Abstract
Background
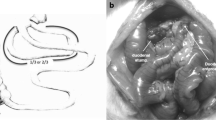
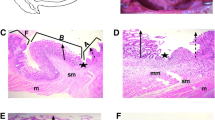
Duodenal–jejunal bypass (DJB) has been shown to reverse type 2 diabetes (T2DM) in Goto–Kakizaki (GK) rats, a rodent model of non-obese T2DM. Skeletal muscle insulin resistance is a hallmark decrement in T2DM. The aim of the current work was to investigate the effects of DJB on skeletal muscle insulin signal transduction and glucose disposal. It was hypothesized that DJB would increase skeletal muscle insulin signal transduction and glucose disposal in GK rats.
Methods
DJB was performed in GK rats. Sham operations were performed in GK and nondiabetic Wistar–Kyoto (WKY) rats. At 2 weeks post-DJB, oral glucose tolerance (OGTT) was measured. At 3 weeks post-DJB, insulin-induced signal transduction and glucose disposal were measured in skeletal muscle.
Results
In GK rats and compared to sham operation, DJB did not (1) improve fasting glucose or insulin, (2) improve OGTT, or (3) increase skeletal muscle insulin signal transduction or glucose disposal. Interestingly, skeletal muscle glucose disposal was similar between WKY-Sham, GK-Sham, and GK-DJB.
Conclusions
Bypassing of the proximal small intestine does not increase skeletal muscle glucose disposal. The lack of skeletal muscle insulin resistance in GK rats questions whether this animal model is adequate to investigate the etiology and treatments for T2DM. Additionally, bypassing of the foregut may lead to different findings in other animal models of T2DM as well as in T2DM patients.



Similar content being viewed by others
References
American Diabetes Association. Economic costs of diabetes in the U.S. in 2002. Diabetes Care. 2003;26:917–32.
Brozinick Jr JT, Roberts BR, Dohm GL. Defective signaling through Akt-2 and -3 but not Akt-1 in insulin-resistant human skeletal muscle: potential role in insulin resistance. Diabetes. 2003;52:935–41.
Buchwald H, Avidor Y, Braunwald E, et al. Bariatric surgery: a systematic review and meta-analysis. JAMA. 2004;292:1724–37.
Buchwald H, Estok R, Fahrbach K, et al. Weight and type 2 diabetes after bariatric surgery: systematic review and meta-analysis. Am J Med. 2009;122:248–56. e245.
Cani PD, Bibiloni R, Knauf C, et al. Changes in gut microbiota control metabolic endotoxemia-induced inflammation in high-fat diet-induced obesity and diabetes in mice. Diabetes. 2008;57:1470–81.
Chou CJ, Membrez M, Blancher F. Gut decontamination with norfloxacin and ampicillin enhances insulin sensitivity in mice. Nestle Nutr Workshop Ser Pediatr Program. 2008;62:127–37. discussion 137–140.
Cohen RV, Schiavon CA, Pinheiro JS, et al. Duodenal–jejunal bypass for the treatment of type 2 diabetes in patients with body mass index of 22–34 kg/m(2): a report of 2 cases. Surg Obes Relat Dis. 2007;3:195–7.
Corcoran MP, Lamon-Fava S, Fielding RA. Skeletal muscle lipid deposition and insulin resistance: effect of dietary fatty acids and exercise. Am J Clin Nutr. 2007;85:662–77.
Dadke S, Kusari J, Chernoff J. Down-regulation of insulin signaling by protein-tyrosine phosphatase 1B is mediated by an N-terminal binding region. J Biol Chem. 2000;275:23642–7.
DeFronzo RA, Ferrannini E, Simonson DC. Fasting hyperglycemia in non-insulin-dependent diabetes mellitus: contributions of excessive hepatic glucose production and impaired tissue glucose uptake. Metabolism. 1989;38:387–95.
