Abstract
Background
To compare toxicities in relation to standard radiation treatments [conventional fractionation RT (CRT) and moderate hypofractionated RT (MRT)] with ultrahypofractionated RT (URT) in the treatment of patients with localized PCa.
Methods
A searched was performed in Medline, Embase, Cochrane CENTRAL, and LILACS to January 2020 for studies comparing URT to CRT and/or MRT in relation to genitourinary (GU) and gastrointestinal (GI) toxicity in the treatment of patients with localized PCa. URT, MRT and CRT were defined as protocols delivering a daily dose of ≥5 Gy, 2.4–4.9 Gy, and <2.4 Gy per fractions regardless total dose, respectively.
Results
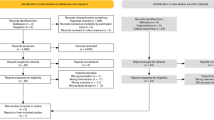
Eight studies with 2929 patients with localized PCa were included in the analysis. These eight studies did not find any difference between URT and MRT/CRT groups in relation to acute GU toxicity (21.0% × 23.8%, RD −0.04; 95% CI −0.13, 0.06; p = 0.46; I2 = 89%) and acute GI toxicity (4.9% × 6.9%, RD −0.03; 95% CI −0.07, 0.01; p = 0.21; I2 = 79%). Six studies did not find any difference between URT and MRT/CRT groups in relation to late GU toxicity (3.9% × 4.7%, RD −0.01; 95% CI −0.03, 0.00; p = 0.16; I2 = 19%) and late GI toxicity (2.1% × 3.5%, RD −0.01; 95% CI −0.03, 0.00; p = 0.05; I2 = 22%).
Conclusion
The present study suggests that acute GU/GI and late GU/GI toxicity are similar between URT and standard protocols. More studies with longer follow-ups directed to oncology outcomes are warranted before any recommendation on this topic.





