Abstract
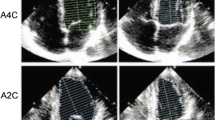
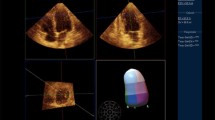
Assessing left ventricular diastolic and regional function is a crucial part of the cardiovascular evaluation. Diastolic function is as important as systolic function for left ventricular performance because it is the determinant of the ability of the left atrium and ventricle to fill at relatively low pressures. Additionally, diastolic function plays an important role in the management and prognosis of patients with symptoms and signs of heart failure. Technical advances in the imaging modalities have allowed a comprehensive noninvasive assessment of global and regional cardiac mechanics and precise estimation of cardiovascular hemodynamics. In this review, we will discuss and compare clinically available techniques and novel approaches using echocardiography, cardiac magnetic resonance, and computed tomography for the assessment of diastolic and regional left ventricular function.








Similar content being viewed by others
Abbreviations
- ASE:
-
American Society of Echocardiography
- CMR:
-
Cardiac magnetic resonance imaging
- CW:
-
Continuous-wave
- D:
-
Pulmonary venous diastolic flow wave
- DENSE:
-
Displacement encoding with stimulated echoes
- DSCT:
-
Dual source computed tomography
- DT:
-
Deceleration time
- E:
-
Early transmitral flow velocity
- e′:
-
Early diastolic velocity of the mitral annulus
- EACVI:
-
European Association of Cardiovascular Imaging
- Echo:
-
Echocardiography
- ECV:
-
Extracellular volume
- EF:
-
Ejection fraction
- FT-MRI:
-
Feature-tracking magnetic resonance imaging
- HFpEF:
-
Heart failure with preserved ejection fraction
- HFrEF:
-
Heart failure with reduced ejection fraction
- IVRT:
-
Isovolumetric relaxation time
- LA:
-
Left atrial
- LV:
-
Left ventricular
- LVEDP:
-
Left ventricular end-diastolic pressure
- MDCT:
-
Multidetector computed tomography
- PW:
-
Pulsed-wave
- S:
-
Pulmonary venous systolic flow wave
- SENC:
-
Strain-encoded imaging
- SPAMM:
-
Spatial modulation of magnetization
- SRE :
-
Strain rate during early diastole
- SRIVR :
-
Strain rate during isovolumetric relaxation
- SSFP:
-
Balanced steady-state free precession
- SQUEEZ:
-
Stretch Quantifier of Endocardial Engraved Zones
- TDI:
-
Tissue Doppler imaging
- TPM:
-
Tissue phase mapping
- Vp:
-
M-mode flow propagation velocity
- β:
-
Load-independent passive LV stiffness constant
- τ:
-
Tau or time constant of left ventricular pressure decay
- 2D:
-
2-Dimensional
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Zile MR, Brutsaert DL. New concepts in diastolic dysfunction and diastolic heart failure: Part I: diagnosis, prognosis, and measurements of diastolic function. Circulation. 2002;105(11):1387–93.
Yamada H, Klein AL. Diastology 2010: clinical approach to diastolic heart failure. J Echocardiogr. 2010;8(3):65–79.
Yancy CW et al. 2013 ACCF/AHA guideline for the management of heart failure: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol. 2013;62(16):e147–239.
Gardin JM et al. Relationship of Doppler-echocardiographic left ventricular diastolic function to exercise performance in systolic heart failure: the HF-ACTION study. Am Heart J. 2009;158(4 Suppl):S45–52.
Cavalcante JL et al. Diastolic function improvement is associated with favourable outcomes in patients with acute non-ischaemic cardiomyopathy: insights from the multicentre IMAC-2 trial. Eur Heart J Cardiovasc Imaging. 2016;17(9):1027–35.
•• Nagueh SF et al. Recommendations for the evaluation of left ventricular diastolic function by echocardiography: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J Am Soc Echocardiogr. 2016;29(4):277–314. This document provides a comprehensive practical approach for the assessment of LV diastolic function utlitizing Echo.
• Flachskampf FA et al. Cardiac imaging to evaluate left ventricular diastolic function. J Am Coll Cardiol Img. 2015;8(9):1071–93. This study provides a thorough review about the current and experimental multimodality immaging parameters for the assessment of the LV diastolic function.
• Mor-Avi V et al. Current and evolving echocardiographic techniques for the quantitative evaluation of cardiac mechanics: ASE/EAE consensus statement on methodology and indications endorsed by the Japanese Society of Echocardiography. J Am Soc Echocardiogr. 2011;24(3):277–313. This document provides a detailed information about the echocardiographic techniques utilized for the assessment of cardiac mechanics and the clinical applications of these techniques.
Kinno M, et al. Comparison of echocardiography, cardiac magnetic resonance, and computed tomographic imaging for the evaluation of left ventricular myocardial function: part 1 (global assessment). Curr Cardiol Rep. 2016.
