Abstract
The intricate nature of the human brain and the limitations of existing model systems to study molecular and cellular causes of neuropsychiatric disorders represent a major challenge for basic research. The promising progress in patient-derived stem cell technology and in our knowledge on the role of the brain oxytocin (OXT) system in health and disease offer new possibilities in that direction. In this study, the rat hair follicle stem cells (HFSCs) were isolated and expanded in vitro. The expression of oxytocin receptors (OXTR) was evaluated in these cells. The cellular viability was assessed 12 h post stimulation with OXT. The activation of OXTR-coupled intracellular signaling cascades, following OXT treatment was determined. Also, the influence of OXT on neurite outgrowth and cytoskeletal rearrangement were defined. The assessment of OXTR protein expression revealed this receptor is expressed abundantly in HFSCs. As evidenced by the cell viability assay, no adverse or cytotoxic effects were detected following 12 h treatment with different concentrations of OXT. Moreover, OXTR stimulation by OXT resulted in ERK1/2, CREB, and eEF2 activation, neurite length alterations, and cytoskeletal rearrangements that reveal the functionality of this receptor in HFSCs. Here, we introduced the rat HFSCs as an easy-to-obtain stem cell model that express functional OXTR. This cell-based model can contribute to our understanding of the progression and treatment of neuropsychiatric disorders with oxytocinergic system deficiency.
Graphical Abstract








Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- ASD :
-
Autism spectrum disorder
- GAD :
-
Generalized anxiety disorder
- iPSCs :
-
Induced pluripotent stem cells
- HFSCs :
-
Hair follicle-derived stem cells
- OXTR :
-
Oxytocin receptor
- OXT :
-
Oxytocin
- SNP :
-
Single nucleotide polymorphisms
- eEF2a :
-
Eukaryotic elongation factor 2a
References
Nestler, E. J., & Hyman, S. E. (2010). Animal models of neuropsychiatric disorders. Nature Neuroscience, 13(10), 1161.
Lago, S. G., Tomasik, J., & Bahn, S. (2021). Functional patient-derived cellular models for neuropsychiatric drug discovery. Translational Psychiatry, 11(1), 1–11.
Haggarty, S. J., Silva, M. C., Cross, A., Brandon, N. J., & Perlis, R. H. (2016). Advancing drug discovery for neuropsychiatric disorders using patient-specific stem cell models. Molecular and Cellular Neuroscience, 73, 104–115.
Paşca, S. P., Panagiotakos, G., & Dolmetsch, R. E. (2014). Generating human neurons in vitro and using them to understand neuropsychiatric disease. Annual Review of Neuroscience, 37, 479–501.
Adegbola, A., Bury, L. A., Fu, C., Zhang, M., & Wynshaw-Boris, A. (2017). Concise review: Induced pluripotent stem cell models for neuropsychiatric diseases. Stem Cells Translational Medicine, 6(12), 2062–2070.
Haggarty, S. J., & Perlis, R. H. (2014). Translation: Screening for novel therapeutics with disease-relevant cell types derived from human stem cell models. Biological Psychiatry, 75(12), 952–960.
Wang, M., Zhang, L., & Gage, F. H. (2020). Modeling neuropsychiatric disorders using human induced pluripotent stem cells. Protein & Cell, 11(1), 45–59.
Hoffman, G. E., Schrode, N., Flaherty, E., & Brennand, K. J. (2019). New considerations for hiPSC-based models of neuropsychiatric disorders. Molecular Psychiatry, 24(1), 49–66.
Kampmann, M. (2020). CRISPR-based functional genomics for neurological disease. Nature Reviews Neurology, 16(9), 465–480.
Soliman, M., Aboharb, F., Zeltner, N., & Studer, L. (2017). Pluripotent stem cells in neuropsychiatric disorders. Molecular Psychiatry, 22(9), 1241–1249.
Vierbuchen, T., Ostermeier, A., Pang, Z. P., Kokubu, Y., Südhof, T. C., & Wernig, M. (2010). Direct conversion of fibroblasts to functional neurons by defined factors. Nature, 463(7284), 1035–1041.
Yang, N., Ng, Y. H., Pang, Z. P., Südhof, T. C., & Wernig, M. (2011). Induced neuronal cells: How to make and define a neuron. Cell Stem Cell, 9(6), 517–525.
