Abstract
Objective
Metabolic tumor volume (MTV) and total lesion glycolysis (TLG) are imaging parameters derived from 18F-FDG PET/CT that have been proposed for risk stratification of cancer patients. The aim of our study was to test whether these whole-body volumetric imaging parameters may predict outcome in patients with non-small cell lung cancer (NSCLC).
Methods
Sixty-five patients (45 men, 20 women; mean age ± SD, 65 ± 12 years), with histologically proven NSCLC who had undergone 18F-FDG PET/CT scan before any therapy, were included in the study. Imaging parameters including SUVmax, SUVmean, total MTV (MTVTOT) and whole-body TLG (TLGWB) were determined. Univariate and multivariate analyses of clinical and imaging variables were performed using Cox proportional hazards regression. Survival analysis was performed using Kaplan–Meier method and log-rank tests.
Results
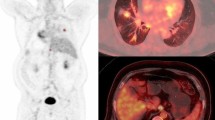
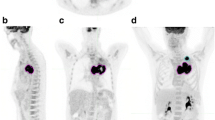
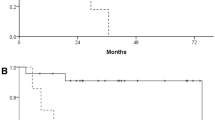
A total of 298 lesions were analyzed including 65 primary tumors, 114 metastatic lymph nodes and 119 distant metastases. MTVTOT and TLGWB could be determined in 276 lesions. Mean value of MTVTOT was 81.83 ml ± 14.63 ml (SE) whereas mean value of TLGWB was 459.88 g ± 77.02 g (SE). Univariate analysis showed that, among the variables tested, primary tumor diameter (p = 0.0470), MTV of primary tumor (p = 0.0299), stage (p < 0.0001), treatment (p < 0.0001), MTVTOT (p = 0.0003) and TLGWB (p = 0.0002) predicted progression-free survival in NSCLC patients, while age (p = 0.0550), MTV of primary tumor (p = 0.0375), stage (p < 0.0001), treatment (p < 0.0001), MTVTOT (p = 0.0001) and TLGWB (p = 0.0008) predicted overall survival. At multivariate analysis age, TLGWB and stage were retained in the model for prediction of progression-free survival (p < 0.0001), while age, MTVTOT and stage were retained in the model for prediction of overall survival (p < 0.0001). Survival analysis showed that patients with TLGWB ≤ 54.7 g had a significantly prolonged progression-free survival as compared to patients with TLGWB > 54.7 g (p < 0.0001). Moreover, overall survival was significantly better in patients showing a MTVTOT ≤ 9.5 ml as compared to those having MTVTOT > 9.5 ml (p < 0.0001). Similar results were obtained in a subgroup of 43 patients with advanced disease (stages III and IV).
Conclusions
Whole-body PET-based volumetric imaging parameters are able to predict outcome in NSCLC patients.




Similar content being viewed by others
References
Ferlay J, Soerjomataram I, Dikshit R, Eser S, Mathers C, Rebelo M, et al. Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN 2012. Int J Cancer. 2015;136:E359–E386386.
Herbst RS, Morgensztern D, Boshoff C. The biology and management of non-small cell lung cancer. Nature. 2018;553:446–54.
Jones CM, Brunelli A, Callister ME, Franks KN. Multimodality treatment of advanced non-small cell lung cancer: where are we with the evidence? Curr Surg Rep. 2018;6:5.
Detterbeck FC, Boffa DJ, Kim AW, Tanoue LT. The eighth edition lung cancer stage classification. Chest. 2017;151:193–203.
Lababede O, Meziane M, Rice T. Seventh edition of the cancer staging manual and stage grouping of lung cancer: quick reference chart and diagrams. Chest. 2011;139:183–9.
Spadafora M, Pace L, Evangelista L, Mansi L, Del Prete F, Saladini G, et al. Risk-related (18)F-FDG PET/CT and new diagnostic strategies in patients with solitary pulmonary nodule: the ITALIAN multicenter trial. Eur J Nucl Med Mol Imaging. 2018;45:1908–14.
Sauter AW, Schwenzer N, Divine MR, Pichler BJ, Pfannenberg C. Image-derived biomarkers and multimodal imaging strategies for lung cancer management. Eur J Nucl Med Mol Imaging. 2015;42:634–43.
Higashi K, Matsunari I, Ueda Y, Ikeda R, Guo J, Oguchi M, et al. Value of whole-body FDG PET in management of lung cancer. Ann Nucl Med. 2003;17:1–14.
Hutchings M, Barrington SF. PET/CT for therapy response assessment in lymphoma. J Nucl Med. 2009;50(Suppl 1):21S–30S.
Fonti R, Pace L, Cerchione C, Catalano L, Salvatore B, De Luca S, et al. 18F-FDG PET/CT, 99mTc-MIBI, and MRI in the prediction of outcome of patients with multiple myeloma: a comparative study. Clin Nucl Med. 2015;40:303–8.
Van de Wiele C, Kruse V, Smeets P, Sathekge M, Maes A. Predictive and prognostic value of metabolic tumour volume and total lesion glycolysis in solid tumours. Eur J Nucl Med Mol Imaging. 2013;40:290–301.
Park SY, Lee SJ, Yoon JK. The prognostic value of total lesion glycolysis via 18F-fluorodeoxyglucose PET-CT in surgically treated esophageal squamous cell carcinoma. Ann Nucl Med. 2016;30:81–8.
Ouyang ML, Xia HW, Xu MM, Lin J, Wang LL, Zheng XW, et al. Prediction of occult lymph node metastasis using SUV, volumetric parameters and intratumoral heterogeneity of the primary tumor in T1–2N0M0 lung cancer patients staged by PET/CT. Ann Nucl Med. 2019;33:671–80.
