Abstract
Triple-negative breast cancer (TNBC) has a faster rate of metastasis compared to other breast cancer subtypes, and no effective targeted therapies are currently FDA-approved. Recent data indicate that the androgen receptor (AR) promotes tumor survival and may serve as a potential therapeutic target in TNBC. Studies of AR in disease progression and the systemic effects of anti-androgens have been hindered by the lack of an AR-positive (AR+) immunocompetent preclinical model. In this study, we identified the transgenic MMTV-PyMT (mouse mammary tumor virus-polyoma middle tumor-antigen) mouse mammary gland carcinoma model of breast cancer and Met-1 cells derived from this model as tools to study the role of AR in breast cancer progression. AR protein expression was examined in late-stage primary tumors and lung metastases from MMTV-PyMT mice as well as in Met-1 cells by immunohistochemistry (IHC). Sensitivity of Met-1 cells to the AR agonist dihydrotestosterone (DHT) and anti-androgen therapy was examined using cell viability, migration/invasion, and anchorage-independent growth assays. Late-stage primary tumors and lung metastases from MMTV-PyMT mice and Met-1 cells expressed abundant nuclear AR protein, while negative for estrogen and progesterone receptors. Met-1 sensitivity to DHT and AR antagonists demonstrated a reliance on AR for survival, and AR antagonists inhibited invasion and anchorage-independent growth. These data suggest that the MMTV-PyMT model and Met-1 cells may serve as valuable tools for mechanistic studies of the role of AR in disease progression and how anti-androgens affect the tumor microenvironment.
Similar content being viewed by others
Introduction
Even though the 5-year survival rate for non-metastatic breast cancer is nearly 99%, a lack of effective treatments means that only approximately a quarter of women diagnosed with metastatic breast cancer will survive up to 5 years [1]; thus, understanding the progression of this disease is critical. Triple-negative breast cancer (TNBC), which accounts for approximately 15–20% of newly diagnosed breast cancers, is the most clinically aggressive subtype with a peak rate of metastasis in the first 3 years post-diagnosis [2, 3]. These tumors are especially difficult to treat since, by definition, they lack expression of the most common breast cancer molecular biomarkers/therapeutic targets: estrogen receptor-alpha (ERα), progesterone receptor (PR), and human epidermal growth factor receptor 2 (HER2).
Interestingly, the androgen receptor (AR) is expressed in up to 50% of TNBCs [4] and is currently being investigated as a potential therapeutic target [5, 6]. Inhibition of AR activity in TNBC cells decreases migration, invasion, and anchorage-independent growth, indicating that AR may promote the metastatic potential of TNBC cells in culture [5]. In addition, single cell sequencing of TNBC patient-derived xenograft models indicates that AR is upregulated in early-stage metastases as compared to primary tumor cells [7]. Furthermore, in breast cancer patient tumors, AR levels are often maintained from the primary tumor to metastases [8–10]. Together, these data suggest that AR may promote the metastatic spread of breast cancer by supporting the survival of breast cancer cells during metastasis.
Metastasis to distant organs is dependent on the microenvironment both at the primary and metastatic sites [11]. In order to fully understand the potentially complex mechanisms by which AR contributes to TNBC metastasis and how AR+ cells within the microenvironment respond to anti-androgen therapies, an immunocompetent preclinical model of breast cancer is needed. However, AR protein expression has not been examined in any of the well-established, commonly used transgenic mouse models of breast cancer.
The MMTV-PyMT (mouse mammary tumor virus-polyoma middle tumor-antigen) mouse model of breast cancer is widely used and well characterized. MMTV-PyMT mice develop spontaneous mammary tumors that closely resemble the progression and morphology of human breast cancers [12–14]. MMTV-PyMT tumors lose expression of ERα and PR as they progress [14], and though MMTV-PyMT primary tumors are reported to express HER2 [14], levels are low compared to those in human HER2+ cell lines that have amplified HER2 (data not shown). Notably, gene expression profiling clustered MMTV-PyMT tumors with ERα-negative “luminal” human breast cancers [15], which is a gene signature similar to the luminal-AR (LAR) TNBC subtype characterized by high AR expression [16] and the molecular apocrine ER/PR negative, but AR+ tumors described prior to molecular subtyping [17, 18]. In order to determine whether the MMTV-PyMT mouse model might serve as a useful tool to study the role of AR in breast cancer progression, we characterized AR expression and function using late-stage MMTV-PyMT primary mammary tumors and lung metastases as well as the Met-1 cell line generated from a late-stage MMTV-PyMT primary tumor [19].
