Abstract
Transarterial chemoembolization (TACE) therapy is an effective locoregional anticancer treatment for liver cancer patients. Serum biomarkers involved in immunogenic cell death may be valuable for early predicting therapy response and estimating prognosis. Sera of 50 prospectively and consecutively included hepatocellular carcinoma (HCC) patients, undergoing TACE therapy, were taken before and 24 h after TACE application. In these samples, soluble biomarkers involved in immunogenic cell death, and among them, high-mobility group box 1 (HMGB1), soluble receptor of advanced glycation end products (sRAGE), and DNase activity were measured. They were compared with radiological response to therapy. A total of 71 TACE therapies were evaluated, of which 32 were classified as “no progression,” and 39, as “progression.” While HMGB1 levels increased already 24 h after TACE, there was an early decrease of sRAGE and DNase activity. Pretherapeutic and 24-h values of sRAGE were significantly higher in the no progression group than those in the progression group. There was no difference with respect to treatment response for DNase and HMGB1. Soluble RAGE is a new parameter with predictive relevance in primary liver cancer patients undergoing TACE therapy.
Similar content being viewed by others
Introduction
Every year, more than 700,000 patients are diagnosed with hepatocellular cancers (HCC), making it the number five concerning cancer incidence and number three concerning cancer-related mortality worldwide [1, 2]. Due to the high prevalence of risk factors, such as diabetes, hepatitis C, and liver cirrhosis, HCC rates are particularly increasing in industrialized countries [3, 4]. Because HCC often is detected in late stages, curative therapy approaches like resection, liver transplantation, and radiofrequency ablation (RFA) are often not applicable [5, 6]. However, even in advanced stages of HCC, beside external beam radiotherapy [7], transarterial chemoembolization (TACE) has shown to be effective. As the tumor is mainly fed by the hepatic artery, the local application of cytotoxic drugs, iodized oil, and embolic material leads to ischemic necrosis and tumor shrinkage. In contrast, normal liver tissue that is nourished by the portal vein is greatly spared [8, 9].
However, as extensive tumor necrosis is only induced in 30–50 % of the patients [5], predictive and prognostic markers are needed for pretherapeutic stratification of the patients and for potentially early modification during the therapy. Up to date, clinical parameters like tumor size, portal invasion, ascites, performance status, and Child-Pugh score, as well as laboratory parameters bilirubin and alpha fetoprotein (AFP), have been reported as pretherapeutic prognostic and predictive parameters [10]. In addition, computed (CT) and magnetic resonance tomography (MRI) have demonstrated to indicate insufficient therapy response within 1 or 2 months [11–13]. Further promising candidates are blood-based biochemical biomarkers that are related to the organ, the tumor, or to the effect of therapy for they are measured noninvasively and cost-effectively also in serial determinations [14]. As cell death is effectively induced by diverse cytotoxic drugs, biomarkers reflecting necrotic and apoptotic processes are supposed as appropriate parameters that indicate the therapeutic efficacy already during the first days after drug application [15–17].
Indeed, cell death markers nucleosomes and cytokeratin-19 fragments (CYFRA 21–1) were found to enable specific and sensitive estimation of response to first-line chemotherapy in lung cancer patients already after the first cytotoxic drug administration [18, 19]. In HCC patients undergoing TACE therapy, serum levels of nucleosomes were elevated just 24 h after TACE treatment and were associated with later therapy response [20]. As the increase of serum nucleosomes may result from enhanced release into blood or reduced elimination from circulation, we here investigated the rate of serum DNase activity reduction during TACE and its relation to therapy response and prognosis. This seems to be relevant as DNase is not only involved in the hydrolysis of nuclear nucleosomal DNA in apoptotic cells but also present in the blood and potentially important for the degradation of circulating nucleosomes [21].
