Abstract
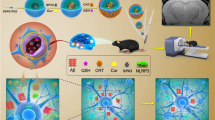
Alzheimer’s disease is becoming a serious concern in the medical field due to its severity and prevalence. This multifactorial disease manifested by various genetic and nongenetic factors makes its treatment very difficult. Due to the inefficacy of the currently available drugs, newer therapeutic strategies are increasingly in demand. Most of the current drug discovery initiatives are pivoted around amyloid pathology which is considered to be central to the disease progression. In this work, we propose the use of amyloid-binding aptamer conjugated to poly(lactic-co-glycolic acid) (PLGA)-coated curcumin nanoparticles to bind to the amyloid plaques. Curcumin is a plant-derived compound with reported anti-amyloid activity. Recent reports reveal the importance of plasma amyloid in Alzheimer development. We propose that the amyloid-binding aptamer attached curcumin–PLGA nanoparticles can be used as a potential tool in targeting the plasma amyloid and thus helps in Alzheimer therapy.









Similar content being viewed by others
References
Hardy, J., Selkoe, D. J. (2002). The amyloid hypothesis of Alzheimer's disease: Progress and problems on the road to therapeutics. Science, 297, 353–356. doi:10.1126/science.1072994.
Mathew, A., Yoshida, Y., Maekawa, T., Sakthi Kumar, D. (2011). Alzheimer's disease: Cholesterol a menace? Brain Research Bulletin, 86, 1–12. doi:10.1016/j.brainresbull.2011.06.006.
Mawuenyega, K. G., Sigurdson, W., Ovod, V., Munsell, L., Kasten, T., Morris, J. C., Yarasheski, K. E., Bateman, R. J. (2010). Decreased clearance of CNS β-amyloid in Alzheimer’s disease. Science, 330, 1774. doi:10.1126/science.1197623.
Ghiso, J., & Frangione, B. (2002). Amyloidosis and Alzheimer’s disease. Advanced Drug Delivery Reviews, 54, 1539–1551. doi:10.1016/S0169-409X(02)00149-7.
Karran, E., Mercken, M., Strooper, B. D. (2011). The amyloid cascade hypothesis for Alzheimer's disease: An appraisal for the development of therapeutics. Nature Review Drug Discovery, 10, 698–712. doi:10.1038/nrd3505.
Iwata, N., Higuchi, M., Saido, T. C. (2005). Metabolism of amyloid-β peptide and Alzheimer's disease. Pharmacology & Therapeutics, 108, 129–148. doi:10.1016/j.pharmthera.2005.03.010.
Seppälä, T. T., Herukka, S.-K., Hänninsen, T., Tervo, S., Hallikainen, M., Soininen, H., Pirttilä, T. (2010). Plasma Aβ42 and Aβ40 as markers of cognitive change in follow-up: A prospective, longitudinal, population-based cohort study. Journal of Neurology, Neurosurgery & Psychiatry, 81(10), 1123–1127. doi:10.1136/jnnp.2010.205757.
Pan, W., Solomon, B., Maness, L. M., Kastin, A. J. (2002). Antibodies to β-amyloid decrease the blood-to-brain transfer of β-amyloid peptide. Experimental Biology and Medicine, 227, 609–615.
Villemagne, V. L., Perez, K. A., Pike, K. E., Kok, W. M., Rowe, C. C., White, A. R., Bourgeat, P., Salvado, O., Bedo, J., Hutton, C. A., Faux, N. G., Masters, C. L., Barnham, K. J. (2010). Blood-borne amyloid-β dimer correlates with clinical markers of Alzheimer's disease. The Journal of Neuroscience, 30, 6315–6322. doi:10.1523/JNEUROSCI.5180-09.2010.
Takeda, S., Sato, N., Rakugi, H., Morishita, R. (2010). Plasma β-amyloid as potential biomarker of Alzheimer disease: Possibility of diagnostic tool for Alzheimer disease. Molecular BioSystems, 6, 1760–1766. doi:10.1039/C003148H.