Materials and Methods
Mouse Tissue
MMTV-PyMT: Formalin-fixed, paraffin-embedded (FFPE) MMTV-PyMT mouse mammary tumors and metastatic lung tissue generated by JLC were kindly provided by Susan Kane (City of Hope, Duarte, CA, USA). Tissue was collected from 20-week-old hemizygous, mixed background (C57BL/6 and FVB/NJ) MMTV-PyMT females with multiple mammary tumors. For a detailed description of background and breeding strategy, refer to [20]. AR control tissue: Liver and testis were collected from mixed background adult male mice obtained from the University of Colorado Center for Comparative Medicine (Aurora, CO, USA) in accordance with the NIH Guidelines of Care and Use of Laboratory Animals. Mice were euthanized by carbon dioxide (CO2) inhalation followed by cervical dislocation. Tissue was immediately frozen whole in liquid nitrogen.
Cell Culture and Reagents
The mouse mammary tumor cell line Met-1 was derived from a MMTV-PyMT mammary tumor (FVB/N) by Alexander Borowsky [19]. This cell line was kindly provided in 2015 by Donald McDonnell (Duke University, Durham, NC, USA) with permission granted by Alexander Borowsky (University of California – Davis, Davis, CA, USA). Met-1 cells were maintained in DMEM with 10% FBS in 5% CO2. The human TNBC cell lines MDA-MB-231, SUM159PT, and MDA-MB-453 were cultured in 5% CO2. MDA-MB-231 cells were purchased in 2008 from the American Type Culture Collection (ATCC, Rockville, MD, USA) and maintained in MEM with 5% FBS, 1% non-essential amino acids, and insulin. SUM159PT cells were obtained in 2013 from the University of Colorado Cancer Center (UCCC) Tissue Culture Core (Aurora, CO, USA) and maintained in Ham’s/F-12 with 5% FBS, 1% HEPES, 1 μg/mL hydrocortisone, and 5 μg/mL insulin. MDA-MB-453 cells were purchased from ATCC and maintained in DMEM with 10% FBS. Only cells of under ten passages were used in this study. All the cell lines were routinely tested for mycoplasma contamination, and the human cell lines were authenticated in 2014 by short tandem repeat analysis in the UCCC Tissue Culture Core. The androgen dihydrotestosterone (DHT; Sigma-Aldrich Corporation, St. Louis, MO, USA) was diluted in 100% ethanol (EtOH). The AR antagonist enzalutamide (Enza) was provided by Medivation, Inc. (San Francisco, CA, USA). JRK-01 and JRK-04 are structurally novel AR degraders that are, respectively, non-competitive and competitive with AR agonists. All the AR antagonists were diluted in dimethyl sulfoxide (DMSO).
Immunohistochemistry (IHC)
For the analysis of cell pellets, cells were fixed in 10% buffered formalin, pelleted in Histogel from ThermoFisher Scientific Inc. (Waltham, MA, USA) and the UC Denver Tissue Biobanking and Processing Core performed tissue processing and paraffin embedding. Five-micrometer sections of FFPE tissue or cell pellets were deparaffinized in a series of xylenes and ethanols, and antigens were heat-retrieved in either 10 mM citrate buffer pH 6.0 or 10 mM Tris/1 mM EDTA pH 9.0 (ERα). Antibodies used include the following: rat monoclonal antibody specific for PyMT (#NB-100-2749; Novus Biological LLC, Littleton, CO, USA), mouse monoclonal antibody specific for ERα (#M7047 clone 1D5; Agilent Technologies Inc., Santa Clara, CA, USA), rabbit polyclonal antibody specific for PR (#A0098, Agilent), and rabbit polyclonal antibody specific to AR (#RB-9030-P0, ThermoFisher). ERα and AR antibodies were detected with Envision-HRP (Agilent) and PyMT and PR with biotinylated goat anti-rat (Jackson ImmunoResearch, West Grove, PA, USA) and biotinylated goat anti-rabbit (Agilent), respectively, each followed by streptavidin HRP (Agilent). Tris-buffered saline with 0.05% Tween 20 was used for all washes. Representative images were taken using a BX40 microscope (Olympus, Center Valley, PA, USA) with a SPOT Insight Mosaic 4.2 camera and software (Diagnostic Instruments, Inc., Sterling Heights, MI, USA). Expression levels, presented as the percentage of positive cells, were scored visually for the entire sample/tumor/metastasis or measured per field in five non-overlapping fields per sample using ImageJ software measuring the percentage of positive pixels.
