Abstract
Purpose
Obesity is associated with increased breast cancer risk in women. Bariatric surgery induces substantial weight loss. However, the effects of such weight loss on subsequent breast cancer risk in women with obesity are poorly understood. To examine breast cancer incidence and related outcomes in women with obesity undergoing bariatric surgery.
Materials and Methods
This was a population-based matched cohort study of breast surgery outcomes utilizing linked clinical databases in Ontario, Canada. Women with obesity who underwent bariatric surgery were 1:1 matched using a propensity score to non-surgical controls for age and breast cancer screening history. The main outcomes were incidence of breast cancer after lag periods of 1, 2, and 5 years. Additional outcomes included tumor hormone receptor status, cancer stage, and treatments undertaken. Time-varying Cox proportional hazard models accounting for screening during follow-up were used to model cancer incidence.
Results
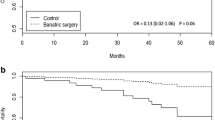
A total of 12,724 women per group were included, average age 45.09. After a 1-year lag, breast cancer incidence occurred in 1.09% and 0.79% of the control and surgery groups, respectively (adjusted hazard ratio, 0.81 [95%CI 0.69–0.95]; p = 0.01). This association was maintained after lag periods of 2 and 5 years. Women in the surgical cohort diagnosed with breast cancer were more likely to have low-grade tumors and less likely to have high-grade tumors (overall p < 0.01). No association was found for tumor hormone receptor status, although the surgical group was more likely to have her2neu-negative tumors (p = 0.01).
Conclusion
Bariatric surgery was associated with a lower incidence of breast cancer and lower tumor grade in women with obesity. Further evaluation of outcomes, including mortality, is required.
Graphical abstract



Similar content being viewed by others
References
Lauby-Secretan B, Dossus L, Marant-Micallef C, His M. Obésité et cancer [Obesity and Cancer]. Bull Cancer. 2019;106(7–8):635–646. French. https://doi.org/10.1016/j.bulcan.2019.04.008.
Lauby-Secretan B, Scoccianti C, Loomis D, Grosse Y, Bianchini F, Straif K. International agency for research on cancer handbook working group. Body fatness and cancer- viewpoint of the IARC working group. N Engl J Med. 2016;375(8):794–8. https://doi.org/10.1056/NEJMsr1606602.
Bruno DS, Berger NA. Impact of bariatric surgery on cancer risk reduction. Ann Transl Med. 2020;8:S13–S13.
Heshmati K, Harris DA, Rosner B, Pranckevicius E, Ardestani A, Cho N, et al. Association of bariatric surgery status with reduced HER2+ breast cancers: a retrospective cohort study. Obes Surg Obesity Surgery. 2019;29:1092–8.
Feigelson HS, Caan B, Weinmann S, Leonard AC, Powers JD, Yenumula PR, et al. Bariatric surgery is associated with reduced risk of breast cancer in both premenopausal and postmenopausal women. Ann Surg. 2019;271:1.
Neuhouser ML, Aragaki AK, Prentice RL, Manson JE, Chlebowski R, Carty CL et al. Overweight, obesity, and postmenopausal invasive breast cancer risk: A secondary analysis of the women's health initiative randomized clinical trials. JAMA Oncol. 2015;1(5):611–21. https://doi.org/10.1001/jamaoncol.2015.1546.
Liu K, Zhang W, Dai Z, Wang M, Tian T, Liu X, et al. Association between body mass index and breast cancer risk: evidence based on a dose–response meta-analysis. Cancer Manag Res. 2018;10:143–51.
Park JW, Han K, Shin DW, Yeo Y, Chang JW, Yoo JE et al. Obesity and breast cancer risk for pre- and postmenopausal women among over 6 million Korean women. Breast Cancer Res Treat. 2021;185(2):495–506. https://doi.org/10.1007/s10549-020-05952-4.
Renehan AG, Tyson M, Egger M, Heller RF, Zwahlen M. Body-mass index and incidence of cancer: a systematic review and meta-analysis of prospective observational studies. Lancet. 2008;371(9612):569–78. https://doi.org/10.1016/S0140-6736(08)60269-X.
Moley KH, Colditz GA. Effects of obesity on hormonally driven cancer in women. Sci Transl Med. 2016;8:1–6.
Picon-Ruiz M, Morata-Tarifa C, Valle-Goffin JJ, Friedman ER, Slingerland JM. Obesity and adverse breast cancer risk and outcome: Mechanistic insights and strategies for intervention. CA Cancer J Clin. 2017;67(5):378–397. https://doi.org/10.3322/caac.21405.
