Abstract
Background
Total hip replacement (THR) and total knee replacement (TKR) surgeries are being performed with increasing regularity and are associated with a high risk of developing a venous thromboembolism (VTE). New oral anticoagulants (NOACs) may be more effective at preventing VTEs but are associated with more bleeding events versus traditional anticoagulants.
Objective
The objective of this systematic review was to identify published economic analyses of NOACs for primary VTE prophylaxis following THR and TKR surgeries, and to summarise the modelling techniques used and the cost-effectiveness results.
Methods
Electronic searches of MEDLINE, EconLit and The Cochrane Library were performed from January 2008 to February 2015. Reference lists of included articles and reviews were examined for relevant studies.
Results
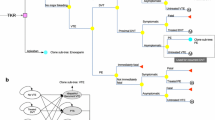
Sixteen relevant economic analyses were identified, all of which used decision-tree structures to model acute events after surgery; 13 included a chronic-phase Markov module to capture long-term complications of VTE and recurrent VTE events. All studies included prophylaxis-related major bleeding events and captured both symptomatic and asymptomatic VTE-related events; nine studies distinguished between distal and proximal deep vein thrombosis events. Overall, rivaroxaban dominated enoxaparin in eight of 11 studies and dalteparin in one study, dabigatran dominated enoxaparin in five of seven studies and apixaban dominated enoxaparin in two of two studies. Rivaroxaban dominated dabigatran in four of four studies, apixaban dominated dabigatran in two of two studies and rivaroxaban dominated apixaban in one study.
Conclusions
The economic analyses showed reasonable consistency in the model structures used and the events captured. The results strongly suggested that NOACs are cost effective alternatives to low molecular-weight heparin. Dabigatran appeared to be the least cost effective NOAC. More research is needed to assess the cost effectiveness of apixaban and edoxaban.

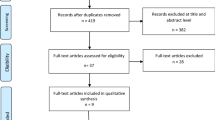
Adapted from Moher et al. [9]
Similar content being viewed by others
References
Derman PB, Fabricant PD, David G. The role of overweight and obesity in relation to the more rapid growth of total knee arthroplasty volume compared with total hip arthroplasty. J Bone Joint Surg. 2014;96(11):922–8.
Falck-Ytter Y, Francis CW, Johanson NA, Curley C, Dahl OE, Schulman S, American College of Chest Physicians, et al. Prevention of VTE in orthopedic surgery patients: antithrombotic therapy and prevention of thrombosis, 9th ed. American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. Chest. 2012;141:e278S–325S.
National Institute for Health and Care Excellence. Clinical guideline 92. Venous thromboembolism in adults admitted to hospital: reducing the risk. 2007. https://www.nice.org.uk/guidance/cg92. Accessed 10 Sept 2015.
Adam SS, McDuffie JR, Lachiewicz PF, Ortel TL, Williams JW Jr. Comparative effectiveness of new oral anticoagulants and standard thromboprophylaxis in patients having total hip or knee replacement: a systematic review. Ann Intern Med. 2013;159(4):275–84.
Gómez-Outes A, Terleira-Fernández AI, Suárez-Gea ML, Vargas-Castrillón E. Dabigatran, rivaroxaban, or apixaban versus enoxaparin for thromboprophylaxis after total hip or knee replacement: systematic review, meta-analysis, and indirect treatment comparisons. BMJ. 2012;344:e3675.
Wolowacz SE, Hess N, Brennan VK, Monz BU, Plumb JM. Cost-effectiveness of venous thromboembolism prophylaxis in total hip and knee replacement surgery: the evolving application of health economic modelling over 20 years. Curr Med Res Opin. 2008;24(10):2993–3006.
Siragusa S, Beltrametti C, Barone M, Piovella F. Clinical course and incidence of post-thrombophlebitic syndrome after profound asymptomatic deep vein thrombosis. Results of a transverse epidemiologic study [in Italian]. Minerva Cardioangiol. 1997;45:57–66.
Kapoor A, Chuang W, Radhakrishnan N, Smith KJ, Berlowitz D, Segal JB, et al. Cost effectiveness of venous thromboembolism pharmacological prophylaxis in total hip and knee replacement: a systematic review. Pharmacoeconomics. 2010;28(7):521–38.
Moher D, Liberati A, Tetzlaff J, Altman DG, The PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;6(7):e1000097.