Western Analysis
A homogenizer was used to extract protein from frozen tissue in ice-cold RIPA buffer supplemented with 1X protease inhibitor cocktail from Roche Applied Science (Indianapolis, IN, USA). Whole cell lysates were collected on ice in SDS Lysis Buffer (1% SDS, 10 mM EDTA, and 50 mM Tris–HCl, pH 8.1) supplemented with 1X protease inhibitor cocktail. Protein concentrations were determined with the BioRad RC DC protein assay (Hercules, CA, USA). Proteins (40 μg) were separated on an 8% SDS-PAGE gel and transferred to a polyvinylidene fluoride membrane. Five percent nonfat dry milk was used for blocking buffer and for primary antibody incubation. Primary antibodies included rabbit polyclonal antibody that recognizes both human and mouse AR (#RB-9030-P0) from ThermoFisher and mouse monoclonal antibody to α-Tubulin (#T5168) from Sigma-Aldrich. Secondary antibodies were horseradish peroxidase-conjugated anti-rabbit and anti-mouse IgG antibodies from Cell Signaling Technology (Danvers, MA, USA). The secondary antibodies were detected using an ECL Plus kit from ThermoFisher. Each experiment was repeated a minimum of two times.
Drug Sensitivity Assays
Met-1 cells were plated at a density of 350 cells per well in 96-well plates (for cell viability assays; SUM159PT cells at a density of 500 cells per well and MDA-MB-453 cells at 5 × 103 cells per well) and 5 × 104 cells per well in 60-mm plates (for AR cellular localization IHCs). For experiments involving DHT-induced proliferation or localization of AR, cells were cultured in media containing hormone-stripped serum (using dextran-coated charcoal (DCC)) for 48 h prior to supplementation with 0.1% ethanol (EtOH) or 10 nM DHT. For dose–response experiments, the cells were cultured in media containing 10% FBS. The cells were treated with either DMSO or AR antagonists (Enza, JRK-01, and JRK-04) at concentrations ranging from 1 to 100 μM for 3–5 days. Crystal violet cell viability assay: the cells were fixed with 10% formalin, stained with 5% crystal violet dye, and the dye was then solubilized with 10% acetic acid. Absorbance was measured at 540 nm. Data are presented as relative cell number or percent cell viability and normalized to the mean absorbance of EtOH- or DMSO-treated cells. Each experiment was run in quintuplicate and repeated a minimum of three times. AR cellular localization: cell pellets were collected and AR protein was stained by IHC (see details above).
Migration and Invasion Scratch Wound Assays
5 × 104 cells were plated per well in a 96-well plate. In the following day, a wound was made in each well, and the cells were treated with media containing 1% FBS and 5 μg/mL mitomycin C (for migration assays) or 10% FBS (for invasion assays) with 0.3% DMSO, 30 μM Enza, or 10 μM JRK-01. Migration across an empty wound or invasion across a wound filled with 100% Matrigel from BD Biosciences (Franklin Lakes, NJ, USA) was measured every 4 h using the IncuCyte ZOOM Live Cell Imaging apparatus (Essen BioScience, Ann Arbor, MI, USA). Data are presented as percent wound density and normalized to empty wound area from time 0 h for each drug treatment. Each experiment was run in quintuplicate and repeated a minimum of three times.
Anchorage-Independent Growth Assay
Soft agar colony formation assays [21] were performed in 0.5% bottom and 0.3% top layer agar (Difco Agar Noble, BD Biosciences) containing 0.2% DMSO, 20 μM Enza, 10 μM JRK-01, or 10 μM JRK-04; 2 × 103 cells were plated per well in a 6-well plate. Fresh media was added to each well weekly. Colonies were photographed using a Canon PowerShot A470 digital camera. Colony count and size were quantified using ImageJ software. Each experiment was run in triplicate and repeated a minimum of two times.
Statistical Analysis
Statistically significant differences, p values <0.05, were calculated using the GraphPad Prism 6.0 statistical software. Differences between groups were determined by two-tailed Student’s t test.
Results
AR Protein Is Expressed in the MMTV-PyMT Mouse Model
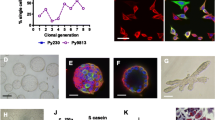
Similar to the molecular biomarker expression patterns observed in human TNBC cells, late-stage MMTV-PyMT tumors and derived Met-1 cells have previously been shown to express little to no ERα and PR and relatively low HER2 [14, 19]. In order to determine if the MMTV-PyMT mouse model could be used to study AR in an immunocompetent system analogous to TNBC, AR protein was examined in matched primary mammary tumors and metastatic lungs collected from 20-week-old MMTV-PyMT females. While few PyMT-positive primary tumors and metastases expressed ERα and PR at this late-stage in tumor development (0–2% of primary tumors and 0% of metastases), a high percentages were positive for AR (95–99% of primary tumors and 85–100% of lung metastases; Fig. 1). Furthermore, micrometastases showed consistent AR expression when compared to the expression levels of larger metastases (Supplemental Fig. 1).