Frenkel, D., & Solomon, B. (2001). Towards Alzheimer's β-amyloid vaccination. Biologicals, 29, 243–247. doi:10.1006/biol.2001.0294.
Schnabel, J. (2011). Vaccines: Chasing the dream. Nature, 475, S18–S19. doi:10.1038/475S18a.
Smith, E. E., & Greenberg, S. M. (2009). β-Amyloid, blood vessels, and brain function. Stroke, 40, 2601–2606. doi:10.1161/STROKEAHA.108.536839.
Sundelof, J., Giedraitis, V., Irizarry, M. C., Sundstrom, J., Ingelsson, E., Ronnemaa, E., Arnlov, J., Gunnarsson, M. D., Hyman, B. T., Basun, H., Ingelsson, M., Lannfelt, L., Kilander, L. (2008). Plasma β amyloid and the risk of Alzheimer disease and dementia in elderly men: A prospective, population-based cohort study. Archives of Neurology, 65, 256–263. doi:10.1001/archneurol.2007.57.
Okereke, O. I., Xia, W., Selkoe, D. J., Grodstein, F. (2009). Ten-year change in plasma amyloid beta levels and late-life cognitive decline. Archives of Neurology, 66, 1247–1253. doi:10.1001/archneurol.2009.207.
Schupf, N., Tang, M. X., Fukuyama, H., Manly, J., Andrews, H., Mehta, P., Ravetch, J., Mayeux, R. (2008). Peripheral Aβ subspecies as risk biomarkers of Alzheimer's disease. Proceedings of the National Academy of Sciences, 105, 14052–14057. doi:10.1073/pnas.0805902105.
Pesaresi, M., Lovati, C., Bertora, P., Mailland, E., Galimberti, D., Scarpini, E., Quadri, P., Forloni, G., Mariani, C. (2006). Plasma levels of beta-amyloid (1–42) in Alzheimer's disease and mild cognitive impairment. Neurobiology of Aging, 27, 904–905. doi:10.1016/j.neurobiolaging.2006.03.004.
Brenn, A., Grube, M., Peters, M., Fischer, A., Jedlitschky, G., Kroemer, H. K., Warzok, R. W., Vogelgesang, S. (2011). Beta-amyloid downregulates MDR1-P-glycoprotein (Abcb1) expression at the blood–brain barrier in mice. International Journal of Alzheimer's Disease. doi:10.4061/2011/690121.
Matsuoka, Y., Saito, M., LaFrancois, J., Saito, M., Gaynor, K., Olm, V., Wang, L., Casey, E., Lu, Y., Shiratori, C., Lemere, C., Duff, K. (2003). Novel therapeutic approach for the treatment of Alzheimer's disease by peripheral administration of agents with an affinity to β-amyloid. The Journal of Neuroscience, 23, 29–33.
Sutcliffe, J. G., Hedlund, P. B., Thomas, E. A., Bloom, F. E., Hilbush, B. S. (2011). Peripheral reduction of β-amyloid is sufficient to reduce brain β-amyloid: Implications for Alzheimer's disease. Journal of Neuroscience Research, 89, 808–814. doi:10.1002/jnr.22603.
Shi, H., Tang, Z., Kim, Y., Nie, H., Huang, Y. F., He, X., Deng, K., Wang, K., Tan, W. (2010). In vivo fluorescence imaging of tumors using molecular aptamers generated by cell-SELEX. Chemistry, an Asian Journal, 5, 2209–13. doi:10.1002/asia.201000242.
Kim, D., Jeong, Y. Y., Jon, S. (2010). A drug-loaded aptamer-gold nanoparticle bioconjugate for combined CT imaging and therapy of prostate cancer. ACS Nano, 4, 3689–96. doi:10.1021/nn901877h.
Fang, X., & Tan, W. (2010). Aptamers generated from cell-SELEX for molecular medicine: A chemical biology approach. Accounts of Chemical Research, 43, 48–57. doi:10.1021/ar900101s.
Brody, E. N., & Gold, L. (2000). Aptamers as therapeutic and diagnostic agents. Reviews in Molecular Biotechnology, 74, 5–13. doi:10.1016/S1389-0352(99)00004-5.