High-mobility group box 1 (HMGB1) is a nuclear protein that is closely associated to the chromatin and plays an essential role in the regulation of transcription processes [22, 23]. Recent studies indicate that HMGB1 is not only released during necrotic but also during late apoptotic cell death. Then, HMGB1 is strongly attached to the chromatin resulting in a release within HMGB1-nucleosome complexes [24]. In the blood circulation, HMGB1 is known to act as a danger-associated molecular pattern (DAMP) protein that binds to specific immune cells and promotes phagocytation and presentation of pathogenic cell death products and stimulation of immune responses [22, 25]. Those effects are mediated by HMGB1 binding to specific receptors on dendritic or antigen-presenting cells such as the receptor of advanced glycation end products (RAGE) or the toll-like receptors 4 (TLR4), particularly in conjunction with bacterial lipopolysaccharides, and to TLR2 as complexes with nucleosomes [23, 26]. In cancer diseases, tumor-related particles are phagocytized, processed intracellularly, and cross-presented at the cellular surface which leads to promotion of tumor-specific cytotoxic T cell response [17, 25, 27]. During recent years, there is growing evidence that DAMP release during this form of “immunogenic cell death,” which may be based on biochemical features of necrosis and apoptosis, is crucial for the sustained effects of chemotherapy [27–29]. In contrast, knockdown or neutralization of HMGB1 or TLR4 induces reduced anticancer immune response both in vitro and in vivo and poor therapy outcome [25, 27–29]. Nevertheless, it is still not clear whether the serum levels of HMGB1 have prognostic or predictive relevance in cancer diseases [30, 31].
Beyond triggering the protective T cell response, HMGB1 is also known to promote neoangiogenesis [15, 32]. Overexpression of HMGB1 and its receptor RAGE is further important for invasion and metastasis of tumors, as seen in gastric and colorectal cancers [33]. In contrast, serum levels of RAGE have been found to be decreased in some cancer entities [34, 35]. These findings may show the double role of RAGE, being involved as a surface receptor in the transmission of DAMP signals on the one side and acting as a decoy receptor for circulating DAMPs when shed from the cellular surface. Alternatively, it may simply correlate with a high expression of cellular RAGE [36–38]. Here, this new and challenging set of markers involved in cell death, tumor growth, and immunogenicity is investigated in HCC patients to identify their role in prediction of response to TACE therapy during the early treatment phase.
Methods
Patients
In total, 50 HCC patients (42 males and eight females, mean age 66.7 years) were prospectively and consecutively included in the present study. All patients were diagnosed and staged at the University Hospital Munich-Grosshadern between 2006 and 2008. Patient characteristics are summarized in Table 1. Median age of the patients was 66.7 years (range 45–84 years). Diagnosis of HCC was confirmed by a fine needle biopsy or by radiological criteria (two coincident imaging techniques) or combined criteria (one imaging technique associated with elevated AFP levels according to the Barcelona EASL Conference 2000 criteria; [39]). The 50 patients received a total of 77 TACE therapies.
For evaluation of response to therapy, only 44 patients with 71 TACE therapies were included because six patients received TACE therapy 1 day prior to radiofrequency ablation and had to be excluded due to possible confounding effects. The study was approved by the local ethics committee, and written informed consent was obtained from each patient before the first blood drawing.
Treatment procedures
All TACE procedures were performed under angiographic control (Multistar TOP and Axiom Artis dTA, Siemens, Munich, Germany) and under local anesthesia. After inserting a 4-French (Fr) pigtail catheter into the femoral artery via a microincision into the groin, a panviscerography was performed to detect potentially aberrant or additional hepatic and possibly tumor-feeding arteries. After identifying the tumor-feeding arteries, a 4-Fr catheter (e.g., cobra configuration) for selective use or a superselective microcatheter, which could be placed through the primary 4-Fr catheter, was directed as close as possible to the tumor-feeding vessels. The embolizing moiety was prepared by extensive mixing between two syringes, typically 3–5 mL Lipiodol, microparticles of 150–500 μm (e.g., Contour SE®, Boston Scientific, Ratingen, Germany) and Farmorubicin (1 mg/kg b.w.). Subsequently, the embolizing agent was slowly injected under fluoroscopic control to avoid retrograde embolization of nontarget areas due to back spill. As soon as stasis within the tumor vessels occurred, the injection was stopped. Treatment was terminated if a flow within the tumor vessels was no longer detectable, over 5–10 min. Otherwise, another injection was performed. In cases of several main feeders, those vessels were treated subsequently.