Nuclear receptor expression in MMTV-PyMT tumors and derived Met-1 cells. Primary mammary tumors and lungs were collected from 20-week-old MMTV-PyMT mice (n = 8 primary tumors and n = 9–12 lung metastasis, from two mice). Met-1 cells were cultured in media with 10% FBS. Tissue and cells were formalin-fixed and paraffin-embedded. Five-micrometer sections were stained for PyMT, ERα, PR, and AR (1:100). The percentage of positive cells for each sample was scored visually, and the range of expression is indicated for each stain. Shown are representative images; 40× objective, scale bar = 50 μm
AR Is Functional in Met-1 Cells
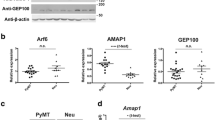
AR protein was expressed in Met-1 cells (Figs. 1 and 2a). To determine if AR is functional and whether Met-1 cells rely on it for growth, the response of Met-1 cells to AR agonists and antagonists was examined. Met-1 cells cultured in hormone-stripped serum were treated with the AR agonist dihydrotestosterone (DHT). DHT caused an increase in AR expression (p = 0.004) as well as a translocation to the nucleus, an indicator of AR activation (Fig. 2b). It is important to note that DHT did not alter PyMT protein expression in Met-1 cells (Supplemental Fig. 2). DHT also induced Met-1 cell proliferation relative to control-treated cells (p = 0.041; Fig. 2c). The AR antagonists enzalutamide (Enza) and JRK-01 significantly decreased AR protein expression and nuclear localization when compared to control-treated cells (p = 0.004 for Enza, p < 0.0001 for JRK-01; Fig. 3a). AR antagonists inhibited Met-1 cell viability, both DHT-induced proliferation (p = 0.044 for 20 μM Enza, p = 0.0001 for 30 μM Enza; Fig. 3b), as well as the viability of cells cultured in full serum media (Fig. 3c), with Met-1 IC50 values similar to those observed in human TNBC cell lines (Fig. 3d and Supplemental Table S1).
Met-1 response to an AR agonist. a Met-1 cells were cultured in media containing 10% FBS. AR protein levels were measured by Western analysis. Mouse liver and testes were used as controls for mouse AR and the MDA-MB-231, SUM159PT and MDA-MB-453 cell lines were used to examine the relative levels of AR in Met-1 cells compared to human TNBC cells. α-Tubulin was used as a loading control. b, c Met-1 cells were grown in media with hormone-stripped serum (10% DCC) for 48 h then treated with 0.1% EtOH or 10 nM dihydrotestosterone (DHT) for 3 days. b Met-1 cells were formalin-fixed and paraffin-embedded. Five-micrometer sections were stained for AR (1:800). Shown are representative images; 40× objective, scale bar = 50 μm; inset zoom ×2. The percentage of AR-positive cells per field in five non-overlapping fields per sample; mean, ** p < 0.01. c Cell viability was determined by crystal violet assay. Data was normalized to the mean absorbance of EtOH-treated cells; mean ± standard deviation, * p < 0.05
Met-1 response to AR antagonists. a Met-1 cells were grown in media with hormone-stripped serum (10% DCC) for 48 h then treated for 3 days with 10 nM DHT plus 0.2% DMSO, 20 μM enzalutamide (Enza), or 10 μM JRK-01. Cells were formalin-fixed and paraffin-embedded. Five-micrometer sections were stained for AR (1:800). Shown are representative images; 40× objective, scale bar = 50 μm; inset zoom ×2. The percentage of AR-positive cells per field in five non-overlapping fields per sample; mean, ** p < 0.01, **** p < 0.0001. b Met-1 cells were grown in media with hormone-stripped serum (10% DCC) for 48 h then treated for 3 days with 10 nM DHT plus 0.3% DMSO (-) and increasing concentrations of Enza. Cell viability was determined by crystal violet assay. Data was normalized to the mean absorbance of DMSO-treated cells; mean ± standard deviation, * p < 0.05, *** p < 0.001. c Met-1 cells were cultured in media with 10% FBS. Cell viability was determined by crystal violet assay after a 5-day exposure to 0.1% DMSO (0) or increasing concentrations of Enza, JRK-01, or JRK-04. Data was normalized to the mean absorbance of DMSO-treated cells; mean ± standard deviation. d AR-positive TNBC cell lines SUM159PT and MDA-MB-453 were grown in full serum media (10% FBS). Cell viability was determined by crystal violet assay after a 4-day exposure to either 0.1% DMSO (0) or increasing concentrations of AR antagonists. Data was normalized to the mean absorbance of DMSO-treated cells; mean ± standard deviation
AR Inhibition Decreases Met-1 Metastatic Potential
AR has been shown to promote the metastatic potential of human TNBC cells in vitro [5]. In order to investigate the role of AR in the metastatic potential of Met-1 cells, we examined the effects of AR inhibition on the classic in vitro markers of metastatic potential: migration, invasion, and anchorage-independent growth. AR antagonists had little effect on Met-1 cell migration (Fig. 4a), but significantly decreased Met-1 cell invasion when compared to control-treated cells (p = 0.0002 for Enza, p = 0.031 for JRK-01; Fig. 4b). In soft agar colony formation assays, AR antagonists significantly decreased Met-1 anchorage-independent growth relative to those in control-treated cells (colony count p = 0.0002 for JRK-01, p = 0.003 for JRK-04; colony size p = 0.032 for Enza, p = 0.0004 for JRK-01, p = 0.002 for JRK-04; Fig. 4c).
