Abstract
Purpose
To compare long-term outcomes in patients with adrenal incidentalomas (AIs) with the response to a 1 mg overnight dexamethasone suppression test (DST).
Methods
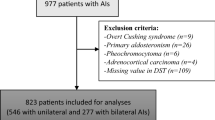
Consecutive patients with “non-functional” AIs (n = 365) were examined. Patients with overt hormone excess, adrenocortical cancer and known malignancy had been excluded. Patients were classified to normal cortisol secretion group (n = 204, DST ≤ 50 nmol/l), possible autonomous cortisol secretion group (n = 128, DST 51–138 nmol/l) and autonomous cortisol secretion group (n = 33, DST ≥ 138 nmol/l).
Results
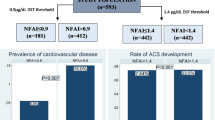
Thirty-seven patients (10.1%) deceased during the follow-up period (5.2 ± 2.3 years): 16(7.8%) in the non-secreting group (time from diagnosis to death: 3.9 ± 2.9 years), 15 in the possible autonomous cortisol secretion group (11.7%, 3.2 ± 1.8 years) and 6 in the autonomous cortisol secretion group (18.2%, 2.3 ± 1.5 years), respectively (P = 0.019). Multivariate analysis only found significant association with age and the tumour size but if cortisol levels post-DST were analysed as a continuous variable it was significant as well. All deaths in autonomous cortisol secretion group were due to cancer not related to adrenal glands. Hypertension, cardiovascular disease and medications were more common in the possible and autonomous cortisol secretion group, especially in the former. More bilateral AIs and larger AI size were found in the two latter groups.
Conclusions
Patients with autonomous cortisol secretion had higher mortality than those with non-functioning AIs though cortisol levels post-DST as a continuous variable, age and tumour size were better predictor of mortality. Cardiovascular disease and osteoporosis medication seemed more prevalent in the possible and autonomous cortisol secretion groups, especially in the former.


Similar content being viewed by others
References
G. Di Dalmazi, R. Pasquali, F. Beuschlein, M. Reincke, Subclinical hypercortisolism: a state, a syndrome, or a disease? Eur. J. Endocrinol. 173(4), 61–71 (2015)
N. I. H. Consensus and S. Statements, NIH state-of-the-science statement on management of the clinically inapparent adrenal mass (‘incidentaloma’). NIH Consens State Sci. Statements 19(2), 1–25 (2002)
M. Fassnacht, W. Arlt, I. Bancos, I. Dralle, Management of adrenal incidentalomas: European society of endocrinology clinical practice guideline in collaboration with the European network for the study of adrenal tumors. Eur. J. Endocrinol. 175(2), 1–34 (2016)
M. Terzolo, G. Osella, A. Alì, G. Borretta, F. Cesario, P. Paccotti, Subclinical Cushing’s syndrome in adrenal incidentaloma. Clin. Endocrinol. 48(1), 89–97 (1998)
M. Zeiger, G.B. Thompson, Q.-Y. Duh, A.H. Hamrahian, P. Angelos, D. Elaraj, E. Fishman, The American association of clinical endocrinologists and American association of endocrine surgeons medical guidelines for the management of adrenal incidentalomas. Endocr. Pract. 15(1), 1–20 (2009)
M. Debono, J. Newell-Price, Subclinical hypercortisolism in adrenal incidentaloma. Curr. Opin. Endocrinol. Diabetes. Obes. 22(3), 185–192 (2015)
M. Debono, M. Bradburn, M. Bull, B. Harrison, R.J. Ross, J. Newell-Price, Cortisol as a marker for increased mortality in patients with incidental adrenocortical adenomas. J. Clin. Endocrinol. Metab. 99(12), 4462–4470 (2014)
H. Falhammar, L. Frisen, A.L. Hirschberg, C. Norrby, C. Almqvist, A. Nordenskjold, A. Nordenstrom, Increased cardiovascular and metabolic morbidity in patients with 21-hydroxylase deficiency: a Swedish population-based national cohort study. J. Clin. Endocrinol. Metab. 100(9), 3520–3528 (2015)
J. Patrova, I. Jarocka, H. Wahrenberg, H. Falhammar, Clinical outcomes in adrenal incidentaloma: experience from one center. Endocr. Pract. 21(8), 870–877 (2015)
L. Barzon, M. Boscaro, Diagnosis and management of adrenal incidentalomas. J. Urol. 163(2), 398–407 (2000)
B. Bülow, S. Jansson, C. Juhlin, L. Steen, M. Thorén, H. Wahrenberg, S. Valdemarsson, B. Wängberg, B. Ahrén, Adrenal incidentaloma-Follow up results from a Swedish prospective study. Eur. J. Endocrinol. 154(3), 419–423 (2006)
H. Yeomans, J. Calissendorff, C. Volpe, H. Falhammar, B. Mannheimer, Limited value of long-term biochemical follow-up in patients with adrenal incidentalomas-a retrospective cohort study. BMC Endocr. Disord. 15(6), 1–6 (2015)
L. Barzon, C. Scaroni, N. Sonino, F. Fallo, Risk factors and long-term follow-up of adrenal incidentalomas. J. Clin. Endocrinol. Metab. 84(2), 520–526 (1999)
