Abstract
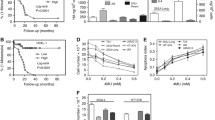
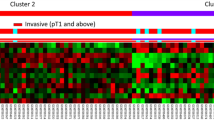
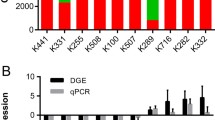
Via data mining a published transcriptomic database of UBUC (GSE31684), we discovered hyaluronan synthase-3 (HAS3) as the most significant gene stepwise downregulated from early tumorigenesis to progression among those associated with hyaluronan synthase activity (GO:0050501). We consequently analyzed HAS3 protein expression and their association with clinicopathological factors and survival in our well-characterized cohort of urothelial carcinoma of upper urinary tract (UTUC) and urinary bladder (UBUC). HAS3 expression was assessed by immunohistochemistry and evaluated by using H score method in 295 UBUCs and 340 UTUCs, respectively. HAS3 protein expression statuses were further correlated with clinicopathological parameters and evaluated the prognostic significance for disease-specific survival (DSS) and metastasis-free survival (MeFS). HAS3 protein underexpression was significantly associated with advanced pT status, nodal metastasis, high histological grade, vascular invasion, and frequent mitoses in both groups of UCs. HAS3 underexpression not only predicted poorer DSS and MeFS with univariate analysis, but also indicated dismal DSS and MeFS in multivariate analysis. HAS3 underexpression is associated with advanced tumor stage and adverse pathological features, as well as implies inferior clinical outcomes for both groups of patients with UTUCs and UBUCs, suggesting its critical role in tumor progression in UCs and may serve as a prospective prognostic biomarker and a novel therapeutic target in UCs.



Similar content being viewed by others
References
Eble JN, Sauter G, Epstein JI, Sesterhenn IA. World Health Organization classification of tumours. Pathology and genetics of tumours of the urinary system and male genital organs. Lyon: International Agency for Research on Cancer (IARC) press; 2004.
Ploeg M, Aben KK, Kiemeney LA. The present and future burden of urinary bladder cancer in the world. World J Urol. 2009;27(3):289–93. doi:10.1007/s00345-009-0383-3.
Roupret M, Zigeuner R, Palou J, Boehle A, Kaasinen E, Sylvester R, et al. European guidelines for the diagnosis and management of upper urinary tract urothelial cell carcinomas: 2011 update. Eur Urol. 2011;59(4):584–94. doi:10.1016/j.eururo.2010.12.042.
McLaughlin JK, Silverman DT, Hsing AW, Ross RK, Schoenberg JB, Yu MC, et al. Cigarette smoking and cancers of the renal pelvis and ureter. Cancer Res. 1992;52(2):254–7.
Shinka T, Miyai M, Sawada Y, Inagaki T, Okawa T. Factors affecting the occurrence of urothelial tumors in dye workers exposed to aromatic amines. Int J Urol. 1995;2(4):243–8.
Pommer W, Bronder E, Klimpel A, Helmert U, Greiser E, Molzahn M. Urothelial cancer at different tumour sites: role of smoking and habitual intake of analgesics and laxatives. Results of the Berlin Urothelial Cancer Study. Nephrol Dial Transplant. 1999;14(12):2892–7.
Dragicevic D, Djokic M, Pekmezovic T, Micic S, Hadzi-Djokic J, Vuksanovic A, et al. Survival of patients with transitional cell carcinoma of the ureter and renal pelvis in Balkan endemic nephropathy and non-endemic areas of Serbia. BJU Int. 2007;99(6):1357–62. doi:10.1111/j.1464-410X.2007.06793.x.
Debelle FD, Vanherweghem JL, Nortier JL. Aristolochic acid nephropathy: a worldwide problem. Kidney Int. 2008;74(2):158–69. doi:10.1038/ki.2008.129.
Laing C, Hamour S, Sheaff M, Miller R, Woolfson R. Chinese herbal uropathy and nephropathy. Lancet. 2006;368(9532):338. doi:10.1016/S0140-6736(06)69079-X.
Stewart JH, Hobbs JB, McCredie MR. Morphologic evidence that analgesic-induced kidney pathology contributes to the progression of tumors of the renal pelvis. Cancer. 1999;86(8):1576–82.