Pandamooz, S., Naji, M., Alinezhad, F., Zarghami, A., & Pourghasem, M. (2013). The influence of cerebrospinal fluid on epidermal neural crest stem cells may pave the path for cell-based therapy. Stem Cell Research & Therapy, 4(4), 1–9.
Pandamooz, S., Salehi, M. S., Zibaii, M. I., Ahmadiani, A., Nabiuni, M., & Dargahi, L. (2018). Epidermal neural crest stem cell-derived glia enhance neurotrophic elements in an ex vivo model of spinal cord injury. Journal of Cellular Biochemistry, 119(4), 3486–3496.
Pandamooz, S., Jafari, A., Salehi, M. S., Jurek, B., Ahmadiani, A., Safari, A., et al. (2020). Substrate stiffness affects the morphology and gene expression of epidermal neural crest stem cells in a short term culture. Biotechnology and Bioengineering, 117(2), 305–317.
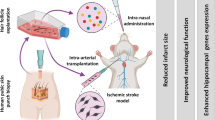
Salehi, M. S., Pandamooz, S., Safari, A., Jurek, B., Tamadon, A., Namavar, M. R., et al. (2020). Epidermal neural crest stem cell transplantation as a promising therapeutic strategy for ischemic stroke. CNS Neuroscience & Therapeutics, 26(7), 670–681.
Karimi-Haghighi, S., Pandamooz, S., Jurek, B., Fattahi, S., Safari, A., Azarpira, N., et al. (2023). From hair to the brain: The short-term therapeutic potential of human hair follicle-derived stem cells and their conditioned medium in a rat model of stroke. Molecular Neurobiology, 60, 2587–2601.
Mousavi, S. M., Akbarpour, B., Karimi-Haghighi, S., Pandamooz, S., Belém-Filho, I. J. A., Masís-Calvo, M., et al. (2022). Therapeutic potential of hair follicle-derived stem cell intranasal transplantation in a rat model of ischemic stroke. BMC Neuroscience, 23, 47.
Hu, Y. F., Zhang, Z. J., & Sieber-Blum, M. (2006). An epidermal neural crest stem cell (EPI-NCSC) molecular signature. Stem Cells, 24(12), 2692–2702.
Jurek, B., & Meyer, M. (2020). Anxiolytic and anxiogenic? how the transcription factor MEF2 might explain the manifold behavioral effects of oxytocin. Frontiers in Endocrinology, 11, 186.
Grinevich, V., & Neumann, I. D. (2021). Brain oxytocin: How puzzle stones from animal studies translate into psychiatry. Molecular Psychiatry, 26(1), 265–279.
Neumann, I. D., & Landgraf, R. (2012). Balance of brain oxytocin and vasopressin: Implications for anxiety, depression, and social behaviors. Trends in Neurosciences, 35(11), 649–659.
Romano, A., Tempesta, B., Micioni Di Bonaventura, M. V., & Gaetani, S. J. F. I. N. (2016). From autism to eating disorders and more: the role of oxytocin in neuropsychiatric disorders. Frontiers in Neuroscience, 9, 497.
LoParo, D., & Waldman, I. J. M. P. (2015). The oxytocin receptor gene (OXTR) is associated with autism spectrum disorder: A meta-analysis. Molecular Psychiatry, 20(5), 640–646.
Baribeau, D. A., Dupuis, A., Paton, T. A., Scherer, S. W., Schachar, R. J., Arnold, P. D., et al. (2017). Oxytocin receptor polymorphisms are differentially associated with social abilities across neurodevelopmental disorders. Scientific Reports, 7(1), 1–11.
Kimura, R., Tomiwa, K., Inoue, R., Suzuki, S., Nakata, M., Awaya, T., et al. (2020). Dysregulation of the oxytocin receptor gene in Williams syndrome. Psychoneuroendocrinology, 115, 104631.
Ziegler, C., Dannlowski, U., Bräuer, D., Stevens, S., Laeger, I., Wittmann, H., et al. (2015). Oxytocin receptor gene methylation: Converging multilevel evidence for a role in social anxiety. Neuropsychopharmacology, 40(6), 1528–1538.
Uhrig, S., Hirth, N., Broccoli, L., von Wilmsdorff, M., Bauer, M., Sommer, C., et al. (2016). Reduced oxytocin receptor gene expression and binding sites in different brain regions in schizophrenia: A post-mortem study. Schizophrenia Research, 177(1–3), 59–66.