DeFronzo RA, Jacot E, Jequier E, et al. The effect of insulin on the disposal of glucose: results from indirect calorimetry and hepatic and femoral venous catheterization. Diabetes. 1981;30:1000–7.
Dohm GL, Kasperek GJ, Tapscott EB, et al. Effect of exercise on synthesis and degradation of muscle protein. Biochem J. 1980;188:255–62.
Dolan PL, Tapscott EB, Dorton PJ, et al. Contractile activity restores insulin responsiveness in skeletal muscle of obese Zucker rats. Biochem J. 1993;289(Pt 2):423–6.
Ferzli GS, Dominique E, Ciaglia M, et al. Clinical improvement after duodenojejunal bypass for nonobese type 2 diabetes despite minimal improvement in glycemic homeostasis. World J Surg. 2009;33:972–9.
Friedman JE, Dohm GL, Leggett-Frazier N, et al. Restoration of insulin responsiveness in skeletal muscle of morbidly obese patients after weight loss. Effect on muscle glucose transport and glucose transporter GLUT4. J Clin Invest. 1992;89:701–5.
Geloneze B, Geloneze SR, Fiori C, et al. Surgery for nonobese type 2 diabetic patients: an interventional study with duodenal–jejunal exclusion. Obes Surg. 2009;19:1077–83.
Krein SL, Funnell MM, Piette JD. Economics of diabetes mellitus. Nurs Clin North Am. 2006;41:499–511. v–vi.
Krook A, Kawano Y, Song XM, et al. Improved glucose tolerance restores insulin-stimulated Akt kinase activity and glucose transport in skeletal muscle from diabetic Goto–Kakizaki rats. Diabetes. 1997;46:2110–4.
Matthews DR, Hosker JP, Rudenski AS, et al. Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia. 1985;28:412–9.
Membrez M, Blancher F, Jaquet M, et al. Gut microbiota modulation with norfloxacin and ampicillin enhances glucose tolerance in mice. FASEB J. 2008;22:2416–26.
Movassat J, Bailbe D, Lubrano-Berthelier C, et al. Follow-up of GK rats during prediabetes highlights increased insulin action and fat deposition despite low insulin secretion. Am J Physiol Endocrinol Metab. 2008;294:E168–75.
Petersen KF, Shulman GI. Etiology of insulin resistance. Am J Med. 2006;119:S10–6.
Pories WJ, Caro JF, Flickinger EG, et al. The control of diabetes mellitus (NIDDM) in the morbidly obese with the Greenville gastric bypass. Ann Surg. 1987;206:316–23.
Pories WJ, Swanson MS, MacDonald KG, et al. Who would have thought it? An operation proves to be the most effective therapy for adult-onset diabetes mellitus. Ann Surg. 1995;222:339–50. discussion 350–332.
Portha B, Serradas P, Bailbe D, et al. Beta-cell insensitivity to glucose in the GK rat, a spontaneous nonobese model for type II diabetes. Diabetes. 1991;40:486–91.
Rubino F, Forgione A, Cummings DE, et al. The mechanism of diabetes control after gastrointestinal bypass surgery reveals a role of the proximal small intestine in the pathophysiology of type 2 diabetes. Ann Surg. 2006;244:741–9.
Rubino F, Marescaux J. Effect of duodenal–jejunal exclusion in a non-obese animal model of type 2 diabetes: a new perspective for an old disease. Ann Surg. 2004;239:1–11.
Acknowledgments
This study was supported by an East Carolina University Research Development grant (TP Gavin) and a National Institute on Health grant-R01 DK046121 (GL Dohm).
Conflicts of Interest
The authors declare no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gavin, T.P., Sloan, R.C., Lukosius, E.Z. et al. Duodenal–Jejunal Bypass Surgery Does Not Increase Skeletal Muscle Insulin Signal Transduction or Glucose Disposal in Goto–Kakizaki Type 2 Diabetic Rats. OBES SURG 21, 231–237 (2011). https://doi.org/10.1007/s11695-010-0304-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-010-0304-y