Abstract
Background
Prostate cancer remains a prevalent diagnosis with a spectrum of treatment choices that offer similar oncologic outcomes but differing side effect profiles and associated costs. As the technology for prostate radiation therapy has advanced, its associated costs have escalated, thus making cost-effectiveness analyses critical to assess the value of competing treatment options, including watchful waiting, surgery, brachytherapy, intensity-modulated radiation therapy (IMRT), 3D-conformal radiation therapy (3D-CRT), proton beam therapy (PBT), and stereotactic body radiation therapy (SBRT).
Objective
The aim of this systematic review was to identify articles that performed a cost-effectiveness analysis on different radiation treatment options for localized prostate cancer, summarize their findings, and highlight the main drivers of cost effectiveness.
Methods
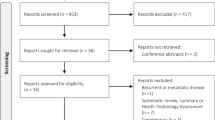
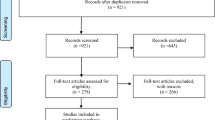
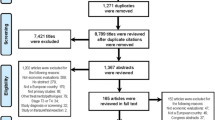
A literature search was performed on two databases, PubMed and the Cost-Effectiveness Analysis Registry (https://research.tufts-nemc.org/cear4), using search terms that included ‘prostate’, ‘cost effectiveness prostate radiation’ and ‘cost analysis comparative effectiveness prostate radiation’. Studies were included in this review if the cost data were from 2002 or later, and outcomes reported both cost and effectiveness, preferably including a cost–utility analysis with the outcome of an incremental cost-effectiveness ratio with quality-adjusted life-year (QALY) as the effectiveness measure.
Results
There were 14 articles between 2003 and 2013 that discussed cost effectiveness of prostate radiotherapy in men over the age of 65. All but four of the papers were from the US; the others were from Canada and the UK. The majority of the papers used Markov decision analysis and estimated cost from a payer’s perspective, usually from Medicare reimbursement data. Assumptions for the model and utilities to calculate QALYs were estimated using published literature at the time of the analysis. Each analysis had a sensitivity analysis to compensate for the uncertainty of the model inputs. The main drivers of cost effectiveness were the cost of the radiation treatment and the differential QALYs accrued because of different treatment-related morbidities. Brachytherapy was consistently found to be more cost effective when compared with surgery and other radiation treatment options. IMRT was cost effective when compared with 3D-CRT. PBT was not found to be cost effective in any of the analyses, mostly due to the high costs of PBT. SBRT was the newest technology that was analyzed, and it was also found to be cost effective compared with IMRT and PBT.
Conclusions
Cost-effectiveness research of prostate radiation treatments allows patients, providers, and payers to better understand the true value of each treatment choice. Due to the variation in each of these analyses (e.g., costing, and disease and complication assumptions, etc.), it is difficult to generalize the results. One must be careful in drawing conclusions from these studies and extrapolating to individual patients, particularly with the clear utility dependence seen in the majority of these studies.

Similar content being viewed by others
References
IOM (Institute of Medicine). Initial National Priorities for Comparative Effectiveness Research. Washington, DC: The National Academics Press; 2009.
Ollendorf DA, Hayes J, McMahon P, Kuba M, Pearson SD. Management options for low-risk prostate cancer: a report on comparative effectiveness and value. http://www.icer-review.org/index.php/mgmtoptionlrpc.html. Boston: Institute for Clinical and Economic Review; 2009.
Siegel R, et al. Cancer statistics, 2011: the impact of eliminating socioeconomic and racial disparities on premature cancer deaths. CA Cancer J Clin. 2011;61(4):212–36.
Nguyen PL, et al. Cost implications of the rapid adoption of newer technologies for treating prostate cancer. J Clin Oncol. 2011;29(12):1517–24.
Dearnaley DP, et al. Escalated-dose versus standard-dose conformal radiotherapy in prostate cancer: first results from the MRC RT01 randomised controlled trial. Lancet Oncol. 2007;8(6):475–87.
