Abstract
Background
Prenatal diagnosis and planned peripartum care is an unexplored concept in China. This study aimed to evaluate the effects of the “prenatal diagnosis and postnatal treatment integrated model” for newborns with critical congenital heart disease.
Methods
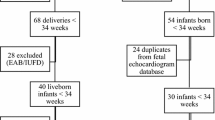
The medical records of neonates (≤ 28 days) admitted to Fuwai Hospital were reviewed retrospectively from January 2019 to December 2020. The patients were divided into “prenatal diagnosis and postnatal treatment integrated group” (n = 47) and “non-integrated group” (n = 69).
Results
The age of admission to the hospital and the age at surgery were earlier in the integrated group than in the non-integrated group (5.2 ± 7.2 days vs. 11.8 ± 8.0 days, P < 0.001; 11.9 ± 7.0 days vs. 16.5 ± 7.7 days, P = 0.001, respectively). The weight at surgery also was lower in the integrated group than in the non-integrated group (3.3 ± 0.4 kg vs. 3.6 ± 0.6 kg, P = 0.010). Longer postoperative recovery time was needed in the integrated group, with a median mechanical ventilation time of 97 h (interquartile range 51–259 h) vs. 69 h (29–168 h) (P = 0.030) and with intensive care unit time of 13.0 days (8.0–21.0 days) vs. 9.0 days (4.5–16.0 days) (P = 0.048). No significant difference was observed in the all-cause mortality (2.1 vs. 8.7%, P = 0.238), but it was significantly lower in the integrated group for transposition of the great arteries (0 vs. 18.8%, log rank P = 0.032).
Conclusions
The prenatal diagnosis and postnatal treatment integrated model could significantly shorten the diagnosis and hospitalization interval of newborns, and surgical intervention could be performed with a lower risk of death, especially for transposition of the great arteries.


Similar content being viewed by others
Data availability
The datasets generated and/or analyzed during the current study were available from the corresponding author on reasonable request.
References
Khoshnood B, Lelong N, Houyel L, Thieulin AC, Jouannic JM, Magnier S, et al. Prevalence, timing of diagnosis and mortality of newborns with congenital heart defects: a population-based study. Heart. 2012;98:1667–73.
Dolk H, Loane M, Garne E, European Surveillance of Congenital Anomalies (EUROCAT) Working Group. Congenital heart defects in Europe: prevalence and perinatal mortality, 2000 to 2005. Circulation. 2011;123:841–9.
Zhao QM, Liu F, Wu L, Ma XJ, Niu C, Huang GY. Prevalence of congenital heart disease at live birth in China. J Pediatr. 2019;204:53–8.
Holland BJ, Myers JA, Woods CR Jr. Prenatal diagnosis of critical congenital heart disease reduces risk of death from cardiovascular compromise prior to planned neonatal cardiac surgery: a meta-analysis. Ultrasound Obstet Gynecol. 2015;45:631–8.
Bakker MK, Bergman JEH, Krikov S, Amar E, Cocchi G, Cragan J, et al. Prenatal diagnosis and prevalence of critical congenital heart defects: an international retrospective cohort study. BMJ Open. 2019. https://doi.org/10.1136/bmjopen-2018-028139.
Costello JM, Pasquali SK, Jacobs JP, He X, Hill KD, Cooper DS, et al. Gestational age at birth and outcomes after neonatal cardiac surgery: an analysis of the society of thoracic surgeons congenital heart surgery database. Circulation. 2014;129:2511–7.
Kansy A, Tobota Z, Maruszewski P, Maruszewski B. Analysis of 14,843 neonatal congenital heart surgical procedures in the European Association for Cardiothoracic Surgery Congenital Database. Ann Thorac Surg. 2010;89:1255–9.
Chu C, Yan Y, Ren Y, Li X, Gui Y. Prenatal diagnosis of congenital heart diseases by fetal echocardiography in second trimester: a Chinese multicenter study. Acta Obstet Gynecol Scand. 2017;96:454–63.
Zhang X, Sun Y, Zhu J, Zhu Y, Qiu L. Epidemiology, prenatal diagnosis, and neonatal outcomes of congenital heart defects in eastern China: a hospital-based multicenter study. BMC Pediatr. 2020;20:416.
Lacour-Gayet F, Clarke D, Jacobs J, Comas J, Daebritz S, Daenen W, et al. The Aristotle score: a complexity-adjusted method to evaluate surgical results. Eur J Cardiothorac Surg. 2004;25:911–24.
