Abstract
Introduction
Adherence to poison center (PC) recommendations for the management of calcium channel blocker (CCB) poisoning is inconsistent. This study aimed to identify behaviors that determine adherence to hyperinsulinemia-euglycemia therapy (HIET) for CCB poisoning.
Methods
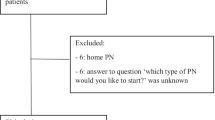
Semistructured interviews were conducted involving a convenience sample of 18 intensivists. Interview responses were analyzed using the theoretical domains framework (TDF) to identify relevant domains influencing physician adherence to HIET. Two independent reviewers performed qualitative content analysis of the interview transcripts to identify beliefs influencing decisions to initiate HIET. Initially, beliefs were classified and frequencies reported as being likely to facilitate, likely to decrease, or unlikely to affect adherence. Subsequently, beliefs were linked to a domain within the TDF. Based on the potential impact on physician behavior and frequency of reported behavior, we selected the most relevant domains likely to influence physician adherence to HIET for CCB poisoning.
Results
Positive beliefs were identified in the following domains: “behavioral regulation” (e.g., algorithm for adjustment of perfusions), “belief about capabilities” (e.g., confidence about being able to manage HIET), “belief about consequences” (e.g., fear of clinical deterioration), and “reinforcement” (e.g., clinical instability). Negative beliefs were identified in the following domains as “nature of behavior” (e.g., preference for vasopressors over HIET) and “environmental context and resources” (e.g., accessing dextrose 50% and increased nurse workload).
Conclusion
This qualitative study identified potential behavioral targets for future implementation strategies to address to improve adherence to HIET.
Similar content being viewed by others
References
Gummin DD, Mowry JB, Spyker DA, Brooks DE, Fraser MO, Banner W. Annual report of the American Association of Poison Control Centers’ National Poison Data System (NPDS): 34th annual report. Clin Toxicol. 2016;55(10):1072–254.
Greene SL, Gawarammana I, Wood DM, Jones AL, Dargan PI. Relative safety of hyperinsulinaemia/euglycaemia therapy in the management of calcium channel blocker overdose: a prospective observational study. Intensive Care Med. 2007;33(11):2019–24.
Espinoza T, Bryant SM, Aks SE. Hyperinsulin therapy for calcium channel antagonist poisoning: a seven—year retrospective study. Am J Ther. 2013;20:29–31.
Patel NP, Pugh ME, Goldberg S, Eiger G. Hyperinsulinemic euglycemia therapy for verapamil poisoning: a review. Am J Crit Care. 2007;16(5):498–503.
St-Onge M, Archambault P, Lesage N, Guimont C, Poitras J, Blais R. Adherence to calcium channel blocker poisoning treatment recommendations in two Canadian cities. Clin Toxicol (Phila). 2012;50(5):424–30.
Darracq MA, Thornton SL, Do HM BD, Clark RF, Cantrell FL. Utilization of hyperinsulinemia euglycemia and intravenous fat emulsion following poison center recommendations. J Med Toxicol. 2013;9(3):226–30.
St-Onge M, Anseeuw K, Cantrell FL, Gilchrist IC, Hantson P, Bailey B, et al. Experts consensus recommendations for the management of calcium channel blocker poisoning in adults. Crit Care Med. 2017;45(3):e306–15.
Curran J, Brehaut J, Patey A, Osmond M, Stiell I, Grimshaw J. Understanding the Canadian adult CT head rule trial: use of the theoretical domains framework for process evaluation. Implement Sci. 2013;8:25.
Kiyoshi-Teo H, Cabana MD, Froelicher ES, Blegen MA. Adherence to institution-specific ventilator-associated pneumonia prevention guidelines. Am J Crit Care. 2014;23(3):201–14.
Cabana MD, Rand CS, Powe NR, Wu AW, Wilson MH, Abboud PA, et al. Why don’t physicians follow clinical practice guidelines? A framework for improvement. JAMA. 1999;282(15):1458–65.