Zhang Z, Furge KA, Yang XJ, Teh BT, Hansel DE. Comparative gene expression profiling analysis of urothelial carcinoma of the renal pelvis and bladder. BMC Med Genet. 2010;3:58. doi:10.1186/1755-8794-3-58.
Catto JW, Azzouzi AR, Rehman I, Feeley KM, Cross SS, Amira N, et al. Promoter hypermethylation is associated with tumor location, stage, and subsequent progression in transitional cell carcinoma. J Clin Oncol. 2005;23(13):2903–10. doi:10.1200/JCO.2005.03.163.
Catto JW, Yates DR, Rehman I, Azzouzi AR, Patterson J, Sibony M, et al. Behavior of urothelial carcinoma with respect to anatomical location. J Urol. 2007;177(5):1715–20. doi:10.1016/j.juro.2007.01.030.
Liotta LA, Stetler-Stevenson WG. Tumor invasion and metastasis: an imbalance of positive and negative regulation. Cancer Res. 1991;51(18):5054s–9s.
Sironen RK, Tammi M, Tammi R, Auvinen PK, Anttila M, Kosma VM. Hyaluronan in human malignancies. Exp Cell Res. 2011;317(4):383–91. doi:10.1016/j.yexcr.2010.11.017.
Nykopp TK, Rilla K, Tammi MI, Tammi RH, Sironen R, Hamalainen K, et al. Hyaluronan synthases (HAS1-3) and hyaluronidases (HYAL1-2) in the accumulation of hyaluronan in endometrioid endometrial carcinoma. BMC Cancer. 2010;10:512. doi:10.1186/1471-2407-10-512.
Teng BP, Heffler MD, Lai EC, Zhao YL, LeVea CM, Golubovskaya VM, et al. Inhibition of hyaluronan synthase-3 decreases subcutaneous colon cancer growth by increasing apoptosis. Anti Cancer Agents Med Chem. 2011;11(7):620–8.
Siiskonen H, Poukka M, Tyynela-Korhonen K, Sironen R, Pasonen-Seppanen S. Inverse expression of hyaluronidase 2 and hyaluronan synthases 1–3 is associated with reduced hyaluronan content in malignant cutaneous melanoma. BMC Cancer. 2013;13:181. doi:10.1186/1471-2407-13-181.
Kultti A, Zhao C, Singha NC, Zimmerman S, Osgood RJ, Symons R, et al. Accumulation of extracellular hyaluronan by hyaluronan synthase 3 promotes tumor growth and modulates the pancreatic cancer microenvironment. BioMed Res Int. 2014;2014:817613. doi:10.1155/2014/817613.
Liu N, Gao F, Han Z, Xu X, Underhill CB, Zhang L. Hyaluronan synthase 3 overexpression promotes the growth of TSU prostate cancer cells. Cancer Res. 2001;61(13):5207–14.
Nykopp TK, Rilla K, Sironen R, Tammi MI, Tammi RH, Hamalainen K, et al. Expression of hyaluronan synthases (HAS1-3) and hyaluronidases (HYAL1-2) in serous ovarian carcinomas: inverse correlation between HYAL1 and hyaluronan content. BMC Cancer. 2009;9:143. doi:10.1186/1471-2407-9-143.
Huang WW, Huang HY, Liao AC, Shiue YL, Tai HL, Lin CM, et al. Primary urothelial carcinoma of the upper tract: important clinicopathological factors predicting bladder recurrence after surgical resection. Pathol Int. 2009;59(9):642–9. doi:10.1111/j.1440-1827.2009.02420.x.
Budwit-Novotny DA, McCarty KS, Cox EB, Soper JT, Mutch DG, Creasman WT, et al. Immunohistochemical analyses of estrogen receptor in endometrial adenocarcinoma using a monoclonal antibody. Cancer Res. 1986;46(10):5419–25.
McClelland RA, Finlay P, Walker KJ, Nicholson D, Robertson JF, Blamey RW, et al. Automated quantitation of immunocytochemically localized estrogen receptors in human breast cancer. Cancer Res. 1990;50(12):3545–50.
Rogers HJ. The structure and function of hyaluronate. Biochem Soc Symp. 1961;20:51–79.