Classification of response to therapy
In all patients, staging investigations were performed before the start of the next TACE therapy, consisting of abdominal CT or MRI and laboratory examinations. The median evaluation time of therapy response was 70 days after TACE. The response to therapy was classified according to RECIST criteria for solid tumors defining “complete remission” as complete disappearance of all such manifestations of disease, “partial remission” as reduction of tumor diameter of ≥30 %, “progression” as tumor increase of ≥20 % or appearance of new tumor manifestations, and “stable disease” as tumor reduction of <30 % or increase of <20 % in medical imaging [40]. For evaluation, partial remission and stable disease were joined into the “no progression” group and compared with progressive patients.
Sample collection and assays
Blood samples of all participating patients were collected prospectively before TACE and 24 h after TACE. The blood samples were centrifuged at 3,000 × g for 15 min within 1 to 2 h after venipuncture. Subsequently, aliquots of serum samples were stored at −80 °C. Later, samples were analyzed in batches. All samples of a patient always were measured in one run to avoid interassay variations. To control the quality of the assays, serum pools of diverse levels were included in all assays.
The quantification of serum DNase activity was performed by a solid-phase enzyme immunoassay (ELISA) of Orgentec Diagnostika GmbH (Mainz, Germany), which measured the reduction of activity of desoxyribonuclease. Pathologic samples are supposed to exhibit a higher activity reduction (%AR), which means lower DNase activities. HMGB1 concentration was measured by use of a Sandwich ELISA from SHINO-Test/IBL (Tokyo, Japan/Hamburg, Germany). Levels of sRAGE were measured by use of the Quantikine® Colorimetric Sandwich Elisa of R&D Systems (Abingdon, UK), all according to the instructions of the manufacturers.
Prior to this study, RAGE and HMGB1 assays were tested on their methodical quality including the intra- and interassay imprecision and dilution linearity of the assay as well as some influencing factors like freeze-thawing, use of different materials (serum/plasma), and storage at diverse temperatures and times before and after centrifugation on RAGE and HMGB1 values. Thereby, both assays showed good methodical quality and robustness against preanalytic influences [41, 42]. Similar results were obtained for the DNase assay in an internal evaluation.
Statistics
Concentrations of all measured markers before and 24 h after TACE, as well as their percentage changes, were considered for statistical evaluation. Kinetics of marker changes during therapy are described. Correlations between pretherapeutic levels of immunogenic markers, as well as other organ, cancer, inflammation, and cell death markers, were calculated by Spearman’s rank correlation test. Concerning evaluation of response to therapy, partial remission and stable disease were joined into the no progression group and compared to patients who suffered from progressive disease (progression group). Marker concentrations between these two groups were compared by means of the Wilcoxon test. A p value of <0.05 was considered statistically significant. All calculations were performed by software of SAS (version 9.2, SAS Institute Inc., Cary, NC, USA).
Results
Kinetics of the markers
Already 24 h after application of TACE, median concentration of HMGB1 significantly increased from 1.7 to 2.3 ng/mL with a median percentual increase of 60.4 %. Median DNase activity reduction values increased as well, from 18.0 % AR before treatment to 20.3 % AR after treatment. This corresponds with slightly lower DNase activities after TACE (median reduction of −15.8 %). Similarly, median sRAGE values slightly decreased after TACE from 1.03 ng/mL before to 1.02 ng/mL after therapy (−5.6 %) (Table 2; Fig. 1).
Correlation of the markers
Concerning tumor stage, significantly lower pretherapeutic RAGE levels were found in T3 than in T1 and T2 tumors (p = 0.019), while for the other markers and 24 h values, no correlation with T stage was found. Concerning other markers, pretherapeutic DNase activity reduction levels inversely correlated with levels of AFP (R = −0.27; p = 0.016), lactate dehydrogenase (LDH; R = −0.31; p = 0.006), aspartate aminotransferase (R = −0.36; p = 0.001), bilirubin (R = −0.33; p = 0.004), alkaline phosphatase (R = −0.35; p = 0.002), amylase (R = −0.39; p < 0.001), lipase (R = −0.46; p < 0.001), and choline esterase (R = −0.62; p < 0.001), which were available from earlier studies [20]. Pretherapeutic HMGB levels strongly correlated with nucleosomes (R = 0.61; p < 0.001), CYFRA 21–1 (R = 0.41; p < 0.001), C-reactive protein (R = 0.44; p < 0.001), bilirubin (R = 0.33; p = 0.004), and gamma-glutamyltransferase (GGT; R = 0.26; p = 0.026) and inversely with CHE levels (R = −0.25; p = 0.029). sRAGE inversely correlated with nucleosome (R = −0.23; p = 0.039), alanine aminotransferase (R = −0.28; p = 0.013), and GGT levels (R = −0.29; p = 0.010). Similar correlations were seen 24 h after TACE; in addition, HMGB1 strongly correlated with cell death marker LDH (R = 0.40; p < 0.001).