Grimshaw J, Eccles M, Thomas R, MacLennan G, Ramsay C, Fraser C, et al. Toward evidence-based quality improvement evidence (and its limitations) of the effectiveness of guideline dissemination and implementation strategies 1966–1998. J Gen Intern Med. 2006;21:S14–20.
Rello J, Lorente C, Bodí M, Diaz E, Ricart M, Kollef MH. Why do physicians not follow evidence-based guidelines for preventing ventilator-associated pneumonia?: a survey based on the opinions of an international panel of intensivists. Chest. 2002;122(2):656–61.
Michie S, Johnston M, Abraham C, Lawton R, Parker D, Walker A. Making psychological theory useful for implementing evidence based practice: a consensus approach. Qual Saf Health Care. 2005;14(1):26–33.
Cane J, O’Connor D, Michie S. Validation of the theoretical domains framework for use in behaviour change and implementation research. Implement Sci. 2012;7:37.
Roberts N, Hooper G, Lorencatto F, Storr W, Spivey M. Barriers and facilitators towards implementing the Sepsis Six care bundle (BLISS-1): a mixed methods investigation using the theoretical domains framework. Scand J Trauma Resusc Emerg Med. 2017;25(1):96.
Lavallée JF, Gray TA, Dumville J, Cullum N. Barriers and facilitators to preventing pressure ulcers in nursing home residents: a qualitative analysis informed by the Theoretical Domains Framework. Int J Nurs Stud. 2018;82:79–89.
Isenor JE, Minard LV, Stewart SA, Curran JA, Deal H, Rodrigues G, Sketris IS. Identification of the relationship between barriers and facilitators of pharmacist prescribing and self-reported prescribing activity using the theoretical domains framework. Res Soc Adm Pharm. 2017.
Joosen MC, van Beurden KM, Terluin B, van Weeghel J, Brouwers EP, van der Klink JJ. Improving occupational physicians’ adherence to a practice guideline: feasibility and impact of a tailored implementation strategy. BMC Med Educ. 2015;15:82.
Ista E, van Dijk M, van Achterberg T. Do implementation strategies increase adherence to pain assessment in hospitals? A systematic review. Int J Nurs Stud. 2013;50(4):552–68.
Cochrane Effective Practice and Organisation of Care Group. Effective Practice and Organisation of Care (EPOC). EPOC Taxonomy. Oslo: Norwegian Knowledge Centre for the Health Services. 2015. Available at: https://epoc.cochrane.org/epoc-taxonomy.
Mazza D, Bairstow P, Buchan H, Chakraborty SP, Van Hecke O, Grech C, et al. Refining a taxonomy for guideline implementation: results of an exercise in abstract classification. Implement Sci. 2013;8:32.
Atkins L, Francis J, Islam R, O’Connor D, Patey A, Ivers N, et al. A guide to using the Theoretical Domains Framework of behaviour change to investigate implementation problems. Implement Sci. 2017;12:77.
Francis J, Stockton C, Eccles M, Johnston M, Cuthbertson B, Grimshaw J, et al. Evidence-based selection of theories for designing behaviour change interventions: using methods based on theoretical construct domains to understand clinicians' blood transfusion behaviour. Br J Health Psychol. 2009;14:625–46.
Guest G, Bunce A, Johnson L. How many interviews are enough? An experiment with data saturation and variability. Field Methods. 2006;18(1):59–82.
Francis JJ, Johnston M, Robertson C, Glidewell L, Entwistle V, Eccles MP, et al. What is an adequate sample size? Operationalising data saturation for theory-based interview studies. Psychol Health. 2010;25(10):1229–45.
Temple B, Young A. Qualitative research and translation dilemmas. Qual Res. 2004;4(2):161–78.
van Nes F, Abma T, Jonsson H, Deeg D. Language differences in qualitative research: is meaning lost in translation? Eur J Ageing. 2010;7(4):313–6.
Bussieres AE, Patey AM, Francis JJ, Sales AE, Grimshaw J. Identifying factors likely to influence compliance with diagnostic imaging guideline recommendations for spine disorders among chiropractors in North America: a focus group study using the Theoretical Domains Framework. Implement Sci. 2012;7:82.
