Abstract
Objectives
To report data on Idiopathic inflammatory myopathies (IIM) from eastern India.
Methods
All IIM patients diagnosed over the last 5 y (2011–2016) were included through a retrospective review of records from the hospital and specialty clinic at Institute of Postgraduate Medical Education & Research (I.P.G.M.E.&R.), Kolkata.
Results
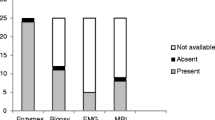
Out of the 11 IIM patients, 9 had Juvenile dermatomyositis (JDM) and 2 had overlap myositis (OM) [with systemic lupus erythematosus (SLE) and scleroderma]. The overall sex ratio was M: F = 1: 2.6. The mean age at diagnosis was 6.94 y for JDM and 7 y for OM. The mean interval from onset to diagnosis was 5.2 mo. All patients had heliotrope rash and proximal myopathy (n = 11,100%). Other findings included Gottron papule (n = 7; 64%), arthritis (n = 6; 54%), malar rash (n = 5; 45%), dysphagia (n = 4; 36%), nasal intonation (n = 3; 27%), subcutaneous nodule (n = 2; 18%), cutaneous sinus (n = 1; 9%), calcinosis universalis (n = 1; 9%), GI bleed (n = 1; 9%). All patients had raised erythrocyte sedimentation rate (ESR), aspartate aminotransferase (AST), lactate dehydrogenase (LDH) while 10 had raised creatine kinase (CK). Three were anti-nuclear-antibody (ANA) positive. Electromyography (EMG) showed proximal myopathy in most cases (n = 9; 82%). All patients received corticosteroid. Intravenous immunoglobulin (IVIG) was given to 2 patients. Two received hydroxychloroquine. Cyclophosphamide and azathioprine were given in one each.
Conclusions
This study, first reported profile of IIM from eastern India, showed JDM as the commonest form of IIM with a female preponderance. Five children had complete and 2 had partial remission. Two patients of JDM and 1 of OM died. Increased awareness, early referral, prompt diagnosis and treatment might improve the outcome and survival.


Similar content being viewed by others
References
Dimachkie MM, Barohn RJ, Amato AA. Idiopathic inflammatory myopathies. Neurol Clin. 2014;32:595–628.
Lazarou IN, Guerne PA. Classification, diagnosis, and management of idiopathic inflammatory myopathies. J Rheumatol. 2013;40:550–64.
Lorenzoni PJ, Scola RH, Kay CS, Prevedello PG, Espíndola G, Werneck LC. Idiopathic inflammatory myopathies in childhood: a brief review of 27 cases. Pediatr Neurol. 2011;45:17–22.
Rider LG, Lindsley CB, Miller FW. Juvenile dermatomyositis. In: Petty RE, Laxer RM, Lindsley CB, Lucy Wedderburn L, editors. Textbook of Pediatric Rheumatology. 7th ed. Philadelphia: Saunders; 2016. p. 351–83.
Singh S, Kumar L, Shankar KR. Juvenile dermatomyositis in North India. Indian Pediatr. 1997;34:193–8.
Singh S, Bansal A. Twelve years experience of juvenile dermatomyositis in North India. Rheumatol Int. 2006;26:510–5.
Singh S, Suri D, Aulakh R, Gupta A, Rawat A, Kumar RM. Mortality in children with juvenile dermatomyositis: two decades of experience from a single tertiary care centre in North India. Clin Rheumatol. 2014;33:1675–9.
Khubchandani RP, Mankad D, Chickermane PR. Disease patterns in juvenile dermatomyositis patients from Mumbai, India. Pediatr Rheumatol Online J. 2011;9:P53.
Chickermane PR, Mankad D, Khubchandani RP. Disease patterns of juvenile dermatomyositis from western India. Indian Pediatr. 2013;50:961–3.
Chowdhary V, Wakhlu A, Aggarwal A, Misra R. Outcome in juvenile dermatomyositis. Indian Pediatr. 2002;39:931–5.
Prasad S, Misra R, Agarwal V, Lawrence A, Aggarwal A. Juvenile dermatomyositis at a tertiary care hospital: is there any change in the last decade? Int J Rheum Dis. 2013;16:556–60.
Bohan A, Peter JB. Polymyositis and dermatomyositis (second of two parts). N Engl J Med. 1975;292:403–7.
