 1998;36(8 Suppl):AS31–45.
Swancutt DR, Greenfield SM, Wilson S, Women’s colposcopy experience and preferences: a mixed methods study. BMC Womens Health. 2008;8:2.
Al-Janabi H, Flynn TN, Coast J. Estimation of a preference-based carer experience scale. Med Decis Mak. 2011;31(3):458–68.
Keeney RL, Raiffa H. Decisions with multiple objectives: preferences and value trade-offs. Cambridge: Cambridge University Press; 1993.
Chapman GB, et al. A multi-attribute model of prostate cancer patients’ preferences for health states. Qual Life Res. 1999;8(3):171–80.
Hummel MJM, et al. Using the analytic hierarchy process to elicit patient preferences: prioritizing multiple outcome measures of antidepressant drug treatment. Patient. 2012;5(4):225–37.
Cunich M, et al. Integrating evidence and individual preferences using a web-based multi-criteria decision analytic tool: an application to prostate cancer screening. Patient. 2011;4(3):153–62.
McCormack HM, Horne DJ, Sheather S. Clinical applications of visual analogue scales: a critical review. Psychol Med. 1988;18(4):1007–19.
Heckerling PS, Verp MS, Albert N. Patient or physician preferences for decision analysis: the prenatal genetic testing decision. Med Decis Mak. 1999;19(1):66–77.
Davis M, Hoffman J, Hsu J. Impact of patient acuity on preference for information and autonomy in decision making. Acad Emerg Med. 1999;6(8):781–5.
Ruland C. Decision support for patient preference-based care planning effects on nursing care and patient outcomes. J Am Med Inform Assoc. 1999;6(4):304–12.
Fiks A, et al. Development of an instrument to measure parents’ preferences and goals for the treatment of attention deficit-hyperactivity disorder. Acad Pediatr. 2012;12(5):445–55.
Guerlain S, Hugine A, Wang L. A comparison of 4 epinephrine autoinjector delivery systems: usability and patient preference. Ann Allerg Asthma Immunol. 2010;104(2):172–7.
Fagerlin A, Zikmund-Fisher B, Ubel P. Cure me even if it kills me: preferences for invasive cancer treatment. Med Decis Mak. 2005;25(6):614–9.
De Boer A, et al. Transhiatal vs extended transthoracic resection in oesophageal carcinoma: patients’ utilities and treatment preferences. Br J Cancer. 2002;86(6):851–7.
Johnson FR, et al. Quantifying women’s stated benefit–risk trade-off preferences for IBS treatment outcomes. Value Health. 2010;13(4):418–23.
Bewtra M, et al. Patient preferences for surgical versus medical therapy for ulcerative colitis. Inflamm Bowel Dis. 2014;20(1):103–14.
Hauber AB, et al. Patients’ benefit–risk preferences for chronic idiopathic thrombocytopenic purpura therapies. Ann Pharmacother. 2010;44(3):479–88.
Sanelli PC, et al. Work-in-progress toward incorporating patients’ preferences in practice guidelines for imaging aneurysmal subarachnoid hemorrhage. Acad Radiol. 2009;16(5):535–40.
Carroll AE, Downs SM. Improving decision analyses: parent preferences (utility values) for pediatric health outcomes. J Pediatr. 2009;155(1):21–5.
Netten A, et al. Outcomes of social care for adults: developing a preference-weighted measure. Health Technol Assess. 2012;16(16):1–166.
Desser AS, Olsen JA, Grepperud S. Eliciting preferences for prioritizing treatment of rare diseases: the role of opportunity costs and framing effects. PharmacoEconomics. 2013;31(11):1051–61.
Mason H, Baker R, Donaldson C. Understanding public preferences for prioritizing health care interventions in England: does the type of health gain matter? J Health Serv Res Policy. 2011;16(2):81–9.
Ratcliffe J. Public preferences for the allocation of donor liver grafts for transplantation. Health Econ. 2000;9(2):137–48.
Beusterien K, et al. Patient preferences for chemotherapies used in breast cancer. Int J Womens Health. 2012;4:279–87.
Aristides M, et al. Conjoint analysis of a new chemotherapy: willingness to pay and preference for the features of raltitrexed versus standard therapy in advanced colorectal cancer. PharmacoEconomics. 2002;20(11):775–84.