Gregory, S. G., Connelly, J. J., Towers, A. J., Johnson, J., Biscocho, D., Markunas, C. A., et al. (2009). Genomic and epigenetic evidence for oxytocin receptor deficiency in autism. BMC Medicine, 7(1), 1–13.
Lee, M. R., Sheskier, M., Farokhnia, M., Feng, N., Marenco, S., Lipska, B., et al. (2018). Oxytocin receptor mRNA expression in dorsolateral prefrontal cortex in major psychiatric disorders: A human post-mortem study. Psychoneuroendocrinology, 96, 143–147.
King, L. B., Walum, H., Inoue, K., Eyrich, N. W., & Young, L. J. J. B. P. (2016). Variation in the oxytocin receptor gene predicts brain region–specific expression and social attachment. Biological Psychiatry, 80(2), 160–169.
Danoff, J. S., Wroblewski, K. L., Graves, A. J., Quinn, G. C., Perkeybile, A. M., Kenkel, W. M., et al. (2021). Genetic, epigenetic, and environmental factors controlling oxytocin receptor gene expression. Clinical Epigenetics, 13(1), 1–16.
Takayanagi, Y., Yoshida, M., Bielsky, I. F., Ross, H. E., Kawamata, M., Onaka, T., et al. (2005). Pervasive social deficits, but normal parturition, in oxytocin receptor-deficient mice. Proceedings of the National Academy of Sciences of the United States of America, 102(44), 16096–16101.
Wei, J., Ma, L., Ju, P., Yang, B., Wang, Y.-X., & Chen, J. (2020). Involvement of oxytocin receptor/Erk/MAPK signaling in the mPFC in early life stress-induced autistic-like behaviors. Frontiers in Cell and Developmental Biology, 8, 564485.
Horiai, M., Otsuka, A., Hidema, S., Hiraoka, Y., Hayashi, R., Miyazaki, S., et al. (2020). Targeting oxytocin receptor (Oxtr)-expressing neurons in the lateral septum to restore social novelty in autism spectrum disorder mouse models. Scientific Reports, 10(1), 1–13.
Tomizawa, K., Iga, N., Lu, Y.-F., Moriwaki, A., Matsushita, M., Li, S.-T., et al. (2003). Oxytocin improves long-lasting spatial memory during motherhood through MAP kinase cascade. Nature Neuroscience, 6(4), 384–390.
Jurek, B., Slattery, D. A., Maloumby, R., Hillerer, K., Koszinowski, S., Neumann, I. D., et al. (2012). Differential contribution of hypothalamic MAPK activity to anxiety-like behaviour in virgin and lactating rats. PLoS ONE, 7(5), e37060.
Jurek, B., Slattery, D. A., Hiraoka, Y., Liu, Y., Nishimori, K., Aguilera, G., et al. (2015). Oxytocin regulates stress-induced Crf gene transcription through CREB-regulated transcription coactivator 3. Journal of Neuroscience, 35(35), 12248–12260.
Martinetz, S., Meinung, C.-P., Jurek, B., von Schack, D., van den Burg, E. H., Slattery, D. A., et al. (2019). De novo protein synthesis mediated by the eukaryotic elongation factor 2 is required for the anxiolytic effect of oxytocin. Biological Psychiatry, 85(10), 802–811.
Flavell, S. W., Cowan, C. W., Kim, T.-K., Greer, P. L., Lin, Y., Paradis, S., et al. (2006). Activity-dependent regulation of MEF2 transcription factors suppresses excitatory synapse number. Science, 311(5763), 1008–1012.
Schildge, S., Bohrer, C., Beck, K., Schachtrup, C. (2013). Isolation and culture of mouse cortical astrocytes. Journal of visualized experiments, 71, 50079.
Pandamooz, S., Jurek, B., Dianatpour, M., Haerteis, S., Limm, K., Oefner, P. J., et al. (2023). The beneficial effects of chick embryo extract preconditioning on hair follicle stem cells: A promising strategy to generate Schwann cells. Cell Proliferation, 56(7), e13397.
Bustin, S. A., Benes, V., Garson, J. A., Hellemans, J., Huggett, J., Kubista, M., et al. (2009). The MIQE guidelines: Minimum information for publication of quantitative real-time PCR experiments. Clinical Chemistry, 55(4), 611–622.
