Abstract
Background and Objective
The economic outcomes of dual antiplatelet therapy in East Asian patients are still unclear. We aimed to evaluate the economic outcomes of ticagrelor versus clopidogrel for patients with acute coronary syndrome (ACS) in China, Japan, Korea, Taiwan and Hong Kong.
Methods
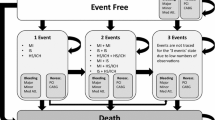
A two-phase model consisting of a 1-year decision tree and a lifetime Markov model was used to estimate the economic outcomes. The data from the East Asian subgroup of Platelet Inhibition and Patient Outcomes (PLATO) and PHILO studies were used for the calculation of the events rate for ticagrelor and clopidogrel in the first 12 months, whereas the costs were obtained from East Asian sources and utility from the published literature. Sensitivity analyses were conducted to test model robustness.
Results
Ticagrelor showed the marginal lifetime quality-adjusted life-year (QALY) of 0.0050, 0.0091, 0.0107, 0.0050, and 0.0050 in China, Japan, Korea, Taiwan, and Hong Kong compared with clopidogrel, with marginal healthcare costs of (all values in US dollars) $562, $595, $975, $611, and $672, respectively. The marginal cost per QALY gained with ticagrelor was $112,051, $65,692, $91,207, $121,838, and $133,953 from a public healthcare system perspective of China, Japan, Korea, Taiwan, and Hong Kong, respectively. The sensitivity analysis showed consistent results.
Conclusion
Treatment of ACS for 12 months with ticagrelor is not a cost-effective option for the prevention of thrombotic events in East Asia.



Similar content being viewed by others
References
Zhou M, Wang H, Zhu J, Chen W, Wang L, Liu S, et al. Cause-specific mortality for 240 causes in China during 1990–2013: a systematic subnational analysis for the Global Burden of Disease Study 2013. Lancet. 2016;387:251–72.
Wang W, Hu SS, Kong LZ, Gao RL, Zhu ML, Wang WYJ, et al. Summary of report on cardiovascular diseases in China, 2012. Biomed Environ Sci. 2014;27:552–8.
Chan MY, Du X, Eccleston D, Ma C, Mohanan PP, Ogita M, et al. Acute coronary syndrome in the Asia-Pacific region. Int J Cardiol. 2016;202:861–9.
Cheng TO. The current state of cardiology in China. Int J Cardiol. 2004;96:425–39.
Deng M, Li H, Shi M, He Y, Liao J, Yang J, et al. Prevalence of acute coronary heart disease among farmers in Panyu, Guangzhou: a 20-year population-based study. Zhonghua Xin Xue Guan Bing Za Zhi. 2014;42:236–40.
Cowley MJ, Kuritzky L. Developments in antiplatelet therapy for acute coronary syndromes and considerations for long-term management. Curr Med Res Opin. 2009;25:1477–90.
Htun WW, Steinhubl SR. Ticagrelor: the first novel reversible P2Y(12) inhibitor. Expert Opin Pharmacother. 2013;14:237–45.
Höchtl T, Sinnaeve PR, Adriaenssens T, Huber K. Oral antiplatelet therapy in acute coronary syndromes: update 2012. Eur Heart J Acute Cardiovasc Care. 2012;1:79–86.
Wallentin L, Becker RC, Budaj A, Cannon CP, Emanuelsson H, Held C, et al. Ticagrelor versus clopidogrel in patients with acute coronary syndromes. N Engl J Med. 2009;361:1045–57.
Cannon CP, Harrington RA, James S, Ardissino D, Becker RC, Emanuelsson H, et al. Comparison of ticagrelor with clopidogrel in patients with a planned invasive strategy for acute coronary syndromes (PLATO): a randomised double-blind study. Lancet. 2010;375:283–93.
Cayla G, Silvain J, Collet J-P, Montalescot G. Updates and current recommendations for the management of patients with non-ST-elevation acute coronary syndromes: what it means for clinical practice. Am J Cardiol. 2015;115:10A–22A.
Speciality Committee on Prevention and Treatment of Thrombosis of Chinese College of Cardiovascular Physicians, Section of Interventional Cardiology of Chinese Society of Cardiology of Chinese Medical Association, Editorial Board of Chinese Journal of Cardiology. Chinese expert consensus statement on clinical use of ticagrelor. Zhonghua Xin Xue Guan Bing Za Zhi. 2016;44:112–20.