McCann LJ, Juggins AD, Maillard SM, et al. The juvenile dermatomyositis National Registry and repository (UK and Ireland)- clinical characteristics of children recruited within the first 5 yr. Rheumatology. 2006;45:1255–60.
Mathiesen PR, Zak M, Herlin T, Nielsen SM. Clinical features and outcome in a Danish cohort of juvenile dermatomyositis patients. Clin Exp Rheumatol. 2010;28:782–9.
Sallum AM, Kiss MH, Sachetti S, et al. Juvenile dermatomyositis: clinical, laboratorial, histological, therapeutical and evolutive parameters of 35 patients. Arq Neuropsiquiatr. 2002;60:889–99.
Pachman LM, Hayford JR, Chung A, et al. Juvenile dermatomyositis at diagnosis: clinical characteristics of 79 children. J Rheumatol. 1998;25:1198–204.
Mondal R, Sarkar S, Nandi M, et al. Overlap syndrome: a child cohort. Indian J Pediatr. 2013;80:434–5.
Jayanthi MR, Basher RK, Bhadada SK, Bhattacharya A, Mittal BR. A case of adult dermatomyositis with calcinosis universalis. Indian J Nucl Med. 2014;29:278–9.
Terroso G, Bernardes M, Aleixo A, et al. Therapy of calcinosis universalis complicating adult dermatomyositis. Acta Reumatol Port. 2013;38:44–8.
Touimy M, Janani S, Rachidi W, Etaouil N, Mkinsi O. Calcinosis universalis complicating juvenile dermatomyositis: improvement after intravenous immunoglobulin therapy. Joint Bone Spine. 2013;80:108–9.
Jazayeri SB, Mehdizadeh M, Shahlaee A. Sketched x-rays: calcinosis universalis. Eur J Pediatr. 2012;171:1577–8.
Yun SJ, Lee JB, Kim SJ, Lee SC, Won YH, Kang HC. Calcinosis cutis universalis with joint contractures complicating juvenile dermatomyositis. Dermatology. 2006;212:401–3.
Boelch SP, Barthel T, Goebel S, Rudert M, Plumhoff P. Calcinosis universalis of the elbow: a rare case with classical presentation. Case Rep Orthop. 2015;2015:505420. doi:10.1155/2015/505420.
Malik A, Hayat G, Kalia JS, Guzman MA. Idiopathic inflammatory myopathies: clinical approach and management. Front Neurol. 2016;7:64.
Malattia C, Damasio MB, Madeo A, et al. Whole-body MRI in the assessment of disease activity in juvenile dermatomyositis. Ann Rheum Dis. 2014;73:1083–90.
Enders FB, Bader-Meunier B, Baildam E, et al. Consensus-based recommendations for the management of juvenile dermatomyositis. Ann Rheum Dis. 2016. doi:10.1136/annrheumdis-2016-209247.
Huber AM. Idiopathic inflammatory myopathies in childhood: current concepts. Pediatr Clin N Am. 2012;59:365–80.
Huber AM, Giannini EH, Bowyer SL, et al. Protocols for the initial treatment of moderately severe juvenile dermatomyositis: results of a Children's arthritis and rheumatology research alliance consensus conference. Arthritis Care Res (Hoboken). 2010;62:219–25.
Huber AM, Mamyrova G, Lachenbruch PA, et al. Childhood myositis heterogeneity collaborative study group. Early illness features associated with mortality in the juvenile idiopathic inflammatory myopathies. Arthritis Care Res. 2014;66:732–40.
Ravelli A, Trail L, Ferrari C, et al. Long-term outcome and prognostic factors of juvenile dermatomyositis: a multinational, multicenter study of 490 patients. Arthritis Care Res. 2010;62:63–72.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
SD, RM, SS, AS were involved in management of cases. TM and AS collected the data, drafted the manuscript, did the analysis of cases. AS, SS, TM searched the literature. SD,SS, TM did the critical review. All the authors approved the final version of the manuscript. SD remains the guarantor.
Compliance with Ethical Standards
ᅟ
Conflict of Interest
None.
Source of Funding
None.
Rights and permissions
About this article
Cite this article
Sarkar, S., Mondal, T., Saha, A. et al. Profile of Pediatric Idiopathic Inflammatory Myopathies from a Tertiary Care Center of Eastern India. Indian J Pediatr 84, 299–306 (2017). https://doi.org/10.1007/s12098-017-2302-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12098-017-2302-8