Abstract
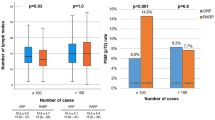
Robotic-assisted laparoscopic radical prostatectomy (RALP) is an established trend in surgical treatment for localized prostate cancer in the USA; however, RALP is still in its infancy in Taiwan. We have tracked various indicators of proficiency as a single Taiwanese surgeon became familiar with the procedure through experience with 30 initial RALP surgeries using the da Vinci system between December 2005 and April 2007. Here, we report the changes in these proficiency indicators, and the short-term outcomes for the patients. Thirty consecutive patients were classified into group 1 (cases 1–15) and group 2 (cases 16–30). Preoperative clinical characteristics, including age, body mass index (BMI), American Society of Anesthesiologists anesthetic surgical risks class (ASA), prostate-specific antigen levels (PSA), and Gleason scores were similar between the groups. The clinical stage (T1/T2) was significantly higher in group 2 than in group 1 (p = 0.028). Group 1 needed more frequent insertion of a double-J stent (60% versus 0%) before surgery and evaluation by cystogram before removal of urethral catheter (80% versus 6.7%) than group 2; these differences were statistically significant. Blood loss and transfusion rates were lower in group 2, but complication and conversion rates were higher in group 1. These differences were not statistically significant. Positive surgical margins, continence rates, potency, and intercourse rates at 12 months were similar between the groups. Console time was 262 min in group 1 and 190 min in group 2 (p = 0.033); this appeared to be the best indicator of proficiency. Establishing proficiency as determined by functional outcomes required about 30 cases, but the positive surgical margin rates indicate that experience with more than 30 cases was needed to ascend the learning curve with respect to oncological outcomes.

Similar content being viewed by others
References
Patel VR, Chammas MF Jr, Shah S (2007) Robotic assisted laparoscopic radical prostatectomy: a review of the current state of affairs. Int J Clin Pract 61(2):309–314
Pu YS, Chiang HS, Lin CC et al (2004) Changing trends of prostate cancer in Asia. Aging Male 7(2):120–132
Ou YC, Chen JT, Yang CR et al (2002) Predicting prostate specific antigen failure after radical retropubic prostatectomy for T1c prostate cancer. Jpn J Clin Oncol 32(12):536–542
Patel VR, Tully AS, Holmes R et al (2005) Robotic radical prostatectomy in the community setting—the learning curve and beyond: initial 200 cases. J Urol 174(1):269–272
Sahabudin RM, Arni T, Ashani N et al (2006) Development of robotic program: an Asian experience. World J Urol 24(2):161–164 Epub 2006 Apr 11
Patel VR, Thaly R, Shah K (2007) Robotic radical prostatectomy: outcomes of 500 cases. BJU Int 99(5):1109–1112
Patel VR, Shah K, Thaly R (2007) Robotic-assisted laparoscopic radical prostatectomy: the Ohio State University technique. J Robot Surg 1:51–59
Van Velthoven RF, Ahlering TE, Peltier A, Skarecky DW, Clayman RV (2003) Technique for laparoscopic running urethrovesical anastomosis: the single knot method. Urology 61(4):699–702
Brawley OW, Knopf K, Thompson I (2006) The epidemiology of prostate cancer part II: the risk factors. Semin Urol Oncol 16:193–201
Menon M, Tewari A, Baize B et al (2002) Prospective comparison of radical retropubic prostatectomy and robot-assisted anatomic prostatectomy: the Vattikuti Urology Institute experience. Urology 60(5):864–868
Ahlering TE, Woo D, Eichel L et al (2004) Robot-assisted versus open radical prostatectomy: a comparison of one surgeon’s outcomes. Urology 63(5):819–822
Menon M, Tewari A, Vattikuti Institute prostatectomy team (2003) Robotic radical prostatectomy and the Vattikuti Urology Institute technique: an interim analysis of results and technical points. Urology 61(4 Suppl 1):15–20
Cathelineau X, Rozet F, Vallancien G (2004) Robotic radical prostatectomy: the European experience. Urol Clin North Am 31(4):693–699 viii
Menon M, Tewari A, Peabody JO et al (2004) Vattikuti Institute prostatectomy, a technique of robotic radical prostatectomy for management of localized carcinoma of the prostate: experience of over 1,100 cases. Urol Clin North Am 31(4):701–717
Ahlering TE, Skarecky D, Lee D et al (2003) Successful transfer of open surgical skills to a laparoscopic environment using a robotic interface: initial experience with laparoscopic radical prostatectomy. J Urol 170(5):1738–1741
Smith JA Jr (2004) Robotically assisted laparoscopic prostatectomy: an assessment of its contemporary role in the surgical management of localized prostate cancer. Am J Surg 188(4):63S–67S
Pasticier G, Rietbergen JB, Guillonneau B et al (2001) Robotically assisted laparoscopic radical prostatectomy: feasibility study in men. Eur Urol 40(1):70–74
Poore RE, McCullough DL, Jarow JP (1998) Puboprostatic ligament sparing improves urinary continence after radical retropubic prostatectomy. Urology 51(1):67–72
Stolzenburg JU, Liatsikos EN, Rabenalt R et al (2006) Nerve sparing endoscopic extraperitoneal radical prostatectomy—effect of puboprostatic ligament preservation on early continence and positive margins. Eur Urol 49(1):103–111; discussion 111-2. Epub 2005 Nov 2
Takenaka A, Tewari AK, Leung RA et al (2007) Preservation of the puboprostatic collar and puboperineoplasty for early recovery of urinary continence after robotic prostatectomy: anatomic basis and preliminary outcomes. Eur Urol 51(2):433–440; discussion 440. Epub 2006 Jul 28
Tewari A, Srivasatava A, Menon M et al (2003) A prospective comparison of radical retropubic and robot-assisted prostatectomy: experience in one institution. BJU Int 92(3):205–210
Menon M, Kaul S, Bhandari A et al (2005) Potency following robotic radical prostatectomy: a questionnaire based analysis of outcomes after conventional nerve sparing and prostatic fascia sparing techniques. J Urol 174(6):2291–2296; discussion 2296
Martinez-Salamanca JI, Rao S, Ramanathan R et al (2007) Robotic radical prostatectomy: Cornell University technique athermal robotic technique (ART). Arch Esp Urol 60(4):383–396 Spanish
Atug F, Castle EP, Srivastav SK et al (2006) Positive surgical margins in robotic-assisted radical prostatectomy: impact of learning curve on oncologic outcomes. Eur Urol 49(5):866–871; discussion 871-2
Herrell SD, Smith JA Jr (2005) Robotic-assisted laparoscopic prostatectomy: what is the learning curve. Urology 66(5A):105–107
Acknowledgments
The authors thank Miss Hsiu-Ying Chang of the Biostatics Task Force of Taichung Veteran General Hospital for her assistance with statistical analyses.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ou, YC., Yang, CR., Wang, J. et al. Robotic-assisted radical prostatectomy by a single surgeon in Taiwan: experience with the initial 30 cases. J Robotic Surg 2, 173–179 (2008). https://doi.org/10.1007/s11701-008-0107-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11701-008-0107-5