Di Benedetto, A., Sun, L., Zambonin, C. G., Tamma, R., Nico, B., Calvano, C. D., et al. (2014). Osteoblast regulation via ligand-activated nuclear trafficking of the oxytocin receptor. Proceedings of the National Academy of Sciences, 111(46), 16502–16507.
Conti, F., Sertic, S., Reversi, A., & Chini, B. (2009). Intracellular trafficking of the human oxytocin receptor: Evidence of receptor recycling via a Rab4/Rab5 “short cycle.” American Journal of Physiology-Endocrinology and Metabolism, 296(3), E532–E542.
Meyer, M., Jurek, B., Alfonso-Prieto, M., Ribeiro, R., Milenkovic, V. M., Winter, J., et al. (2022). Structure-function relationships of the disease-linked A218T oxytocin receptor variant. Molecular Psychiatry, 27(2), 907–917.
Jurek, B., & Neumann, I. D. (2018). The oxytocin receptor: From intracellular signaling to behavior. Physiological Reviews, 98(3), 1805–1908.
Tojkander, S., Ciuba, K., & Lappalainen, P. (2018). CaMKK2 regulates mechanosensitive assembly of contractile actin stress fibers. Cell Reports, 24(1), 11–19.
Winter, J., & Jurek, B. (2019). The interplay between oxytocin and the CRF system: Regulation of the stress response. Cell and Tissue Research, 375(1), 85–91.
Winter, J., Meyer, M., Berger, I., Royer, M., Bianchi, M., Kuffner, K., et al. (2021). Chronic oxytocin-driven alternative splicing of Crfr2α induces anxiety. Molecular Psychiatry. https://doi.org/10.1038/s41380-021-01141-x
Greenwood, M. A., & Hammock, E. A. (2017). Oxytocin receptor binding sites in the periphery of the neonatal mouse. PLoS ONE, 12(2), e0172904.
Greenwood, M. A., & Hammock, E. A. (2019). Oxytocin receptor binding sites in the periphery of the neonatal prairie vole. Frontiers in Neuroscience, 13, 474.
Wahis, J., Baudon, A., Althammer, F., Kerspern, D., Goyon, S., Hagiwara, D., et al. (2021). Astrocytes mediate the effect of oxytocin in the central amygdala on neuronal activity and affective states in rodents. Nature Neuroscience, 24(4), 529–541.
Van Den Burg, E. H., Stindl, J., Grund, T., Neumann, I. D., & Strauss, O. (2015). Oxytocin stimulates extracellular Ca2+ influx through TRPV2 channels in hypothalamic neurons to exert its anxiolytic effects. Neuropsychopharmacology, 40(13), 2938–2947.
Amoh, Y., Li, L., Katsuoka, K., Penman, S., & Hoffman, R. M. (2005). Multipotent nestin-positive, keratin-negative hair-follicle bulge stem cells can form neurons. Proceedings of the National Academy of Sciences of the United States of America, 102(15), 5530–5534.
Narytnyk, A., Verdon, B., Loughney, A., Sweeney, M., Clewes, O., Taggart, M. J., et al. (2014). Differentiation of human epidermal neural crest stem cells (hEPI-NCSC) into virtually homogenous populations of dopaminergic neurons. Stem Cell Reviews and Reports, 10(2), 316–326.
Yamane, M., Takaoka, N., Obara, K., Shirai, K., Aki, R., Hamada, Y., et al. (2021). Hair-follicle-associated pluripotent (HAP) stem cells can extensively differentiate to tyrosine-hydroxylase-expressing dopamine-secreting neurons. Cells, 10(4), 864.
Lin, H., Liu, F., Zhang, C., Zhang, Z., Guo, J., Ren, C., et al. (2009). Pluripotent hair follicle neural crest stem-cell-derived neurons and schwann cells functionally repair sciatic nerves in rats. Molecular Neurobiology, 40(3), 216–223.
Sakaue, M., & Sieber-Blum, M. (2015). Human epidermal neural crest stem cells as a source of Schwann cells. Development, 142(18), 3188–3197.
Pournajaf, S., Valian, N., Shalmani, L. M., Khodabakhsh, P., Jorjani, M., & Dargahi, L. (2020). Fingolimod increases oligodendrocytes markers expression in epidermal neural crest stem cells. European Journal of Pharmacology, 885, 173502.