Abdel-Qadir H, Roifman I, Wijeysundera HC. Cost-effectiveness of clopidogrel, prasugrel and ticagrelor for dual antiplatelet therapy after acute coronary syndrome: a decision-analytic model. CMAJ Open. 2015;3:E438–46.
Chin CT, Mellstrom C, Chua TSJ, Matchar DB. Lifetime cost-effectiveness analysis of ticagrelor in patients with acute coronary syndromes based on the PLATO trial: a Singapore healthcare perspective. Singap Med J. 2013;54:169–75.
Grima DT, Brown ST, Kamboj L, Bainey KR, Goeree R, Oh P, et al. Cost-effectiveness of ticagrelor versus clopidogrel in patients with acute coronary syndromes in Canada. Clinicoecon Outcomes Res. 2014;6:49–62.
Janzon M, James S, Cannon CP, Storey RF, Mellström C, Nicolau JC, et al. Health economic analysis of ticagrelor in patients with acute coronary syndromes intended for non-invasive therapy. Heart. 2015;101:119–25.
Liew D, De Abreu Lourenço R, Adena M, Chim L, Aylward P. Cost-effectiveness of 12-month treatment with ticagrelor compared with clopidogrel in the management of acute coronary syndromes. Clin Ther. 2013;35(1110–1117):e9.
Nikolic E, Janzon M, Hauch O, Wallentin L, Henriksson M, PLATO Health Economic Substudy Group. Cost-effectiveness of treating acute coronary syndrome patients with ticagrelor for 12 months: results from the PLATO study. Eur Heart J. 2013;34:220–8.
Jeong Y-H. “East asian paradox”: challenge for the current antiplatelet strategy of “one-guideline-fits-all races” in acute coronary syndrome. Curr Cardiol Rep. 2014;16:485.
Levine GN, Jeong Y-H, Goto S, Anderson JL, Huo Y, Mega JL, et al. Expert consensus document: World Heart Federation expert consensus statement on antiplatelet therapy in East Asian patients with ACS or undergoing PCI. Nat Rev Cardiol. 2014;11:597–606.
Kang H-J, Clare RM, Gao R, Held C, Himmelmann A, James SK, et al. Ticagrelor versus clopidogrel in Asian patients with acute coronary syndrome: a retrospective analysis from the Platelet Inhibition and Patient Outcomes (PLATO) Trial. Am Heart J. 2015;169(899–905):e1.
Goto S, Huang C-H, Park S-J, Emanuelsson H, Kimura T. Ticagrelor vs. clopidogrel in Japanese, Korean and Taiwanese patients with acute coronary syndrome—randomized, double-blind, phase III PHILO study. Circ J. 2015;79:2452–60.
Yan X, Gu X, Zhou L, Lin H, Wu B. Cost effectiveness of apixaban and enoxaparin for the prevention of venous thromboembolism after total knee replacement in China. Clin Drug Investig. 2016;36:1001–10.
Jiang M, You JH. Cost-effectiveness analysis of personalized antiplatelet therapy in patients with acute coronary syndrome. Pharmacogenomics. 2016;17:701–13.
Tsutani K, Igarashi A, Fujikawa K, Evers T, Kubin M, Lamotte M, et al. A health economic evaluation of aspirin in the primary prevention of cardiovascular disease in Japan. Intern Med. 2007;46:157–62.
Chan L, Chen C-H, Hwang J-J, Yeh S-J, Shyu K-G, Lin R-T, et al. Cost-effectiveness of amlodipine compared with valsartan in preventing stroke and myocardial infarction among hypertensive patients in Taiwan. Int J Gen Med. 2016;9:175–82.
Kwon J-W, Park H-Y, Kim YJ, Moon S-H, Kang H-Y. Cost-effectiveness of pharmaceutical interventions to prevent osteoporotic fractures in postmenopausal women with osteopenia. J Bone Metab. 2016;23:63–77.
Wu B, Lin H, Tobe RG, Zhang L, He B. Ticagrelor versus clopidogrel in East-Asian patients with acute coronary syndromes: a meta-analysis of randomized trials. J Comp Eff Res. 2018;7:281–91.
