Abstract
Objective
The purpose of this study was to determine the clinical implication of the myocardial FDG uptake patterns by comparing with the results of stress myocardial perfusion imaging (MPI) as the reference standard.
Methods
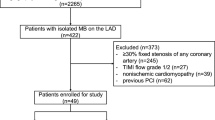
By reviewing the medical records, 86 pairs of stress MPI and FDG PET/CT of 84 patients who underwent stress MPI and oncologic FDG PET/CT in 1 month were included in this study. The patterns of the myocardial FDG uptake were classified into five patterns such as ‘low’, ‘diffuse’, ‘basal ring’, ‘focal high’, and ‘focal defect on diffuse high’. MPI was evaluated using a 5-point scoring model ranging from 0 (normal uptake) to 4 (uptake absent) based on the 17-segment model. The summed stress score of 4 or higher was defined as ‘abnormal MPI’. Factors predictive of abnormal MPI were analyzed using a log-rank multivariate test and p < 0.05 was set as significant.
Results
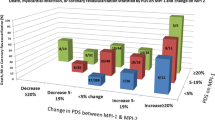
Abnormal MPI was observed in only 16 of 36 (44%) patients with ‘low’ pattern, 10 of 23 (43%) patients with ‘diffuse high’ pattern, and 1 of 9 (11%) patients with ‘basal ring’ pattern, but in 8 of 9 (89%) patients with ‘focal high’ pattern, and 8 of 9 (89%) patients with ‘focal defect on diffuse high’ pattern. The log-rank multivariate test revealed that ‘focal high’ and ‘focal defect on diffuse high’ pattern were correlated with an abnormal MPI.
Conclusions
These results indicate that further cardiac work-up might be helpful in the patients with ‘focal high’ pattern or ‘focal defect on diffuse high’ pattern of myocardial FDG at oncologic PET. A prospective study should be needed to further support this conclusion.



Similar content being viewed by others
References
Hillner BE, Siegel BA, Shields AF, Liu D, Gareen IF, Hanna L, et al. The impact of positron emission tomography (PET) on expected management during cancer treatment: findings of the National Oncologic PET Registry. Cancer. 2009;115(2):410–8.
Randle PJ, Garland PB, Hales CN, Newsholme EA. The glucose fatty-acid cycle its role in insulin sensitivity and the metabolic disturbances of diabetes mellitus. Lancet. 1963;1(7285):785–9.
Lucignani G, Paolini G, Landoni C, Zuccari M, Paganelli G, Galli L, et al. Presurgical identification of hibernating myocardium by combined use of technetium-99m hexakis 2-methoxyisobutylisonitrile single photon emission tomography and fluorine-18 fluoro-2-deoxy-D-glucose positron emission tomography in patients with coronary artery disease. Eur J Nucl Med. 1992;19(10):874–81.
Uehara T, Ishida Y, Hayashida K, Shimonagata T, Miyake Y, Sago M, et al. Myocardial glucose metabolism in patients with hypertrophic cardiomyopathy: assessment by F-18-FDG PET study. Ann Nucl Med. 1998;12(2):95–103.
Vilain D, Bochet J, Le Stanc E, Wattel C, Hameg A, Tainturier C. Unsuspected hibernating myocardium detected by routine oncology (18)F-FDG PET/CT. Eur J Nucl Med Mol Imaging. 2010;37(2):409.
Hiasa G, Okayama H, Kawaguchi N, Kazatani Y. Coronary artery disease incidentally detected by routine oncology F-18-fluorodeoxyglucose positron emission tomography. J Nucl Cardiol. 2018;25(2):688–90.
Minamimoto R, Morooka M, Miyata Y, Ito K, Okasaki M, Hara H, et al. Incidental focal FDG uptake in heart is a lighthouse for considering cardiac screening. Ann Nucl Med. 2013;27(6):572–80.
Yamanouchi M, Yoshida K, Niwayama H, Nakagawa K, Aioi S, Shikama N, et al. Effect of the duration of fasting on myocardial fluorine-18-fluorodeoxyglucose positron emission tomography images in normal males. Jpn Circ J. 1996;60(6):319–27.
Nose H, Otsuka H, Otomi Y, Terazawa K, Takao S, Iwamoto S, et al. The physiological uptake pattern of (18)F-FDG in the left ventricular myocardium of patients without heart disease. J Med Invest. 2014;61(1–2):53–8.