Khodabakhsh, P., Pournajaf, S., Mohaghegh Shalmani, L., Ahmadiani, A., & Dargahi, L. (2021). Insulin promotes Schwann-like cell differentiation of rat epidermal neural crest stem cells. Molecular Neurobiology, 58(10), 5327–5337.
Hu, Y. F., Gourab, K., Wells, C., Clewes, O., Schmit, B. D., & Sieber-Blum, M. (2010). Epidermal neural crest stem cell (EPI-NCSC)—mediated recovery of sensory function in a mouse model of spinal cord injury. Stem Cell Reviews and Reports, 6(2), 186–198.
Obara, K., Shirai, K., Hamada, Y., Arakawa, N., Yamane, M., Takaoka, N., et al. (2022). Chronic spinal cord injury functionally repaired by direct implantation of encapsulated hair-follicle-associated pluripotent (HAP) stem cells in a mouse model: Potential for clinical regenerative medicine. PLoS ONE, 17(1), e0262755.
Li, Y., Yao, D., Zhang, J., Liu, B., Zhang, L., Feng, H., et al. (2017). The effects of epidermal neural crest stem cells on local inflammation microenvironment in the defected sciatic nerve of rats. Frontiers in Molecular Neuroscience, 10, 133.
Zhang, L., Li, B., Liu, B., & Dong, Z. (2019). Co-transplantation of epidermal neural crest stem cells and olfactory ensheathing cells repairs sciatic nerve defects in rats. Frontiers in Cellular Neuroscience, 13, 253.
Mousavi, S. M., Akbarpour, B., Karimi-Haghighi, S., Pandamooz, S., Belém-Filho, I. J. A., Masís-Calvo, M., et al. (2022). Therapeutic potential of hair follicle-derived stem cell intranasal transplantation in a rat model of ischemic stroke. BMC Neuroscience, 23(1), 1–14.
Zhang, X., Tang, H., Mao, S., Li, B., Zhou, Y., Yue, H., et al. (2020). Transplanted hair follicle stem cells migrate to the penumbra and express neural markers in a rat model of cerebral ischaemia/reperfusion. Stem Cell Research & Therapy, 11(1), 1–12.
Akbari, S., Hooshmandi, E., Bayat, M., Haghighi, A. B., Salehi, M. S., Pandamooz, S., et al. (2022). The neuroprotective properties and therapeutic potential of epidermal neural crest stem cells transplantation in a rat model of vascular dementia. Brain Research, 1776, 147750.
Quadrato, G., Brown, J., & Arlotta, P. (2016). The promises and challenges of human brain organoids as models of neuropsychiatric disease. Nature Medicine, 22(11), 1220–1228.
Salehi, M. S., Neumann, I. D., Jurek, B., & Pandamooz, S. (2021) Co-stimulation of oxytocin and arginine-vasopressin receptors affect hypothalamic neurospheroid size. International Journal of Molecular Sciences, 22(16), 8464.
Lestanova, Z., Bacova, Z., Kiss, A., Havranek, T., Strbak, V., & Bakos, J. (2016). Oxytocin increases neurite length and expression of cytoskeletal proteins associated with neuronal growth. Journal of Molecular Neuroscience, 59(2), 184–192.
Lestanova, Z., Puerta, F., Alanazi, M., Bacova, Z., Kiss, A., Castejon, A., et al. (2017). Downregulation of oxytocin receptor decreases the length of projections stimulated by retinoic acid in the U-87MG cells. Neurochemical Research, 42(4), 1006–1014.
Zatkova, M., Reichova, A., Bacova, Z., Strbak, V., Kiss, A., & Bakos, J. (2018). Neurite outgrowth stimulated by oxytocin is modulated by inhibition of the calcium voltage-gated channels. Cellular and Molecular Neurobiology, 38(1), 371–378.
Zatkova, M., Bacova, Z., Puerta, F., Lestanova, Z., Alanazi, M., Kiss, A., et al. (2018). Projection length stimulated by oxytocin is modulated by the inhibition of calcium signaling in U-87MG cells. Journal of Neural Transmission, 125(12), 1847–1856.
Meyer, M., Berger, I., Winter, J., & Jurek, B. (2018). Oxytocin alters the morphology of hypothalamic neurons via the transcription factor myocyte enhancer factor 2A (MEF-2A). Molecular and Cellular Endocrinology, 477, 156–162.
