Abstract
Background
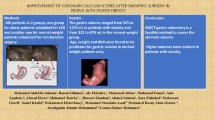
Most bariatric treatments employ gastric volume reduction. However, there has been no appropriate tool that could assess the anatomical factors of the stomach, and few studies have investigated proper stomach measurement for bariatric treatment. Thus, this study aimed to objectively estimate the individual stomach using three-dimensional (3D) computed tomography (CT) gastrography for the possible acquisition of information that could facilitate bariatric treatment and to validate these factors.
Methods
A total of 100 consecutive patients with different degrees of obesity who underwent 3D CT gastrography were enrolled. Using semiautomatic and manual segmentation tools, 3D volume-rendered images were constructed, and the total volume of the distended stomach, abdominal diameter, and abdominal fat volume (visceral and subcutaneous fat) were measured. Data on patients’ baseline characteristics and laboratory findings were collected.
Results
The stomach volume measured using 3D CT gastrography ranged from 268 to 751 mL, whereas the stomach capacity was 572 ± 301.6 mL and 438.5 ± 163.4 mL in patients with body mass index (BMI) ≥ 25 kg/m2 and < 25 kg/m2, respectively. Visceral fat volume, abdominal circumference, and visceral-to-subcutaneous fat ratio tended to be associated with increased stomach volume. Multivariate analysis showed that BMI and visceral fat volume were significantly associated with stomach volume in female patients.
Conclusions
The results of this study indicated the association of stomach volume with obesity status. Objective estimation of the individual stomach presented the possibility of tailored therapeutic approach to obese patients requiring more effective bariatric treatment.



Similar content being viewed by others
References
Hoque ME, Mannan M, Long KZ, et al. Economic burden of underweight and overweight among adults in the Asia-Pacific region: a systematic review. Tropical Med Int Health. 2016;21(4):458–69.
Sartoretto A, Sui Z, Hill C, et al. Endoscopic sleeve gastroplasty (ESG) is a reproducible and effective endoscopic bariatric therapy suitable for widespread clinical adoption: a large, international multicenter study. Obes Surg. 2018;28(7):1812–21.
Bray GA, Kim KK, Wilding JPH. World Obesity Federation. Obesity: a chronic relapsing progressive disease process. A position statement of the World Obesity Federation. Obes Rev. 2017;18(7):715–23.
Maleckas A, Gudaitytė R, Petereit R, et al. Weight regain after gastric bypass: etiology and treatment options. Gland Surg. 2016;5(6):617–24.
Kim SH, Chun HJ, Choi HS, et al. Current status of intragastric balloon for obesity treatment. World J Gastroenterol. 2016;22(24):5495–504.
Choi HS, Chun HJ. Recent trends in endoscopic bariatric therapies. Clin Endosc. 2017;50(1):11–6.
Yoo IK, Chun HJ, Jeen YT. Gastric perforation caused by an intragastric balloon: endoscopic findings. Clin Endosc. 2017;50(6):602–4.
Bouras EP, Delgado-Aros S, Camilleri M, et al. SPECT imaging of the stomach: comparison with barostat, and effects of sex, age, body mass index, and fundoplication. Single photon emission computed tomography. Gut. 2002;51(6):781–6.
Delgado-Aros S, Cremonini F, Castillo JE, et al. Independent influences of body mass and gastric volumes on satiation in humans. Gastroenterology. 2004;126(2):432–40.
Geliebter A. Gastric distension and gastric capacity in relation to food intake in humans. Physiol Behav. 1988;44(4–5):665–8.
Geliebter A, Hashim SA. Gastric capacity in normal, obese, and bulimic women. Physiol Behav. 2001;74(4–5):743–6.
Geliebter A, Schachter S, Lohmann-Walter C, et al. Reduced stomach capacity in obese subjects after dieting. Am J Clin Nutr. 1996;63(2):170–3.
Csendes A, Burgos AM. Size, volume and weight of the stomach in patients with morbid obesity compared to controls. Obes Surg. 2005;15(8):1133–6.
Huh J, Lee IS, Kim KW, et al. CT gastrography for volumetric measurement of remnant stomach after distal gastrectomy: a feasibility study. Abdom Radiol (NY). 2016;41(10):1899–905.
Ruiz-Tovar J, Carbajo MA, Jimenez JM, et al. Long-term follow-up after sleeve gastrectomy versus Roux-en-Y gastric bypass versus one-anastomosis gastric bypass: a prospective randomized comparative study of weight loss and remission of comorbidities. Surg Endosc. 2019;33(2):401–10. https://doi.org/10.1007/s00464-018-6307-9.
Alvarez V, Carrasco F, Cuevas A, et al. Mechanisms of long-term weight regain in patients undergoing sleeve gastrectomy. Nutrition. 2016;32(3):303–8.
Goulart A, Leão P, Costa P, et al. Doctor, how much weight will I lose?—a new individualized predictive model for weight loss. Obes Surg. 2016;26(6):1357–9. WOS:000375794000034;26(6):1357–9
Funding
This work was supported by the National Research Foundation of Korea (NRF) grant funded by the Korean Government (NRF-2019R1C1C1009819) and was supported by a grant of Korea University Anam Hospital, Seoul, Republic of Korea (Grant No. O1801001).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kim, S.H., Keum, B., Choi, H.S. et al. Stomach Volume Assessment Using Three-dimensional Computed Tomography Gastrography for Bariatric Treatment. OBES SURG 30, 401–406 (2020). https://doi.org/10.1007/s11695-019-04189-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-019-04189-5