Daida H, Miyauchi K, Ogawa H, Yokoi H, Matsumoto M, Kitakaze M, et al. Management and two-year long-term clinical outcome of acute coronary syndrome in Japan: prevention of atherothrombotic incidents following ischemic coronary attack (PACIFIC) registry. Circ J. 2013;77:934–43.
Cui M, Tu CC, Chen EZ, Wang XL, Tan SC, Chen C. A cost-effectiveness analysis of clopidogrel for patients with non-ST-segment elevation acute coronary syndrome in China. Adv Ther. 2016;33:1600–11.
WHO|Life tables [Internet]. [cited 2016 Sep 22]. http://www.who.int/gho/mortality_burden_disease/life_tables/life_tables/en/.
Coleman CI, Limone BL. Cost-effectiveness of universal and platelet reactivity assay-driven antiplatelet therapy in acute coronary syndrome. Am J Cardiol. 2013;112:355–62.
Bo H, Fu AZ. Predicting utility for joint health states: a general framework and a new nonparametric estimator. Med Decis Mak. 2010;30:E29–39.
Kang H-Y, Ko S-K, Liew D. Results of a Markov model analysis to assess the cost-effectiveness of statin therapy for the primary prevention of cardiovascular disease in Korea: the Korean Individual-Microsimulation Model for Cardiovascular Health Interventions. Clin Ther. 2009;31:2919–30.
Li T, Liu M, Ben H, Xu Z, Zhong H, Wu B. Clopidogrel versus aspirin in patients with recent ischemic stroke and established peripheral artery disease: an economic evaluation in a Chinese setting. Clin Drug Investig. 2015;35:365–74.
Davis KL, Meyers J, Zhao Z, McCollam PL, Murakami M. High-risk atherosclerotic cardiovascular disease in a real-world employed Japanese population: prevalence, cardiovascular event rates, and costs. J Atheroscler Thromb. 2015;22:1287–304.
Hosaka A, Miyata T, Onishi Y, Liao L, Zhang Q. Clinical and economic burden in patients with diagnosis of peripheral arterial disease in a claims database in Japan. Clin Ther. 2014;36:1223–30, 1230.e1–4.
Tang CH, Chuang PY, Chen CA, Fang YC. Medical costs of cardiovascular diseases in Taiwan. Value Health. 2014;17:A759–60.
Kumar RS, Douglas PS, Peterson ED, Anstrom KJ, Dai D, Brennan JM, et al. Effect of race and ethnicity on outcomes with drug-eluting and bare metal stents: results in 423 965 patients in the linked National Cardiovascular Data Registry and centers for Medicare & Medicaid services payer databases. Circulation. 2013;127:1395–403.
Sorich MJ, Rowland A, McKinnon RA, Wiese MD. CYP2C19 genotype has a greater effect on adverse cardiovascular outcomes following percutaneous coronary intervention and in Asian populations treated with clopidogrel: a meta-analysis. Circ Cardiovasc Genet. 2014;7:895–902.
Inohara T, Kohsaka S, Goto M, Furukawa Y, Fukushima M, Sakata R, et al. Hypothesis of long-term outcome after coronary revascularization in Japanese patients compared to multiethnic groups in the US. PLoS ONE. 2015;10:e0128252.
Ye Z, Liu EHC, Higgins JPT, Keavney BD, Lowe GDO, Collins R, et al. Seven haemostatic gene polymorphisms in coronary disease: meta-analysis of 66,155 cases and 91,307 controls. Lancet. 2006;367:651–8.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Funding
This study was supported by grants from the Fourth Round of a Three-year Action Plan on Public Health Discipline and Talent Program (Evidence-based Public Health and Health Economics, No. 15GWZK0901). The funding agency had no role in the study design, data collection and analysis, or the decision to publish.
Rights and permissions
About this article
Cite this article
Wu, B., Tobe, R.G., Liu, Y. et al. Health Economic Analysis of Antiplatelet Therapy for Acute Coronary Syndromes in the Context of Five Eastern Asian Countries. Clin Drug Investig 38, 621–630 (2018). https://doi.org/10.1007/s40261-018-0649-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40261-018-0649-x