Abstract
Background and Objectives
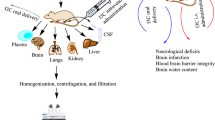
Pueraria labata has traditionally been applied in the treatment of stroke in Chinese clinics. Puerarin is the key ingredient in it for brain protection effect. To find a superior administration route for puerarin in the treatment of ischemic cerebrovascular disease, the pharmacokinetics of puerarin based on the middle cerebral artery occlusion (MCAO) rat via different administration routes were studied and compared.
Methods
Ten rats (MCAO model) divided into two groups were treated with puerarin via intravenous and intranasal routes. Samples of brain and plasma were collected by microdialysis and tested by high-performance liquid chromatography with tandem mass spectrometric detection (HPLC–MS/MS).
Results
In olfactory bulb, the intranasal group got a higher C max, which was eight times higher than that of intravenous group. The AUC of puerarin were 255.96 ± 87.74 and 24.56 ± 15.50 min·μg/ml for intranasal and intravenous group, respectively. The intranasal group also got a longer T 1/2 compared with intravenous group. The drug target index (DTI) of intranasal group was up to 47.98%, which was highly improved, compared with intravenous group.
Conclusions
The in vivo experiments based on the MCAO model showed that, compared with intravenous route, the bioavailability and brain-targeting of drug were highly improved via intranasal route. In pathological conditions, compared with normal rats, the AUC of puerarin in brain and DTI increased significantly.



Similar content being viewed by others
References
Xu X, Zhang S, Zhang L, Yan W, Zheng X. The neuroprotection of puerarin against cerebral ischemia is associated with the prevention of apoptosis in rats. Planta Med. 2005;71:585–91.
Xu XH, Zheng XX, Zhou Q, Li H. Inhibition of excitatory amino acid efflux contributes to protective effects of puerarin against cerebral ischemia in rats. Biomed Environ Sci. 2007;20:336–42.
Luo JX, Xue SP, Yang LX, Zheng H. Adverse drug reactions of puerarin injection: a study of evidence based medicine. Chin J Inform Tradit Chin Med. 2012;19:27–30.
Tang YJ. Analysis of adverse drug reactions caused by puerarin injection. Chin J Clin Ration Drug Use. 2015;. doi:10.15887/j.cnki.13-1389/r.2015.28.072.
Dhuria SV, Hanson LR, Frey WH. Intranasal delivery to the central nervous system: mechanisms and experimental considerations. J Pharm Sci. 2010;99:1654–73.
Lochhead JJ, Thorne RG. Intranasal delivery of biologics to the central nervous system. Adv Drug Deliv Rev. 2012;64:614–28.
Lu Y, Du SY, Bai J, Li PY, Wen R, Zhao XJ. Bioavailability and brain-targeting of geniposide in gardenia-borneol co-compound by different administration routes in mice. Int J Mol Sci. 2012;13:14127–35.
Delgado JM, DeFeudis FV, Roth RH, et al. Dialytrode for longterm intracerebral perfusion in awake monkeys. Arch Int Pharmacodyn Ther. 1972;198:9–21.
Zhang Q, Wu D, Wu J, Qu Y, Mu C, Han B, Zhang Q. Improved blood–brain barrier distribution: effect of borneol on the brain pharmacokinetics of kaempferol in rats by in vivo microdialysis sampling. J Ethnopharmacol. 2015;162:270–7.
Wei JB, Lai Q, Shumyak SP, Xu LF, Zhang CX, Ling JJ, Yu Y. An LC/MS quantitative and microdialysis method for cyclovirobuxine D pharmacokinetics in rat plasma and brain: the pharmacokinetic comparison of three different drug delivery routes. J Chromatogr B. 2015;1002:185–93.
Xiao BX, Feng L, Cao FR, Pan RL, Liao YH, Liu XM, Chang Q. Pharmacokinetic profiles of the five isoflavonoids from Pueraria lobata roots in the CSF and plasma of rats. J Ethnopharmacol. 2016;184:22–9.
Luo CF, Yuan M, Chen MS, Liu SM, Huang BY, Liu XW, Zhu L. Determination of puerarin in rat plasma by rapid resolution liquid chromatography tandem mass spectrometry in positive ionization mode. J Chromatogr B. 2011;879:1497–501.
Longa EZ, Weinstein PR, Carlson S, Cummins R. Reversible middle cerebral artery occlusion without craniectomy in rats. Stroke. 1989;20:84–91.
