Abstract
Objective
To investigate the protective effects of modified Linggui Zhugan Decoction (加味苓桂术甘汤, MLZD), a traditional Chinese medicine formula, on obese type 2 diabetes mellitus (T2DM) rats.
Methods
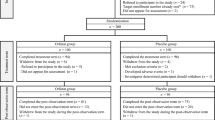
Fifty Sprague-Dawley rats were randomly divided into 5 groups by a random number table, including normal, obese T2DM (ob-T2DM), MLZD low-dose [MLDZ-L, 4.625 g/(kg·d)], MLZD middle-dose [MLD-M, 9.25 g/(kg·d) ] and MLZD high-dose [MLD-H, 18.5 g/(kg·d)] groups, 10 rats in each group. After 4-week intervention, blood samples and liver, pancreas, muscle tissues were collected to assess the insulin resistance (IR), blood lipid, adipokines and inflammation cytokines. The alteration of phosphatidylinositol 3 kinase (PI3K)-protein kinase B (PKB or Akt)/the mammalian target of rapamycin (mTOR)-ribosome protein subunit 6 kinase 1 (S6K1 )/AMP-activated protein kinase (AMPK)-peroxisome proliferator-activated receptor gamma coactivator 1 alpha (PGC-1 α) pathways were also studied.
Results
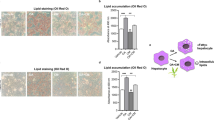
MLZD dose-dependently reduced fasting blood glucose, fasting insulin, homeostasis model of assessment for IR index and increased insulin sensitive index compared with ob-T2DM rats (P<0.05). Similarly, total cholesterol, triglyceride, low-density lipoprotein cholesterol and free fatty acids were also decreased compared with ob-T2DM rats after 4-week treatment (P<0.05 or P<0.01). Improvements in adipokines and inflammatory cytokines were observed with a raised level of adiponectin and a reduced level of leptin, resistin, tumor necrosis factor-α and interleukin-6 (P<0.05 or P<0.01). MLZD regulated the PI3K-Akt/mTOR-S6K1/AMPK-PGC-1 α pathways and restored the tissue structure of liver and pancreas (P<0.05 or P<0.01).
Conclusions
MLZD ameliorated glycolipid metabolism and inflammation, which may be attributed to the regulation of PI3K-Akt/mTOR-S6K1/AMPK-PGC-1 α pathways.
Similar content being viewed by others
References
Wright AK, Kontopantelis E, Emsley R, Buchan I, Sattar N, Rutter MK. Life expectancy and cause-specific mortality in type 2 diabetes: a population-based cohort study quantifying relationships in ethnic subgroups. Diabetes Care 2017;40:338–345.
Collaborators GBDO, Afshin A, Forouzanfar MH, Reitsma MB, Sur P, Estep K, et al. Health effects of overweight and obesity in 195 countries over 25 years. N Engl J Med 2017;377:13–27.
Chen Y, Copeland WK, Vedanthan R, Grant E, Lee JE, Gu D, et al. Association between body mass index and cardiovascular disease mortality in east Asians and south Asians: pooled analysis of prospective data from the Asia Cohort Consortium. BMJ 2013;347:f5446.
Global Burden of Metabolic Risk Factors for Chronic Diseases C, Lu Y, Hajifathalian K, Ezzati M, Woodward M, Rimm EB, et al. Metabolic mediators of the effects of body-mass index, overweight, and obesity on coronary heart disease and stroke: a pooled analysis of 97 prospective cohorts with 1.8 million participants. Lancet 2014;383:970–983.
Roden M, Shulman GI. The integrative biology of type 2 diabetes. Nature 2019;576:51–60.
Scherer PE. The many secret lives of adipocytes: implications for diabetes. Diabetologia 2019;62:223–232.
Zhang ZJ. Synopsis of Golden Chamber. Beijing: People's Medical Publishing House 2005;12:44–45.
Liu T, Yang LL, Zou L, Li DF, Wen HZ, Zheng PY, et al. Chinese medicine formula Lingguizhugan Decoction improves beta-oxidation and metabolism of fatty acid in high-fat-diet-induced rat model of fatty liver disease. Evid Based Complement Alternat Med 2013;2013:429738.
Liu MT, Huang YJ, Zhang TY, Tan LB, Lu XF, Qin J. Lingguizhugan Decoction attenuates diet-induced obesity and hepatosteatosis via gut microbiota. World J Gastroenterol 2019;25:3590–3606.