Berghmans T, Dusart M, Paesmans M, Hossein-Foucher C, Buvat I, Castaigne C, et al. Primary tumor standardized uptake value (SUVmax) measured on fluorodeoxyglucose positron emission tomography (FDG-PET) is of prognostic value for survival in non-small cell lung cancer (NSCLC): a systematic review and meta-analysis (MA) by the European Lung Cancer Working Party for the IASLC Lung Cancer Staging Project. J Thorac Oncol. 2008;3:6–12.
Paesmans M, Berghmans T, Dusart M, Garcia C, Hossein-Foucher C, Lafitte JJ, et al. Primary tumor standardized uptake value measured on fluorodeoxyglucose positron emission tomography is of prognostic value for survival in non-small cell lung cancer: update of a systematic review and meta-analysis by the European Lung Cancer Working Party for the International Association for the Study of Lung Cancer Staging Project. J Thorac Oncol. 2010;5:612–9.
Davison J, Mercier G, Russo G, Subramaniam RM. PET-based primary tumor volumetric parameters and survival of patients with non-small cell lung carcinoma. Am J Roentgenol. 2013;200:635–40.
Im HJ, Pak K, Cheon GJ, Kang KW, Kim SJ, Kim IJ, et al. Prognostic value of volumetric parameters of (18)F-FDG PET in non-small-cell lung cancer: a meta-analysis. Eur J Nucl Med Mol Imaging. 2015;42:241–51.
Tamura T, Kurishima K, Nakazawa K, Kagohashi K, Ishikawa H, Satoh H, et al. Specific organ metastases and survival in metastatic non-small-cell lung cancer. Mol Clin Oncol. 2015;3:217–21.
Liao S, Penney BC, Wroblewski K, Zhang H, Simon CA, Kampalath R, et al. Prognostic value of metabolic tumor burden on 18F-FDG PET in nonsurgical patients with non-small cell lung cancer. Eur J Nucl Med Mol Imaging. 2012;39:27–38.
Finkle JH, Jo SY, Ferguson MK, Liu HY, Zhang C, Zhu X, et al. Risk-stratifying capacity of PET/CT metabolic tumor volume in stage IIIA non-small cell lung cancer. Eur J Nucl Med Mol Imaging. 2017;44:1275–84.
Bazan JG, Duan F, Snyder BS, Horng D, Graves EE, Siegel BA, et al. Metabolic tumor volume predicts overall survival and local control in patients with stage III non-small cell lung cancer treated in ACRIN 6668/RTOG 0235. Eur J Nucl Med Mol Imaging. 2017;44:17–24.
Fonti R, Larobina M, Del Vecchio S, De Luca S, Fabbricini R, Catalano L, et al. Metabolic tumor volume assessed by 18F-FDG PET/CT for the prediction of outcome in patients with multiple myeloma. J Nucl Med. 2012;53:1829–35.
Iommelli F, De Rosa V, Gargiulo S, Panico M, Monti M, Greco A, et al. Monitoring reversal of MET-mediated resistance to EGFR tyrosine kinase inhibitors in non-small cell lung cancer using 3'-deoxy-3'-[18F]-fluorothymidine positron emission tomography. Clin Cancer Res. 2014;20:4806–15.
Ilyas H, Mikhaeel NG, Dunn JT, Rahman F, Moller H, Smith D, et al. Defining the optimal method for measuring baseline metabolic tumour volume in diffuse large B cell lymphoma. Eur J Nucl Med Mol Imaging. 2018;45:1142–54.
Werner-Wasik M, Nelson AD, Choi W, Arai Y, Faulhaber PF, Kang P, et al. What is the best way to contour lung tumors on PET scans? Multiobserver validation of a gradient-based method using a NSCLC digital PET phantom. Int J Radiat Oncol Biol Phys. 2012;82:1164–71.
Liu J, Dong M, Sun X, Li W, Xing L, Yu J. Prognostic value of 18F-FDG PET/CT in surgical non-small cell lung cancer: a meta-analysis. PLoS ONE. 2016;11:e0146195.
Lapa P, Oliveiros B, Marques M, Isidoro J, Alves FC, Costa JMN, et al. Metabolic tumor burden quantified on [(18)F]FDG PET/CT improves TNM staging of lung cancer patients. Eur J Nucl Med Mol Imaging. 2017;44:2169–78.
Chen HH, Chiu NT, Su WC, Guo HR, Lee BF. Prognostic value of whole-body total lesion glycolysis at pretreatment FDG PET/CT in non-small cell lung cancer. Radiology. 2012;264:559–66.
Kaira K, Higuchi T, Naruse I, Arisaka Y, Tokue A, Altan B, et al. Metabolic activity by (18)F-FDG-PET/CT is predictive of early response after nivolumab in previously treated NSCLC. Eur J Nucl Med Mol Imaging. 2018;45:56–66.
Acknowledgements
This work was partly supported by Associazione Italiana per la Ricerca sul Cancro (AIRC, project no. IG-17249) and Programma Operativo Regionale POR Campania, Fondo Europeo Sviluppo Regionale 2014/2020.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No potential conflicts of interest were disclosed.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Pellegrino, S., Fonti, R., Mazziotti, E. et al. Total metabolic tumor volume by 18F-FDG PET/CT for the prediction of outcome in patients with non-small cell lung cancer. Ann Nucl Med 33, 937–944 (2019). https://doi.org/10.1007/s12149-019-01407-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12149-019-01407-z