Jacobs JP, Jacobs ML, Maruszewski B, Lacour-Gayet FG, Clarke DR, Tchervenkov CI, et al. Current status of the European association for cardio-thoracic surgery and the society of thoracic surgeons congenital heart surgery database. Ann Thorac Surg. 2005;80:2278–83 (Discussion 2283–4).
Su Z, Xiang L, Liu Z, Wu H, Li S, Chen H, et al. The current landscape of congenital heart surgery in northern china: a geographic and population-based analysis. Front Pediatr. 2021. https://doi.org/10.3389/fped.2021.555141.
Nagata H, Glick L, Lougheed J, Grattan M, Mondal T, Thakur V, et al. Prenatal diagnosis of transposition of the great arteries reduces postnatal mortality: a population-based study. Can J Cardiol. 2020;36:1592–7.
Quartermain MD, Hill KD, Goldberg DJ, Jacobs JP, Jacobs ML, Pasquali SK, et al. Prenatal diagnosis influences preoperative status in neonates with congenital heart disease: an analysis of the society of thoracic surgeons congenital heart surgery database. Pediatr Cardiol. 2019;40:489–96.
Bonnet D, Coltri A, Butera G, Fermont L, Le Bidois J, Kachaner J, et al. Detection of transposition of the great arteries in fetuses reduces neonatal morbidity and mortality. Circulation. 1999;99:916–8.
Seale AN, Uemura H, Webber SA, Partridge J, Roughton M, Ho SY, et al. Total anomalous pulmonary venous connection: morphology and outcome from an international population-based study. Circulation. 2010;122:2718–26.
Domadia S, Kumar SR, Votava-Smith JK, Pruetz JD. Neonatal outcomes in total anomalous pulmonary venous return: the role of prenatal diagnosis and pulmonary venous obstruction. Pediatr Cardiol. 2018;39:1346–54.
Yang L, He X, Lu Y, Huang F, Shi G, Chen H, et al. Integrated model for the prenatal diagnosis and postnatal surgical treatment of total anomalous pulmonary venous connection: a multidisciplinary collaborative experience and preliminary results. J Card Surg. 2019;34:1264–72.
Liu X, Hong HF, Zhang HB, Xu ZM, Liu JF, Zhang H. Neonatal surgical outcomes after prenatal diagnosis of complex congenital heart disease: experiences of a perinatal integrated diagnosis and treatment program. World J Pediatr. 2020;16:494–501.
Li SJ, Chen WD, Zhang Y, Zhang H, Hua ZD, Wang D, et al. Hybrid therapy for pulmonary atresia with intact ventricular septum. Ann Thorac Surg. 2011;91:1467–71.
Li SJ, Zhang H, Shen XD, Yan J, Deng XC, Chen WD, et al. Intraoperative hybrid cardiac surgery for neonates and young children with congenital heart disease: 5 years of experience. Ann Thorac Cardiovasc Surg. 2010;16:406–9.
Ou-Yang WB, Li SJ, Xie YQ, Hu SS, Wang SZ, Zhang FW, et al. Hybrid balloon valvuloplasty for the treatment of severe congenital aortic valve stenosis in infants. Ann Thorac Surg. 2018;105:175–80.
Zhao QM, Ma XJ, Ge XL, Liu F, Yan WL, Wu L, et al. Pulse oximetry with clinical assessment to screen for congenital heart disease in neonates in China: a prospective study. Lancet. 2014;384:747–54.
Acknowledgements
We gratefully acknowledged the doctors and nurses who were involved in the study.
Funding
This work was supported by National Key R & D Program of China (2017YFC1308100) and Beijing Municipal Science & Technology Commission (Z201100005520001).
Author information
Authors and Affiliations
Contributions
GXW collected and analyzed the data and drafted the manuscript. GXW, KM, KJP, XW, and SJL designed the study. KM, LQ, YY, and FQM contributed to the critical revision of the manuscript for important intellectual content, and SJL approved the final version of the manuscript. SJL obtained fundings. All the authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical approval
This retrospective study was conducted at department of pediatric cardiac surgery, Fuwai Hospital in Beijing, China. It was approved by our institutional ethics committee. The specific ethical number was 2017-977 and it was approved on November 30, 2019. The need for individual patient informed consent was waived.
Conflict of interest
No financial or nonfinancial benefits have been received or will be received from any party related directly or indirectly to the subject of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wang, GX., Ma, K., Pang, KJ. et al. Two approaches for newborns with critical congenital heart disease: a comparative study. World J Pediatr 18, 59–66 (2022). https://doi.org/10.1007/s12519-021-00482-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12519-021-00482-5