Abstract
Background
Older adults with dementia are vulnerable to the central deteriorating effects of drugs with anticholinergic properties (DAPs). These effects include falls and confusion and may exacerbate dementia-related symptoms. Many individuals with dementia also receive acetylcholinesterase inhibitors (AChEIs), indicated for mild to moderate Alzheimer’s disease. AChEIs have opposing effects to DAPs and, consequently, concomitant use of DAPs and AChEIs may further impair cognition among patients with dementia.
Objectives
Our objectives were to (1) evaluate the anticholinergic burden among nursing home (NH) residents with dementia; (2) characterize trends in use of DAPs and concomitant use of DAPs and AChEIs among NH residents with dementia; and (3) identify factors associated with the use of DAPs and concomitant use of DAPs and AChEIs.
Methods
We conducted a retrospective analysis of Medicare data from 2007 to 2008 linked to the Minimum Data Set.
Results
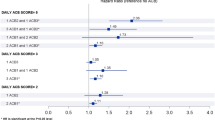
During the study period, 53,805 (77 %) NH residents with dementia used at least one DAP each month. Sixty-seven percent of residents with dementia used Anticholinergic Cognitive Burden Scale (ACBS) level 1 DAPs, 3 % used level 2 DAPs, and 31 % used level 3 DAPs. Thirteen percent of NH residents with dementia concomitantly used ACBS levels 2 or 3 DAPs and AChEIs.
Conclusions
This study sheds new light on the prevalence of DAP use and concomitant use of DAPs and AChEIs among NH residents with dementia. Clinicians should consider alternatives with lower anticholinergic effects, particularly in patients already taking DAPs.

Similar content being viewed by others
References
Harris-Kojetin L, Sengupta M, Park-Lee E, Valverde R. Long-term care services in the United States: 2013 overview. Hyattsville: National Center for Health Statistics; 2013.
Alzheimer’s Association. 2014 Alzheimer’s disease facts and figures. Alzheimer’s Dement. 2014;10(2):e47–92.
Carnahan RM, Lund BD, Perry PJ, Chrischilles EA. The concurrent use of anticholinergics and cholinesterase inhibitors: rare event or common practice? J Am Geriatr Soc. 2004;52(12):2082–7.
Mintzer J, Burns A. Anticholinergic side-effects of drugs in elderly people. J R Soc Med. 2000;93(9):457–62.
Doraiswamy PM, Husain MM. Anticholinergic drugs and elderly people: a no brainer? Lancet Neurol. 2006;5(5):379–80.
Chatterjee S, Mehta S, Sherer JT, Aparasu RR. Prevalence and predictors of anticholinergic medication use in elderly nursing home residents with dementia: analysis of data from 2004 National Nursing Home Survey. Drugs Aging. 2010;27(12):987–97.
Uusvaara J, Pitkala KH, Kautinainen H, Tilvis RS, Strandberg TE. Detailed cognitive function and use of drugs with anticholinergic properties in older people: a community-based cross-sectional study. Drugs Aging. 2013;30(3):177–82.
Gnjidic D, Hilmer SN, Blyth FM, Naganathan V, Cumming RG, Handelsman DJ, et al. High-risk prescribing and incidence of frailty among older community-dwelling men. Clin Pharmacol Ther. 2012;91(3):521–8.
Fox C, Smith T, Maidment I, Chan WY, Bua N, Myint PK, et al. Effect of medications with anti-cholinergic properties on cognitive function, delirium, physical function and mortality: a systematic review. Age Ageing. 2014;43:604–15.
Ellis JM. Cholinesterase inhibitors in the treatment of dementia. J Am Osteopathol Assoc. 2005;105:145–58.
Forchetti CM. Treating patients with moderate to severe Alzheimer’s disease: implications of recent pharmacologic studies. Prim Care Companion J Clin Psychiatry. 2005;7:155–61.
Teramura-Gronblad M, Muurinen S, Soini H, Suominen M, Pitkala KH. Use of anticholinergic drugs and cholinesterase inhibitors and their association with psychological well-being among frail older adults in residential care facilities. Ann Pharmacother. 2011;45(5):596–602.
Johnell K, Fastborn J. Concurrent use of anticholinergic drugs and cholinesterase inhibitors: register-based study of over 70,000 elderly people. Drugs Aging. 2008;25(10):871–7.
Gill SS, Mamdani M, Naglie G, Streiner DL, Bronskill SE, Kopp A, et al. A prescribing cascade involving cholinesterase inhibitors and anticholinergic drugs. Arch Intern Med. 2005;165(7):808–13.