Met-1 migration and invasion. a Migration was measured every 4 h in cells cultured in media containing 1% FBS and 5 μg/mL mitomycin C with 0.3% DMSO, 30 μM enzalutamide (Enza), or 10 μM JRK-01 for 20 h; mean ± standard deviation. b Invasion across a wound filled with 100% Matrigel was measured every 4 h in cells cultured in media containing 10% FBS with 0.3% DMSO, 30 μM Enza, or 10 μM JRK-01; mean ± standard deviation. Statistical differences were measured comparing the final time-points. c Anchorage-independent growth was measured using the soft agar colony formation assay. Cells were grown in 0.3% agar media containing 0.2% DMSO, 20 μM Enza, 10 μM JRK-01, or 10 μM JRK-04; mean ± standard deviation, * p < 0.05, ** p < 0.01, *** p < 0.001. Shown are representative images
Discussion
Evidence from preclinical studies suggests that AR expression in breast cancer cells promotes a metastatic phenotype [5, 7]. We previously demonstrated that inhibition of AR dramatically decreased proliferation, migration, invasion, anchorage-independent growth, and tumor formation in multiple human TNBC cell lines [5, 22]. Our data in the MMTV-PyMT model and Met-1 cells is consistent with this, showing that AR is retained in MMTV-PyMT lung metastases and that AR antagonists inhibit Met-1 proliferation and invasion as well as anchorage-independent growth, a well-established predictor of the capacity for metastasis in vivo [23]. Met-1 cells are highly migratory, which may explain why we did not observe the decrease in migration by AR antagonism that we previously observed in human TNBC cells. AR may promote expression of factors responsible for degradation of the extracellular matrix (ECM), a critical early step in the metastatic cascade, since AR inhibition has a more pronounced effect on Met-1 cell invasion versus migration. In fact, AR promotes metalloproteinase (MMP) expression, specifically MMP-2 and MMP-9, in a number of cancer types [24, 25], and this has been linked clinically to more aggressive tumors in patients with hepatocellular carcinoma [26]. In breast cancer patients, AR expression positively associates with higher expression of several MMPs [27]. Further research is necessary to understand the direct relationship between AR and ECM remodeling proteins, such as MMPs. We also demonstrated previously that the greatest effect of the anti-androgen Enza was on human TNBC cell growth on soft agar [5], and we observe a strong effect on the Met-1 cells here. Our data is also consistent with recent data in a human TNBC patient-derived xenograft model showing an increase in AR gene expression in circulating tumor cells and early lung metastases as compared to the primary tumor [7], and closely recapitulates what is often observed in AR+ breast cancer patients where AR levels are maintained from the primary tumor to metastases [8–10]. Taken together, these data support the hypothesis that AR supports cancer cell invasion and survival during metastasis to distant sites.
Our data also demonstrate that the phenotypic effects following treatment with AR agonists and antagonists in the Met-1 model are due to changes in AR activity and not to changes in PyMT expression. There is some evidence that steroid hormone receptors can regulate the MMTV promoter, but MMTV activation by steroid receptors is known to be both cell type- and context-dependent [28–30]. DHT-induced AR activation had no effect on PyMT expression in Met-1 cells (Supplemental Fig. 2), suggesting that the MMTV promoter is not androgen responsive in this model and that the observed effects on cell viability and metastatic potential are a consequence of changes in AR expression and activity.