Correlation with therapy response
For evaluation of response to TACE therapy, 71 therapies of 44 patients were included. Radiological staging investigations after a median of 70 days after TACE showed 32 TACE treatments having been successful (30 stable disease, two partial remission, no progression group), while the outcome of the remaining 39 treatments was progressive disease (progression group).
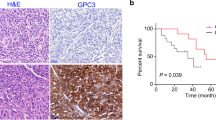
Concerning clinical factors, age, gender, and T stage did not significantly affect the outcome of the therapy. However, the number of TACE cycles correlated with progressive disease (p = 0.027) [20]. Comparing therapy response with the three measured markers, only the pretherapeutic and 24-h values of the multiligand receptor sRAGE indicated later response to therapy. Lower sRAGE levels were significantly associated with progressive disease during therapy (p = 0.029 and 0.041, respectively) (Table 3; Fig. 2).
DNase and HMGB1 levels were not associated with response to therapy. Although the median values of DNase activity reduction were somewhat lower in the progressive patient group before and 24 h after therapy, they did not reach the level of significance. The median values of HMGB1 were quite similar in both response groups before and 24 h after TACE and did not indicate later therapy response (Table 3; Fig. 2).
Discussion
Although the introduction of screening programs in patients with major risk factors like HBV or HCV infection led to earlier diagnosis of HCC, most liver cancer patients are still diagnosed in advanced stages of disease [5, 43]. Since those patients cannot be treated anymore with a curative approach by surgery or ablative therapies, TACE is a widely recognized and accepted treatment option that, recently, has been shown to improve survival as compared with the best supportive care [8, 9]. As only some of patients benefit from TACE therapy, prognostic and predictive markers are needed in order to identify those patients who are most likely to respond to the therapy.
After application of TACE, CT and MRI are the most frequently used methods to evaluate the therapeutic efficacy [11–13]. Because macroscopic changes in tumor volume often occur only after several months and those diagnostics are quite expensive, blood-based biochemical markers that provide early and specific information on the response to therapy would be ideal [14–17]. This would enable effective modifications or intensifications of the therapy such as by the use of sorafenib or other targeted agents on an individual basis [44]. Beyond therapy response, the outcome in terms of survival is even more relevant for the single patient. Several scoring systems, like Barcelona Clinic Liver Cancer, Cancer of the Liver Italian Program, and Japanese Integrated Staging, have been established as informative prognostic tools that mainly based on clinical variables and liver parameters [45]. In order to improve those already existing models, new biochemical markers are needed, which reflect the tumor biology and early therapy effects. Among others, blood-based cell death biomarkers, such as circulating nucleosomes, have shown to be useful for therapy prediction and prognosis [14–17]. Recently, we observed elevated serum nucleosome levels in HCC patients as compared with healthy controls and those levels further increased already 24 h after TACE therapy. In addition, the levels of circulating nucleosomes 24 h after TACE indicated later treatment response with high values being associated with poor therapy outcome [20].
Because the enzyme DNase catalyzes the hydrolyzation of chromatin to shorter nucleosomal fragments during apoptotic cell death and because it is supposed to play a relevant role in the clearance of nucleosomes from the blood, it seemed to be a promising additional marker in our setting. As expected, the activity of DNase was reduced 24 h after TACE therapy; however, there was no difference between the groups of patients with favorable or insufficient efficacy of therapy. This observation was surprising as in an earlier study on head and neck cancer patients, DNase activity was higher in patients with response to therapy than that in patients who suffered from therapy progression [46]. Further, it is known that serum nucleosome levels are elevated in cancer disease and correlate with poor therapy response and prognosis [16, 18, 47, 48]. Therefore, it could be assumed that patients with advanced cancers and with poor prognosis would have a lower DNase activity (higher AR%) that leads to a reduced elimination of DNA and nucleosomes from the blood circulation. Eventually, our findings may be explained by the dramatically increased release of nucleosomes in patients with poor survival causing a maximum upregulation of DNase activity, particularly in those patients. Indeed, high nucleosome levels 24 h after TACE were observed in nonresponsive patients and in those with unfavorable prognosis—possibly despite an upregulated DNase activity [20, 49].