Ryttberg L, Diamantopoulos A, Forster F, Lees M, Fraschke A, Björholt I. Cost-effectiveness of rivaroxaban versus heparins for prevention of venous thromboembolism after total hip or knee surgery in Sweden. Expert Rev Pharmacoecon Outcomes Res. 2011;11(5):601–15.
Monreal M, Folkerts K, Diamantopoulos A, Imberti D, Brosa M. Cost-effectiveness impact of rivaroxaban versus new and existing prophylaxis for the prevention of venous thromboembolism after total hip or knee replacement surgery in France, Italy and Spain. Thromb Haemost. 2013;110(5):987–94.
Diamantopoulos A, Lees M, Wells PS, Forster F, Ananthapavan J, McDonald H. Cost-effectiveness of rivaroxaban versus enoxaparin for the prevention of postsurgical venous thromboembolism in Canada. Thromb Haemost. 2010;104(4):760–70.
Duran A, Sengupta N, Diamantopoulos A, Forster F, Kwong L, Lees M. Cost and outcomes associated with rivaroxaban vs enoxaparin for the prevention of postsurgical venous thromboembolism from a US payer’s perspective. J Med Econ. 2011;14(6):824–34.
Duran A, Sengupta N, Diamantopoulos A, Forster F, Kwong L, Lees M. Cost effectiveness of rivaroxaban versus enoxaparin for prevention of post-surgical venous thromboembolism from a US payer’s perspective. Pharmacoeconomics. 2012;30(2):87–101.
Gómez-Cerezo JF, Gómez-Arrayás I, Suárez-Fernández C, Betegón-Nicolás L, de Salas-Cansado M, Rubio-Terrés C. Cost-effectiveness analysis of apixaban compared to dabigatran in the prevention of venous thromboembolism in patients subjected to total knee or hip replacement [in Spanish]. Rev Esp Cir Ortop Traumatol. 2012;56(6):459–70.
McCullagh L, Tilson L, Walsh C, Barry M. A cost-effectiveness model comparing rivaroxaban and dabigatran etexilate with enoxaparin sodium as thromboprophylaxis after total hip and total knee replacement in the Irish healthcare setting. Pharmacoeconomics. 2009;27(10):829–46.
McCullagh L, Walsh C, Barry M. Value-of-information analysis to reduce decision uncertainty associated with the choice of thromboprophylaxis after total hip replacement in the Irish healthcare setting. Pharmacoeconomics. 2012;30(10):941–59.
McDonald H, Diamantopoulos A, Wells P, Lees M, Folkerts K, Forster F, et al. Cost-effectiveness of rivaroxaban in the prevention of venous thromboembolism: a Canadian analysis using the Ontario Ministry of Health Perspective. J Med Econ. 2012;15(5):817–28.
Migliaccio-Walle K, Rublee D, Simon TA. Anticoagulation prophylaxis in orthopedic surgery: an efficiency frontier approach. Postgrad Med. 2012;124(1):41–9.
Omel’ianovskiĭ VV, Zagorodniĭ NV, Margieva AV, Tsfasman FM. Cost-effectiveness analysis of methods for thromboprophylaxis after orthopedic surgery [in Russian]. Khirurgiia (Mosk). 2010;5:72–81.
Revankar N, Patterson J, Kadambi A, Raymond V, El-Hadi W. A Canadian study of the cost-effectiveness of apixaban compared with enoxaparin for post-surgical venous thromboembolism prevention. Postgrad Med. 2013;125(4):141–53.
Ringerike T, Hamidi V, Hagen G, Reikvam A, Klemp M. Thromboprophylactic treatment with rivaroxaban or dabigatran compared with enoxaparin or dalteparin in patients undergoing elective hip- or knee replacement surgery. Report from Kunnskapssenteret (Norwegian Knowledge Centre for the Health Services) No. 13-2011. Health technology assessment (HTA) (medisinskmetodevurdering). 2011. http://hera.helsebiblioteket.no/hera/bitstream/10143/193189/1/NOKCrapport13_2011.pdf. Accessed 8 June 2015.
Wolowacz SE, Roskell NS, Maciver F, Beard SM, Robinson PA, Plumb JM, et al. Economic evaluation of dabigatran etexilate for the prevention of venous thromboembolism after total knee and hip replacement surgery. Clin Ther. 2009;31(1):194–212.