Hiligsmann M, et al. Health technology assessment in osteoporosis. Calcif Tissue Int. 2013;93(1):1–14.
Laba TL, et al. Patient preferences for adherence to treatment for osteoarthritis: the Medication Decisions in Osteoarthritis Study (MEDOS). BMC Musculoskelet Disord. 2013;14(160):1471–2474.
Benjamin L, et al. Physicians’ preferences for prescribing oral and intravenous anticancer drugs: a discrete choice experiment. Eur J Cancer. 2012;48(6):912–20.
Witticke, D et al. Do we prescribe what patients prefer? Pilot study to assess patient preferences for medication regimen characteristics. Patient Prefer Adher, 2012;6:679–84.
Rhodes E, et al. Preferences for type 2 diabetes health states among adolescents with or at risk of type 2 diabetes mellitus. Pediatr Diabetes. 2011;12(8):724–32.
Johnson F, et al. Are gastroenterologists less tolerant of treatment risks than patients? Benefit–risk preferences in Crohn’s disease management. J Manag Care Pharm. 2010;16(8):616–28.
Vermeulen H, et al. Preferences of patients, doctors, and nurses regarding wound dressing characteristics: a conjoint analysis. Wound Repair Regen. 2007;15(3):302–7.
Pardon K, et al. Preferences of advanced lung cancer patients for patient-centred information and decision-making: a prospective multicentre study in 13 hospitals in Belgium. Patient Educ Couns. 2009;77(3):421–9.
Pardon K, et al. Are patients’ preferences for information and participation in medical decision-making being met? Interview study with lung cancer patients. Palliative Med. 2011;25(1):62–70.
Troche CJ, Paltiel AD, Makuch RW. Evaluation of therapeutic strategies: a new method for balancing risk and benefit. Value Health. 2000;3(1):12–22.
Smith R, et al. The capability approach: an alternative evaluation paradigm for health economics? In: Jones AM (ed). The Elgar companion to health economics. 2nd ed. Cheltenham: Edward Elgar Publishing; 2012:415.
Torrance G, Feeny D, Furlong W. Visual analog scales do they have a role in the measurement of preferences for health states? Med Decis Mak. 2001;21(4):329–34.
Johnson F, et al. Crohn’s disease patients’ risk-benefit preferences: serious adverse event risks versus treatment efficacy. Gastroenterology. 2007;133(3):769–79.
Johnson F, et al. Multiple sclerosis patients’ benefit–risk preferences: serious adverse event risks versus treatment efficacy. J Neurol. 2009;256(4):554–62.
European Medicines Agency (2010). Benefit–risk methodology project. Available from: http://www.ema.europa.eu/ema/index.jsp?curl=pages/special_topics/document_listing/document_listing_000314.jsp. Accessed 29 Oct 2013.
Diaby V, Goeree R. How to use multi-criteria decision analysis methods for reimbursement decision-making in healthcare: a step-by-step guide. Expert Rev Pharmacoecon Outcomes Res. 2014;14(1):81–99.
Johnson FR, et al. Constructing experimental designs for discrete-choice experiments: report of the ISPOR Conjoint Analysis Experimental Design Good Research Practices Task Force. Value Health. 2013;16(1):3–13.
Goel V, et al. Randomized trial of a patient decision aid for choice of surgical treatment for breast cancer. Med Decis Mak. 2001;21(1):1–6.
Ruland C. Decision support for patient preference-based care planning effects on nursing care and patient outcomes. J Am Med Informat Assoc. 1999;6(4):304–12.
Acknowledgments
Marieke G.M. Weernink, Sarah I.M. Janus, Janine A. van Til, Dennis W. Raisch, Jeannette G. van Manen and Maarten J. IJzerman have no conflicts of interest that are directly relevant to the content of this review. No sources of funding were used in the preparation of this review.
Author information
Authors and Affiliations
Corresponding author
Additional information
Marieke G. M. Weernink and Sarah I. M. Janus contributed equally to this work.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Weernink, M.G.M., Janus, S.I.M., van Til, J.A. et al. A Systematic Review to Identify the Use of Preference Elicitation Methods in Healthcare Decision Making. Pharm Med 28, 175–185 (2014). https://doi.org/10.1007/s40290-014-0059-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40290-014-0059-1