New-generation anti-androgens are in clinical trials for the treatment of breast cancer, and there is potential for women to be on such therapy for extended periods as are men with prostate cancer. Consequently, further investigation into how systemically administered anti-androgens affect stromal and immune cell populations is warranted. AR is expressed in various normal cells throughout the body, including cells in metastatic sites such as the lung, and in a wide variety of immune cells, many of which contribute to the anti-tumor immune response [31, 32]. There exists some controversy regarding whether new-generation anti-androgens, such as enzalutamide, promote or dampen the anti-tumor T cell response [33–36]. To date, this question has been examined primarily in models of prostate cancer, and since this is the first report of an immunocompetent AR+ mammary carcinoma model, this issue has not yet been examined in the context of a breast cancer in vivo model. Anti-androgens lead to increased susceptibility of both prostate and breast cancer cells to cytotoxic T cell killing in vitro, which could have positive implications for the future combination of AR antagonists with immunotherapies that stimulate the anti-tumor immune response [34, 36]. However, Yang-Xin Fu’s group used immunocompetent mouse models of prostate cancer to show that AR antagonists have an immunosuppressive effect on T cell priming, diminishing the anti-tumor immune response and eventually leading to accelerated tumor recurrence [35]. For anti-androgens to be effective long-term breast cancer therapeutics, it is essential that we understand how they affect host immunity and, in particular, what effects they may have on the anti-tumor immune response. Ultimately, the MMTV-PyMT model and Met-1 cells will help unravel the complex ways in which anti-androgens affect breast cancer progression.
Tumor progression is not an isolated process. Complex interactions between tumor and stromal cells, both at the primary and metastatic sites, play a critical role in determining the extent of tumor progression [11]. TNBC is particularly aggressive and difficult to treat; thus, it is essential to better understand how the tumor microenvironment contributes to the rapid progression of this subtype of breast cancer. The data presented here suggest that the MMTV-PyMT model and Met-1 cells may serve as valuable tools for mechanistic studies of how AR and anti-androgens affect breast cancer progression and serve as an immunocompetent model of progression to AR+ TNBC (LAR) metastatic disease.
References
Howlader N, Noone AM, Krapcho M, Miller D, Bishop K, Altekruse SF, Kosary CL, Yu M, Ruhl J, Tatalovich Z, Mariotto A, Lewis DR, Chen HS, Feuer EJ, Cronin KA (2016) SEER Cancer Statistics Review, 1975–2013. November 2015 SEER data submission. National Cancer Institute, Bethesda
Foulkes WD, Smith IE, Reis-Filho JS (2010) Triple-negative breast cancer. N Engl J Med 363:1938–1948
Howlader N, Altekruse SF, Li CI, Chen VW, Clarke CA, Ries LA, Cronin KA (2014) US incidence of breast cancer subtypes defined by joint hormone receptor and HER2 status. J Natl Cancer Inst 106
McNamara KM, Yoda T, Takagi K, Miki Y, Suzuki T, Sasano H (2013) Androgen receptor in triple negative breast cancer. J Steroid Biochem Mol Biol 133:66–76
Barton VN, D’Amato NC, Gordon MA, Lind HT, Spoelstra NS, Babbs BL, Heinz RE, Elias A, Jedlicka P, Jacobsen BM, Richer JK (2015) Multiple molecular subtypes of triple-negative breast cancer critically rely on androgen receptor and respond to enzalutamide in vivo. Mol Cancer Ther 14:769–778
Traina TA, Miller K, Yardley DA, O’Shaughnessy J, Cortes J, Awada A, Kelly CM, Trudeau ME, Schmid P, Gianni L, Garcia-Estevez L, Nanda R, Ademuyiwa FO, Chan S, Steinberg JL, Blaney ME, Tudor IC, Uppal H, Peterson AC, Hudis CA (2015) Results from a phase 2 study of enzalutamide, and androgen receptor inhibitor, in advanced AR+ triple-negative breast cancer. J Clin Oncol 33(suppl; abstr 1003)
Lawson DA, Bhakta NR, Kessenbrock K, Prummel KD, Yu Y, Takai K, Zhou A, Eyob H, Balakrishnan S, Wang CY, Yaswen P, Goga A, Werb Z (2015) Single-cell analysis reveals a stem-cell program in human metastatic breast cancer cells. Nature 526:131–135
Hattori Y, Yoshida A, Yoshida M, Takahashi M, Tsuta K (2015) Evaluation of androgen receptor and GATA binding protein 3 as immunohistochemical markers in the diagnosis of metastatic breast carcinoma to the lung. Pathol Int 65:286–292