Ranieri VM, Thompson BT, Barie PS, Dhainaut JF, Douglas IS, Finfer S, et al. Drotrecogin alfa (activated) in adults with septic shock. N Engl Med. 2012;366(22):2055–64.
Ellington L, Sheldon LK, Matwin S, Smith JA, Poynton MM, Crouch BI, et al. An examination of adherence strategies and challenges in poison control communication. J Emerg Nurs. 2009;35(3):186–274.
Watts M, Fountain JS, Reith D, Schep L. Compliance with poisons center referral advice and implications for toxicovigilance. J Toxicol Clin Toxicol. 2004;42:603–10.
Wezorek CM, Dean BS, Krenzelok EP. Factors influencing non-compliance with poison center recommendations. Vet Hum Toxicol. 1992;34:151–3.
Weiss CH, Baker DW, Tulas K, Weiner S, Bechel M, Rademaker A, et al. A critical care clinician survey comparing attitudes and perceived barriers to low tidal volume ventilation with actual practice. Ann Am Thorac Soc. 2017;14(11):1682–9.
Cook D, Duffett M, Lauzier F, Ye C, Dodek P, Paunovic B, et al. Barriers and facilitators of thromboprophylaxis for medical-surgical intensive care unit patients: a multicenter survey. J Crit Care. 2014;29(3):471.e1–9.
Latif A, Kelly B, Edrees H, Kent PS, Weaver SJ, Jovanovic B, et al. Implementing a multifaceted intervention to decrease central line-associated bloodstream infections in SEHA (Abu Dhabi Health Services Company) intensive care units: the Abu Dhabi experience. Infect Control Hosp Epidemiol. 2015;36(7):816–22.
Islam R, Tinmouth AT, Francis JJ, Brehaut JC, Born J, Stockton C, et al. A cross-country comparison of intensive care physicians’ beliefs about their transfusion behaviour: a qualitative study using the theoretical domains framework. Implement Sci. 2012;7:93.
Cuthbertson BH, Francis J, Campbell M, MacIntyre L, Sepelt I, Grimshaw J. A study of the perceived risks, benefits and barriers to the use of SDD in adult critical care units. Trials. 2010;11:117.
Duncan EM, Cuthbertson BH, Prior ME, Marshall AP, Wells EC, Todd LE, et al. The views of health care professionals about selective decontamination of the digestive tract: an international, theoretically-informed study. J Crit Care. 2014;29(4):634–40.
Francis JJ, Duncan EM, Prior ME, MacLennan GS, Dombrowski SU, Bellingan G, et al. Selective decontamination of the digestive tract in critically ill patients treated in intensive care units: a mixed-methods feasibility study. Health Technol Assess. 2014;18(25):1–170.
Romnew W, Salbach N, Parrott JS, Deutsch JE. A knowledge translation intervention designed using audit and feedback and the Theoretical Domains Framework for physical therapists working in inpatient rehabilitation: a case report. Physiother Theory Pract. 2018;16:1–17.
Garbutt JM, Dodd S, Walling E, Lee AA, Kulka K, Lobb R. Theory-based development of an implementation intervention to increase HPV vaccination in pediatric primary care practices. Implement Sci. 2018;13(1):45.
Ciprut S, Sedlander E, Watts KL, Matulewicz RS, Stange KC, Sherman SE, et al. Designing a theory-based intervention to improve the guideline-concordant use of imaging to stage incident prostate cancer. Urol Oncol. 2018;36(5):246–51.
Craig LE, Taylor N, Grimley R, Cadilhac DA, McInnes E, Phillips R, et al. Development of a theory-informed implementation intervention to improve the triage, treatment and transfer of stroke patients in emergency departments using the Theoretical Domains Framework (TDF): the T3 Trial. Implement Sci. 2017;12(1):88.