An immunogenic cell death pathway is supposed to be crucial for sufficient therapy response after cytotoxic therapies [27–29]. This pathway includes the active secretion of the DNA-binding nuclear protein HMGB1 upon cytokine stimulation or its passive release during cell death [22–24]. Indeed, HMGB1 levels were increased already 24 h after TACE therapy. Similar kinetics were seen for circulating nucleosomes in an earlier study [20]. Interestingly, HMGB1 strongly correlated with nucleosomes before and 24 h after TACE. However, there was no difference in HMGB1 levels between patient groups with good and poor responses to therapy. In earlier studies, elevated HMGB1 expression levels were reported in diverse cancers, including colon, prostate, pancreatic, breast cancer, and melanoma [17, 30, 31, 41, 50]. Further, HMGB1 was associated with invasion and metastasis and was proposed as prognostic factor in gastric, lung, and liver cancer patients [30, 50, 51], while other studies did not find a prognostic value for HMGB1 [31].
Beyond TLR2 and TLR4, RAGE is the most relevant receptor of circulating HMGB1 for mediating immune effects. In addition, cellular RAGE plays an important role in regulating the invasiveness of tumor cells [17, 32, 37]. Whether soluble RAGE shed from the cellular surface simply corresponds with its cellular expression and is upregulated in cancer disease or whether it acts as a decoy receptor for circulating HMGB1 and is downregulated in cancer disease is still in debate [36–38]. While some groups have found higher rates of RAGE in hepatocellular cancer tissue [52, 53], we here describe lower serum RAGE values being highly relevant indicators for poor therapy response in HCC patients undergoing TACE. These results are in line with other studies that have reported decreased RAGE values in cancer disease [34, 35] and support the decoy receptor hypothesis of RAGE. If lower levels of soluble RAGE are present in advanced cancer stages and are further lowered by cytotoxic therapy, HMGB1 may exert its functions as DAMP more efficiently and lead to a nonfavorable, general inflammatory state that, in consequence, leads to the poor outcome of the patients [36–38].
As drawbacks of the present study, the limited number of patients and the scatter in the intervals of determining therapy response may be mentioned. Although most patients have been screened before they received the next TACE treatment or at radiological control exams between 60 and 90 days after TACE treatment, there were some exceptions. One person died already 22 days after TACE due to the cancer disease and was therefore classified as nonresponder. Another patient did not return to hospital due to his good physical condition and only was staged after 216 days. In total, there were only four patients with staging intervals more than 4 months of who two responded well to therapy.
However, as particular strength of the study, it has to be emphasized that all patients were included prospectively and with no other selection criteria as indicated into the study. Further, serial blood drawings were done in all patients during the first TACE day, and all preanalytical and analytical steps were strictly controlled, resulting in a high quality of the data presented. It will be highly interesting to include those immunogenic biomarkers also in systemic and targeted therapeutic approaches in HCC patients [54].
Conclusions
The present study reveals for the first time the effect of TACE therapy on serum levels of the immunogenic cell death markers HMGB1, sRAGE, and DNase in HCC patients. Soluble RAGE levels were found to be related to therapy response of the patients and may be included in further validation studies.
References
Parkin DM, Bray F, Ferlay J, Pisani P. Estimating the world cancer burden: Globocan 2000. Int J Cancer. 2001;94:153–6.
El-Serag HB, Rudolph L. Hepatocellular carcinoma: epidemiology and molecular carcinogenesis. Gastroenterol. 2007;132:2557–76.
Jepsen P, Vilstrup H, Tarone RE, Friis S, Sorensen HT. Incidence rates of hepatocellular carcinoma in the US and Denmark: recent trends. Int J Cancer. 2007;121:1624–6.