Pollack A, et al. Prostate cancer radiation dose response: results of the M. D. Anderson phase III randomized trial. Int J Radiat Oncol Biol Phys. 2002;53(5):1097–105.
Zietman AL, et al. Comparison of conventional-dose vs high-dose conformal radiation therapy in clinically localized adenocarcinoma of the prostate—a randomized controlled trial. JAMA—J Am Med Assoc. 2005;294(10):1233–9.
Sheets NC, et al. Intensity-modulated radiation therapy, proton therapy, or conformal radiation therapy and morbidity and disease control in localized prostate cancer. JAMA. 2012;307(15):1611–20.
Nutting CM, et al. Reduction of small and large bowel irradiation using an optimized intensity-modulated pelvic radiotherapy technique in patients with prostate cancer. Int J Radiat Oncol Biol Phys. 2000;48(3):649–56.
Zelefsky MJ, et al. Incidence of late rectal and urinary toxicities after three-dimensional conformal radiotherapy and intensity-modulated radiotherapy for localized prostate cancer. Int J Radiat Oncol Biol Phys. 2008;70(4):1124–9.
Liberati A, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. Ann Intern Med. 2009;151(4):W65–94.
Hayes JH, et al. Observation versus initial treatment for men with localized, low-risk prostate cancer: a cost-effectiveness analysis. Ann Intern Med. 2013;158(12):853–60.
Parthan A, et al. Comparative cost-effectiveness of stereotactic body radiation therapy versus intensity-modulated and proton radiation therapy for localized prostate cancer. Front Oncol. 2012;2:81.
Cooperberg MR, et al. Primary treatments for clinically localised prostate cancer: a comprehensive lifetime cost-utility analysis. BJU Int. 2013;111(3):437–50.
Hummel S, et al. Clinical and cost-effectiveness of new and emerging technologies for early localised prostate cancer: a systematic review. Health Technol Assess. 2003;7(33):iii, ix–x, 1–157.
Hummel SR, et al. A model of the cost-effectiveness of intensity-modulated radiotherapy in comparison with three-dimensional conformal radiotherapy for the treatment of localised prostate cancer. Clin Oncol (R Coll Radiol). 2012;24(10):e159–67.
Konski A, et al. Is proton beam therapy cost effective in the treatment of adenocarcinoma of the prostate? J Clin Oncol. 2007;25(24):3603–8.
Konski A, et al. Using decision analysis to determine the cost-effectiveness of intensity-modulated radiation therapy in the treatment of intermediate risk prostate cancer. Int J Radiat Oncol Biol Phys. 2006;66(2):408–15.
Sher DJ, et al. Cost-effectiveness analysis of SBRT versus IMRT for low-risk prostate cancer. Am J Clin Oncol. 2014;37(3):215–21.
Yong JH, et al. Cost-effectiveness of intensity-modulated radiotherapy in prostate cancer. Clin Oncol (R Coll Radiol). 2012;24(7):521–31.
Shah C, et al. Brachytherapy provides comparable outcomes and improved cost-effectiveness in the treatment of low/intermediate prostate cancer. Brachytherapy. 2012;11(6):441–5.
Showalter TN, et al. Costs of early adjuvant radiation therapy after radical prostatectomy: a decision analysis. Ann Oncol. 2012;23(3):701–6.
Quigley MM, Mate TP, Sylvester JE. Prostate tumor alignment and continuous, real-time adaptive radiation therapy using electromagnetic fiducials: clinical and cost-utility analyses. Urol Oncol. 2009;27(5):473–82.
D’Amico AV, et al. Biochemical outcome after radical prostatectomy, external beam radiation therapy, or interstitial radiation therapy for clinically localized prostate cancer. JAMA. 1998;280(11):969–74.