Similar content being viewed by others
References
Ferlay J, Ervik M, Lam F, Colombet M, Mery L, Piñeros M, et al. Global cancer observatory: cancer today. Lyon, France: International Agency for Research on Cancer. 2020. Available from: https://gco.iarc.fr/today. Accessed 02 June 2021.
Gandaglia G, Leni R, Bray F, Fleshner N, Freedland SJ, Kibel A, Stattin P, Van Poppel H, La Vecchia C. Epidemiology and prevention of prostate cancer. Eur Urol Oncol. 2021;S2588–9311(21):00181–4.
Carvalho ÍT, Baccaglini W, Claros OR, Chen FK, Kayano PP, Lemos GC, et al. Genitourinary and gastrointestinal toxicity among patients with localized prostate cancer treated with conventional versus moderately hypofractionated radiation therapy: systematic review and meta-analysis. Acta Oncol (Madr). 2018;57(8):1003–10.
Greco C, Pimentel N, Pares O, Louro V, Fuks ZY. Single-dose radiotherapy (SDRT) in the management of intermediate risk prostate cancer: early results from a phase II randomized trial. J Clin Oncol. 2018;36(6 suppl):128. https://doi.org/10.1200/JCO.2018.36.6_suppl.128.
Cancer Therapy Evaluation Program (CTEP). Common terminology criteria for adverse events (CTCAE).v.5.0 [5x7]. Cancer Ther Eval Progr [Internet]. 2017;155. Available from: https://ctep.cancer.gov/protocolDevelopment/electronic_applications/ctc.htm#ctc_50
Group RTO. RTOG/EORTC late radiation morbidity scoring schema. 2014. p. 2–3.
Moher D, Liberati A, Tetzlaff J, Altman DG. Preferred reporting items for systematic reviews and meta-analyses : the PRISMA statement. PLoS Med. 2009;6(7):e1000097.
Nicosia L, Mazzola R, Rigo M, Figlia V, Giaj N, Giuseppe L. Moderate versus extreme hypofractionated radiotherapy: a toxicity comparative analysis in low and favorable intermediate risk prostate cancer patients. J Cancer Res Clin Oncol. 2019. https://doi.org/10.1007/s00432-019-02983-3.
Marvaso G, Ciardo D, Gandini S, Riva G, Frigo E, Volpe S, et al. Comparison of outcomes and toxicity between extreme and moderate radiation therapy hypofractionation in localized prostate cancer: a propensity score analysis. Radiat Oncol Biol. 2019. https://doi.org/10.1016/j.ijrobp.2019.07.027.
Ha B, Cho KH, Lee KH, Joung JY, Kim Y, Lee SU, et al. Long-term results of a phase II study of hypofractionated proton therapy for prostate cancer: moderate versus extreme hypofractionation. Radiat Oncol. 2019;14:1–9.
Franzese C, D’Agostino G, Di Brian L, Navarria P, De Rose F, Comito T, et al. Linac-based stereotactic body radiation therapy vs moderate hypofractionated radiotherapy in prostate cancer: propensity-score based comparison of outcome and toxicity. Br J Radiol. 2019;92(1097):20190021.
Widmark A, Gunnlaugsson A, Beckman L, Thellenberg-karlsson C, Hoyer M, Lagerlund M, et al. Articles ultra-hypofractionated versus conventionally fractionated radiotherapy for prostate cancer: 5-year outcomes of the HYPO-RT-PC randomised, non-inferiority, phase 3 trial. Lancet. 2019;6736(19):1–11.
Brand DH, Tree AC, Ostler P, Van Der VH, Loblaw A, Chu W, et al. Articles intensity-modulated fractionated radiotherapy versus stereotactic body radiotherapy for prostate cancer (PACE-B): acute toxicity findings from an international, randomised, open-label, phase 3, non-inferiority trial. Lancet Oncol. 2019;2045(19):1–13.
Głowacki G, Majewski W, Wojcieszek P, Grabinska K, Wozniak G, Miszczyk L, et al. Ultrahypofractionated CyberKnife TM based stereotactic radiotherapy versus conventional radiotherapy in patients with prostate cancer—acute toxicity evaluation in two phase II prospective studies. Neoplasma. 2017;64:599–604.
Vargas ACE, Schmidt MQ, Hartsell WF, Sameer R, Doh L, Chang JH, et al. Trial of hypofractionated versus standard fractionated proton therapy for low-risk. Adv Radiat Oncol. 2018. https://doi.org/10.1016/j.adro.2018.02.004.
Brenner DJ, Martinez AA, Edmundson GK, Mitchell C, Thames HD, Armour EP. Direct evidence that prostate tumors show high sensitivity to fractionation (low α/β ratio), similar to late-responding normal tissue. Int J Radiat Oncol Biol Phys. 2002;52(1):6–13.
Katz AJ, Santoro M, Diblasio F, Ashley R. Stereotactic body radiotherapy for localized prostate cancer: disease control and quality of life at 6 years. Radiat Oncol. 2013;8(1):1.
Hegemann NS, Guckenberger M, Belka C, Ganswindt U, Manapov F, Li M. Hypofractionated radiotherapy for prostate cancer. Radiat Oncol. 2014;9(1):1–15.
Zerini D, Jereczek-Fossa BA, Vavassori A, Bossi-Zanetti I, Mauro R, Ivaldi GB, et al. 3D-conformal hypofractionated radiotherapy for prostate cancer with daily transabdominal ultrasonography prostate localization: toxicity and outcome of a pilot study. Tumori. 2010;96:941–6.
Kang JK, Cho CK, Choi CW, Yoo SY, Kim MS, Yang KM, et al. Image-guided stereotactic body radiation therapy for localized prostate cancer. Tumori. 2011;97:43–8.
Hofman MS, Violet J, Hicks RJ, Ferdinandus J, Ping Thang S, Akhurst T, et al. [177 Lu]-PSMA-617 radionuclide treatment in patients with metastatic castration-resistant prostate cancer (LuPSMA trial): a single-centre, single-arm, phase 2 study. Lancet Oncol. 2018;19(6):825–33. https://doi.org/10.1016/S1470-2045(18)30198-0.
Madsen BL, Hsi RA, Pham HT, Fowler JF, Esagui L, Corman J. Stereotactic hypofractionated accurate radiotherapy of the prostate (SHARP), 33.5 Gy in five fractions for localized disease: first clinical trial results. Int J Radiat Oncol Biol Phys. 2007;67(4):1099–105.
King CR, Brooks JD, Gill H, Pawlicki T, Cotrutz C, Presti JC. Stereotactic body radiotherapy for localized prostate cancer: interim results of a prospective phase II clinical trial. Int J Radiat Oncol Biol Phys. 2009;73(4):1043–8.
Sander L, Langkilde NC, Holmberg M, Carl J. MRI target delineation may reduce long-term toxicity after prostate radiotherapy. Acta Oncol (Madr). 2014;53(6):809–14.
Kasaova L, Sirak I, Jansa J, Paluska P, Petera J. Quantitative evaluation of the benefit of fiducial image-guidance for prostate cancer intensity modulated radiation therapy using daily dose volume histogram analysis. Technol Cancer Res Treat. 2014;13(1):47–55.
Michalski JM, Yan Y, Watkins-Bruner D, Bosch WR, Winter K, Galvin JM, et al. Preliminary toxicity analysis of 3-dimensional conformal radiation therapy versus intensity modulated radiation therapy on the high-dose arm of the Radiation Therapy Oncology Group 0126 prostate cancer trial. Int J Radiat Oncol Biol Phys. 2013;87(5):932–8. https://doi.org/10.1016/j.ijrobp.2013.07.041.
Mendenhall NP, Hoppe BS, Nichols RC, Mendenhall WM, Morris CG, Li Z, et al. Five-year outcomes from 3 prospective trials of image-guided proton therapy for prostate cancer. Int J Radiat Oncol Biol Phys. 2014;88(3):596–602. https://doi.org/10.1016/j.ijrobp.2013.11.007.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Ethical approval
This article does not contain any studies with human or animal subjects performed by the any of the authors.
Informed consent
For this type of study informed consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary data 1.
Acute genitourinary toxicity—comparison between URT and MRT/CRT considering only RCT. (PDF 185 KB)
Supplementary data 2.
Acute gastrointestinal toxicity—comparison between URT and MRT/CRT considering only RCT. (PDF 169 KB)
Supplementary data 3.
Late genitourinary toxicity—comparison between URT and MRT/CRT considering only RCT. (PDF 154 KB)
Supplementary data 4.
Late gastrointestinal toxicity—comparison between URT and MRT/CRT considering only RCT. (PDF 150 KB)
Appendices
Appendix 1
Newcastle–Ottawa checklists for observational comparative studies (cohorts)


Appendix 2
Risk of bias summary assessment for randomized clinical trials

Rights and permissions
About this article
Cite this article
Baccaglini, W., de Carvalho, I.T., Glina, F.P.A. et al. Radiotherapy-related toxicity for localized prostate cancer: meta-analysis comparing conventional or moderately hypofractionated vs. ultrahypofractionated protocols. Clin Transl Oncol 24, 1425–1439 (2022). https://doi.org/10.1007/s12094-022-02790-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12094-022-02790-2