Abstract
Introduction
In clinical practice, endoscopic findings are often used for assessing disease activity in inflammatory bowel disease (IBD). In recent years, blood and stool markers are being increasingly used for this purpose. Among them, the fecal calprotectin (FC) level is probably the most favored. Data on the reliability of FC are lacking from countries like India, where gut infections are common.
Objective
The aims of this study were to compare the FC level with the erythrocyte sedimentation rate (ESR) and the C-reactive protein (CRP) as non-invasive markers of IBD and, in patients with ulcerative colitis (UC), and to study its correlation with disease extent, clinical activity, and endoscopic severity.
Methods
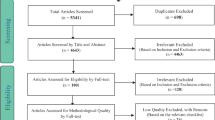
Records of patients with IBD who had tests for FC, ESR and CRP and colonoscopy done within a 2-week period, between 2012 and 2014, were retrieved. Sixty-three patients (UC 32, Crohn’s disease [CD] 31) were included for analysis. ESR, CRP and FC were compared to endoscopy to assess inflammation.
Results
Patients with UC had higher levels of FC than those with ileocolonic CD (median FC 800 mcg/g vs. 619 mcg/g, respectively; p = 0.04). FC levels correlated with CRP (r = 0.4, p < 0.001) but not with ESR (r = 0.21, p = 0.09). In patients with UC with endoscopic evidence of inflammation, more (86.9 %) had FC >200 mcg/g (cut-off for disease activity in our laboratory) than had ESR >20 mm in the first hour (60.6 %) or positive CRP (65.6 %) (<0.01); FC levels increased with increasing endoscopic Mayo score (p = 0.001) and Truelove-Witt’s clinical severity score (p = 0.006), but did not correlate with disease extent (p = 0.7). The best FC cut-off level to identify ‘active UC’ (Mayo grade 2 or more) was 800 mcg/g.
Conclusion
Fecal calprotectin level correlates with CRP but not with ESR. In patients with UC with inflammation, FC >200 mcg/g is more often positive than raised ESR or CRP; it also correlates with clinical and endoscopic activity but not with disease extent. FC level >800 mcg/g can be used to differentiate active from inactive UC.


Similar content being viewed by others
References
Loftus EV Jr. Clinical perspectives in Crohn’s disease. Objective measures of disease activity: alternatives to symptom indices. Rev Gastroenterol Disord. 2007;7 Suppl 2:S8–16.
Denis MA, Reenaers C, Fontaine F, Belaiche J, Louis E. Assessment of endoscopic activity index and biological inflammatory markers in clinically active Crohn’s disease with normal C-reactive protein serum level. Inflamm Bowel Dis. 2007;13:1100–5.
Johne B, Fagerhol MK, Lyberg T, et al. Functional and clinical aspects of the myelomonocyte protein calprotectin. Mol Pathol. 1997;50:113–23.
Yui S, Nakatani Y, Mikami M. Calprotectin (S100A8/S100A9), an inflammatory protein complex from neutrophils with a broad apoptosis inducing activity. Biol Pharm Bull. 2003;26:753–60.
Tibble JA, Sigthorsson G, Foster R, Forgacs I, Bjarnason I. Use of surrogate markers of inflammation and Rome criteria to distinguish organic from nonorganic intestinal disease. Gastroenterology. 2002;123:450–60.
Costa F, Mumolo MG, Ceccarelli L, et al. Calprotectin is a stronger predictive marker of relapse in ulcerative colitis than in Crohn’s disease. Gut. 2005;54:364–8.
Berni Canani R, Rapacciuolo L, Romano MT, et al. Diagnostic value of fecal calprotectin in pediatric gastroenterology clinical practice. Dig Liver Dis. 2004;36:467–70.
Røseth AG, Aadland E, Jahnsen J, Raknerud N. Assessment of disease activity in ulcerative colitis by fecal calprotectin, a novel granulocyte marker protein. Digestion. 1997;58:176–80.
Chang JC, Cohen RD. Medical management of severe ulcerative colitis. Gastroenterol Clin N Am. 2004;33:235–50.
Su C, Lewis JD, Goldberg B, Brensinger C, Lichtenstein GR. A meta-analysis of the placebo rates of remission and response in clinical trials of active ulcerative colitis. Gastroenterology. 2007;132:516–26.
Daperno M, Castiglione F, Ridder L, et al. Results of the 2nd part Scientific Workshop of the ECCO. II: measures and markers of prediction to achieve, detect, and monitor intestinal healing in inflammatory bowel disease. J Crohns Colitis. 2011;5:484–98.
Canani RB, de Horatio LT, Terrin G, et al. Combined use of noninvasive tests is useful in the initial diagnostic approach to a child with suspected inflammatory bowel disease. J Pediatr Gastroenterol Nutr. 2006;42:9–15.
Joishy M, Davies I, Ahmed M, et al. Fecal calprotectin and lactoferrin as noninvasive markers of pediatric inflammatory bowel disease. J Pediatr Gastroenterol Nutr. 2009;48:48–54.