Maurer AH, Burshteyn M, Adler LP, Gaughan JP, Steiner RM. Variable cardiac 18FDG patterns seen in oncologic positron emission tomography computed tomography: importance for differentiating normal physiology from cardiac and paracardiac disease. J Thorac Imaging. 2012;27(4):263–8.
Takanami K, Arai A, Umezawa R, Takeuchi T, Kadoya N, Taki Y, et al. Association between radiation dose to the heart and myocardial fatty acid metabolic impairment due to chemoradiation-therapy: Prospective study using I-123 BMIPP SPECT/CT. Radiother Oncol. 2016;119:77.
Jingu K, Nemoto K, Kaneta T, Oikawa M, Ogawa Y, Ariga H, et al. Temporal change in brain natriuretic peptide after radiotherapy for thoracic esophageal cancer. Int J Radiat Oncol Biol Phys. 2007;69(5):1417–23.
Ramirez R, Trivieri M, Fayad ZA, Ahmadi A, Narula J, Argulian E. Advanced imaging in cardiac sarcoidosis. J Nucl Med. 2019;60(7):892–8.
Bauckneht M, Ferrarazzo G, Fiz F, Morbelli S, Sarocchi M, Pastorino F, et al. Doxorubicin effect on myocardial metabolism as a pre-requisite for subsequent development of cardiac toxicity: a translational 18F-FDG PET/CT observation. J Nucl Med. 2017;58:1638.
Tilkemeier PL, Bourque J, Doukky R, Sanghani R, Weinberg RL. ASNC imaging guidelines for nuclear cardiology procedures. J Nucl Cardiol. 2017;24(6):2064–128.
Berman DS, Kang XP, Van Train KF, Lewin HC, Cohen I, Areeda J, et al. Comparative prognostic value of automatic quantitative analysis versus semiquantitative visual analysis of exercise myocardial perfusion single-photon emission computed tomography. J Am Coll Cardiol. 1998;32(7):1987–95.
Holly TA, Abbott BG, Al-Mallah M, Calnon DA, Cohen MC, DiFilippo FP, et al. Single photon-emission computed tomography. J Nucl Cardiol. 2010;17(5):941–73.
Viera AJ, Garrett JM. Understanding interobserver agreement: the kappa statistic. Fam Med. 2005;37(5):360–3.
Dilsizian V, Bacharach SL, Beanlands RS, Bergmann SR, Delbeke D, Dorbala S, et al. ASNC imaging guidelines/SNMMI procedure standard for positron emission tomography (PET) nuclear cardiology procedures. J Nucl Cardiol. 2016;23(5):1187–226.
Abbott BG, Liu YH, Arrighi JA. [18F]Fluorodeoxyglucose as a memory marker of transient myocardial ischaemia. Nucl Med Commun. 2007;28(2):89–94.
Lyall A, Capobianco J, Strauss HW, Gonen M, Schoder H. Treadmill exercise inducing mild to moderate ischemia has no significant effect on skeletal muscle or cardiac 18F-FDG uptake and image quality on subsequent whole-body PET scan. J Nucl Med. 2012;53(6):917–21.
Dou KF, Xie BQ, Gao XJ, Li Y, Yang YJ, He ZX, et al. Use of resting myocardial 18F-FDG imaging in the detection of unstable angina. Nucl Med Commun. 2015;36(10):999–1006.
de Groot M, Meeuwis AP, Kok PJ, Corstens FH, Oyen WJ. Influence of blood glucose level, age and fasting period on non-pathological FDG uptake in heart and gut. Eur J Nucl Med Mol Imaging. 2005;32(1):98–101.
Schatka I, Bengel FM. Advanced imaging of cardiac sarcoidosis. J Nucl Med. 2014;55(1):99–106.
Bertagna F, Treglia G. Comment on Minamimoto: incidental focal FDG uptake in heart is a lighthouse for considering cardiac screening. Ann Nucl Med. 2013;27(9):870–1.
Fukuchi K, Ohta H, Matsumura K, Ishida Y. Benign variations and incidental abnormalities of myocardial FDG uptake in the fasting state as encountered during routine oncology positron emission tomography studies. Brit J Radiol. 2007;80(949):3–11.
Abel ED. Glucose transport in the heart. Front Biosci. 2004;9:201–15.