Yuan JM, Govindarajan S, Arakawa K, Yu MC. Synergism of alcohol, diabetes, and viral hepatitis on the risk of hepatocellular carcinoma in blacks and whites in the US. Cancer. 2004;101:1009–17.
El-Serag HB, Marrero JA, Rudolph L, Reddy KR. Diagnosis and treatment of hepatocellular carcinoma. Gastroenterol. 2008;134:1752–63.
Forner A, Hessheimer AJ, Real MI, Bruix J. Treatment of hepatocellular carcinoma. Crit Rev Oncol Hematol. 2006;60:89–98.
Hoffe SE, Finkelstein SE, Russel MS, Shridhar S. Nonsurgical options for hepatocellular carcinoma: evolving role of external beam radiotherapy. Cancer Control. 2010;17:100–10.
Llovet JM, Bruix J. Systematic review of randomized trials for unresectable hepatocellular carcinoma: chemoembolization improves survival. Hepatol. 2003;37:429–42.
Takayasu K, Arii S, Ikao I, Omata M, Okita K, Ichida T, Matsuyama Y, Nakanuma Y, Kojiro M, Makuuchi M, Yamaoka Y. Prospective cohort study of transarterial chemoembolization for unresectable hepatocellular carcinoma in 8510 patients. Gastroenterol. 2006;131:461–9.
Bruix JSM, Llovet JM. Chemoembolization for hepatocellular carcinoma. Gastroenterol. 2004;127:179–88.
Lim HS, Jeong YY, Kang HK, Kim JK, Park JG. Imaging features of hepatocellular carcinoma after transcatheter arterial chemoembolization and radiofrequency ablation. Am J Roentgenol. 2006;187:W341–9.
Takayasu K, Arii S, Matsuo N, Yoshikawa M, Ryu M, Takasaki K, Sato M, Yamanaka N, Shimamura Y, Ohto M. Comparison of CT findings with resected specimens after chemoembolization with iodized oil for hepatocellular carcinoma. Am J Roentgenol. 2000;175:699–704.
Thabet A, Kalva S, Gervais DA. Percutaneous image-guided therapy of intra-abdominal malignancy: imaging evaluation of treatment response. Abdom Imaging. 2009;34:593–609.
Beachy SH, Repasky EA. Using extracellular biomarkers for monitoring efficacy of therapeutics in cancer patients: an update. Cancer Immunol Immunother. 2008;57:759–75.
Holdenrieder S, Stieber P. Apoptotic markers in cancer. Clin Biochem. 2004;37:605–17.
Holdenrieder S, Stieber P. Clinical use of circulating nucleosomes. Crit Rev Lab Med Sci. 2009;46:1–24.
Sims GP, Rowe DC, Rietdijk ST, Herbst R, Coyle AJ. HMGB1 and RAGE in inflammation and cancer. Annu Rev Immunol. 2010;28:367–88.
Holdenrieder S, Stieber P, von Pawel J, Raith H, Nagel D, Feldmann K, Seidel D. Circulating nucleosomes predict the response to chemotherapy in patients with advanced non small cell lung cancer. Clin Cancer Res. 2004;10:5981–7.
Holdenrieder S, Stieber P, von Pawel J, Raith H, Nagel D, Feldmann K, Seidel D. Early and specific prediction of the therapeutic efficacy in lung cancer by nucleosomal DNA and cytokeratin 19 fragments. Ann N Y Acad Sci. 2006;1075:244–75.
Kohles N, Nagel D, Jungst D, Durner J, Stieber P, Holdenrieder S. Relevance of circulating nucleosomes and oncological biomarkers for predicting response to transarterial chemoembolization therapy in liver cancer patients. BMC Cancer. 2011;11:202.
Zhang JH, Xu M. Apoptotic DNA fragmentation and tissue homeostasis. Trends Cell Biol. 2002;12:84–9.
Lotze MT, Tracey KJ. High-mobility group box 1 protein (HMGB1): nuclear weapon in the immune arsenal. Nat Rev Immunol. 2005;5:331–42.
Bianchi ME. HMGB1 loves company. J Leukocyte Biol. 2009;86:573–6.
Urbonaviciute V, Furnrohr BG, Meister S, Munoz L, Heyder P, De Marchis F, Bianchi ME, Kirschning C, Wagner H, Manfredi AA, Kalden JR, Schett G, et al. Induction of inflammatory and immune responses by HMGB1-nucleosome complexes: implications for the pathogenesis of SLE. J Exp Med. 2008;205:3007–18.