Zhu M, Hao S, Liu T, Yang L, Zheng P, Zhang L, et al. Lingguizhugan Decoction improves non-alcoholic fatty liver disease by altering insulin resistance and lipid metabolism related genes: a whole trancriptome study by RNA-Seq. Oncotarget 2017;8:82621–82631.
Yang Y, Li Q, Chen S, Ke B, Huang Y, Qin J. Effects of modified Lingguizhugan Decoction combined with weekend fasting on metabolic syndrome. J Tradit Chin Med 2014;34:48–51.
Vanhaesebroeck B, Whitehead MA, Pineiro R. Molecules in medicine mini-review: isoforms of PI3K in biology and disease. J Molecul Med (Berlin, Germany) 2016;94:5–11.
Hemmings BA, Restuccia DF. PI3K-PKB/Akt pathway. Cold Spring Harb Perspect Biol 2012;4:a011189.
Nelson VL, Jiang YP, Dickman KG, Ballou LM, Lin RZ. Adipose tissue insulin resistance due to loss of PI3K p110alpha leads to decreased energy expenditure and obesity. Am J Physiol Endocrinol Metab 2014;306:E1205–E1216.
Yu C, Chen Y, Cline GW, Zhang D, Zong H, Wang Y, et al. Mechanism by which fatty acids inhibit insulin activation of insulin receptor substrate-1 (IRS-l)-associated phosphatidylinositol 3-kinase activity in muscle. J Biol Chem 2002;277:50230–502236.
Zhou H, Huang S. The complexes of mammalian target of rapamycin. Curr Protein Pept Sci 2010; 11:409–424.
Dann SG, Selvaraj A, Thomas G. mTOR Complexl-S6K1 signaling: at the crossroads of obesity, diabetes and cancer. Trends Mol Med 2007;13:252–259.
Hardie DG, Ross FA, Hawley SA. AMPK: a nutrient and energy sensor that maintains energy homeostasis. Nature Rev Molecul Cell Bio 2012;13:251–262.
Wu H, Deng X, Shi Y, Su Y, Wei J, Duan H. PGC-1alpha, glucose metabolism and type 2 diabetes mellitus. J Endocrinol 2016;229:R99–R115.
Cork GK, Thompson J, Slawson C. Real talk: the inter-play between the mTOR, AMPK, and hexosamine biosynthetic pathways in cell signaling. Front Endocrinol (Lausanne) 2018;9:522.
Salmanoglu DS, Gurpinar T, Vural K, Ekerbicer N. Dariverenli E, Var A. Melatonin and L-carnitin improves endothelial disfunction and oxidative stress in type 2 diabetic rats. Redox Biol 2016;8:199–204.
Nair AB, Jacob S. A simple practice guide for dose conversion between animals and human. J Basic Clin Pharm 2016;7:27–31.
Bray GA, Heisel WE, Afshin A, Jensen MD, Dietz WH, Long M, et al. The science of obesity management: an Endocrine Society Scientific Statement. Endocr Rev 2018;39:79–132.
Samuel VT, Petersen KF, Shulman GI. Lipid-induced insulin resistance: unravelling the mechanism. Lancet 2010;375:2267–2277.
Ghadge AA, Khaire AA. Leptin as a predictive marker for metabolic syndrome. Cytokine 2019;121:154735.
Su KZ, Li YR, Zhang D, Yuan JH, Zhang CS, Liu Y, et al. Relation of circulating resistin to insulin resistance in type 2 diabetes and obesity: a systematic review and metaanalysis. Front Physiol 2019; 10:1399.
Chakraborti CK. Role of adiponectin and some other factors linking type 2 diabetes mellitus and obesity. World J Diabetes 2015;6:1296–1308.
Perseghin G, Petersen K, Shulman GI. Cellular mechanism of insulin resistance: potential links with inflammation. Intern J Obesity Relat Metab Disord 2003:S6–S11.
Alzamil H. Elevated serum TNF-α is related to obesity in type 2 diabetes mellitus and is associated with glycemic control and insulin resistance. J Obesity 2020;2020:5076858.
Bertin E, Nguyen P, Guenounou M, Durlach V, Potron G, Leutenegger M. Plasma levels of tumor necrosis factor-alpha (TNF-alpha) are essentially dependent on visceral fat amount in type 2 diabetic patients. Diabet Metab 2000;26:178–182.