Shi, H., He, X., Wang, K., Wu, X., Ye, X., Guo, Q., Tan, W., Qing, Z., Yang, X., Zhou, B. (2011). Activatable aptamer probe for contrast-enhanced in vivo cancer imaging based on cell membrane protein-triggered conformation alteration. Proceedings of the National Academy of Sciences of the United States of America, 108, 3900–5. doi:10.1073/pnas.1016197108.
Ylera, F., Lurz, R., Erdmann, V. A., Fürste, J. P. (2002). Selection of RNA aptamers to the Alzheimer's disease amyloid peptide. Biochemical and Biophysical Research Communications, 290, 1583–1588. doi:10.1006/bbrc.2002.6354.
Rahimi, F., Murakami, K., Summers, J. L., Chen, C.-H. B., Bitan, G. (2009). RNA aptamers generated against oligomeric Aβ40 recognize common amyloid aptatopes with low specificity but high sensitivity. PloS One, 4, e7694. doi:10.1371/journal.pone.0007694.
Rentmeister, A., Bill, A., Wahle, T., Walter, J., Famulok, M. (2006). RNA aptamers selectively modulate protein recruitment to the cytoplasmic domain of β-secretase BACE1 in vitro. RNA, 12, 1650–1660. doi:10.1261/rna.126306.
Bunka, D. H. J., Mantle, B. J., Morten, I. J., Tennent, G. A., Radford, S. E., Stockley, P. G. (2007). Production and characterization of RNA aptamers specific for amyloid fibril epitopes. Journal of Biological Chemistry, 282, 34500–34509. doi:10.1074/jbc.M703679200.
Rahimi, F., Bitan, G. (2010). Selection of aptamers for amyloid beta-protein, the causative agent of Alzheimer’s disease. Journal of Visualized Experiments. e1955. doi: 10.3791/1955
Takahashi, T., Tada, K., Mihara, H. (2009). RNA aptamers selected against amyloid β-peptide (Aβ) inhibit the aggregation of Aβ. Molecular BioSystems, 5, 986–991. doi:10.1039/B903391B.
Cartiera, M. S., Ferreira, E. C., Caputo, C., Egan, M. E., Caplan, M. J., Saltzman, W. M. (2009). Partial correction of cystic fibrosis defects with PLGA nanoparticles encapsulating curcumin. Molecular Pharmaceutics, 7(1), 86–93. doi:10.1021/mp900138a.
Westhof, E., Masquida, B., Jossinet, F. (2011). Predicting and modeling RNA architecture. Cold Spring Harbor Perspectives in Biology, 3. doi:10.1101/cshperspect.a003632.
Zuker, M. (2003). Mfold web server for nucleic acid folding and hybridization prediction. Nucleic Acids Research, 31, 3406–3415. doi:10.1093/nar/gkg595.
Mathews, D. H., Disney, M. D., Childs, J. L., Schroeder, S. J., Zuker, M., Turner, D. H. (2004). Incorporating chemical modification constraints into a dynamic programming algorithm for prediction of RNA secondary structure. Proceedings of the National Academy of Sciences of the United States of America, 101, 7287–7292. doi:10.1073/pnas.0401799101.
Mathews, D. H., Sabina, J., Zuker, M., Turner, D. H. (1999). Expanded sequence dependence of thermodynamic parameters improves prediction of RNA secondary structure. Journal of Molecular Biology, 288, 911–940. doi:10.1006/jmbi.1999.2700.
Acknowledgments
A. Mathew, A. Aravind, and D. Brahatheeswaran would like to sincerely acknowledge the receipt of Monbukagakusho Scholarship from the Ministry of Education, Culture, Sports, Science and Technology (MEXT), Japan.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mathew, A., Aravind, A., Brahatheeswaran, D. et al. Amyloid-Binding Aptamer Conjugated Curcumin–PLGA Nanoparticle for Potential Use in Alzheimer’s Disease. BioNanoSci. 2, 83–93 (2012). https://doi.org/10.1007/s12668-012-0040-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12668-012-0040-y