Israel O, Weiler-Sagie M, Rispler S, Bar-Shalom R, Frenkel A, Keidar Z, et al. PET/CT quantitation of the effect of patient-related factors on cardiac 18F-FDG uptake. J Nucl Med. 2007;48(2):234–9.
Gibbons RJ, Chatterjee K, Daley J, Douglas JS, Fihn SD, Gardin JM, et al. ACC/AHA/ACP-ASIM guidelines for the management of patients with chronic stable angina: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee on Management of Patients With Chronic Stable Angina). J Am Coll Cardiol. 1999;33(7):2092–197.
Kapur A, Latus KA, Davies G, Dhawan RT, Eastick S, Jarritt PH, et al. A comparison of three radionuclide myocardial perfusion tracers in clinical practice: the ROBUST study. Eur J Nucl Med Mol Imaging. 2002;29(12):1608–16.
Taillefer R, DePuey EG, Udelson JE, Beller GA, Latour Y, Reeves F. Comparative diagnostic accuracy of Tl-201 and Tc-99m sestamibi SPECT imaging (perfusion and ECG-gated SPECT) in detecting coronary artery disease in women. J Am Coll Cardiol. 1997;29(1):69–77.
Dai N, Zhang X, Zhang Y, Hou L, Li W, Fan B, et al. Enhanced diagnostic utility achieved by myocardial blood analysis: a meta-analysis of noninvasive cardiac imaging in the detection of functional coronary artery disease. Int J Cardiol. 2016;221:665–73.
Danad I, Raijmakers PG, Driessen RS, Leipsic J, Raju R, Naoum C, et al. Comparison of coronary CT angiography, SPECT, PET, and hybrid imaging for diagnosis of ischemic heart disease determined by fractional flow reserve. JAMA Cardiol. 2017;2(10):1100–7.
Danad I, Szymonifka J, Twisk JR, Norgaard BL, Zarins CK, Knaapen P, et al. Diagnostic performance of cardiac imaging methods to diagnose ischaemia-causing coronary artery disease when directly compared with fractional flow reserve as a reference standard: a meta-analysis. Eur Heart J. 2017;38(13):991.
Gaemperli O, Schepis T, Valenta I, Koepfli P, Husmann L, Scheffel H, et al. Functionally relevant coronary artery disease: comparison of 64-section CT angiography with myocardial perfusion SPECT. Radiology. 2008;248(2):414–23.
Hacker M, Jakobs T, Matthiesen F, Vollmar C, Nikolaou K, Becker C, et al. Comparison of spiral multidetector CT angiography and myocardial perfusion imaging in the noninvasive detection of functionally relevant coronary artery lesions: first clinical experiences. J Nucl Med. 2005;46(8):1294–300.
Miller TD, Roger VL, Milavetz JJ, Hopfenspirger MR, Milavetz DL, Hodge DO, et al. Assessment of the exercise electrocardiogram in women versus men using tomographic myocardial perfusion imaging as the reference standard. Am J Cardiol. 2001;87(7):868–73.
Nakahara T, Toyama T, Jinzaki M, Seki R, Saito Y, Higuchi T, et al. Quantitative analysis of iodine image of dual-energy computed tomography at rest comparison With Tc-99m-tetrofosmin stress-rest single-photon emission computed tomography myocardial perfusion imaging as the reference standard. J Thorac Imag. 2018;33(2):97–104.
Schuijf JD, Wijns W, Jukema JW, Atsma DE, de Roos A, Lamb HJ, et al. Relationship between noninvasive coronary angiography with multi-slice computed tomography and myocardial perfusion imaging. J Am Coll Cardiol. 2006;48(12):2508–14.
Bauckneht M, Ferrarazzo G, Fiz F, Morbelli S, Sarocchi M, Pastorino F, et al. Doxorubicin effect on myocardial metabolism as a prerequisite for subsequent development of cardiac toxicity: a translational F-18-FDG PET/CT observation. J Nucl Med. 2017;58(10):1638–45.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No potential conflicts of interest were disclosed.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee (include name of committee + reference number) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Takanami, K., Saito, M., Matsumoto, Y. et al. Clinical implication of myocardial FDG uptake pattern in oncologic PET: retrospective comparison study with stress myocardial perfusion imaging as the reference standard. Ann Nucl Med 34, 233–243 (2020). https://doi.org/10.1007/s12149-020-01437-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12149-020-01437-y