Wolowacz SE, Roskell NS, Plumb JM, Clemens A, Noack H, Robinson PA, et al. Economic evaluation of dabigatran etexilate for the prevention of venous thromboembolism in patients aged over 75 years or with moderate renal impairment undergoing total knee or hip replacement. Thromb Haemost. 2010;103(2):360–71.
Zindel S, Stock S, Müller D, Stollenwerk B. A multi-perspective cost-effectiveness analysis comparing rivaroxaban with enoxaparin sodium for thromboprophylaxis after total hip and knee replacement in the German healthcare setting. BMC Health Serv Res. 2012;12:192.
Pengo V, Lensing A, Prins M, Marchiori A, Davidson B, Tiozzo F, et al. Incidence of chronic thromboembolic pulmonary hypertension after pulmonary embolism. N Engl J Med. 2004;350:2257–64.
Eriksson BI, Borris LC, Friedman RJ, Haas S, Huisman MV, Kakkar AK, RECORD1 Study Group, et al. Rivaroxaban versus enoxaparin for thromboprophylaxis after hip arthroplasty. N Engl J Med. 2008;358:2765–75.
Kakkar AK, Brenner B, Dahl OE, Eriksson BI, Mouret P, Muntz J, RECORD2 Investigators, et al. Extended-duration rivaroxaban versus short-term enoxaparin for the prevention of venous thromboembolism after total hip arthroplasty: a double-blind, randomised controlled study. Lancet. 2008;372(9632):31–9.
Lassen MR, Ageno W, Borris LC, Lieberman JR, Rosencher N, Bandel TJ, RECORD3 Investigators, et al. Rivaroxaban versus enoxaparin for thromboprophylaxis after total knee arthroplasty. N Engl J Med. 2008;358:2776–86.
Eriksson BI, Dahl OE, Rosencher N, Kurth AA, van Dijk CN, Frostick SP, RE-MODEL Study Group, et al. Oral dabigatran etexilate vs. subcutaneous enoxaparin for the prevention of venous thromboembolism after total knee replacement: the RE-MODEL randomized trial. J Thromb Haemost. 2007;5:2178–85.
Eriksson BI, Dahl OE, Rosencher N, Kurth AA, van Dijk CN, Frostick SP, RE-NOVATE Study Group, et al. Dabigatran etexilate versus enoxaparin for prevention of venous thromboembolism after total hip replacement: a randomised, double-blind, non-inferiority trial. Lancet. 2007;370(9591):949–56.
Lassen MR, Gallus A, Raskob GE, Pineo G, Chen D, Ramirez LM, ADVANCE-3 Investigators. Apixaban versus enoxaparin for thromboprophylaxis after hip replacement. N Engl J Med. 2010;363:2487–98.
Lassen MR, Raskob GE, Gallus A, Pineo G, Chen D, Portman RJ. Apixaban or enoxaparin for thromboprophylaxis after knee replacement. N Engl J Med. 2009;361:594–604.
Lassen MR, Raskob GE, Gallus A, Pineo G, Chen D, Hornick D, ADVANCE-2 Investigators. Apixaban versus enoxaparin for thromboprophylaxis after knee replacement (ADVANCE-2): a randomised double-blind trial. Lancet. 2010;375:807–15.
Eriksson BI, Dahl OE, Huo MH, Kurth AA, Hantel S, Hermansson K, RE-NOVATE II Study Group, et al. Oral dabigatran versus enoxaparin for thromboprophylaxis after primary total hip arthroplasty (RE-NOVATE II). Thromb Haemost. 2011;105(4):721–9.
Acknowledgements
James Brockbank and Sorrel Wolowacz are employees of RTI Health Solutions.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
James Brockbank and Sorrel Wolowacz are employees of RTI Health Solutions, a provider of research and consulting services to biopharmaceutical companies.
Funding
No sources of funding were received to conduct this research or prepare this manuscript.
Author contributions
Mr Brockbank and Dr Wolowacz contributed to the study design and preparation of the manuscript; Mr Brockbank performed the literature searches and data abstraction.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Brockbank, J., Wolowacz, S. Economic Evaluations of New Oral Anticoagulants for the Prevention of Venous Thromboembolism After Total Hip or Knee Replacement: A Systematic Review. PharmacoEconomics 35, 517–535 (2017). https://doi.org/10.1007/s40273-017-0486-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40273-017-0486-4