Tesniere A, Panaretakis T, Kepp O, Apetoh L, Ghiringhelli F, Zitvogel L, Kroemer G. Molecular characteristics of immunogenic cancer cell death. Cell Death Diff. 2008;15:3–12.
Park JS, Gamboni-Robertson F, He Q, Svetkauskaite D, Kim JY, Strassheim D, Sohn JW, Yamada S, Maruyama I, Banerjee A, et al. High mobility group box 1 protein interacts with multiple toll-like receptors. Am J Physiol Cell Physiol. 2006;290:917–24.
Kepp O, Tesniere A, Schlemmer F, Michaud M, Senovilla L, Zitvogel L, Kroemer G. Immunogenic cell death modalities and their impact on cancer treatment. Apoptosis. 2009;14:364–75.
Apetoh L, Ghiringhelli F, Tesniere A, Obeid M, Ortiz C, Criollo A, Mignot G, Maiuri MC, Ullrich E, Saulnier P, Yang H, Amigorena S, et al. Toll-like receptor 4-dependent contribution of the immune system to anticancer chemotherapy and radiotherapy. Nat Med. 2007;13:1050–9.
Apetoh L, Tesniere A, Ghiringhelli F, Kroemer G, Zitvogel L. Molecular interactions between dying tumor cells and the innate immune system determine the efficacy of conventional anticancer therapies. Cancer Res. 2008;68:4026–30.
Chung HW, Lee SG, Kim H, Hong DJ, Chung JB, Stroncek D, Lim JB. Serum high mobility group box-1 (HMGB1) is closely associated with the clinical and pathologic features of gastric cancer. J Transl Med. 2009;7:38.
Naumnik W, Nilklińska W, Ossolińska M, Chyczewska E. Serum levels of HMGB1, survivin, and VEGF in patients with advanced non-small cell lung cancer during chemotherapy. Folia Histochem Cytobiol. 2009;47:703–9.
Zitvogel L, Apetoh L, Ghiringhelli F, Kroemer G. Immunological aspects of cancer chemotherapy. Nat Rev Immunol. 2008;8:59–73.
Tang DL, Kang R, Zeh HJ, Lotze MT. High-mobility group box 1 and cancer. Biochim Biophys Acta. 2010;1799:131–40.
Jiao L, Weinstein SJ, Albanes D, Taylor PR, Graubard BI, Virtamo J, Stolzenberg-Solomon RZ. Evidence that serum levels of the soluble receptor for advanced glycation end products are inversely associated with pancreatic cancer risk: a prospective study. Cancer Res. 2011;71:3582–9.
Stötzer OJ, Fersching DIM, Salat C, Siegele B, Nagel D, Holdenrieder S. Prediction of response to neoadjuvant chemotherapy in breast cancer patients by circulating soluble HMGB1 and RAGE. Tumor Biol. 2012 (in press)
Bierhaus A, Nawroth PP. Multiple levels of regulation determine the role of the receptor for AGE (RAGE) as common soil in inflammation, immune responses and diabetes mellitus and its complications. Diabetologica. 2009;52:2251–63.
Sparvero LJ, Asafu-Adjei D, Kang R, Tang D, Amin N, Im J, Rutledge R, Lin B, Amoscato AA, Zeh HJ, Lotze MT. RAGE, RAGE ligands, and their role in cancer and inflammation. J Translat Med. 2010;7:17.
Geroldi D, Falcone C, Emanuele E. Soluble receptor for advanced glycation end products: from disease marker to potential therapeutic target. Curr Med Chem. 2006;13:1971–8.
Bruix J, Sherman M, Llovet JM, Beaugrand M, Lencioni R, Burroughs AK, Christensen E, Pagliaro L, Colombo M, Rodes J. Clinical management of hepatocellular carcinoma. Conclusions of the Barcelona-2000 EASL Conference. J Hepatol. 2001;35:421–30.
Therasse P, Arbuck SG, Eisenhauer EA, Wanders J, Kaplan RS, Rubinstein L, Verweij J, Van Glabbeke M, van Oosterom AT, Christian MC, Gwyther SG. New guidelines to evaluate the response to treatment in solid Tumors. J Natl Cancer Inst. 2000;92:205–16.