Li PY, Bai J, Lu Y, Wen R, Du SY. Bioavailability and brain-targeting of puerarin by different administration routes in rats. J Drug Deliv Sci Technol. 2013;23:583–6.
Freeman SM, Samineni S, Allen PC, Stockinger D, Bales KL, Hwa GG, Roberts JA. Plasma and CSF oxytocin levels after intranasal and intravenous oxytocin in awake macaques. Psychoneuroendocrinology. 2016;66:185–94.
Wei JB, Lai Q, Shumyak SP, Xu LF, Zhang CX, Ling JJ, Yu Y. An LC/MS quantitative and microdialysis method for cyclovirobuxine D pharmacokinetics in rat plasma and brain: the pharmacokinetic comparison of three different drug delivery routes. J Chromatogr B Analyt Technol Biomed Life Sci. 2015;1002:185–93.
Knowland D, Arac A, Sekiguchi KJ, Hsu M, Lutz SE, Perrino J, Steinberg GK, Barres BA, Nimmerjahn A, Agalliu D. Stepwise recruitment of transcellular and paracellular pathways underlies blood–brain barrier breakdown in stroke. Neuron. 2014;82:603–17.
Sandoval KE, Witt KA. Blood–brain barrier tight junction permeability and ischemic stroke. Neurobiol Dis. 2008;32:200–19.
Xu P, Li Y, Du SY, Lu Y, Bai J, Guo Q. Comparative pharmacokinetics of borneol in cerebral ischemia-reperfusion and sham-operated rats. J Zhejiang Univ-Sci B. 2014;15:84–91.
Zeng MF, Pan LM, Zhu HX, Zhang QC, Guo LW. Comparative pharmacokinetics of baicalin in plasma after oral administration of Huang–Lian–Jie–Du–Tang or pure baicalin in MCAO and sham-operated rats. Fitoterapia. 2010;81:490–6.
Li YT, Lu Y, Hu JC, Gong Z, Yang W, Wang AM, Zheng J, Liu T, Chen TT, Hu J, Mi L, Li YJ, Lan YY, Wang YL. Pharmacokinetic comparison of scutellarin and paeoniflorin in sham-operated and middle cerebral artery occlusion ischemia and reperfusion injury rats after intravenous administration of Xin-Shao formula. Molecules. 2016;21:e1191.
Zhao W, Wang S, Li FJ. Progress in understanding the multiple organ injury induced by cerebral ischemia–reperfusion. Acta Neuropharmacol. 2014;4:55–63.
Carlos RCL, Beatriz EIY, Fernando GR. Gastrointestinal complications after ischemic stroke. J Neurol Sci. 2014;346:20–5.
Jura E. Gastrointestinal disturbances in stroke. Acta Neurol Scand. 1987;76:168–71.
Zhao XJ, Lu Y, Du SY, Wang S, Gong WH, Lei XJ. Irritation of Xingnaojing microemulsion to nasal mucosa in rats. J Beijing Univ Tradit Chin Med. 2012;35:626–71.
Kozlovskaya L, Abou-Kaoud M, Stepensky D. Quantitative analysis of drug delivery to the brain via nasal route. J Control Release. 2014;189:133–40.
Acknowledgements
The words and grammar of the manuscript were checked by Yali Wu and Puning Cao.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Funding
The project was supported by Beijing Natural Science Foundation (No. 7164274), National Natural Science Foundation of China (No. 81473363) and Beijing University of Chinese Medicine Special Foundation for Young Teachers (No. 2015-JYB-QNJSZX002).
Conflict of interest
All of the authors, Pengyue Li, Jie Bai, Boyu Dong, Yang Lu, Shengwei Zhang, Shuang Guo, Ning Tan, Mengdi Zhao, Shouying Du, Puning Cao declare no conflict of interest.
Ethical approval
The animal experiments were conducted according to approval of Institutional Animal Care and Use Committee of Chinese Medicine, and the Guiding Principles for the Care and Use of Laboratory Animal were followed.
Rights and permissions
About this article
Cite this article
Li, P., Bai, J., Dong, B. et al. In Vivo Pharmacokinetics of Puerarin via Different Drug Administration Routes Based on Middle Cerebral Artery Occlusion Model. Eur J Drug Metab Pharmacokinet 42, 719–727 (2017). https://doi.org/10.1007/s13318-016-0388-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13318-016-0388-4