Sink KM, Thomas J 3rd, Xu H, Craig B, Kritchevsky S, Sands LP. Dual use of bladder anticholinergics and cholinesterase inhibitors: long-term functional and cognitive outcomes. J Am Geriatr Soc. 2008;56(5):847–53.
Modi A, Weiner M, Craig BA, Sands LP, Rosenman MB, Thomas J 3rd. Concomitant use of anticholinergics with acetylcholinesterase inhibitors in Medicaid recipients with dementia and residing in nursing homes. J Am Geriatr Soc. 2009;57(7):1238–44.
Kolanowski A, Fick DM, Campbell J, Litaker M, Boustani M. A preliminary study of anticholinergic burden and relationship to a quality of life indicator, engagement in activities, in nursing home residents with dementia. J Am Med Dir Assoc. 2009;10(4):252–7.
Centers for Medicare and Medicaid Services. Chronic conditions data warehouse. http://www.ccwdata.org/web/guest/condition-categories. Accessed 31 Jul 2014.
Boustani MA, Campbell NL, Munger S, Maidment I, Fox C. Impact of anticholinergics on the aging brain: a review and practical application. Aging Health. 2008;4(3):311–20.
Aging Brain Program of the Indiana University Center for Aging Research. Anticholinergic cognitive burden scale (2012 update). Aging brain care. 2012. http://www.agingbraincare.org/uploads/products/ACB_scale_-_legal_size.pdf. Accessed 7 Jul 2014
Kersten H, Wyller TB. Anticholinergic drug burden in older people’s brain—how well is it measured? Basic Clin Pharmacol Toxicol. 2014;114(2):151–9.
Perlman CM, Hirdes JP. The aggressive behavior scale: a new scale to measure aggression based on the minimum data set. Am Geriatr Soc. 2008;56(12):2298–303.
Morris JN, Fries BE, Mehr DR, Hawes C, Phillips C, Mor V, et al. MDS Cognitive Performance Scale. J Gerontol. 1994;49(4):M174–82.
Morris JN, Fries BE, Morris SA. Scaling ADLs within MDS. J Gerontol A Biol Sci Med Sci. 1999;54(11):M546–53.
Carnahan RM, Lund BD, Perry PJ, Pollock BG, Culp KR. The Anticholinergic Drug Scale as a measure of drug-related anticholinergic burden: associations with serum anticholinergic activity. J Clin Pharmacol. 2006;46(12):1281–6.
Boudreau DM, Yu O, Gray SL, Raebel MA, Johnson J, Larson EB. Concomitant use of cholinesterase inhibitors and anticholinergics: prevalence and outcomes. J Am Geriatr Soc. 2011;59:2069–76.
Briesacher BA, Limcangco MR, Simoni-Wastila L, Doshi JA, Levens SR, Shea DS, et al. The quality of antipsychotic drug prescribing in nursing homes. Arch Intern Med. 2005;165:1280–5.
Shekelle P, Maglione M, Bagley S, et al. Efficacy and comparative effectiveness of off-label use of atypical antipsychotics. Rockville: Agency for Healthcare Research and Quality (US); 2007. (Comparative Effectiveness Review no. 6, AHRQ publication no. 07-EHC003-EF)
United States Food and Drug Administration. Public Health Advisory: deaths with antipsychotics in elderly patients with behavioral disturbances. 2005. http://www.fda.gov/drugs/drugsafety/postmarketdrugsafetyinformationforpatientsandproviders/ucm053171. Accessed 22 Oct 2014
Acknowledgments
Drs. Palmer, Albrecht, Park, Dutcher, Rattinger, Simoni-Wastila, and Zuckerman, and Ms. Walker would like to thank Dr. Xingang Liu and Ms. Xian Shen for SAS® coding assistance and acknowledge Ms. Zippora Kiptanui for assistance with the IRB protocol. This work was supported in part by the Food and Drug Administration (Collaborative agreement U01FD004320). Dr. Albrecht is supported by National Institutes of Health grant T32AG000262-14 (J. Magaziner, Primary Investigator). Drs. Palmer and Park are supported by a fellowship grant from Novartis. The authors declare no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Palmer, J.B., Albrecht, J.S., Park, Y. et al. Use of Drugs with Anticholinergic Properties Among Nursing Home Residents with Dementia: A National Analysis of Medicare Beneficiaries from 2007 to 2008. Drugs Aging 32, 79–86 (2015). https://doi.org/10.1007/s40266-014-0227-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40266-014-0227-8