Riis A, Jensen CE, Bro F, Maindal HT, Petersen KD, Bendtsen MD, et al. A multifaceted implementation strategy versus passive implementation of low back pain guidelines in general practice: a cluster randomised controlled trial. Implement Sci. 2016;11(1):143.
Acknowledgements
We thank all participants who participated in this study. We thank the Canadian Critical Care Society for sharing access to their electronic mailing list of members.
Sources of Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of Interest
None.
Additional information
Previously presented at the American College of Medical Toxicology (ACMT) Annual Scientific Meeting (ASM), March 2017, San Juan, Puerto Rico.
Appendix 1
Appendix 1
Interview questions for intensivists
This is a semistructured interview with the purpose of identifying barriers and facilitators to adherence to PCC treatment recommendations for patients with a calcium channel blocker intoxication. By answering these questions, we consider that you consent to the recording of your answers and their use for research purposes. All information will be kept confidential and no nominal information will be kept.
Use of HIET
What place do you perceive your PCC protocol suggests for the use of HIET?
How does the strength of the evidence behind HIET influence your decision to use it?
Do you tend to use more vasopressors or to initiate a HIET?
What reasons would limit you to initiate a HIET?
Does the knowledge behind the mechanism of action and the reasons why it is recommended have an influence on your decision to initiate HIET?
How confident are you about proceeding to a HIET and the potential technical difficulties?
How is it easy or complicated for you to proceed to a HIET?
How does the credibility you give to your PCC influence your decision to initiate HIET if suggested by the PCC?
What is the impact on your perception of your professional identity and autonomy when PCC suggests to initiate HIET?
What problems have you encountered while doing it?
What could help you to do a HIET?
What is your level of optimism or pessimism about the effects of a HIET?
What do you think could happen if you do not use a HIET (for example if you only use pressors)?
How does the risk–benefit of a HIET influence your decision to initiate it?
What incentives are there for you to initiate a HIET?
What is your level of motivation to initiate a HIET when you have a CCB-poisoned patient?
What other goals could interfere with the HIET? What is your priority?
Is there any conflict between these treatment recommendations and other guidelines that you need to follow? How does it influence your decision to initiate a HIET?
Is HIET something you usually do?
How is it intuitive for you to consider a HIET when you have a patient with CCB poisoning?
What reasons could make you decide not to do a HIET when it is recommended by the PCC?
How do other tasks requesting your attention limit you to initiate a HIET with a patient with significant CCB poisoning?
How does CCP recommendations to initiate a HIET influence your decision-making process?
How do resources limitations influence your decision to initiate a HIET (staff, financial, time, or other)?
Are the resources necessary to do a HIET accessible when needed?
Have you seen colleagues use a HIET? Does it influences your decision to use it?
Do you perceive opposition by other professionals or colleagues when you want to initiate a HIET? How does it influence your decision to initiate it?
Does using a HIET ever brought you interpersonal conflicts?
Are treatment recommendations from the PCC a practice standard, an option, an opinion, a norm?
What emotional response do you have while initiating HIET (apprehension, anxiety, worry?)
How does this emotional response affect your decision to initiate or not a HIET?
What preliminary steps appear essential to you before you initiate a HIET (personal or structural etc.)
Are there processes or strategies that you think would facilitate the application of a HIET?
Do you receive any feedback or follow-up on your CCB-poisoned patients when PCC recommends to initiate a HIET?
How much does your ease with therapeutic options that were used before the arrival of HIE influence your decision to initiate a HIE?
What effect does your past practice have on your decision to initiate a HIE when it is recommended by PCC?
Do you think physicians consider or will consider HIE as a standard treatment? If not will it become a standard? Will it be long?
Rights and permissions
About this article
Cite this article
Brassard, E., Archambault, P., Lacombe, G. et al. Barriers and Facilitators of Intensivists’ Adherence to Hyperinsulinemia-Euglycemia Therapy in the Treatment of Calcium Channel Blocker Poisoning. J. Med. Toxicol. 14, 283–294 (2018). https://doi.org/10.1007/s13181-018-0676-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13181-018-0676-2