Thomas JD, Popovic ZB. Assessment of left ventricular function by cardiac ultrasound. J Am Coll Cardiol. 2006;48(10):2012–25.
Lang RM, et al. ASE’s Comprehensive echocardiography. 2nd ed. Philadelphia, PA: Elsevier Saunders. 879; 2016. p. 19103–2899
Opdahl A et al. Determinants of left ventricular early-diastolic lengthening velocity: independent contributions from left ventricular relaxation, restoring forces, and lengthening load. Circulation. 2009;119(19):2578–86.
Wang J et al. Global diastolic strain rate for the assessment of left ventricular relaxation and filling pressures. Circulation. 2007;115(11):1376–83.
Dokainish H et al. Usefulness of new diastolic strain and strain rate indexes for the estimation of left ventricular filling pressure. Am J Cardiol. 2008;101(10):1504–9.
Adhyapak SM, Parachuri VR. Architecture of the left ventricle: insights for optimal surgical ventricular restoration. Heart Fail Rev. 2010;15(1):73–83.
Sengupta PP et al. Twist mechanics of the left ventricle: principles and application. J Am Coll Cardiol Img. 2008;1(3):366–76.
Takeuchi M et al. Age-related changes in left ventricular twist assessed by two-dimensional speckle-tracking imaging. J Am Soc Echocardiogr. 2006;19(9):1077–84.
Wang J et al. Left ventricular untwisting rate by speckle tracking echocardiography. Circulation. 2007;116(22):2580–6.
Park SJ et al. Left ventricular torsion by two-dimensional speckle tracking echocardiography in patients with diastolic dysfunction and normal ejection fraction. J Am Soc Echocardiogr. 2008;21(10):1129–37.
Notomi Y et al. Ventricular untwisting: a temporal link between left ventricular relaxation and suction. Am J Physiol Heart Circ Physiol. 2008;294(1):H505–13.
Brun P et al. Left ventricular flow propagation during early filling is related to wall relaxation: a color M-mode Doppler analysis. J Am Coll Cardiol. 1992;20(2):420–32.
Hsu PC et al. The ratio of early mitral inflow velocity to global diastolic strain rate as a useful predictor of cardiac outcomes in patients with atrial fibrillation. J Am Soc Echocardiogr. 2014;27(7):717–25.
Ersboll M et al. Early diastolic strain rate in relation to systolic and diastolic function and prognosis in acute myocardial infarction: a two-dimensional speckle-tracking study. Eur Heart J. 2014;35(10):648–56.
Wakami K et al. Correlation between left ventricular end-diastolic pressure and peak left atrial wall strain during left ventricular systole. J Am Soc Echocardiogr. 2009;22(7):847–51.
Kurt M et al. Left atrial function in diastolic heart failure. Circ Cardiovasc Imaging. 2009;2(1):10–5.
Hartiala JJ et al. Velocity-encoded cine MRI in the evaluation of left ventricular diastolic function: measurement of mitral valve and pulmonary vein flow velocities and flow volume across the mitral valve. Am Heart J. 1993;125(4):1054–66.
Paelinck BP et al. Feasibility of tissue magnetic resonance imaging: a pilot study in comparison with tissue Doppler imaging and invasive measurement. J Am Coll Cardiol. 2005;45(7):1109–16.
Ambale-Venkatesh B et al. Diastolic function assessed from tagged MRI predicts heart failure and atrial fibrillation over an 8-year follow-up period: the multi-ethnic study of atherosclerosis. Eur Heart J Cardiovasc Imaging. 2014;15(4):442–9.
Ellims AH et al. Diffuse myocardial fibrosis evaluated by post-contrast t1 mapping correlates with left ventricular stiffness. J Am Coll Cardiol. 2014;63(11):1112–8.
• Rommel KP et al. Extracellular volume fraction for characterization of patients with heart failure and preserved ejection fraction. J Am Coll Cardiol. 2016;67(15):1815–25. This study provides evidence that CMR-derived T1 mapping, a technique to quantify diffuse myocardial fibrosis, can independently predict invasively measured LV stiffness in patients with HFpEF.
Su MY et al. CMR-verified diffuse myocardial fibrosis is associated with diastolic dysfunction in HFpEF. J Am Coll Cardiol Img. 2014;7(10):991–7.
Collins JD. Global and regional functional assessment of ischemic heart disease with cardiac MR imaging. Radiol Clin N Am. 2015;53(2):369–95.
•• Lang RM et al. Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J Am Soc Echocardiogr. 2015;28(1):1–39.e14. This document provide a comprehensive guidelines for the echocardiographic chamber quantification as recommended by the ASE/EACVI.