Kupelian PA, et al. Preliminary observations on biochemical relapse-free survival rates after short-course intensity-modulated radiotherapy (70 Gy at 2.5 Gy/fraction) for localized prostate cancer. Int J Radiat Oncol Biol Phys. 2002;53(4):904–12.
Kupelian PA, et al. Hypofractionated intensity-modulated radiotherapy (70 GY at 2.5 GY per fraction) for localized prostate cancer: Long-term outcomes. Int J Radiat Oncol Biol Phys. 2005;63(5):1463–8.
Morgan PB, et al. A matched pair comparison of intensity modulated radiotherapy and three-dimensional conformal radiotherapy for prostate cancer: toxicity and outcomes. Int J Radiat Oncol Biol Phys. 2007:69(3):S319–S319.
Vora SA, et al. Analysis of biochemical control and prognostic factors in patients treated with either low-dose three-dimensional conformal radiation therapy or high-dose intensity-modulated radiotherapy for localized prostate cancer. Int J Radiat Oncol Biol Phys. 2007;68(4):1053–8.
Hodges JC, et al. Cost-effectiveness analysis of stereotactic body radiation therapy versus intensity-modulated radiation therapy: an emerging initial radiation treatment option for organ-confined prostate cancer. J Oncol Pract. 2012;8(3 Suppl):e31s–7s.
Mohammed N, et al. Comparison of acute and late toxicities for three modern high-dose radiation treatment techniques for localized prostate cancer. Int J Radiat Oncol Biol Phys. 2012;82(1):204–12.
Swanson GP, et al. Predominant treatment failure in postprostatectomy patients is local: analysis of patterns of treatment failure in SWOG 8794. J Clin Oncol. 2007;25(16):2225–9.
Thompson IM, Tangen CM, Klein EA. Is there a standard of care for pathologic stage T3 prostate cancer? J Clin Oncol. 2009;27(18):2898–9.
Thompson IM Jr, et al. Adjuvant radiotherapy for pathologically advanced prostate cancer: a randomized clinical trial. JAMA. 2006;296(19):2329–35.
Perrier L, et al. Cost of prostate image-guided radiation therapy: results of a randomized trial. Radiother Oncol. 2013;106(1):50–8.
Sher DJ, Punglia RS. Decision analysis and cost-effectiveness analysis for comparative effectiveness research-a primer. Semin Radiat Oncol. 2014;24(1):14–24.
Beck JR, Pauker SG. The Markov process in medical prognosis. Med Decis Making. 1983;3(4):419–58.
Russell LB, et al. The role of cost-effectiveness analysis in health and medicine. Panel on Cost-Effectiveness in Health and Medicine. JAMA. 1996;276(14):1172–7.
Hayman JA, et al. A comparison of two methods for estimating the technical costs of external beam radiation therapy. Int J Radiat Oncol Biol Phys. 2000;47(2):461–7.
Churchill DN, Lemon BC, Torrance GW. A cost-effectiveness analysis of continuous ambulatory peritoneal dialysis and hospital hemodialysis. Med Decis Making. 1984;4:489–500.
Winkelmayer WC, et al. Health economic evaluations: the special case of end-stage renal disease treatment. Med Decis Making. 2002;22(5):417–30.
Authors’ contributions
Neha Amin is the guarantor of the content of this paper. She was the primary author who performed the systematic review, reviewed the content of all articles, and wrote the paper.
David Sher reviewed and confirmed the content of the paper.
Andre Konski reviewed and confirmed the content of the paper.
Conflicts of interest
Neha Amin: none.
David Sher: none.
Andre Konski: none.
Study funding
No funding was received for the conduct of this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Amin, N.P., Sher, D.J. & Konski, A.A. Systematic Review of the Cost Effectiveness of Radiation Therapy for Prostate Cancer from 2003 to 2013. Appl Health Econ Health Policy 12, 391–408 (2014). https://doi.org/10.1007/s40258-014-0106-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40258-014-0106-9