Munsell MF, Sprague BL, Berry DA, Chisholm G, Trentham-Dietz A. Body mass index and breast cancer risk according to postmenopausal estrogen-progestin use and hormone receptor status. Epidemiol Rev. 2014;36(1):114–36. https://doi.org/10.1093/epirev/mxt010.
Michels KB, Terry KL, Eliassen AH, Hankinson SE, Willett WC. Adult weight change and incidence of premenopausal breast cancer. Int J Cancer. 2012;130(4):902–9. https://doi.org/10.1002/ijc.26069.
Lovrics O, Butt J, Lee Y, Lovrics P, Boudreau V, Anvari M et al. The effect of bariatric surgery on breast cancer incidence and characteristics: A meta-analysis and systematic review. Am J Surg. 2021;222(4):715–722. https://doi.org/10.1016/j.amjsurg.2021.03.016.
Hardefeldt PJ, Penninkilampi R, Edirimanne S, Eslick GD. Physical activity and weight loss reduce the risk of breast cancer: a meta-analysis of 139 prospective and retrospective studies. Clin Breast Cancer [Internet]. Elsevier Inc.; 2018;18:e601–12. Available from: https://doi.org/10.1016/j.clbc.2017.10.010
Luo J, Hendryx M, Manson JE, Figueiredo JC, LeBlanc ES, Barrington W et al. Intentional weight loss and obesity-related cancer risk. JNCI Cancer Spectr. 2019;3(4):pkz054. https://doi.org/10.1093/jncics/pkz054
Teras LR, Patel AV, Wang M, Yaun SS, Anderson K, Brathwaite R, et al. Sustained weight loss and risk of breast cancer in women 50 years and older: a pooled analysis of prospective data. J Natl Cancer Inst. 2020;112:929–37.
Maciejewski ML, Arterburn DE, Van Scoyoc L, Smith VA, Yancy WS, Weidenbacher HJ, et al. Bariatric surgery and long-term durability of weight loss. JAMA Surg. 2016
Arterburn DE, Telem DA, Kushner RF, Courcoulas AP. Benefits and risks of bariatric surgery in adults: a review. JAMA - J Am Med Assoc. 2020;324:879–87.
Hassinger TE, Mehaffey JH, Hawkins RB, Schirmer BD, Hallowell PT, Schroen AT, Showalter SL. Overall and estrogen receptor-positive breast cancer incidences are decreased following bariatric surgery. Obes Surg. 2019;29(3):776–781. https://doi.org/10.1007/s11695-018-3598-9.
Doumouras AG, Saleh F, Gmora S, Anvari M, Hong D. Regional variations in the public deliver y of bariatric surgery: an evaluation of the center of excellence model. Ann Surg. 2016;263:306–11.
Doumouras AG, Anvari S, Breau R, Anvari M, Hong D, Gmora S. The effect of an online referral system on referrals to bariatric surgery. Surg Endosc. Springer US; 2017;31:5127–34.
Chair MG, Barondess JM, Bellegie NJ, Fromm H, Greenaway F, Halsted CH, et al. Gastrointestinal surgery for severe obesity: consensus statement. Nutr Today. 1991;26:32–5.
Tu K, Mitiku TF, Ivers NM, Guo H, Lu H, Jaakkimainen L, et al. Evaluation of Electronic Medical Record Administrative data Linked Database (EMRALD). Am J Manag Care United States. 2014;20:e15-21.
Austin PC. Balance diagnostics for comparing the distribution of baseline covariates between treatment groups in propensity-score matched samples. Stat Med. 2009;28:3083–107.
Austin PC. An introduction to propensity score methods for reducing the effects of confounding in observational studies. Multivariate Behav Res. 2011;46:399–424.
Mamdani M, Sykora K, Li P, Normand S-LT, Streiner DL, Austin PC, et al. Reader’s guide to critical appraisal of cohort studies: 2. Assessing potential for confounding. BMJ. 2005;330:960–2.
Austin PC. Some methods of propensity-score matching had superior performance to others: results of an empirical investigation and monte carlo simulations. Biometrical J. 2009;51:171–84.
Cancer Care Ontario. Data Sources [Appendices 1] | Cancer Care Ontario [Internet]. [cited 2021 Jul 27]. Available from: https://www.cancercareontario.ca/en/statistical-reports/ontario-cancer-statistics-2020/data-sources
Boyle P, Boniol M, Koechlin A, Robertson C, Valentini F, Coppens K, et al. Diabetes and breast cancer risk: A meta-analysis. Br J Cancer Nature Publishing Group. 2012;107:1608–17.
Kolb R, Zhang W. Obesity and breast cancer: a case of inflamed adipose tissue. Cancers (Basel). 2020;12:1–18.