Cerqueira MD et al. Standardized myocardial segmentation and nomenclature for tomographic imaging of the heart. A statement for healthcare professionals from the Cardiac Imaging Committee of the Council on Clinical Cardiology of the American Heart Association. Circulation. 2002;105(4):539–42.
Raff GL et al. SCCT guidelines for the interpretation and reporting of coronary computed tomographic angiography. J Cardiovasc Comput Tomogr. 2009;3(2):122–36.
Hundley WG et al. Society for cardiovascular magnetic resonance guidelines for reporting cardiovascular magnetic resonance examinations. J Cardiovasc Magn Reson. 2009;11:5.
Heimdal A et al. Real-time strain rate imaging of the left ventricle by ultrasound. J Am Soc Echocardiogr. 1998;11(11):1013–9.
Leitman M et al. Two-dimensional strain-a novel software for real-time quantitative echocardiographic assessment of myocardial function. J Am Soc Echocardiogr. 2004;17(10):1021–9.
Stefani L et al. Two-dimensional tracking and TDI are consistent methods for evaluating myocardial longitudinal peak strain in left and right ventricle basal segments in athletes. Cardiovasc Ultrasound. 2007;5:7.
Lamash Y et al. Strain analysis from 4-D cardiac CT image data. IEEE Trans Biomed Eng. 2015;62(2):511–21.
Rizvi A et al. Analysis of ventricular function by CT. J Cardiovasc Comput Tomogr. 2015;9(1):1–12.
Cerqueira MD, Harp GD, Ritchie JL. Quantitative gated blood pool tomographic assessment of regional ejection fraction: definition of normal limits. J Am Coll Cardiol. 1992;20(4):934–41.
Zeb I et al. Computerized left ventricular regional ejection fraction analysis for detection of ischemic coronary artery disease with multidetector CT angiography. Int J Cardiovasc Imaging. 2013;29(3):685–92.
Pourmorteza A et al. Regional cardiac function assessment in 4D CT: comparison between SQUEEZ and ejection fraction. Conf Proc IEEE Eng Med Biol Soc. 2012;2012:4966–9.
• Pourmorteza A et al. A new method for cardiac computed tomography regional function assessment: stretch quantifier for endocardial engraved zones (SQUEEZ). Circ Cardiovasc Imaging. 2012;5(2):243–50. This study provides evidence that the regional myocardial function obtained by CT SQUEEZ, assessed among 162 segments in the 9 hearts, has good correlation with the tagged MRI as a reference standard for noninvasive regional myocardial function.
Pourmorteza A. et al. Correlation of CT-based regional cardiac function (SQUEEZ) with myocardial strain calculated from tagged MRI: an experimental study. Int J Cardiovasc Imaging. 2015.
Bansal M, Sengupta PP. Longitudinal and circumferential strain in patients with regional LV dysfunction. Curr Cardiol Rep. 2013;15(3):339.
Schuster A et al. Cardiovascular magnetic resonance myocardial feature tracking detects quantitative wall motion during dobutamine stress. J Cardiovasc Magn Reson. 2011;13:58.
Hor KN et al. Comparison of magnetic resonance feature tracking for strain calculation with harmonic phase imaging analysis. J Am Coll Cardiol Img. 2010;3(2):144–51.
Kuetting D et al. Comparison of magnetic resonance feature tracking with harmonic phase imaging analysis (CSPAMM) for assessment of global and regional diastolic function. Eur J Radiol. 2015;84(1):100–7.
Jeung MY et al. Myocardial tagging with MR imaging: overview of normal and pathologic findings. Radiographics. 2012;32(5):1381–98.
Jung B et al. Investigating myocardial motion by MRI using tissue phase mapping. Eur J Cardiothorac Surg. 2006;29 Suppl 1:S150–7.
Kim D, Kellman P. Improved cine displacement-encoded MRI using balanced steady-state free precession and time-adaptive sensitivity encoding parallel imaging at 3 T. NMR Biomed. 2007;20(6):591–601.
Simpson RM, Keegan J, Firmin DN. MR assessment of regional myocardial mechanics. J Magn Reson Imaging. 2013;37(3):576–99.
Osman NF et al. Imaging longitudinal cardiac strain on short-axis images using strain-encoded MRI. Magn Reson Med. 2001;46(2):324–34.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Menhel Kinno, Prashant Nagpal, Stephen Horgan, and Alfonso H. Waller declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Echocardiography
Rights and permissions
About this article
Cite this article
Kinno, M., Nagpal, P., Horgan, S. et al. Comparison of Echocardiography, Cardiac Magnetic Resonance, and Computed Tomographic Imaging for the Evaluation of Left Ventricular Myocardial Function: Part 2 (Diastolic and Regional Assessment). Curr Cardiol Rep 19, 6 (2017). https://doi.org/10.1007/s11886-017-0816-3
Published:
DOI: https://doi.org/10.1007/s11886-017-0816-3