Menzel EJ, Farr C. Hyaluronidase and its substrate hyaluronan: biochemistry, biological activities and therapeutic uses. Cancer Lett. 1998;131(1):3–11.
Hamann KJ, Dowling TL, Neeley SP, Grant JA, Leff AR. Hyaluronic acid enhances cell proliferation during eosinopoiesis through the CD44 surface antigen. J Immunol. 1995;154(8):4073–80.
Ahrens T, Assmann V, Fieber C, Termeer C, Herrlich P, Hofmann M, et al. CD44 is the principal mediator of hyaluronic-acid-induced melanoma cell proliferation. J Investig Dermatol. 2001;116(1):93–101. doi:10.1046/j.1523-1747.2001.00236.x.
Bourguignon LY, Zhu H, Chu A, Iida N, Zhang L, Hung MC. Interaction between the adhesion receptor, CD44, and the oncogene product, p185HER2, promotes human ovarian tumor cell activation. J Biol Chem. 1997;272(44):27913–8.
Tsatas D, Kanagasundaram V, Kaye A, Novak U. EGF receptor modifies cellular responses to hyaluronan in glioblastoma cell lines. J Clin Neurosci: Off J Neurosurg Soc Aust. 2002;9(3):282–8.
Lakshman M, Subramaniam V, Jothy S. CD44 negatively regulates apoptosis in murine colonic epithelium via the mitochondrial pathway. Exp Mol Pathol. 2004;76(3):196–204. doi:10.1016/j.yexmp.2003.12.009.
Lakshman M, Subramaniam V, Rubenthiran U, Jothy S. CD44 promotes resistance to apoptosis in human colon cancer cells. Exp Mol Pathol. 2004;77(1):18–25. doi:10.1016/j.yexmp.2004.03.002.
Voelcker V, Gebhardt C, Averbeck M, Saalbach A, Wolf V, Weih F, et al. Hyaluronan fragments induce cytokine and metalloprotease upregulation in human melanoma cells in part by signalling via TLR4. Exp Dermatol. 2008;17(2):100–7. doi:10.1111/j.1600-0625.2007.00638.x.
Yu Q, Stamenkovic I. Localization of matrix metalloproteinase 9 to the cell surface provides a mechanism for CD44-mediated tumor invasion. Genes Dev. 1999;13(1):35–48.
Yu Q, Stamenkovic I. Cell surface-localized matrix metalloproteinase-9 proteolytically activates TGF-beta and promotes tumor invasion and angiogenesis. Genes Dev. 2000;14(2):163–76.
Sugahara KN, Hirata T, Hayasaka H, Stern R, Murai T, Miyasaka M. Tumor cells enhance their own CD44 cleavage and motility by generating hyaluronan fragments. J Biol Chem. 2006;281(9):5861–8. doi:10.1074/jbc.M506740200.
Itano N, Atsumi F, Sawai T, Yamada Y, Miyaishi O, Senga T, et al. Abnormal accumulation of hyaluronan matrix diminishes contact inhibition of cell growth and promotes cell migration. Proc Natl Acad Sci U S A. 2002;99(6):3609–14. doi:10.1073/pnas.052026799.
Niedworok C, Kretschmer I, Rock K, Vom Dorp F, Szarvas T, Hess J, et al. The impact of the receptor of hyaluronan-mediated motility (RHAMM) on human urothelial transitional cell cancer of the bladder. PLoS One. 2013;8(9):e75681. doi:10.1371/journal.pone.0075681.
Acknowledgments
This study is supported by Chi Mei Medical Center, Ministry of Health and Welfare (Health and Welfare surcharge of tobacco products, MOHW104-TDU-B-212-124-003), and Kaohsiung Medical University (KMU-TP103G01,KMU-TP103G00, KMU-TP103G04 & KMU-TP103G05).
Conflicts of interest
None
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Chang, IW., Liang, PI., Li, CC. et al. HAS3 underexpression as an indicator of poor prognosis in patients with urothelial carcinoma of the upper urinary tract and urinary bladder. Tumor Biol. 36, 5441–5450 (2015). https://doi.org/10.1007/s13277-015-3210-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13277-015-3210-z