Meyer, M., Kuffner, K., Winter, J., Neumann, I. D., Wetzel, C. H., & Jurek, B. (2020). Myocyte enhancer factor 2A (MEF2A) defines oxytocin-induced morphological effects and regulates mitochondrial function in neurons. International Journal of Molecular Sciences, 21(6), 2200.
Bakos, J., Strbak, V., Paulikova, H., Krajnakova, L., Lestanova, Z., & Bacova, Z. (2013). Oxytocin receptor ligands induce changes in cytoskeleton in neuroblastoma cells. Journal of Molecular Neuroscience, 50(3), 462–468.
Gimpl, G., & Fahrenholz, F. (2001). The oxytocin receptor system: Structure, function, and regulation. Physiological Reviews, 81(2), 629–683.
Wang, Y.-F., & Hatton, G. I. (2007). Interaction of extracellular signal-regulated protein kinase 1/2 with actin cytoskeleton in supraoptic oxytocin neurons and astrocytes: Role in burst firing. Journal of Neuroscience, 27(50), 13822–13834.
Parker, K. J., Oztan, O., Libove, R. A., Sumiyoshi, R. D., Jackson, L. P., Karhson, D. S., et al. (2017). Intranasal oxytocin treatment for social deficits and biomarkers of response in children with autism. Proceedings of the National Academy of Sciences of the United States of America, 114(30), 8119–8124.
Griesi-Oliveira, K., Suzuki, A. M., Alves, A. Y., Mafra, A. C. C. N., Yamamoto, G. L., Ezquina, S., et al. (2018). Actin cytoskeleton dynamics in stem cells from autistic individuals. Scientific Reports, 8(1), 1–10.
Unterholzner, J., Millischer, V., Wotawa, C., Sawa, A., & Lanzenberger, R. (2021). Making sense of patient-derived iPSCs, transdifferentiated neurons, olfactory neuronal cells, and cerebral organoids as models for psychiatric disorders. International Journal of Neuropsychopharmacology, 24(10), 759–775.
Masuda, K., Han, X., Kato, H., Sato, H., Zhang, Y., Sun, X., et al. (2021). Dental pulp-derived mesenchymal stem cells for modeling genetic disorders. International Journal of Molecular Sciences, 22(5), 2269.
Borgmann-Winter, K., Willard, S., Sinclair, D., Mirza, N., Turetsky, B., Berretta, S., et al. (2015). Translational potential of olfactory mucosa for the study of neuropsychiatric illness. Translational Psychiatry, 5(3), e527–e527.
Funding
This study was financially supported by Deutsche Forschungsgemeinschaft (IDN: Ne465/27–1, Ne465/31–1 BJ: JU3039-1), the DFG-GRK 2174 and Iran National Science Foundation (INSF, grant No: 99013300) and Shiraz University of Medical Sciences (Grant No: 27044). Partial support was also provided by International Brain Research Organization (IBRO) Research Fellowship award received by the Mohammad Saied Salehi. The funding body played no role in the design of the study and collection, analysis, and interpretation of data and in writing the manuscript.
Author information
Authors and Affiliations
Contributions
SP, MSS and CPM conceptualized the study, performed experiments, analysed the data, and prepared the manuscript draft. BJ, NA and MD involved in manuscript writing, study design, and reviewed and edited the manuscript. IDN substantially reviewed and edited the manuscript and supervised the study and the manuscript.
Corresponding authors
Ethics declarations
Ethics Approval and Consent to Participate
This project entitled “Evaluation of oxytocin effect on hair follicle-derived stem cells” was approved by the Animal Care Committee of Shiraz University of Medical Sciences, Shiraz, Iran (Approval number: IR.SUMS.AEC.1401.111). All eight rats used in this study were euthanized under CO2 inhalation in accordance with Guide for the Care and Use of Laboratory Animals by the National Institutes of Health, Bethesda, MD, USA, and approved by the government of the Oberpfalz, Germany. Hair follicles and cortical tissues were immediately obtained from euthanized animals. No experiment was performed on animals. The study is reported in accordance with ARRIVE guidelines.
Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pandamooz, S., Salehi, M.S., Jurek, B. et al. Oxytocin Receptor Expression in Hair Follicle Stem Cells: A Promising Model for Biological and Therapeutic Discovery in Neuropsychiatric Disorders. Stem Cell Rev and Rep 19, 2510–2524 (2023). https://doi.org/10.1007/s12015-023-10603-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12015-023-10603-4