Fagerberg UL, Lööf L, Myrdal U, Hansson LO, Finkel Y. Colorectal inflammation is well predicted by fecal calprotectin in children with gastrointestinal symptoms. J Pediatr Gastroenterol Nutr. 2005;40:450–5.
Roseth AG. Determination of fecal calprotectin, a novel marker of organic gastrointestinal disorders. Dig Liver Dis. 2003;35:607–9.
Costa F, Mumolo MG, Bellini M, et al. Role of fecal calprotectin as non-invasive marker of intestinal inflammation. Dig Liver Dis. 2003;35:642–7.
Tibble JA, Bjarnason I. Fecal calprotectin as an index of intestinal inflammation. Drugs Today (Barc). 2001;37:85–96.
Narayanan MP, Vaidyanathan K, Gajendra O, Shine S, Balakrishna V. Fecal calprotectin in inflammatory bowel diseases. Indian J Clin Biochem. 2009; Suppl 24:1-24 (Abst.).
Von Roon AC, Karamountzos L, Purkayastha S, et al. Diagnostic precision of fecal calprotectin for inflammatory bowel disease and colorectal malignancy. Am J Gastroenterol. 2007;102:803–13.
Xiang JY, Ouyang Q, Li GD, Xiao NP. Clinical value of fecal calprotectin in determining disease activity of ulcerative colitis. World J Gastroenterol. 2008;14:53–7.
Tibble J, Teahon K, Thjodleifsson B, et al. A simple method for assessing intestinal inflammation in Crohn’s disease. Gut. 2000;47:506–13.
Kobelska-Dubiel N, Ignas I, Krauss H, et al. Calprotectin in feces as a marker of inflammatory bowel in children. Pediatr Gastroenterol, Hepatol Child Nutr. 2007;9:172–5.
Canani RB, Terrin G, Rapacciuolo L, et al. Fecal calprotectin as reliable non-invasive marker to assess the severity of mucosal inflammation in children with inflammatory bowel disease. Dig Liver Dis. 2008;40:547–53.
Langhorst J, Elsenbruch S, Koelzer J, et al. Noninvasive markers in the assessment of intestinal inflammation in inflammatory bowel diseases: performance of fecal lactoferrin, calprotectin, and PMN-elastase, CRP, and clinical indices. Am J Gastroenterol. 2008;103:162–9.
Schoepfer AM, Beglinger C, Straumann A, et al. Fecal calprotectin more accurately reflects endoscopic activity of ulcerative colitis than the Lichtiger Index, C-reactive protein, platelets, hemoglobin, and blood leukocytes. Inflamm Bowel Dis. 2013;19:332–41.
De Vos M, Louis EJ, Jahnsen J, et al. Consecutive fecal calprotectin measurements to predict relapse in patients with ulcerative colitis receiving infliximab maintenance therapy. Inflamm Bowel Dis. 2013;19:2111–7.
Mooiweer E, Severs M, Schipper ME, et al. Low fecal calprotectin predicts sustained clinical remission in inflammatory bowel disease patients: a plea for deep remission. J Crohns Colitis. 2015;9:50–5.
Guardiola J, Lobatón T, Rodríguez-Alonso L, et al. Fecal level of calprotectin identifies histologic inflammation in patients with ulcerative colitis in clinical and endoscopic remission. Clin Gastroenterol Hepatol. 2014;12:1865–70.
Lobatón T, Rodríguez-Moranta F, Lopez A, et al. A new rapid quantitative test for fecal calprotectin predicts endoscopic activity in ulcerative colitis. Inflamm Bowel Dis. 2013;19:1034–42.
Kolho KL, Turner D. Fecal calprotectin and clinical disease activity in pediatric ulcerative colitis. ISRN Gastroenterol. 2013;2013:179024.
Halpin SJ, Ford AC. Prevalence of symptoms meeting criteria for irritable bowel syndrome in inflammatory bowel disease: systematic review and meta-analysis. Am J Gastroenterol. 2012;107:1474–82.
Pezzone MA, Wald A. Functional bowel disorders in inflammatory bowel disease. Gastroenterol Clin N Am. 2002;31:347–57.
Ginsburg PM, Bayless TM. Managing functional disturbances in patients with inflammatory bowel disease. Curr Treat Options Gastroenterol. 2005;8:211–21.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
HS, DD, PA, AJ, TG, AD, and TA declare that they have no conflict of interest.
Ethics statement
Approval for the analysis was obtained from the institution’s review board (P. D. Hinduja National Hospital and Medical Research Centre).The authors declare that the study was performed in a manner to conform with the Helsinki Declaration of 1975, as revised in 2000 and 2008 concerning Human and Animal Rights, and the authors followed the policy concerning Informed Consent as shown on Springer.com.
Rights and permissions
About this article
Cite this article
Samant, H., Desai, D., Abraham, P. et al. Fecal calprotectin and its correlation with inflammatory markers and endoscopy in patients from India with inflammatory bowel disease. Indian J Gastroenterol 34, 431–435 (2015). https://doi.org/10.1007/s12664-015-0608-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12664-015-0608-x