Lowe G, Woodward M, Hillis G, Rumley A, Li Q, Harrap S, et al. Circulating inflammatory markers and the risk of vascular complications and mortality in people with type 2 diabetes and cardiovascular disease or risk factors: the ADVANCE study. Diabetes 2014;63:1115–1123.
Pradhan AD, Manson JE, Rifai N, Buring JE, Ridker PM. C-reactive protein, interleukin 6, and risk of developing type 2 diabetes mellitus. JAMA 2001;286:327–334.
Qu D, Liu J, Lau CW, Huang Y. IL-6 in diabetes and cardiovascular complications. Br J Pharmacol 2014;171:3595–3603.
Chen Y, Wu Y, Gan X, Liu K, Lv X, Shen H, et al. Iridoid glycoside from Cornus officinalis ameliorated diabetes mellitus-induced testicular damage in male rats: Involvement of suppression of the AGEs/RAGE/p38 MAPK signaling pathway. J Ethnopharmacol 2016;194:850–860.
Jeftic I, Jovicic N, Pantic J, Arsenijevic N, Lukic ML. Pejnovic N. Galectin-3 ablation enhances liver steatosis, but attenuates inflammation and IL-33-dependent fibrosis in obesogenic mouse model of nonalcoholic steatohepatitis. Mol Med 2015;21:453–465.
Song Z, Guo Y, Zhou M, Zhang X. The PI3K/p-Akt signaling pathway participates in calcitriol ameliorating podocyte injury in DN rats. Metabolism 2014;63:1324–1333.
Huang X, Liu G, Guo J, Su Z. The PI3K/AKT pathway in obesity and type 2 diabetes. Int J Biol Sci 2018;14:1483–1496.
Ke B, Ke X, Wan X, Yang Y, Huang Y, Qin J, et al. Astragalus polysaccharides attenuates TNF-alpha-induced insulin resistance via suppression of miR-721 and activation of PPAR-gamma and PI3K/AKT in 3T3-L1 adipocytes. Am J Transl Res 2017;9:2195–2206.
Yan F, Dai G, Zheng X. Mulberry anthocyanin extract ameliorates insulin resistance by regulating PI3K/AKT pathway in HepG2 cells and db/db mice. J Nutr Biochem 2016;36:68–80.
Mishra AK, Dingli D. Metformin inhibits IL-6 signaling by decreasing IL-6R expression on multiple myeloma cells. Leukemia 2019;33:2695–2709.
Castilla-Madrigal R, Barrenetxe J, Moreno-Aliaga MJ. Lostao MP. EPA blocks TNF-alpha-induced inhibition of sugar uptake in Caco-2 cells via GPR120 and AMPK. J Cell Physiol 2018;233:2426–2433.
Wang Y, Shi M, Fu H, Xu H, Wei J, Wang T, et al. Mammalian target of the rapamycin pathway is involved in non-alcoholic fatty liver disease. Mol Med Rep 2010;3:909–915.
Liu L, Yao L, Wang S, Chen Z, Han T, Ma P, et al. 6-Gingerol improves ectopic lipid accumulation, mitochondrial dysfunction, and insulin resistance in skeletal muscle of ageing rats: dual stimulation of the AMPK/PGC-1 α signaling pathway via plasma adiponectin and muscular adipoR1. Molecul Nutrit Food Res 2019;63:e1800649.
Minokoshi Y, Kim YB, Peroni OD, Fryer LG, Muller C, Carling D, et al. Leptin stimulates fatty-acid oxidation by activating AMP-activated protein kinase. Nature 2002;415:339–343.
Acknowledgement
We thank professors from scientific sharing platform of Sun Yat-sen University for their technical assistance.
Author information
Authors and Affiliations
Corresponding author
Additional information
Supported by the National Natural Science Foundation of China (No. 81302877), Science and Technology Project of Guangdong Province of China (No. 2014A020212056)
Conflict of Interest|The authors declare no conflict of interest.
Author Contributions|Sun JP, Wang F and Ke B conceived and carried out the experiments. Sun JP, Qin J and Shi L conceived the experiments and analyzed data. Each author participated in the manuscript writing and approved the final version.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Sun, Jp., Shi, L., Wang, F. et al. Modified Linggui Zhugan Decoction (加味苓桂术甘汤) Ameliorates Glycolipid Metabolism and Inflammation via PI3K-Akt/mTOR-S6K1/AMPK-PGC-1 α Signaling Pathways in Obese Type 2 Diabetic Rats. Chin. J. Integr. Med. 28, 52–59 (2022). https://doi.org/10.1007/s11655-020-3285-2
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11655-020-3285-2