Nagahashi M, Yamada A, Katsuta E, Aoyagi T, Huang WC, Terracina KP, et al. Targeting the SphK1/S1P/S1PR1 axis that links obesity, chronic inflammation, and breast cancer metastasis. Cancer Res. 2018;78:1713–25.
Winder AA, Kularatna M, MacCormick AD. Does bariatric surgery affect the incidence of breast cancer development? A systematic review. Obes Surg Obesity Surgery. 2017;27:3014–20.
Tong Y, Wu J, Huang O, He J, Zhu L, Chen W, et al. IGF-1 interacted with obesity in prognosis prediction in HER2-positive breast cancer patients. Front Oncol. 2020;10:1–10.
Anveden Å, Taube M, Peltonen M, Jacobson P, Andersson-Assarsson JC, Sjöholm K, et al. Long-term incidence of female-specific cancer after bariatric surgery or usual care in the Swedish Obese Subjects Study. Gynecol Oncol [Internet]. Elsevier Inc.; 2017;145:224–9. Available from: https://doi.org/10.1016/j.ygyno.2017.02.036
Fabian CJ, Kimler BF, Donnelly JE, Sullivan DK, Klemp JR, Petroff BK, et al. Favorable modulation of benign breast tissue and serum risk biomarkers is associated with >10 % weight loss in postmenopausal women. Breast Cancer Res Treat. 2013;142:119–32.
Rose DP, Gracheck PJ, Davis LV. The interactions of obesity, inflammation and insulin resistance in breast cancer. Cancers (Basel). 2015;7:2134–68.
Ayoub NM, Yaghan RJ, Abdo NM, Matalka II, Akhu-Zaheya LM, Al-Mohtaseb AH. Impact of obesity on clinicopathologic characteristics and disease prognosis in pre- and postmenopausal breast cancer patients: A retrospective institutional study. J Obes. 2019;2019:3820759.
Peláez-Jaramillo MJ, Cárdenas-Mojica AA, Gaete P V., Mendivil CO. Post-liver transplantation diabetes mellitus: a review of relevance and approach to treatment. Diabetes Ther. 2018
Argolo DF, Hudis CA, Iyengar NM. The Impact of obesity on breast cancer. Curr Oncol Rep. 2018;20(6):47. https://doi.org/10.1007/s11912-018-0688-8.
Shrank WH, Patrick AR, Brookhart MA. Healthy user and related biases in observational studies of preventive interventions: a primer for physicians. J Gen Intern Med. 2011
Iwase T, Wang X, Shrimanker TV, Kolonin MG, Ueno NT. Body composition and breast cancer risk and treatment: mechanisms and impact. Breast Cancer Res Treat [Internet]. Springer US; 2021;186:273–83. Available from: https://doi.org/10.1007/s10549-020-06092-5
Owens DK, Davidson KW, Krist AH, Barry MJ, Cabana M, Caughey AB, et al. Medication use to reduce risk of breast cancer: US Preventive Services Task Force recommendation statement. JAMA - J Am Med Assoc. 2019;322:857–67.
Chang SH, Stoll CRT, Song J, Varela JE, Eagon CJ, Colditz GA. The effectiveness and risks of bariatric surgery an updated systematic review and meta-analysis, 2003–2012. JAMA Surg. 2014;149:275–87.
Chlebowski RT, Luo J, Anderson GL, Barrington W, Reding K, Simon MS et al. Weight loss and breast cancer incidence in postmenopausal women. Cancer. 2019;125(2):205 212. https://doi.org/10.1002/cncr.31687.
Funding
This study was supported by ICES, which is funded by an annual grant from the Ontario Ministry of Health. This study was also supported by the Ontario Bariatric Registry. Parts of this material are based on data and information compiled and provided by the Ontario Ministry of Health, Ontario Health, and the Canadian Institute for Health Information. The analyses, conclusions, opinions, and statements expressed herein are solely those of the authors and do not reflect those of the funding or data sources; no endorsement is intended or should be inferred.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Consent to Participate
ICES is an independent, non-profit research institute whose legal status under Ontario’s health information privacy law allows it to collect and analyze healthcare and demographic data, without individual consent, for health system evaluation and improvement. These datasets were linked using unique encoded identifiers and analyzed at ICES. For this type of study, formal consent is not required.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key Points
1. Bariatric surgery is associated with lower incidence of breast cancer compared to a highly matched non-surgery group.
2. Bariatric surgery is associated with more favorable tumor grade.
3. No effect was found for stage at diagnosis or tumor hormone receptor status.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Doumouras, A.G., Lovrics, O., Paterson, J.M. et al. Bariatric Surgery and Breast Cancer Incidence: a Population-Based, Matched Cohort Study. OBES SURG 32, 1261–1269 (2022). https://doi.org/10.1007/s11695-022-05946-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-022-05946-9