L. Barzon, F. Fallo, N. Sonino, M. Boscaro, Development of overt Cushing’s syndrome in patients with adrenal incidentaloma. Eur. J. Endocrinol. 146, 61–66 (2002)
R. Libè, C. Dall’Asta, L. Barbetta, A. Baccarelli, P. Beck-Peccoz, B. Ambrosi, Long-term follow-up study of patients with adrenal incidentalomas. Eur. J. Endocrinol. 147(4), 489–494 (2002)
G. Di Dalmazi, V. Vicennati, S. Garelli, E. Casadio, E. Rinaldi, E. Giampalma, C. Mosconi, R. Golfieri, A. Paccapelo, U. Pagotto, R. Pasquali, Cardiovascular events and mortality in patients with adrenal incidentalomas that are either non-secreting or associated with intermediate phenotype or subclinical Cushing’s syndrome: a 15-year retrospective study. Lancet Diabetes Endocrinol. 2(5), 396–405 (2014)
H.C. Abercrombie, J. Giese-Davis, S. Sephton, E.S. Epel, J.M. Turner-Cobb, M. Spiegel, Flattened cortisol rhythms in metastatic breast cancer patients. Psychoneuroendocrinology 29(8), 1082–1092 (2004)
S.E. Sephton, F.S. Dhabhar, A.S. Keuroghlian, J. Giese-Davis, B.S. McEwen, A.C. Ionan, D. Spiegel, Depression, cortisol, and suppressed cell-mediated immunity in metastatic breast cancer. Brain Behav. Immun. 23(8), 1148–1155 (2009)
E. Filipski, V.M. King, X. Li, T.G. Granda, M.-C. Mormont, X. Liu, B. Claustrat, M.H. Hastings, F. Lévi, Host circadian clock as a control point in tumor progression. J. Natl Cancer Inst. 94(9), 690–697 (2002)
R.M. Sapolsky, T.M. Donnelly, Vulnerability to Stress-Induced Tumor Growth Increases with Age in Rats: role of glucocorticoids. Endocrinology 117(2), 662–666 (1985)
T.J. Moran, S. Gray, C.A. Mikosz, S.D. Conzen, The glucocorticoid receptor mediates a survival signal in human mammary epithelial cells. Cancer Res. 60(4), 867–872 (2000)
T.M. Rae, S.H. Hillier, Steroid signalling in the ovarian surface epithelium. Trends Endocrinol. Metab. 16(7), 327–333 (2005)
G. Di Dalmazi, V. Vicennati, E. Rinaldi, A.M. Morselli-Labate, E. Giampalma, C. Mosconi, U. Pagotto, R. Pasquali, Progressively increased patterns of subclinical cortisol hypersecretion in adrenal incidentalomas differently predict major metabolic and cardiovascular outcomes: a large cross-sectional study. Eur. J. Endocrinol. 166(4), 669–677 (2012)
R. Rossi, L. Tauchmanova, A. Luciano, M.D.I. Martino, C. Battista, O. Molecolare, Subclinical cushing’s syndrome in patients with adrenal incidentaloma: clinical and biochemical features. J. Clin. Endocrinol. Metabol. 85(4), 1440–1448 (2000)
G. Di Dalmazi, Update on the risks of benign adrenocortical incidentalomas. Curr. Opin. Endocrinol. Diabetes Obes. 193–199, (2017)
D. Lopez, M.A. Luque-Fernandez, A. Steele, G.K. Adler, A. Turchin, A. Vaidya, ‘Nonfunctional’ adrenal tumors and the risk for incident diabetes and cardiovascular outcomes. Ann. Intern. Med. 165(8), 533–542 (2016)
H. Olsen, E. Nordenström, A. Bergenfelz, U. Nyman, S. Valdemarsson, E. Palmqvist, Subclinical hypercortisolism and CT appearance in adrenal incidentalomas: a multicenter study from Southern Sweden. Endocrine 42(1), 164–172 (2012)
A.S. Mihailidou, T.Y.L. Le, M. Mardini, Y.W. Funder, Glucocorticoids activate cardiac mineralocorticoid receptors during experimental myocardial infarction. Hypertension 54(6), 1306–1312 (2009)
M. De Leo, R. Pivonello, R.S. Auriemma, A. Cozzolino, P. Vitale, C. Simeoli, M.C. De Martino, G. Lombardi, A. Colao, Cardiovascular disease in Cushing’s syndrome: heart versus vasculature. Neuroendocrinology 92(1), 50–54 (2010)
A. Toniato, I. Merante-Boschin, G. Opocher, M.R. Pelizzo, F. Schiavi, E. Ballotta, Surgical versus conservative management for subclinical Cushing syndrome in adrenal incidentalomas: a prospective randomized study. Ann. Surg. 249(3), 388–391 (2009)
I.I. Androulakis, G.A. Kaltsas, G.E. Kollias, A.C. Markou, A.K. Gouli, D.A. Thomas, K.I. Alexandraki, C.M. Papamichael, D.J. Hadjidakis, G.P. Piaditis, Patients with apparently nonfunctioning adrenal incidentalomas may be at increased cardiovascular risk due to excessive cortisol secretion. J. Clin. Endocrinol. Metab. 99(8), 2754–2762 (2014)
Acknowledgements
We want to thank Dr Sandawana William Majoni, Biomedical Statistician, for his advice on the statistical analysis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Patrova, J., Kjellman, M., Wahrenberg, H. et al. Increased mortality in patients with adrenal incidentalomas and autonomous cortisol secretion: a 13-year retrospective study from one center. Endocrine 58, 267–275 (2017). https://doi.org/10.1007/s12020-017-1400-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-017-1400-8