McNamara KM, Yoda T, Miki Y, Nakamura Y, Suzuki T, Nemoto N, Miyashita M, Nishimura R, Arima N, Tamaki K, Ishida T, Ohuchi N, Sasano H (2015) Androgen receptor and enzymes in lymph node metastasis and cancer reoccurrence in triple-negative breast cancer. Int J Biol Markers 30:184–189
Cimino-Mathews A, Hicks JL, Illei PB, Halushka MK, Fetting JH, De Marzo AM, Park BH, Argani P (2012) Androgen receptor expression is usually maintained in initial surgically resected breast cancer metastases but is often lost in end-stage metastases found at autopsy. Hum Pathol 43:1003–1011
Quail DF, Joyce JA (2013) Microenvironmental regulation of tumor progression and metastasis. Nat Med 19:1423–1437
Fluck MM, Schaffhausen BS (2009) Lessons in signaling and tumorigenesis from polyomavirus middle T antigen. Microbiol Mol Biol Rev 73:542–563, Table of Contents
Guy CT, Cardiff RD, Muller WJ (1992) Induction of mammary tumors by expression of polyomavirus middle T oncogene: a transgenic mouse model for metastatic disease. Mol Cell Biol 12:954–961
Lin EY, Jones JG, Li P, Zhu L, Whitney KD, Muller WJ, Pollard JW (2003) Progression to malignancy in the polyoma middle T oncoprotein mouse breast cancer model provides a reliable model for human diseases. Am J Pathol 163:2113–2126
Shoushtari AN, Michalowska AM, Green JE (2007) Comparing genetically engineered mouse mammary cancer models with human breast cancer by expression profiling. Breast Dis 28:39–51
Lehmann BD, Bauer JA, Chen X, Sanders ME, Chakravarthy AB, Shyr Y, Pietenpol JA (2011) Identification of human triple-negative breast cancer subtypes and preclinical models for selection of targeted therapies. J Clin Invest 121:2750–2767
Doane AS, Danso M, Lal P, Donaton M, Zhang L, Hudis C, Gerald WL (2006) An estrogen receptor-negative breast cancer subset characterized by a hormonally regulated transcriptional program and response to androgen. Oncogene 25:3994–4008
Farmer P, Bonnefoi H, Becette V, Tubiana-Hulin M, Fumoleau P, Larsimont D, Macgrogan G, Bergh J, Cameron D, Goldstein D, Duss S, Nicoulaz AL, Brisken C, Fiche M, Delorenzi M, Iggo R (2005) Identification of molecular apocrine breast tumours by microarray analysis. Oncogene 24:4660–4671
Borowsky AD, Namba R, Young LJ, Hunter KW, Hodgson JG, Tepper CG, McGoldrick ET, Muller WJ, Cardiff RD, Gregg JP (2005) Syngeneic mouse mammary carcinoma cell lines: two closely related cell lines with divergent metastatic behavior. Clin Exp Metastasis 22:47–59
Christenson JL, Kane SE (2014) Darpp-32 and t-Darpp are differentially expressed in normal and malignant mouse mammary tissue. Mol Cancer 13:192
Borowicz S, Van Scoyk M, Avasarala S, Karuppusamy Rathinam MK, Tauler J, Bikkavilli RK, Winn RA (2014) The soft agar colony formation assay. J Vis Exp e51998
Cochrane DR, Bernales S, Jacobsen BM, Cittelly DM, Howe EN, D’Amato NC, Spoelstra NS, Edgerton SM, Jean A, Guerrero J, Gomez F, Medicherla S, Alfaro IE, McCullagh E, Jedlicka P, Torkko KC, Thor AD, Elias AD, Protter AA, Richer JK (2014) Role of the androgen receptor in breast cancer and preclinical analysis of enzalutamide. Breast Cancer Res 16:R7
Mori S, Chang JT, Andrechek ER, Matsumura N, Baba T, Yao G, Kim JW, Gatza M, Murphy S, Nevins JR (2009) Anchorage-independent cell growth signature identifies tumors with metastatic potential. Oncogene 28:2796–2805
Liao X, Thrasher JB, Pelling J, Holzbeierlein J, Sang QX, Li B (2003) Androgen stimulates matrix metalloproteinase-2 expression in human prostate cancer. Endocrinology 144:1656–1663
Zhang BG, Du T, Zang MD, Chang Q, Fan ZY, Li JF, Yu BQ, Su LP, Li C, Yan C, Gu QL, Zhu ZG, Yan M, Liu B (2014) Androgen receptor promotes gastric cancer cell migration and invasion via AKT-phosphorylation dependent upregulation of matrix metalloproteinase 9. Oncotarget 5:10584–10595
Zhang Y, Shen Y, Cao B, Yan A, Ji H (2015) Elevated expression levels of androgen receptors and matrix metalloproteinase-2 and -9 in 30 cases of hepatocellular carcinoma compared with adjacent tissues as predictors of cancer invasion and staging. Exp Ther Med 9:905–908
Gonzalez LO, Corte MD, Vazquez J, Junquera S, Sanchez R, Alvarez AC, Rodriguez JC, Lamelas ML, Vizoso FJ (2008) Androgen receptor expression in breast cancer: relationship with clinicopathological characteristics of the tumors, prognosis, and expression of metalloproteases and their inhibitors. BMC Cancer 8:149
Nelson CC, Hendy SC, Shukin RJ, Cheng H, Bruchovsky N, Koop BF, Rennie PS (1999) Determinants of DNA sequence specificity of the androgen, progesterone, and glucocorticoid receptors: evidence for differential steroid receptor response elements. Mol Endocrinol 13:2090–2107