Lehner J, Wittwer C, Fersching D, Siegele B, Holdenrieder S, Stoetzer OJ. Methodical and preanalytical evaluation of an HMGB1 immunoassay. Anticancer Res. 2012;32:2059–62.
Wittwer C, Lehner J, Fersching D, Siegele B, Stoetzer OJ, Holdenrieder S. Methodical and preanalytical evaluation of a RAGE immunoassay. Anticancer Res. 2012;32:2075–8.
Ikai I, Arii S, Kojiro M, Ichida T, Makuuchi M, Matsuyama Y, Nakanuma Y, Okita K, Omata M, Takayasu K, Yamaoka Y. Reevaluation of prognostic factors for survival after liver resection in patients with hepatocellular carcinoma in a Japanese nationwide survey. Cancer. 2004;101:796–802.
Villanueva A, Llovet JM. Targeted therapies for hepatocellular carcinoma. Gastroenterol. 2011;140:1410–26.
LE Georgiades CS, Frangakis C, Park JU, Kim HW, Hong K, Geschwind JF. Prognostic accuracy of 12 liver staging systems in patients with unresectable hepatocellular carcinoma treated with transarterial chemoembolization. J Vasc Interv Radiol. 2006;17:1619–24.
Patel PS, Patel BP, Rawal RM, Raval GN, Patel MM, Patel JB, Jha FP, Patel DD. Evaluation of serum alkaline DNase activity in treatment monitoring of head and neck cancer patients. Tumor Biol. 2000;21:82–9.
Holdenrieder S, Stieber P, Bodenmueller H, Busch M, Fertig G, Fuerst H, Schalhorn A, Schmeller N, Untch M, Seidel D. Nucleosomes in serum of patients with benign and malignant diseases. Int J Cancer. 2001;95:114–20.
Kuroi K, Tanaka C, Toi M. Clinical significance of plasma nucleosomes levels in cancer patients. Int J Oncol. 2001;19:143–8.
Kohles N, Nagel D, Jüngst D, Durner J, Stieber P, Holdenrieder S. Prognostic value of apoptotic and oncological biomarkers in liver cancer patients undergoing transarterial chemoembolisation therapy. Tumor Biol. 2012;33:33–40.
Shang GH, Jia CQ, Tian H, Xiao W, Li Y, Wang AH, Dong L, Lin DJ. Serum high mobility group box protein 1 as a clinical marker for non-small cell lung cancer. Respirat Med. 2009;103:1949–53.
Cheng BQ, Jia CQ, Liu CT, Lu XE, Zhong N, Zhang ZL, Fan W, Li YQ. Serum high mobility group box chromosomal protein 1 is associated with clinicopathologic features in patients with hepatocellular carcinoma. Digest Liver Dis. 2008;40:446–52.
Kostova N, Zlateva S, Ugrinova I, Pasheva E. The expression of HMGB1 protein and its receptor RAGE in human malignant tumors. Mol Cell Biochem. 2010;337:251–8.
Hiwatashi K, Ueno S, Abeyama K, Kubo F, Sakoda M, Maruyama I, Hamanoue M, Natsugoe S, Aikou T. A novel function of the receptor for advanced glycation end-products (RAGE) in association with tumorigenesis and tumor differentiation of HCC. Annals Surg Oncol. 2008;15:923–33.
Giglia JL, Antonia SJ, Berk LB, Bruno S, Dessureault S, Finkelstein SE. Systemic therapy for advanced hepatocellular carcinoma: past, present, and future. Cancer Control. 2010;17:120–9.
Acknowledgments
We are very grateful for the committed support of Prof. Jüngst who died recently. We thank Dr. Waggershauser from the Institute of Radiology of the University Hospital Munich for the excellent technical assistance in the evaluation of CT and MRI imaging.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kohles, N., Nagel, D., Jüngst, D. et al. Predictive value of immunogenic cell death biomarkers HMGB1, sRAGE, and DNase in liver cancer patients receiving transarterial chemoembolization therapy. Tumor Biol. 33, 2401–2409 (2012). https://doi.org/10.1007/s13277-012-0504-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13277-012-0504-2