Archer TK, Fryer CJ, Lee HL, Zaniewski E, Liang T, Mymryk JS (1995) Steroid hormone receptor status defines the MMTV promoter chromatin structure in vivo. J Steroid Biochem Mol Biol 53:421–429
Otten AD, Sanders MM, McKnight GS (1988) The MMTV LTR promoter is induced by progesterone and dihydrotestosterone but not by estrogen. Mol Endocrinol 2:143–147
Lai JJ, Lai KP, Zeng W, Chuang KH, Altuwaijri S, Chang C (2012) Androgen receptor influences on body defense system via modulation of innate and adaptive immune systems: lessons from conditional AR knockout mice. Am J Pathol 181:1504–1512
Mikkonen L, Pihlajamaa P, Sahu B, Zhang FP, Janne OA (2010) Androgen receptor and androgen-dependent gene expression in lung. Mol Cell Endocrinol 317:14–24
Ardiani A, Farsaci B, Rogers CJ, Protter A, Guo Z, King TH, Apelian D, Hodge JW (2013) Combination therapy with a second-generation androgen receptor antagonist and a metastasis vaccine improves survival in a spontaneous prostate cancer model. Clin Cancer Res 19:6205–6218
Ardiani A, Gameiro SR, Kwilas AR, Donahue RN, Hodge JW (2014) Androgen deprivation therapy sensitizes prostate cancer cells to T-cell killing through androgen receptor dependent modulation of the apoptotic pathway. Oncotarget 5:9335–9348
Pu Y, Xu M, Liang Y, Yang K, Guo Y, Yang X, Fu YX (2016) Androgen receptor antagonists compromise T cell response against prostate cancer leading to early tumor relapse. Sci Transl Med 8:333ra347
Kwilas AR, Ardiani A, Gameiro SR, Richards J, Hall AB, Hodge JW (2016) Androgen deprivation therapy sensitizes triple negative breast cancer cells to immune-mediated lysis through androgen receptor independent modulation of osteoprotegerin. Oncotarget 7:23498–23511
Acknowledgements
The authors thank Susan Kane from the City of Hope for providing MMTV-PyMT tissue; Alexander Borowsky from the University of California – Davis for permission to use the Met-1 cell line, the University of Colorado Denver Tissue Biobanking and Processing Core and the University of Colorado Cancer Center Tissue Culture Core, both supported by the National Institute of Health/National Cancer Institute Cancer Core Support Grant P30 CA046934, for experimental assistance; and Britta Jacobsen for critical reading of the manuscript. Enzalutamide was provided by Astellas, Inc. and Medivation, Inc. (Medivation, Inc. was acquired by Pfizer, Inc. in September 2016).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This study was funded by a National Institute of Health R01 CA187733-01A1 to JKR; NIH NRSA T32 CA190216-01A1 postdoctoral fellowship to JLC; US Army Synergistic Idea Development Awards W81XWH-10-1-0179 and W81XWH-15-1 to JAK, JSJ, JAP, JN, and DPMcD; Breast Cancer Research Foundation grant to BSK; and enzalutamide was provided by Astellas, Inc. and Medivation, Inc. (Medivation, Inc. was acquired by Pfizer, Inc. in September 2016).
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
This article does not contain any studies with human participants performed by any of the authors. All applicable international, national, and/or institutional guidelines for the care and use of animals were followed.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Supplemental Fig. 1
AR expression in micro- and macrometastases from MMTV-PyMT mice. Metastatic lungs were formalin-fixed and paraffin embedded. 5 μm sections were stained for PyMT, AR and H&E. Shown are representative images of a micrometastasis (top, arrow) and a macrometastasis (bottom); 10× and 40× objectives, scale bar = 100 μm, inset zoom ×2.5 (PDF 146 kb)
Supplemental Fig. 2
PyMT expression in response to AR agonist treatment. Met-1 cells were grown in media with hormone-stripped serum (10% DCC) for 48 hours then treated for 3 days with 0.1% EtOH or 10 nM dihydrotestosterone (DHT). Cells were formalin-fixed and paraffin embedded. 5 μm sections were stained for PyMT. Shown are representative images; 40× objective. The percentage of PyMT positive cells per field in five nonoverlapping fields per sample; mean (PDF 44 kb)
Supplemental Table S1
(PDF 162 kb)
Rights and permissions
About this article
Cite this article
Christenson, J.L., Butterfield, K.T., Spoelstra, N.S. et al. MMTV-PyMT and Derived Met-1 Mouse Mammary Tumor Cells as Models for Studying the Role of the Androgen Receptor in Triple-Negative Breast Cancer Progression. HORM CANC 8, 69–77 (2017). https://doi.org/10.1007/s12672-017-0285-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12672-017-0285-6